![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
212 Cards in this Set
- Front
- Back
|
What causes Johne's disease in cattle?
|
M. avium subsp. paratuberculosis
|
|
|
How is johnes disease diagnosed?
|
microscpoy on retal scraping, fecal smear and culture, immunological tests, johnin skin test
|
|
|
What agar is commonly used for fungi and what is its pH?
temperature are they grown at? |
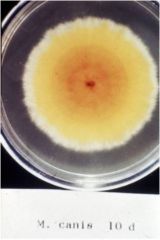
Sabouraud dextrose agar, pH 5.5 @ 25^C
fungi tend to tolerate low pH well |
|
|
What types of fungi are generally:
1. filamentous ? 2. branching ? 3. unicellular? |
1. Filamentous - molds
2. branching - molds 3. unicellular = yeast* * yeast tend to be oval or spherical |
|
|
What is an example of a filamentous fungi (moulds)?
|
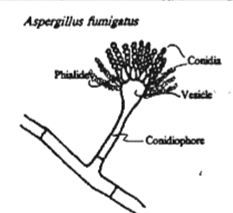
aspergillus
NOT dimorphic because never in yeast form |
|
|
What is an example of the unicellular fungi (yeast)
|
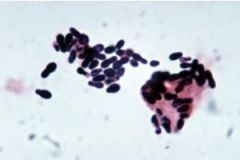
malassezia
|
|
|
What is mycelium?
temp. does it prefer? |
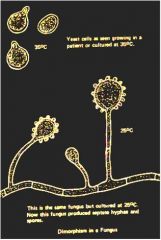
mass of hyphae
~one of dimorphic forms (other being unicellular yeast); grows at 20-25^C |
|
|
What anti-fungal is used for a variety of systemic mycotic infections?
|
Ketoconazole ("nizoral")
|
|
|
What is dimorphic?
|
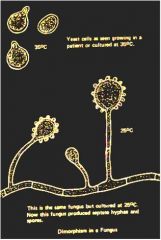
having yeast form (37 degrees) and mycelial form (25 degrees)
|
|
|
What are the categories of fungal disease?
|
Dermatomycoses
Yeast and yeast-like fungi Subcutaneous mycoses Systemic mycoses |
|
|
What narrow spectrum drug is used for yeast infections, including Candida?
|
Nystatin
|
|
|
What is the name for asexual spores?
|
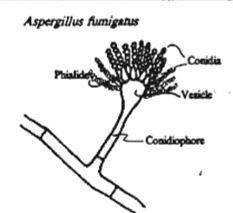
Conidia
|
|
|
Name 4 dimorphic fungi
|
1. Blastomycosis
2. Coccidoidomycosis 3. Histoplasmosis 4. Sporothrix schenckil |
|
|
What anti-fungal is given orally for ringworm infections?
|
Given orally for ringworm infections -> GRISEFULVIN
|
|
|
What are spores from hyphal fragmentation (ring worm fungi)
|
arthroconidia / arthrospores
|
|
|
Which of these cause systemic mycosis?
1. Blastomycosis 2. Coccidoidomycosis 3. Histoplasmosis 4. Sporothrix schenckil Any others? |
1. Blastomycosis
2. Coccidoidomycosis 3. Histoplasmosis Zygomycosis, Aspergillosis |
|
|
What causes ringworm, displays lesions on skin, hair and nails, as well as alopecia, erythema and crusts?
|
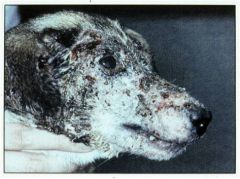
Dermatophytes
|
|
|
Which of these cause subcutaneous mycosis?
1. Blastomycosis 2. Coccidoidomycosis 3. Histoplasmosis 4. Sporothrix schenckil |
4. Sporothrix schenckil
* dimorphic but does NOT cause systemic mycosis, only hangs around in subcutaneous region |
|
|
What is is called when the natural habitat is soil?
|
geophilic
|
|
|
What are four species of Staphylococcus (and their primary hosts)?
|
S. aureus (zoonotic - everyone)
S. intermedius (cats&dogs) S. epidermidis (humans & ?) S. hyicus (neonatal pigs) |
|
|
What is it called when animals are the source?
|
zoophilic
|
|
|
How can Staph be diagnosed?
|
Smear (grape clusters)
Culture for Ab sensitivity Catalase Coagulase |
|
|
What is dermatomycoses?
|
ring worm fungi
|
|
|
Immunity, prevention and treatment of Staph?
|
Bacterins - limited use - (suspension of killed or weakened bacteria used as a vaccine).
Hygiene Drugs - CLOXACILLIN, amoxicillin-clavulanic, cephalosporins |
|
|
What are examples of yeast and yeast-like fungi?
|
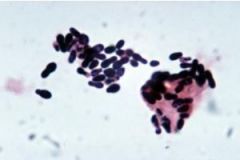
yeast: candida, malassezia
|
|
|
What is an example of subcutaneous mycoses?
|
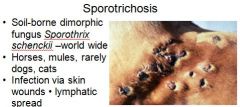
sporotrichosis
|
|
|
Aspergillosis, blastomycosis, histoplasmosis, coccidoidomycosis, and zygomycosis are examples of what?
|
systemic mycoses
|
|
|
What are general features of mycotic infections?
Chronic or acute? Morbidity high or low? Antibodies present? Host susceptibility? |
low morbidity and contagiousness, chronic nature, antibodies rarely present, lowered host resistance, prolonged antibacterial therapy
|
|
|
What are mycology laboratory procedures
|

wet mount with 10% KOH, scotch tape mounts in lactophenol cotton blue of fungal hyphae in culture, histological sections, latex agglutination, ELISA for fungal antigens in clinical specimens.
|
|
|
What are examples of antifungal therapy drugs?
(name 4 major ones and their primary targets) |
Amphotericin B (toxic),
Ketoconazole, Nystatin (for candida infections) Griseofulvin (orally for ring worm infection) Itraconazole (for Cryptoc.neoformans, systemic mycosis) |
|
|
What is caused by ringworm, is zoonotic, lesions restricted to skin, hair, and nails?
|
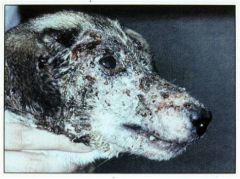
Dermatophytes
|
|
|
How is dermatophytes diagnosed?
|

wood's lamp (diagnostic tool which uses UV light to detect ?
wet mount culture on sabouraud |
|
|
What are signs of dermatomycosis or "ringworm" (3)
Hint: A E C |
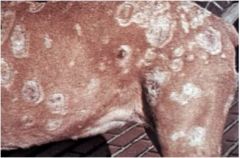
alopecia (loss of hair), erythema (redness of skin), and crusts
|
|
|
Resitance to re-infection of dermatomycosis is associated with what?
|
development of DTH
|
|
|
For ring worm positive cultures note a white powdery growth of possible M. canis on "fungassay" medium. Color of medium changes from what to what in positive cases?
|
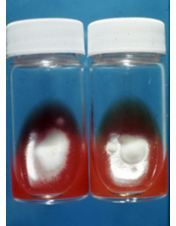
yellow to red
|
|
|
M. canis is mainly in what spp.?
Shape of cells? Morphology? Stain? |

zoophilic dermatophyte, in cats and dogs, spindle-shaped, macroconidia
|
|
|
M. gypseum is found where? morphology?
|
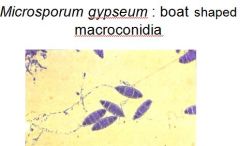
geophilic, in rodents, dogs, and horses, cigar shaped, macroconidium and numerous microconidia
|
|
|
M. nanum is what? host species?
|
M. nanum is geophilic (in soil), in PIGS
|
|
|
T. verrucosum is found in what spp.?
|

zoophilic, in cattle
|
|
|
T. equinum is found in what spp.?
|
zoophilic, in horses
|
|
|
Trichophyton mentagrophytes is found in what spp.?
Morphology? |

zoophilic, in dogs, horses, and cats
macroconidium - large conida microconidia - small conida |
|
|
Griseofluvin can be administered orally to what animals?
|
dogs, cats, and even cattle
|
|
|
What are anti-dermatophyte drugs?
|
Griseofluvin and ketoconazole
|
|
|
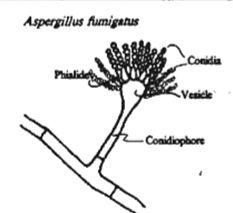
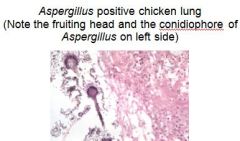
What is a disease mostly caused by A. fumigatus, causes brooder pneumonia in chicks, mycotic abortion in cattle, gutteral pouch mycosis and keratomycosis in horses?
|
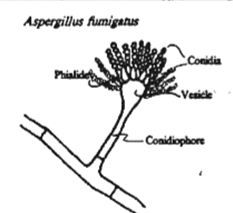
Aspergillosis <- A. fumigatus
also causes Nasal Aspergillosis in dogs! |
|
|
What is destruction of turbinate bones, profuse blood tinged exudate from nose?
|
Nasal Aspergillosis in dogs
|
|
|
Aspergillus produces what?
|
elastases and proteases, which destroy structural barriers of lung
|
|
|
How is aspergillosis diagnosed?
|
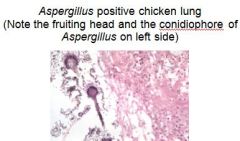
KOH wet mounts of deep scrapings, tissue - septate hyphae, radiograph rhinoscopy, culture on SAB medium, serological test (AGID) for dogs.
|
|
|
How is aspergillosis controlled and treated?
|
litter change, avoid bad hay, silage
Ketoconazole locally + itraconazole systemic for horses Natamycin or miconazole topical for kertitis in horses for Nasal aspergillous use Clotrimazole |
|
|
What is the preferred treatment for nasal aspergillosis in dogs?
|
clotrimazole nasal infusion
|
|
|
Where is yeast normally found?
|
commonly found on skin, mucous membranes
|
|
|
Candida, Cryptococcus, and Malassezia are examples of what?
|
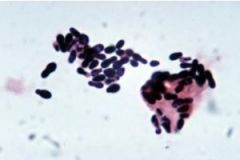
important yeast
|
|
|
What yeast is commensal of alimentary tract, and its infections are endogenous?
|
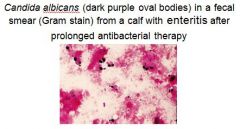
Candida albicans
* with take over if normal bacterial flora are decimated |
|
|
What is genital candidiasis in dogs and cats?
|
Mycotic stomatitis
|
|
|
What mycosis can occur in poultry?
|
crop mycosis or thrush
|
|
|
What causes vaginitis in horses?
|
metritis
|
|
|
What is the pathogenesis of the candida species?
|

Candida adheres to mm, pseudohyphae invade epithelium which leads to pseudomembranous ulcerative inflammation
|
|
|
How do you diagnose the candida species?
|
KoH wet mount or gram stain, culture, latex agglutination kits detect antigen in body fluids
|
|
|
How do you treat the Candida species?
|
Nystatin topical, ketoconazole, nystatin oral for GI overgrowth
|
|
|
What is the habitat of the Cryptococcus neoformans?
|
soil, pigeon droppings
|
|
|
What are symptoms of Cryptococcus neoformans?
|
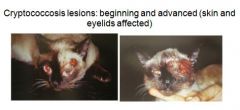
sneezing, snuffling, mucopurulent / hemorrhagic nasal discharge
(most disgusting images ever) |
|
|
How is Cryptococcus treated?
|
ITRACONAZOLE (1st choice in cats), fluconazole (2nd choice)
treatment for 6-10 months! |
|
|
Cryptococcus neoformans remains in YEAST form in what environments?
|

both environment (25 degrees C) and host (37 degrees C)
|
|
|
Cryptococcus produces enzymes including what?
|
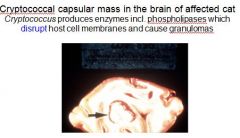
phospholipases which disrupt host cell membranes and cause granulomas
|
|
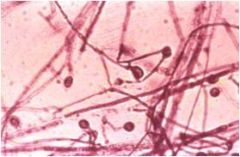
What causes chronic dermatitis (elephant like skin), otitis extern, and is bottle or peanut or footprint shaped yeast?
|

Malassezia pachydermatitis
|
|
|
How do you treat a Malassezia infection?
|
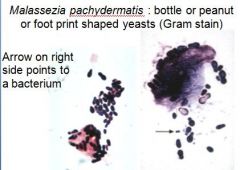
nystatin
|
|
|
what is the main animal affected by dimorphic fungi blastomycosis?
|
dog
|
|
|
What is soil borne, aerosol inhalation, causes granulomatous lesions in lungs, and respiratory distress?
|

Dimorphic fungi blastomycosis
|
|
|
Spores from mycelia can cause infections via what?
|
respiratory tract
|
|
|
What fungus has no capsule?
|
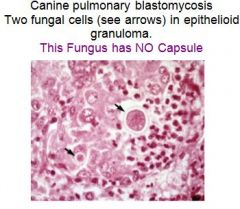
canine pulmonary blastomycosis
|
|
|
how do you diagnose blastomycosis?
|
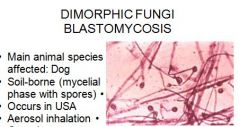
wet mount of transtracheal aspirate or skin lesion exudate, culture at 25 degrees C will show mycelia form
|
|
|
How do you treat blastomycosis?
|
Itraconazole, (60 days of treatment)
|
|
|
What is the source of dimorphic fungus Histoplasma capsulatum?
|
soil enriched with bat or bird excretion in the USA
|
|
|
How is the infection os Histoplasma capsulatum obtained?
|
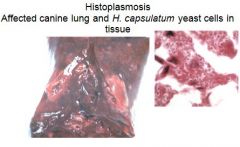
via inhalation, granulomatous lesions / nodules in lungs, intestine may be affected
|
|
|
What are symptoms of Histoplasma capsulatum?
|
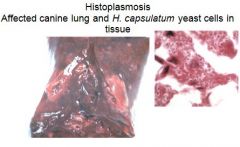
chronic cough, diarrhea, emaciation
|
|
|
How is Histoplasma capsulatum diagnosed?
|
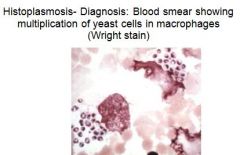
histopathy, buffy coat smear, serology
|
|
|
How do you treat Histoplasma capsulatum?
|
itraconazole or fluconazole
|
|
|
What is a soil or dust-borne dimorphic fungus that is popular in the southern USA and south america and mostly affects dogs?
|
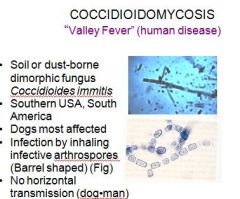
Coccidioidomycosis or "valley fever"
|
|
|
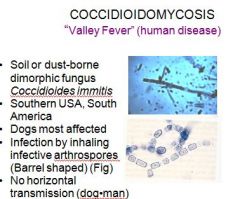
How do you get infected with "valley fever"?
|
Coccidoidomycosis: “Valley Fever” (human disease)
-> get by inhaling infective arthrospores |
|
|
Does coccidioidomycosis have horizontal transmission (dog -> man)?
|
No
|
|
|
What are signs in dogs of Coccidioidomycosis?
|
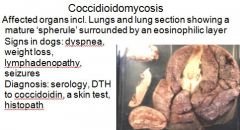
Signs of coccidoidomycosis in dogs:
- DYSPNEA (heavy breathing), weight loss, lymphadenopathy, seizures |
|
|
How is coccidioidomycosis diagnosed?
|
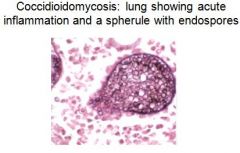
Serology
DTH to coccidioidin Skin test Histopath (shows mature "spherule" with endospores) |
|
|
How is coccidiodomycosis treated and controlled?
|
ketoconazole or itraconazole for up to 12 months, reduce exposure to dust in endemic areas
|
|
|
What is a soil borne dimorphic fungus that affects horses, mules, and rarely dogs and cats, that causes infection via skin wounds
|
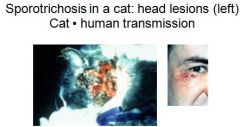
Sporotrichosis
|
|
|
Can sporotrichosis have cat to human transmission?
|
yes
|
|
|
How do you treat sporotrichosis?
|
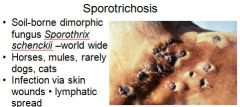
potassium iodide and sodium iodide for horses, itraconazole for cats
|
|
|
Rhizopus, Mucor, Absidia, and Mortierella are examples of what?
|
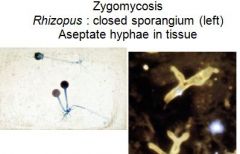
Zygomycosis
|
|
|
How is zyogomycosis treated and what is the prognosis?
|
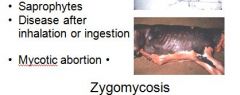
Amphotericin B, prognosis is poor
|
|
|
What is produced by mycotoxins formed by mold growing in feed, is non-contagious and is indicated by decreased feed consumption or feed refusal?
|
mycotoxicoses
|
|
|
What is a form of mycotoxicoses, that mainly affects cattle and poultry, causes bloodly diarrhea, death, icterus (jaundice), and abortion?
|
Aflatoxicosis - causes bloody diarrhea!! make sure to check feed!
|
|
|
What is a form of mycotoxicoses, that affects pigs, poultry and horses, causes weight loss, kidney and liver damage, and abortion?
|
Ochratoxicosis
|
|
|
What is caused by Claviceps purpurea growth in seedheads, affects cattle, sheep, horseas, pigs, and poultry, causes neurotoxicity, convulsions and gangrene of extremities?
|

Ergotism
|
|
|
What causes spoidesmin, liver damage, buildup of phylioerithrin, photodynamic activity, necrosis and sloughing of skin?
|
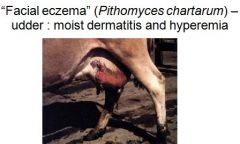
Facial Eczema or Pithomyces chartarum
|
|
|
How is facial eczema diagnosed and controlled?
|
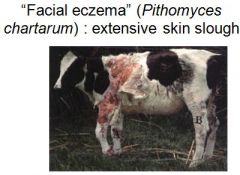
jaundice, history, sporidesmin, detection in blood by ELISA, controlled by fungicide spray, zinc salts in feed
|
|
|
What has > 30 species, mostly commensals of skin, mucous membrane, cause purulent lesions, multiply readily in milk and cheese and survives in hospital environment?
|
staphylococcus
|
|
|
What are staphylococcus tissue destroying enzymes/toxins?
|
lipase, hyaluronidase, exofoliative toxins, leukocidin
|
|
|
What do Beta Lactamases do?
|
destroy penicillins, cephalosporins
|
|
|
What are the disease conditions of staphylococcus in all animal species?
|
wound infections, abscesses, joint infections
|
|
|
What can staph cause in cattle, sheep, and goat? (Name 2)
Hint: 1 is only in lambs |
mastitis, tick pyemia-lambs
|
|
|
What can staph cause in swine?
|
exudative dermatitis/grease pig disease, mastitis
|
|
|
What can staph cause in dogs?
|
otitis externa, UTI, skin and vaginal infections
|
|
|
What can staph cause in cats?
|
secondary skin infections
|
|
|
What cans staph cause in horses?
|
botryomycosis (spermatic cord)
|
|
|
What can staph cause in poultry?
|
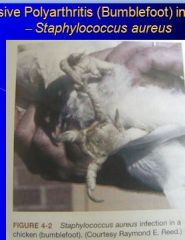
"bumble foot", arthritis
|
|
|
What can staph cause in pet birds?
|
diarrhea
|
|
|
What Staph strain is positive for double zone hemolysis, mostly virulent strains, causes infections in all species, but important in bovine mastitis?
|
S. aureus
|
|
|
What staph strain is positive for double zone hemolysis, associated with dogs pyoderma, otitis, UTI, eye infections?
|
S. intermedius
|
|
|
What staph strain is non-hemolytic, skin commensal, mostly non-pathogenic, occasional infections with cats?
|
S. epidermidis
|
|
|
What strain is non-hemolytic associated with pigs, exudative epidermitis ("greasy pig dz")
|
S. hyicus
|
|
|
How do you diagnose staph infections?
|
smear
culture for antibiotic sensitivity catalase coagulase ID |
|
|
What are signs of bovine mastitis (S. aureus)
|
peracute (gangrenous), fever, depression, anorexia, recumbency, rapid heart rate, acute, subacute, chronic, subclinical.
|
|
|
How do you diagnose bovine mastitis?
|
Culture
Somatic cell count (SCC) California Mastitis Test (CMT) |
|
|
How should bovine mastitis be treated?
How do you prevent bovine mastitis? |
* Antimicro.suscept. testing required.
* Intra-mammary infusion (IM or IV for acute) * Prevention: hygienic precautions dry-cow therapy culling SCC monitoring program - somatic cell count |
|
|
Is Staph intermedius normal on canine skin?
|
yes
|
|
|
What is required for effective treatment of S. intermedius?
|
antibiotic sensitivity testing
|
|
|
What is a commensal of skin, vagina, prepuce, and is a disease in pigs 1-6 weeks of age?
|
Greasy pig disease (staph hyicus)
|
|
|
What are signs of staph hyicus?
|
excessive sebacious secretion, exofoliation, greasy excudation on skin surface, non-pruritic dermatitis, anorexia, dehydration, death
|
|
|
How do you treat staph hyicus?
|
TMS systemic and topical antiseptics, fluid replacement, autogenous bacterins
|
|
|
What is gram + cocci in pairs or chains, is catalase -ve, and has variable types of hemolysis?
|
streptococcus
|
|
|
Can a strep infection be endogenous, exogenous, or both?
|
both
|
|
|
Which hemolytic strain of strep is more pathogenic, alpha or beta?
|
Beta
|
|
|
What strep stains hosts are dogs and horses, commensal of anal and vaginal mucosa, causes suppurative conditions, "puppy strangles", juvenile pyoderma, TSS, and neonatal septicemia in kittens?
|
Strep canis
|
|
What causes equine strangles, is an obligate pathogen, mucoid beta hemolytic colonies on BA, causes purulent pharyngitis, lymphadenitis, and occasionally inhalation pneumonia?
|
Strep equi
|
|
|
What can be transmitted from horse to horse via fomites, can rupture sub-mandibular lymph nodes and discharge highly infectious material, and shedding can take up to 6 weeks?
|
equine strangles
|
|
|
What are symptoms of equine strangles?
|
fever, nasal discharge, mild cough, swallowing difficulty, swollen lymph nodes of head, neck, rarely "bastard strangles", adscesses in many organs
|
|
|
How do you treat equine strangles?
|
penicillin to infected and in-contact horses, isolation, quarantine of new horses, vxns
|
|
|
How are S. equi (equine strangles) and subspecies Zooepidermicus differentiated?
How can equine strangles be differentiated from equine pnemonia? |
sugar fermentation reactions
|
|
|
What strep strain is in tonsils, nasal secretion, feces, repro tract of carriers, has many cap types, and is type 2 virulent?
|
Strep. suis
|
|
|
What can cause bovine mastitis, is mostly beta hemolytic, CAMP +, and is exclusively associated with mammary gland.
|
strep agalactiae
|
|
|
What are three strep strains that cause bovine mastitis?
|
S. agalactiae, S. dysgalactiae, S. uberis
|
|
|
What is the multipoint mastitis control program?
|
1. maintain a dry clean environment
2. establish regular sanitizing maintenance for milking equipment 3. individual wasd/dry towels 4. dry-cow therapy 5. somatic cell count monitoring, culling |
|
|
What is known as "stangles in hogs" cause abscesses in mandibular, pharyngeal, other lymph nodes, and is controlled by tetracyclines in feed at weaning time?
|
Steptococcal lymphadenitis (S. porcinus)
|
|
|
C. diptheriae causes what?
|
human diptheria
|
|
|
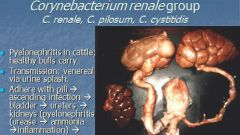
What causes pyelonephritis (kidney and ascending UT infection) in cattle, transmission is either venereal or via urine splash, adhere with pili, ascending infection affects bladder, ureters, kidneys?
|
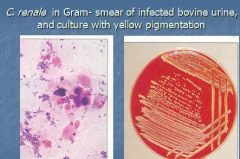
Corynebacteruim renale group, C. renale, C. pilosum, C. cystitidis
|
|
|
What can C. renale also cause that is controlled by reducing protein in diet?
|
Posthitis (inflammation of prepure) / ulcerative balanoposthitis in sheep and goats
-- "posthe" means foreskin in geek, i mean Greek! |
|
|
What is the agent of caseous (=cheese-like) lymphadenitis* in sheep and goats, also cause thin ewe syndrome, and rarely ulcerative lymphagitis in horses?
|
C. pseudotuberculosis
* Lymphadenitis is an infection of the lymph nodes |
|
|
How is C. pseudotuberculosis diagnosed and controlled?
|
diagnosed by smear
culture ELISA controlled by improving management (shearing culling clean dip) |
|
|
What is a gram + coccoid or short/ pleomorphic rods, on BA is pale pink colonies, and lives in intestine of horses, soil, stable contaminated with horse manure?
|
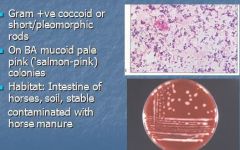
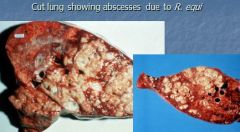
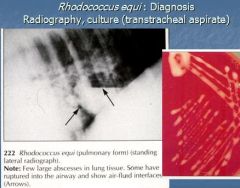
Rhodococcus equi
Gr(+) coccobacillus bacterium; found in dry, dusty soil, infects domesticated animals (horses and goats). |
|
|
Rhodococcus equi causes what in foals ~6 wks (rarely in pigs, humans and other species)
|
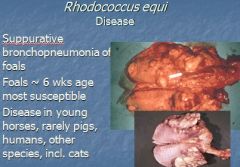
Suppurative bronchopneumonia of foals
|
|
|
What is the pathogenesis of Rhodococcus equi?
|
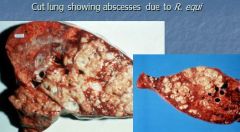
organism inhaled via contaminated dust, destruction of macrophages, destruction of lung parenchyma, suppurative* bronchopneumonia, abscesses in lung, lymph nodes
*suppurative = pus formation |
|
|
What should you treat clinical cases of Rhodococcus equi with > 4 weeks?
|
erythromycin and rifampin
|
|
|
Rifampin mainly used for:
|
Rifampin used for:
Mycobacterium (aerobic gr+ bacteria), Rhodococcus equi |
|
|
Erythromycin is what type of antibacterial agent?
|
Erythromycin is a MACROLIDE antibiotic; usually treats: G+ves mainly (strep, staph), and Campylobacter, Leptospira
|
|
|
What is a G+ pleomorphic rod mostly restricted to cattle, sheep, pigs, is an opportunistic pathogen and its habitat is mucous membranes and skin?
|
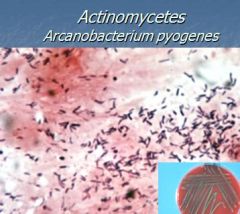
Actinomycetes/ Arcanobacterium pyogenes
|
|
|
pyometritis
purulent |
inflammation of uterus
(pyo = Gk. for "pus") purulent = from Latin word for pus formation (suppurative) |
|
|
What are symptoms of Arcanobacterium pyogenes?
|

abscesses, pneumonic infections, mastitis, pyometritis, arthritis, liver abscesses, foot rot lesions in sheep, lung lesions
|
|
|
What requires an anaerobic atmosphere + CO2, is a commensal of oral cavity of cattle, causes trauma of the oral mucosa, localized osteomyelitits, pyogranuloma with fistulous tracts and swelling?
|
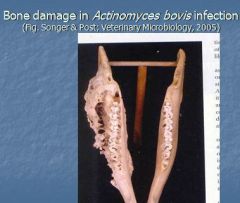
Actinomycetes / Actinomyces bovis
|
|
|
What causes granulomatous abscesses (accumulate of granulocytes) of skin/ subcutis in dogs, cats?
|
Actinomycetes viscosus
|
|
|
What causes localized abscesses or rarely pleuritis, peritonitis, arthritis, associated with grass awns in dogs?
|
Actinomycetes hordeovulneris
|
|
|
What is anaerobic, causes cystitis and pyleonephritis in pigs, anorexia, arching of back, hematuria, healthy boars are carriers, and penicillin is the drug of choice?
|
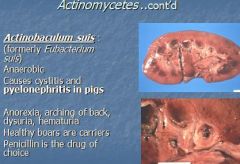
Actinobaculum suis
|
|
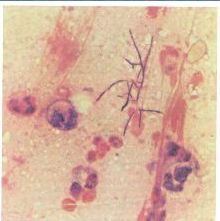
What is a g+ branching saprophyte, grows on BA as yellowis adherent colonies?
|

Nocardia
|
|
|
Can nocardia cause bovine mastitis by affected cow entry via contaminated infusion equipment?
|
yes
|
|
|
What is a cutaneous form of nocardia that causes indolent ulcer or granulomatous swelling with discharging fistulous tracts?
|
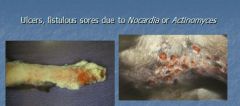
Canine nocardiosis
|
|
|
What is a g+, branching, causes skin infection of cattle, horses, sheep, and goats, causes "rain scald", "rain rot", "lumpy wool dz", "strawberry foot-rot"?
|
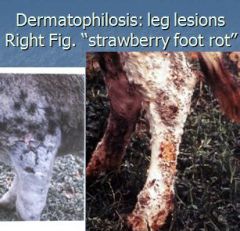
Dermatophilus congolensis
|
|
|
What can predispose animals to dermatophilus congolensis?
|
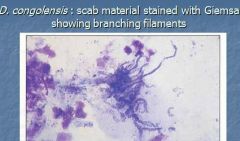
skin trauma, tick infestation,
|
|
|
What causes 'swine ___/diamond skin disease', septicemia in turkeys, arthritis in sheep, ___ in humans, _. tonsillarum endocarditis reported in dogs?
|

**Erysipelothrix rhusiopathiae**
swine erysipeloid, E. tonsillarum endocarditis reported in dogs erysipelas = means "red skin" ~human version not caused by same bacterium |
|
|
What is caused by fish meal contaminated feed or water, skin wounds and insect bites, has a septicemic form that causes red/purple skin patches, and a cardiac form that causes valvular endocarditis, dynsea and sudden death
|

Swine erysiapelas
|
|
|
What causes listerosis, a non-contagious disease in sheep, cattle, goats; also in other animal species including humans, and is small g+ coccobacilli/rods, grows at 5-45 C, tumbling motility at 25-30 C?
|
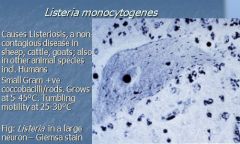
Listeria monocytogenes
|
|
|
What is the habitat of listeria monocytogenes?
|
saphrophyte*, found in poor quality SILAGE, decomposing vegetation, sewage, wild rodent feces
*saprophyte is organism that derives nourishment from dead and decaying matter |
|
|
The neural form of listeria monocytogenes causes what?
|

'circling disease' complete paralysis, death in 2-3 days in sheep
|
|
|
In what species does listeria monocytogenes cause abortion?
|
sheep and cattle
|
|
|
The septicemic form of listeria monocytogenes causes what?
|
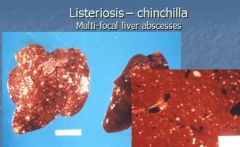
multifocal necrosis of liver and spleen in chinchillas, poultry, and young ruminants
|
|
|
How do you control and treat listeriosis?
|
eliminate bad silage, keep animals off pasture identified for silage, prevent abrasions in eyes from silage, penicillin, ampicillin, tetracycline, no vxn
|
|
|
What is mostly non-pathogenic, found in environment, G+, large spore forming rods which may be arranged as chains or threads, and the colonies have a ground glass surface and irregular appearance?
|
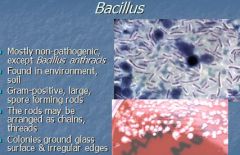
Bacillus
|
|
|
What is a hemolytic large flat colony with irregular edges?
|
Bacillus cereus
|
|
|
What causes septicemia, death, especially in cattle, causes exudation of tarry blood from rectum?
|

Bacillus anthracis
|
|
|
What animals are not susceptible to Bacillus anthracis?
What animal is most susceptible to bacillus anthracis? |
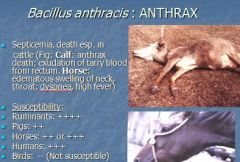
birds
1st: ruminant 2nd: horse/human |
|
|
In Bacillus anthracis, what factors are required for full activity?
|
edema factor, protective antigen, lethal factor
|
|
|
In the wild, what animals can spread bacillus anthracis?
|
flies and carnivorous animals
|
|
|
How do you appropriately deal with an anthrax infested carcass?
|
incinerate, bury deep in calcium oxide
|
|
|
What must be done for disinfection of bacillus anthracis?
|
10% formalin for 10 min
|
|
|
What has terminal drumstick shaped spores, lives in the soil, and causes tetanus?
|
Clostridium tetani
|
|
|
How do you treat/prevent clostridium tetani?
|
vaccination with tetanus toxoid, treat with antitoxin and penicillin, protect affected animal from light and noise
|
|
|
What causes botulism, is the most potent biological poison, can get it from infected feed, abattoir offal, dead fish, maggots, honey with spores (infant botulism)?
|
Clostridium botulinum
|
|
|
What are clinical signs of botulism?
|
straddled posture, profuse salivation, paralysed tongue
|
|
|
What are important histotoxic clostridia?
|
C. chauvoei, C. septicum, C.novyi/ C. haemolyticum, C. perfringens
|
|
|
What causes black leg in ruminants, especially young thriving cattle, lesions usually in hind leg muscle mass?
|
Clostridium chauvoei
|
|
|
What drugs can be used to treat mastitis (staph)?
|
Cloxacillin intramammary
Methicillin Vancomycin (last resort!) |
|
|
What is the pathogenesis of Clostridium chauvoei?
|
- spores in damaged muscle germinate
- multiply, necrotizing myositis, emphysematous gangrene, dark crepitant muscles, - systemic toxemia - death |
|
|
What are symptoms of black leg or C. chauvoei?
|
fever, lameness, crepitus muscle, mostly fatal
|
|
|
What clostridium strain is not common in the US, and is 'braxy' in seep (UK) and causes acute abomasitis after eatting frozen grass?
|
Clostridium septicum
|
|
|
What causes 'big head' in rams, and 'black head' disease in sheep
|
Clostridium septicum
|
|
|
What causes necrotic enteritis in piglets, classical enterotoxemia in sheep, and diarrhea/hemorrhagic enteritis in dogs, "yellow lamb disease"?
|
Clostridium perfingens
|
|
|
What causes Tyzzer's disease (diarrhea/enteritis, liver lesions) in small furies, dogs and calves, and is treated with oxytetracycline?
|
Clostridium piliforme
|
|
|
What causes diarrhea, enterotoxemia in rabbits and lab rodents, is diagnosed by G+ bacteria in feces and is treated by metronidazole and penicillin?
|
Clostridium spiroforme
|
|
|
What cause elcerative colitis in birds and is treated with tetracyclines
|
Clostridium colinum
|
|
|
What have g+ rods but classic species don't stain with gram stain, stain with acid fast + stain, are strictly aerobic; egg based media needed?
|
mycobacterium
|
|
|
What causes Tb in cattle, humans, and monkeys?
|
M. bovis
|
|
|
What causes Tb in humans, parrots, monkeys, and elephants?
|
M. tuberculosis
|
|
|
What causes Tb in birds including poultry and pigs?
|
Mycobacterium avium
|
|
|
What causes human leprosy, affects skin and peripheral nerves, zoonotic (has been found in armadillos), but domestic animals not affected?
Have cases of animal to human transmission ever occurred? |
mycobacterium leprae
Yes, armadillo to human |
|
|
What causes FELINE leprosy, not a zoonotic bacterium (not in humans), causes cutaneous nodules?
How is it treated? |
Mycobacterium lepraemurium
*treated by surgical removal of nodules, and anti-tubercular drug used with antibiotic? |
|
|
What can cause skin nodules in catlle, lesions in turtles, etc?
|
Atypical mycobacteria
|
|
|
What causes pseudomembranous colitis in humans, diarrhea and necrotic enterocolitis in foals, chronic diarrhea in dogs, and mesocolonic edema in piglets?
|
Clostridium difficule
|
|
|
What can be used in horses and in dogs to treat Clostridium difficule?
|
Dogs: Tylosin
Horses: Metronidazole |
|
|
What stain and culturing conditions does mycobacterium require?
|
Acid fast.
Strictly anaerobic, needs egg-based media. |
|
|
What pathogen infects macrophages, causes tubercles and calcification of lymph nodes, and has a 'Wax D' virulence factors?
|
M. Tuberculosis
|
|
|
How can leprosy be diagnosed?
|
Lepromin test (for DH)
ELISA |
|
|
What drug can be used to treat leprosy?
|
Dapsone (a sulfonamide-like compound)
|
|
|
What zoonotic bacterium causes leprosy in cats, which they contract from rats?
|
Mycobacterium lepraemurium
|
|
|
How can Equine Strangles (streptococcus equi) be diagnosed?
|
Culture discharges - mucoid beta hemolytic
Gr. C? Sugar fermentation tests |
|
|
What is used to treat/control equine strangles?
|
Penicillin
|
|
|
What are some example of virulence factors of streptococci?
|
Hemolysin
Streptokinase (indirectly digests fibrin clots) Hyaluronidase (digests CT) |
|
|
Can Streptococcus cause septicemia?
|
Yes
|
|
|
What can occur in dogs and cats, causes toxic shock syndrome, "puppy strangles", and neonatal septicemia in kittens?
|
Streptococcus canis
|
|
|
What vaccines are available for equine strangles?
|
Bacterin, M protein extract, modified live intranasal vaccine
|
|
|
What can Strept suis be treated with?
|
Penicillin
Ampicillin Tiamulin |
|
|
M. bovis lives naturally in the ____ of cattle throughout the world.
Cause of symptoms in ____ and ____ |
*in RESPIRATORY tract of cattle
* usually coloniz. produce no disease, but can cause of symptoms of respiratory disease in calves and feedlot cattle. |
|
|
How can A. bovis be diagnosed?
|
Smear: Gram + branching filaments
Crushed granules positive for clubs/rosettes |
|
|
How can A. bovis be treated, early and late?
|
Early: Penicillin
Late: Surgery and iodine dressing, sodium iodide IV |
|
|
What are other species of Actinomycetes?
|
A. viscosus
A. hordeovulneris Actinobaculum suis Unclassifiied |
|
|
How is Canine nocardiosis treated?
|
Trimethoprim-sulfa (TMS) or tetracyclines.
Penicillin is not effective. |
|
|
how is bacillus anthracis unique from other bacillis?
|
only which is CAPSULATED
|

