![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
56 Cards in this Set
- Front
- Back
|
Which bacteria are alpha hemolytic?
|
Streptococcus (all catalase-negative)
Optochin sensitive, bile soluble, or quellung positive: Streptococcus Pneumoniae Optochin resistant, bile insoluble, or quellung negative: Streptococcus Viridans (eg S. Mutans) |
|
|
Which bacteria are beta-hemolytic?
|
Rods: Listeria monocytogenes
Cocci: Catalase positive and coagulase positive: Staphylococcus Aureus, Catalase negative, Streptococcus -> Bacitracin sensitive, S. pyogenes. Bacitracin resistant, S. agalactiae. |
|
|
What are the important points about Listeria monocytogenes?
|
1. Tumbling motility, 2. Meningitis in newborns, 3. Unpasteurized milk
|
|
|
Gram positive: Which are catalase positive and which are catalase negative?
|
Positive: Staph, Negative: Strep
|
|
|
Gram positive: Which are catalase positive bacteria make coagulase?
|
Staph aureus does. Staph epidermidis and saprophyticus do not.
|
|
|
What is Protein A?
|
Virulence factor of Staphylococcus Aureus. Binds Fc-IgG, inhibiting complement fixation and phagocytosis.
|
|
|
What disease states does Staphylococcus Aureus cause?
|
Inflammatory: Skin infections, Organ abscesses (acute bacterial endocarditis, osteomyelitis),
Pneumonia Toxin-mediated: Toxic shock syndrome (TSST-1), Scalded skin syndrome (exfoliative toxin), Rapid-onset food poisoning (ingestion of preformed enterotoxin) |
|
|
What disease states does Streptococcus Pyogenes cause?
|
Pyogenic: Pharyngitis, Cellulitis, Impetigo; Toxigenic: Scarlet fever, Toxic shock syndrome; Immunologic: Rheumatic fever, Acute glomerulonephritis
|
|
|
What are two sequelae of Streptococcus Pyogenes pharyngitis?
|
Rheumatic fever and acute glomerulonephritis (Mnemonoic: PHaryngitis gives you rheumatic PHever and glomerulonePHritis)
|
|
|
Which antibody enhances host defenses against Streptococcus Pyogenes?
|
Antibody to M protein
|
|
|
Antibody to M protein enhances host defenses against what?
|
Streptococcus Pyogenes
|
|
|
What does ASO titer detect?
|
Recent S. Pyogenes infection
|
|
|
How can one detect recent S. Pyogenes infection?
|
ASO titer
|
|
|
What are the signs and symptoms of rheumatic fever?
|
Subcutaneous nodules, Polyarthritis, Erythema marginatum, Chorea, Carditis (bacterial endocarditis) (Mnemonic: No "rheum" for SPECCulation)
|
|
|
What is streptococcus pneumoniae the most common cause of?
|
Meningitis, Otitis media (in children), Pneumonia, Sinusitis - S. pneumoniae MOPS are Most OPtochin Sensitive
|
|
|
What is the most common cause of meningitis?
|
Streptococcus pneumoniae
|
|
|
What is the most common cause of otitis media?
|
Streptococcus pneumoniae
|
|
|
What is the most common cause of pneumonia?
|
Streptococcus pneumoniae
|
|
|
What is the most common cause of sinusitis?
|
Streptococcus pneumoniae
|
|
|
What is indicated by "rusty" sputum?
|
Streptococcus pneumoniae infection
|
|
|
What are common associations with Pneumococcus?
|
Streptococcus Pneumoniae - "Rusty" sputum, Sepsis in sickle cell anemia, and splenectomy
|
|
|
What does sepsin in sickle cell anemia pt indicate?
|
Streptococcus pneumoniae
|
|
|
What do Group B streptococci cause?
|
B for Baby - Pneumonia, Meningitis, Sepsis
|
|
|
3 most common causes of meningitis in infants younger than 3 months of age
|
E. coli, Listeria monocytogenes, Group B streptococcus
|
|
|
How do infants with meningitis present?
|
Fever, Vomiting, Poor feeding, Irritability
|
|
|
Name the Lancefield Group D bacterial categories and examples of each.
|
Enterococci: Enterococcus faecalis, Enterococcus faecium - Non-enterococci: Streptococcus bovis, Streptococcus equinus
|
|
|
What is Streptococcus bovis infection a sign of?
|
Colonic malignancy
|
|
|
What kind of hemolysis do enterococci cause?
|
Variable (CMMRS says alpha; FA says variable and gamma)
|
|
|
What drug resistances do the enterococci show?
|
Penicillin G, Ampicillin, Vancomycin
|
|
|
What is Lancefield grouping determined by?
|
Differences in the C carbohydrate on the bacterial cell wall
|
|
|
Which Group D bacteria are hardier?
|
Enterococci are hardier than nonenterococci. They can grow in 6.5% NaCl
|
|
|
A colony of bacteria grows in 6.5% NaCl. What is it?
|
Enterococcus
|
|
|
What disease states/problems does Staphylococcus epidermidis cause?
|
Infection of prosthetic devices and catheters. Contaminates blood cultures.
|
|
|
How is Streptococcus Viridans characterized?
|
1. Alpha hemolysis, 2. Optochin resistant, 3. Normal mouth flora (Mnemonic: Viridans lives in the mouth because it is not afraid of-the-chin)
|
|
|
Where is Strep. Viridans part of the normal flora?
|
Oropharynx
|
|
|
What disease states/problems does Streptococcus Viridans cause?
|
1. Dental caries (Streptococcus mutans), 2. Subacute Bacterial endocarditis (Streptococcus Sanguis)
|
|
|
What disease states does Streptococcus mutans cause?
|
Dental caries
|
|
|
What disease states does Streptococcus sanguis cause?
|
Subacute bacterial endocarditis, Sanguis = blood, lots of blood in the heart.
|
|
|
How are clostridia characterized?
|
1. Gram positive rods, 2. Spore forming, 3. Obligate anaerobes
|
|
|
What disease state does Clostridium difficile cause, and what is its mechanism?
|
Disease state: pseudomembranous colitis secondary to clindamycin or ampicillin use. (Mnemonic: DIfficile causes DIarrhea) - Mechanism: Antibiotic kills off protective flora, C. difficile takes hold and proliferates, Produces cytotoxin, an enterotoxin, Cytotoxin kills enterocytes.
|
|
|
Treatment for C. difficile infection
|
Metronidazole
|
|
|
Lab diagnosis basis for Cornyebacterium diphtheriae
|
Gram positive rods with metachromatic granules, grown on tellurite agar (aka Loffler's coagulated serum medium)
|
|
|
How is Bacillus anthracis characterized?
|
Gram positive rod, Spore forming, Protein capsule
|
|
|
Which bacteria have a protein capsule?
|
Bacillus anthracis (the only one)
|
|
|
What are the mechanisms of anthrax infection and disease?
|
Non-inhalation: Formation of malignant pustule (painless ulcer), Progression to bacteremia, Death - Inhalation of spores: Development of flulike symptoms that rapidly progress to fever, pulmonary hemorrhage and shock.
|
|
|
What organism: Development of flulike symptoms followed by fever, pulmonary hemorrhage and shock.
|
Inhalation anthrax: Bacillus anthracis
|
|
|
What do skin lesions in anthrax look like?
|
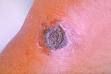
Vesicular papules covered by black eschar
|
|
|
What is Woolsorter's disease
|
Inhalation of Bacillus anthracis spores from contaminated wool
|
|
|
What organism: Gram-positive rods forming long branching filaments resembling fungi
|
Actinomyces israelii or Nocardia asteroides
|
|
|
What organism: Oral or facial abscesses with yellow granules in sinus tracts
|
Actinomyces israelii
|
|
|
What disease state does Actinomyces israelii cause?
|
Oral or facial abscesses with yellow granules draining out skin through sinus tracts
|
|
|
How is Actinomyces israelii characterised?
|
Gram-positive anaerobic rods forming long branching filaments resembling fungi (Nocardia also has this description) - Causes oral or facial abscesses with yellow granules
|
|
|
How is Nocardia asteroides characterized?
|
Gram-positive (weakly acid fast) rods forming long branching filaments resembling fungi (Actinomyces also has this description)
|
|
|
What disease state does Nocardia asteroides cause?
|
Pulmonary infection in immunocompromised patients
|
|
|
What is the treatment for Actinomyces israelii?
|
Penicillin (Mnemonic: SNAP (Sulfa for Nocardia; Acintomyces use Penicillin))
|
|
|
What is the treatment for Nocardia Asteroides?
|
Sulfonamides (Mnemonic: SNAP (Sulfa for Nocardia; Acintomyces use Penicillin))
|

