![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
97 Cards in this Set
- Front
- Back
|
Names for CHD
|
Ischemic heart disease (IHD)
Coronary Artery Disease (CAD) |
|
|
What is the source of most CHD ?
|
Atherosclerosis
|
|
|
Atherosclerosis
|
progressive narrowing of the arterial lumen
|
|
|
What are major risk factors Of CHD ?
|

|
|
|
What is atherosclerotic place mostly composed Of?
|
Lipids
|
|
|
Which Lipids are associated with higher risk of atherosclerosis ?
|
LDL's + Triglycerides
|
|
|
What are the types of Lipids?
|
LDL = BAD
Triglycerides = BAD HDL: Good |
|
|
How are HDL's good For Athero sclerosis ?
|
Transport cholesterol from peripheral tissues back to liver , thus removing plaque
|
|
|
Hyperlipidemia
|
Genetic
- defect in LDL receptor on liver cells - inability of liver to efficiently remove cholesterol from blood |
|
|
How is Atherosclerotic Plaque formed ?
|
1. initiated by injury to coronary artery epithelium
2. After injury endothelium-may become more permeable + recruit leukocytes 3. LDL 's leak through and Macrophages Oxidize them 4. Oxidized LDL's are damaging +timuiate recruitment of macrophages 5.macrophages engulf lipids (foam cells) 6. Macrophages + foam cells attract More leukocyteS 7.Excess lipids and debri accumulate within cell wall 8.They Colace into a lipid pool or core |
|
|
Which plaques are more prone to rupture?
|
ones with large lipid cores
|
|
|
What does a ruptured plaque cause?
|
initiates Platelet aggregation and thrombis formation
|
|
|
Which plaques are less likely to rupture?
|
Older plaques because they have more Collagen and fibrin
|
|
|
What happens when a plaque Occupies 75% or more of arterial lumen ?
|
sig. reduction in blood flow
|
|
|
Where can plaque be located?
|
Anywhere in the 3 major Coronary arteries or secondary branches
|
|
|
Difference between small and large lesions?
|
Small = fatty streaks, precursor lesions and asymptomatic
Advanced= small lesions that acquired More free lipids, cause narrowing Of lumen and are prone to rupture * this can cause thrombis formation |
|
|
What has to happen to be diagnosed with CHD ?
|
Critical narrowing of lumen then Sudden plaque rupture and Thrombs formation
|
|
|
stable plaques
|
asymptomatic
associated with exercise induced agina pain (stable angina pectoris) |
|
|
What is almost always associated With Plaque rupture ?
|
-Acute coronary syndrome
-Unstable angina -MI -.sudden Cardiac arrest |
|
|
What is ischemia?
|
insufficient Oxygen apply that Causes cell death
|
|
|
pathophysiology of Ischemia
|
the heart is unabe to slow its activity when ATP Supplies dwindle, a Steady flow of oxygen is essential
|
|
|
What are the critical factors in meeting cellular demands for Oxygen ?
|
1. Rate of coronary perfusion
2. Myocardial workload |
|
|
How can coronary perfusion be impaired?
|
Atherosclerotic plaque
Thrombis vasospasm Failure of auto regulation by microcirculation poor perfusion pressure |
|
|
Classic or stable Angina pectoris
|
When onset of ischemia is predictabe with certain activities and subsides with rest
|
|
|
ACS occurs when?
|
Obstruction of coronary blood flow results in Acute myocardial ischemia
|
|
|
What enhances risk of thrombus formation?
|
High fibrinogen levels (smokers)
Enhanced platelet adhesiveness (hyperlipidemia) |
|
|
How is a clot formed?
|
Begins with adherence of Platelets to the ruptured plaque
platelets that attach attract more and form a plug |
|
|
coagulation cascade
|
resluts in formation of platelet-fibrin clot that May occlude the vessel or break loose and travel
|
|
|
Aspirins Role?
|
long term use of small doses of aspirin reduces mortality from ischemic heart disease
|
|
|
What are Vulnerable plaques?
|
Those with large lipid cores, thin caps, or high Sheer stress
|
|
|
Myocardial ischemia may be cased by ?
|
coronary vasospasm , hypoxemia, Or low perfusion pressure
|
|
|
Angina Pectoris
|
Chest pain
- associate w/ MI |
|
|
What causes Angina pectoris?
|
conditions that increase myocardial Oxygen demand
• exercise • Stress • SNS activation • increase preload, after load, heart rate or muscle mass |
|
|
Referred pain
|
pain experianced in one location but felt in another
|
|
|
What may Angina pain be described as?
|
burning, crushing, squeezing, or choking
|
|
|
Atypical symptoms of MI ?
|
Back pain
fatigue weakness |
|
|
3 patterns of angina pectoris?
|
1. stable Angina
2. Prinzmetal variant angina 3. Unstable or Crescendo Angina |
|
|
Stable Angina
|
* Most Common form
* Classical or typical * reduction of coronary blood flow * predictable * relieved by rest and nitroglycerin |
|
|
What is nitroglycerin used For and what does it do?
|
Relieves stable Angina
ceases peripheral and Coronary Vasodilaton, reduces preload, and reduces myocardial workload |
|
|
Prinzmetal variant angina
|
* unpredictable attacks of anginal pain
* most have sig. coronary atherosclerosis * atherosclerosis is NOT what causes ischemic symptoms * Vasospasm is the Culprit * Treatment = Calcium channel blocking agents |
|
|
What are patients with Angina at risk for developing?
|
Acute Coronary Syndrome (ACS)
|
|
|
Acute Coronary syndrome
|
* A mix of unstable angina and MI
* Cause Chest pain that may be more severe and lasts longer than typical angina * may occur in those who were previously asymptomatic * Plaque rupture With thrombus formation Occurs |
|
|
Difference between unstable Angina and MI?
|
Unstable = Occlusion is partial or Clot will dissolve before the death of myocardial tissue
MI = occlusion is complete and thrombus persists long enough for development of irreversible damage to myocardial cells (necrosis) |
|
|
What has to be present to determine MI?
|
Bio-Markers
* CK-MB, Troponis I+T |
|
|
What is Reperfusion Therapy?
|
Treatment that restores blood back through blocked arteries
* only effective early in course of infarction |
|
|
Who is a candidate for reperfusion therapy?
|
patients with Chest pain and STEMI
|
|
|
what is a STEMI ?
|
ST-segment elevation
|
|
|
When does MI occur?
|
When prolonged or total disruption of blood flow to myocardium Causes cellular death by necrosis or apoptosis
|
|
|
What is the initiating event that causes MI?
|
thrombus on plaque
* sudden Change in plaque structure |
|
|
What is the role of platelets in Acute MI?
|
Platelets adhere to cracked plaque and forma plug, activate clotting cascade
* Thrombus grows until it occludes the vessel and triggers MI |
|
|
Where are most infarcts located?
|
Left ventricular walls
|
|
|
When can morphologic changes from MI be detected ?
|
6-12 hours after infarct
|
|
|
When does the infarct become Obvious to detect and why?
|
18-24 hours after infect
* area becomes yellowish + soft with a rim of red vascular connective tissue |
|
|
When is the necrotic tissue progressively degraded and Cleared from the site?
|
1 to 2 week after infarct
* myocardium is weak and susceptible to rupture at this time |
|
|
When has the necrotic tissue been replaced by scar tissue?
|
6 weeks after infarct
|
|
|
What is the diagnosis of a MI made from?
|
1. S+S
2. ECG changes 3. Elevaticn in Specific marker proteins |
|
|
MI pain can be described as?
|
Severe crushing, excruciating Chest pain.... may radiate to arm , Shoulder, neck, back
|
|
|
Are MI's relieved by nitroglycerin ?
|
NO
|
|
|
How long do MI's normally last longer than?
|
15 minutes
|
|
|
How is necrotic tissue shown on an ECG?
|

* Abnormally deep Q waves
* Inverted T waves * Elevation of ST |
|
|
List the serum markers
|
CK-MB
Troponin I Troponin T |
|
|
How long does the CK-MB Stay elevated for?
|
48-72 hours after MI
|
|
|
What are the markers of Choice for detecting MI?
|
Troponin I + T
* because they remain elevated for longer periods of time * Not good for new infarction (reinfaction) |
|
|
What causes the Q Wave findings?
|
totally ischemic cells, which die and become electrically silent
* release serum marker proteins |
|
|
What is responsible for ST elevation ?
|
Abnormal iron flux
|
|
|
Treatment for MI is directed at?
|
*decreasing 02 demand
* increasing Myocardial 02 supply |
|
|
What is sudden cardiac Arrest?
|
unexpected death from cardiac arrest within 1 hour of the onset of symptoms
* CAD usually cause * high risk of having another if you survive the first |
|
|
Chronic Ischemic Cardiomyopathy
|
Heart failure develops insidiously as a Consequence of progressive ischemic Myocardial damage
* had a history of angina or mi * common in the old |
|
|
Stenosis
|
Failure of a Valve to Open Completely
|
|
|
Regurgitation (insufficiency)
|
inability of a valve to close completely
|
|
|
What are the primary causes of stenosis?
|
Rheumatic heart disease and Valvular Calcification with aging
|
|
|
What are Valvular disorder often associated with?
|
Abnormal turbulence of blood that produces Murmurs
|
|
|
Mitral Stenosis
|
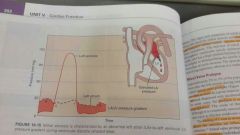
Flow of blood from the left atrium into the left ventricle is impaired
* not enough blood coming out * decrease cardiac output * increased left atrium Pressure from back Flow |
|
|
S+S of Mitral Stenosis
|
left atrium hypertrophy
Afib clots , embolism , Stroke Pulmonary Congestion * orthopenea * cough * dyspnea(exertional)=Most common complaint * poor 02 sat |
|
|
Mitral Regurgitation
|
Backflow of blood from left Ventricle to left atrium during ventricular systole
* giant V wave *high after load increases regurgiant flow *hypertrophy + dilation *eventually lead to left sided HF |
|
|
S+S of Mitral Regurgitation
|
Pulmonary congestion
poor cardiac Output Chronic weakness + fatigue |
|
|
Mitral valve Prolapse
|
Mitral ValVes that balloon into the left atrium during systole
|
|
|
Aortic Stenosis
|
Obstruction to aortic outflow from the left ventricle into the aorta during systole
*Could lead to left heart failure * cause is age related calcification *FORMATION OF CALCIUM DEPOSITS ON CUSPS!! *70-90 years old *high pressure in left ventricle |
|
|
S+S of Aortic stenosis
|
Diminished Cardiac output
* syncope * fatigue * low systolic BP * faint pulses Pulmonary complications later on |
|
|
aortic Regurgitation
|
blood leaks Back from aorta into left ventricle during diastole
* left ventricle becomes overloaded * left Ventricle hypertrophy + dilation * large stroke volume , high systolic bp |
|
|
S+S of Aortic Regurgitation
|
bounding peripheral pulsation
* head may bob with each systole * complain of palpitations and a throbing or pounding heart * left sided heart failure |
|
|
Rheumatic Heart Disease
|
From rheumatic Fever = acute Inflammatory disease from strep
* damage from immune attack on the individuals own tissues |
|
|
Infective Endocarditis
|
inflammation of Endocordium
*vegetation on valves * biggest cause = strep * blood born •IV users • recent value replacement • major surgery -antibiotics b4 procedures |
|
|
Myocarditis
|
inflammation, leukocyte infiltration and necrosis of cardiac muscle cells
|
|
|
Acute myocarditis
|
left ventricular dysfunction or dilation of all four chambers
* myocardium of Ventricle is flabby With patchy or diffuse nerotic lesions |
|
|
Cardiomyopathy
|
Weakening of heart muscle
* heart becomes thick, rigid, or enlarged |
|
|
Dilated Cardiomyopathy
|
Ardiac failure associated With dilation of one or both ventricular Chambers
|
|
|
Causes of DCM
|
Alcohol toxicity
genetic abnormalty pregnancy Post viral myoccrditis |
|
|
Hypertrophic Cardiomyopatty
|
characterized by thickend, hyperkinetic Ventricular muscle mass
* left and\ or right ventricular hypertrophy * asymetric * usually involves septum * genetic |
|
|
restrictive Cardiomyopathy
|
Rarest form
* Stiff, fibrotic Ventricle with impaired diastolic filling * reduced diastolic size of either or both ventricles * idiopathic |
|
|
Pericardial Effusion
|
Accumulation of fluid in the pericardial sac
* normally has 30 -50mL of clear thin fluid |
|
|
Types of effusions
|
Serous= transudate secondary to heart failure or hypoproteineMia
Serosanguineous= serous fluid and blood Chylous = collection of lymph from Obstruction of lymphatic drainage Blood = hemopericardium usually resulting from penetrating trauma to the heart |
|
|
Cardiac Tamponade
|
large fluid accumulation that causes Compression of the heart Chambers Which causes impaired filling
|
|
|
S+S of Cardiac Tamponade
|
3 classical findings
•hypotension •distended neck veins •muffled heart sounds reduce stroke volume increase heart rate systemic venous congestion *distended neck veins waxing and waning of BP |
|
|
Acute Pericarditis
|
*80% are idiopathic -viral
* resolves spontaneously within 2 weeks * NSAID's only therapy * presents with chest pain * rubing of pericardial layers may be heard as a friction rub - squeaky or like scratch sandpaper |
|
|
Chronic Pericarditis
|
Healing of an acute form of pericardial inflammation
• destruction of pericardial sac • adhesion of heart to surrounding mediastinai structures • impaired cardiac contraction |
|
|
Constrictive pericarditis
|
results in a fibrous, Scarred pericardium that restricts cardiac filling
|

