![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
51 Cards in this Set
- Front
- Back
|
Communication |
Exchange of information, thoughts, or messages, includes interpersonal Rapport, also includes the accurate conveyance of information, clear self-expression, and transmission of information and ideas to others |
|
|
Emotional intelligence |
The ability to evaluate, perceive, and control emotions |
|
|
Maslow's hierarchy of needs |
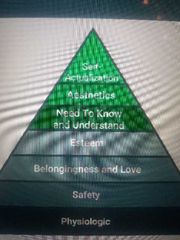
Model of human needs developed by Abraham Maslow, original hierarchy identifies two types of needs: deficiency and growth needs were further divided into seven levels. |
|
|
Patient assessment |
Objective evaluation and determination of the status of a patient |
|
|
Three steps of patient assessment |
Step 1: view the patient's chart or procedure request or both
Step 2: verbal communication with the patient Step 3: informed consent must be obtained from the patient under certain conditions |
|
|
Inpatient |
Someone who has been admitted to the hospital for Diagnostic studies or treatments |
|
|
Outpatient |
Patient who comes to a healthcare facility for diagnosis or treatment but does not usually occupy a bed overnight |
|
|
Verbal communication |
Messages to using spoken words , the exchange of information or thoughts, can be dramatically shaped by vocabulary , Clarity, tone, pitch a voice, and even the organization of sentences |
|
|
Nonverbal communication |
Exchange of information, thoughts, or messages using methods other than the actual words of speech. For example, tone of voice, speed of speech, facial expressions, and body language |
|
|
Speech and grammar |
Vocabulary, Clarity of voice, and even organization of sentences must be at a level appropriate for the patient |
|
|
Humor |
Using humor to relax and open up conversation is acceptable, but the technologist must be extremely careful to avoid cultural slurs and references to age, sex, diseases, and the abilities of other health professionals |
|
|
Paralanguage |
Music of language, the inflection of the voice and rhyme of speech |
|
|
Body language |
The position of the speaker's extremities and torso |
|
|
Three types of touch commonly used by radiologic Techs |
Touching for emotional support.
Touching for emphasis.
Touching for palpation. |
|
|
Palpation |
Application of light pressure with fingers |
|
|
Professional appearance |
Dressing professional help the patient feel more comfortable and confident in the technologist abilities |
|
|
Personal hygiene |
Unkept individuals may prompt patients to suspect that the person's personal behavior is similar to his or hers appearance , neglected |
|
|
Physical presence |
Posture is important because it is perceived as relating to confidence and self esteem |
|
|
Visual contact |
Eye contacts may help ensure that questions, instructions, and other information I have been understood |
|
|
Toddlers 1 to 3 years |
Are only concerned with what you are doing to them at the moment |
|
|
Preschoolers 3 to 5 years |
They must see or hear something to understand and must be actively involved to maintain their short attention spans |
|
|
School-age children 5 to 10 years |
At approximately age 7 children begin to think logically and analyze situations. Pay special attention to divert their attention from negative aspects of the exam |
|
|
Gerontology |
The study of aging and disease of older adults |
|
|
Five stages of grief |
Denial.
Anger.
Bargaining.
Depression.
Acceptance. |
|
|
Denial |
This and isolation may be the initial reaction and should be supported by silence and acceptance of the person without discussion of death |
|
|
Anger |
May occur as a result of the realization that life will be interrupted before everything the person planned has been accomplished and feeling that the person will soon be forgotten |
|
|
Bargaining |
Some patients experience the stage that focuses on Hope and maybe based in religion |
|
|
Depression |
Comes with the realization of the invisibility of death. The feeling is accompanied by a desire for death as a release from suffering. Permit this Behavior |
|
|
Acceptance |
Can only occur if enough time is provided and if the patient is appropriately helped through the other stages. The stage is characterized by a near-total lack of feelings |
|
|
Advance directive |
Legal document prepared by living, competent adult to provide guidance to the Health Care team if the individual should become unable to make decisions regarding Medical Care. May also be called a living will or durable power of attorney for health care |
|
|
Patient Anatomy |
Ability and right of patients to make independent decisions regarding their medical care |
|
|
Clinical history |
Information available regarding a patient's condition. Traditionally compromises data on localization, quality, quantity, chronology, setting comma aggravating or alleviating factors , and associated manifestations |
|
|
Data collection process |
Good history taking involves the collection of accurate objective and subjective data |
|
|
Objective data |
Data that is perceptible to the external senses |
|
|
Subjective data |
Data that is pertaining to or perceived only by the effective individual. Not perceptible to the senses |
|
|
Leading questions |
Undesirable method of questioning that provides information that may direct answers toward a suggested symptom or complaint |
|
|
Sacred seven |
7 elements recognized for a complete medical history Localization. chronology. Quality.
Severity.
Onset.
Aggravation or alleviating factors. Associated manifestations |
|
|
Localization |
Determination of a precise area, usually through gentle palpation or careful wording of questions |
|
|
Chronology |
Time element of the history, usually including the onset, duration, frequency, and course of the symptoms |
|
|
Quality |
Description of the character of the symptoms. For example , the color, quantity or size, and the consistency of blood or other body substances, size or number of lumps or lesions, frequency of urination or coughing, or character of pain. |
|
|
Severity |
Describes the intensity, quantity, or extent of the problem |
|
|
Onset |
Describing the onset of the complaint involves the patient explaining what they were doing when the illness or condition began |
|
|
Aggravation or alleviating factors |
The circumstances that produce the problem or intensify it should be well defined, including anything that aggravated, alleviates, or otherwise modifies it |
|
|
Associated manifestation |
Determining whether other symptoms accompany the chief complaint may be necessary to determine whether all of the symptoms related to the chief complaint or are related to a separate condition |
|
|
Communicating with non-english-speaking patients |
Interactions are greatly enhanced by using touch, facial expressions, and pantomime. Most of these patients understand basic words such as yes, no, and stop |
|
|
Communicating with mentally impaired patients |
Used communication, respect, gentle tones, and a smile. Use their knowledge and equipment and immobilization techniques. Use continuous conversation while preparing the patient for the exam will usually help keep the patient calm and wear |
|
|
communication with substance abusers |
Assess the patient's capabilities. Attempt to establish a means of communication. Used technique knowledge and work efficiently to decrease the exam time. Patient may need to be restrained, but only if prescribed in facility procedure and policy |
|
|
Deficiency and growth |
What two types of needs are identified in Maslow's hierarchy of needs |
|
|
Communication with seriously ill and traumatized patients |
Try to communicate with the patient to determine their coherence level. Work quickly and efficiently while continuing to communicate with the patient. Watch the patient for changes in vital signs. |
|
|
Communication with visually impaired patients |
Gain the confidence of the patient by giving clear instructions before the beginning of the exam. Inform the patient of what is occurring at all times. Reassure the patient through Gentle Touch to guide them through instructions and let them know someone is there if needed |
|
|
Communication with speech impaired or hearing impaired patients |
For patients who can read the primary means of communication can be written. Panta mine and demonstration works as well. Your facility May provide a sign language interpreter. |

