![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
119 Cards in this Set
- Front
- Back
|
List the 4 acquired cystic diseases
|
Cystic dysplasia
Polycystic kidney disease Medullary cystic disease (cilary disfunction causing tubular dilation and cyst formation) Acquired cystic disease |
|
|
Describe the general features of Pckd
|
Bilateral, multiple expanding huge cysts. 10% require transplantation.
Generally presents at 5th decade with pain, renal colic, proteinurea, renal failure. |
|
|
What are the genetic abnormalities of PCKD
|
Autosomal dominant
PKD1 80% and PKD2 |
|
|
What are the extra renal complications of PCKD
|
Liver, spleen, lungs and berry aneurisms. CAD and hypertension are common
|
|
|
How does the histology of juvenile PCKD differ to the adult form
|
Cysts radiate from the medulla
|
|
|
Medullary sponge kidney
|
Affects 1:200 adults
Asymptomatic but 2nd infections, calcili, calcifications |
|
|
Nephronothisis
|
Progressive, childhood onset, commonest cause of end stage disease
Distal tubular pathology where cysts forms in the medulla. Cortex is normal. Cysts are small and not detectable on imaging and diagnosed clinically |
|
|
What sort of calculi and obstruction do dialysis patients get
|
Obstruction of tubules by oxalate. Patients on dialysis get this disease
|
|
|
Prerenal causes of failure
|
Hypotension, hepatorenal syndrome. Atheroemboloc disease, sepsis
|
|
|
Post renal causes of failure
|
Stones, malignancy, prostate, VUR
|
|
|
Causes of ATN
|
Ischaemic, hypertension, toxins
|
|
|
What are reversible and irreversible stages of ATN
|
Sweling
loss of brush border blebbing lethal: necrosis and apoptosis |
|
|
What is the pathology of ischaemic ATN
|
Patchy but full thickness necrosis including the basement membrane causing vacuolated tubules. 50% won't recover
|
|
|
What are the 3 stages of ATN
|
Initiation - normal urine flow
Maintenance - decrease in Urine flow Recovery - regeneration of epthelium |
|
|
Chronic renal failure causes
|
Glomerulonephritis
Vascular Tubulointerstitial - PCKD Obstruction |
|
|
What are the sequelae of CRF
|
CCF
accelerated atheroschlerosis Azotemia and uremia - lethargy and pericarditis hperparathyroidism and hypercalcemia |
|
|
How does CRF look histologically
|
Schlerosed glomeruli and necrosed tubules
|
|
|
Urolithiasis
|
Within pelvis most common due to stagnation. Also infection and stasis promoted calculus formation, Also low urine volume causes supersaturation and precipitation.
|
|
|
What are the 4 types of stones
|
Calcium oxalate, phosphate
Triple Uric acid Cysteine |
|
|
Calcium oxalate stones
|
Hypercalcaemia
|
|
|
Triple stone mechanism of formation
|
Bacteria split urea to ammonia. Alkaline urine causes precipitation of the 3 ions. Staghorn calculi form
|
|
|
What are the factors causing stone formation
|
Concentration
Low or high pH Decreased urine volume Stasis Bacteria |
|
|
What are the sequellae of stone formation
|
Pain
Ulceration and bleeding Hydronephrosis Renal colic Stagnation and infection causing a positive feedback |
|
|
What casts can be found in urine
|
Tam Horsfall (protein produced by distal tubules)
Hyaline (can be normal) Lipid |
|
|
Describe the cancer CCRCC. Whate are the risk factors
|
Clear cell renal cell carcinoma (most common cancer 80%. It is a proximal tubule carcinoma of mesodermal origin) causing haematurea, palpable kidney and paraneoplastic syndrome (epo, pth, acth)
Massive, greasy, yellow, fatty. Risk factors are smoking, obesity, hypertension |
|
|
In CCRCC, why are the cells clear. What is the histological grading system? How is it spread. What other features are visible
|
Fat, glycogen
Grading using Thurman system Haematogenous only. Commonly the veins are invaded. Necrosis, |
|
|
Spindle cells are found in a biopsy of ccrcc. What are the prognostic implications
|
Sarcomapoid change. Poor prognosis reflecting an increase of grading to grade 4
|
|
|
What other renal carcinomas exist other than CCRCC
|
Papillary RCC 10%
Chromophobe RCC 5% Collecting duct RCC 1% |
|
|
How is papillary rcc different to ccrcc
|
It is multifocal, made up of vascular papilla. There are no cysts or necrosis. It is not fatty
|
|
|
Describe a chromophobe rcc
|
Encapsulated fleshy looking, well circumscribed brown tumour. Generally has a central fibrous scar.
|
|
|
A 5cm abdominal renal mass is found on US of a 4 yo child. What is it. Describe the features.
|
Nephroblastoma. Most common abdominal tumour of children 1-4yo. Made up of nephrogenic elements (blastema or undifferentiated mass, abortive glomerulus or spindle cell stroma). Also called Wilms tumour causing WAGR, Beckwith -Wideman syndrome (hemi hypotrophy and microglossia)
Apearance is large, necrotic |
|
|
A 35 yo man has a renal tumour and presents with hypovolaemic shock. On biopsy there are dilated blood vessels adjacent to lots of fat. What is it.
|
Angiomyelolypoma where smooth muscle spindle cells forms around blood vessels causing them to grossly dilate, found together with lots of adipocytes.
It is the most common benign tumour of adult kidneys and can cause retroperitoneal haemorrhage and shock |
|
|
A white circular tumour is found in a child's kidney in the medulla.
|
Medullary fibroma
|
|
|
What are risk factors for bladder cancer
|
smoking
industrial dyes cyclophosphamide IDC inflammation |
|
|
What are the types of bladder cancer
|
Urothelial (pappiloma, carcinoma in situ, low and high grade papillary carcinoma - recall a papilla is a finger like projection with a blood vessel core)
Adenocarcinoma (from the urachis) SCC (schistosomiasis) Rhabdomyosarcoma (young kids) |
|
|
In situ carcinoma is diagnosed how?
|
Epithelium is abnormal and detaches into the urine and easily diagnosed by urine specimen
|
|
|
A patient with clolicy abdo pain shows blood and Proteus in the urine. What is happening
|
Proteus is urea splitting forming ammonium ion cauding precipitation of triple (struvite) stones
|
|
|
What is the consequence of a staghorn calculus in the kidney
|
Hydronephrosis (dilatation of calicys and pelvis)
Pyelonephritis Fibrosis of the cortex and destruction of the medulla leading to renal failure |
|
|
What are the different cells of the glomerulus
|
Endothelium
podocytes mesangium |
|
|
Define proteinurea
|
3.5 g per day in frothy urine
|
|
|
What happens with protein loss with nephrotic syndrome
|
Increased serum lipids as compensatory mechanism for hypoalbuminemia with lipidurea
|
|
|
Nephritic syndrome
|
Deposition of exogenous or endogenous immune complexes causing glomerular inflammation
|
|
|
Complications of biopsty
|
Pain, bleeding, arteriovenous fistula, other organ puncture
|
|
|
Distinguish diffuse, focal, global or segmental glomerular injury
|
Diffuse means widespread
Focal is located in part of the kidney Global means the whole glomerulus Segmental means part of the glomerulus is injured |
|
|
What are the histological classifications of glomerular abnormalities
|
cellular proliferation within the mesangium
GBM thickening |
|
|
Causes of asymptomatic haematurea
|
IgA nephropathy (follows strep)
Alports syndrome Thin GBM nephropathy (alteration of colagen iv genes) |
|
|
Nephrotic syndome
|
Minimal change nephropathy is most common glomerulonephropathy in infants caused by loss of pedicels.
In adults, membranous glomerulonephroprathy caused by thickening of basement membrane as a result of IgM immune complex deposits. It progresses in stages, with stage 1 with naked immune deposits to stage 3 where basement membrane grows over deposits. Causes are lupus, cancer. |
|
|
Diabetic glomerulosclerosis
|
No 1 cause of renal failure in western world caused by glycoselation of proteins. Proteinurea caused by expansion of mesangial matrix, gbm thickening, Klimmelstiel-Wilson nodules (made up of pink hyaline matrix), hyaline arterial sclerosis causing thickened arteriole walls
|
|
|
Focal segmental glomerulosclerosis
|
Granular deposition of IgM and C3 in a segment of the kidney in part of the glomerulus with part of it being normal.
|
|
|
What is meant by a hypercellular glomerulus
|
Deposition of immune complexes causes infiltration of neutrophils and mesangial proliferation
|
|
|
How is acute post strep glomerulonephritis different to IgA glomerulonephritis
|
In acute post strep, IgG and C3 deposits sub epithelial causing proteinurea, haematurea and acute renal failure. With IgA, the deposition is intraglometular and haematurea is asymptomatic
|
|
|
Crescented glomerulonephritis
|
Linear deposition of IgG throughout the basement membrane. Can be associated with Goodpasture and causes rapidly deteriorating renal function
|
|
|
ANCA glomerulonephritis
|
Anti neutrophic antibodies causing release of neutrophil proteases causing destruction of the basement membrane and a form of crescented glomerulonephritis
|
|
|
What are the 3 matching criteria for renal transplantu
|
Blood typing
HLA matching (less important) Cross matching (looking for direct cross reactions between donor and recipient blood - looking for preformed HLA antibodies against the donor) |
|
|
A group A kidney is placed into a group O patient. What happens
|
Glomerular endothelial cells are destroyed by anti A antibodies in the group O recipient
|
|
|
Why is the host v graft response so severe
|
Because the HLA proteins are different, the MHC that is formed with binding of, not only antigens, but anything is recognised as foreign, the immune response is massive
|
|
|
What is the principle action of cyclosporin
|
Inhibits calcineurin and reduces cytokine production, esp IL2
|
|
|
What is mycophenolate
|
Antiproliferative, much stronger than azothioprine and steroids
|
|
|
Describe the most common nephrosis in children
|
Minimal change disease where immune complexes deposit within podocytes causing detachment of pedicels allowing albumin loss
|
|
|
What viral infections are of concern following transplant
|
CMV - primary infection is severe
EBV causes post transplant lymphoproliferative disorder resembling lymphoma |
|
|
What cancers are of concern following transplant
|
30x increased risk of skin cancers (esp SCC)
Women should be screened for cervical and breasr cancers |
|
|
What monitoring should occur pre and post transplant
|
Cancers
Osteoporosis Vaccinations Cardiovascular risk factors (lipids, hypertension, antiplatelets) |
|
|
Describe nephrotic syndrome and it's clinical features
|
Increased permeability of the basement membrane giving the clinical features of:
1) hypoalbuminaemia 2) massive proteinurea > 3.5g/day 3) oedema 4) compensatory lipoprotein production causing hyperlipidemia Four diseases: 1) Minimal change disease (kids) 2) focal segmental glomerulonephrosis (IgM and hyaline deposition) 3) Membranous glomerulonephritis (sub epithelial deposits forming spikes and domes in basement membrane) 4) Membranoproliferative |
|
|
What viral infections are of concern following transplant
|
CMV - primary infection is severe
EBV causes post transplant lymphoproliferative disorder resembling lymphoma |
|
|
What cancers are of concern following transplant
|
30x increased risk of skin cancers (esp SCC)
Women should be screened for cervical and breasr cancers |
|
|
What monitoring should occur pre and post transplant
|
Cancers
Osteoporosis Vaccinations Cardiovascular risk factors (lipids, hypertension, antiplatelets) |
|
|
What viral infections are of concern following transplant
|
CMV - primary infection is severe
EBV causes post transplant lymphoproliferative disorder resembling lymphoma |
|
|
What cancers are of concern following transplant
|
30x increased risk of skin cancers (esp SCC)
Women should be screened for cervical and breasr cancers |
|
|
What monitoring should occur pre and post transplant
|
Cancers
Osteoporosis Vaccinations Cardiovascular risk factors (lipids, hypertension, antiplatelets) |
|
|
What are the host defences against UTIs
|
Iga, lipids, bladder mucin, Tamm-Horsfall protein, urine flushing, urine osmolarity and pH, IgA, lactobacillis and other commensals
|
|
|
What are the uti organisms
|
E.coli 85% commumity and 50% nosocomial
proteus, klebsiella, staph, strep, pseudomonas |
|
|
What are routes of infection for uti
|
Ascending: catheterisation, faecal
Blood borne. Staph and Strep |
|
|
What are the symptoms of a simple uti
|
Cystitis: dysuria, frequency, urgency with no systemic symptoms, no renal pain.
|
|
|
What are causes of complicated uti's
|
Systemic illness or recurrent uti's
Structural abnormalities in bladder, tubes, and kidneys Prostate disorder Immunosuppression |
|
|
Describe the structural abnormalities causing complicated UTI
|
Impairment of urine
1) congenital: mega ureter, posterior urethral valve, reflux, uretocoele 2) acquired: bladder diverticulum, prostatomegaly, stone, urethral stricture, tumour obstruction |
|
|
Vesico-ureteric reflux
|
Ureteric valve doesn't work due to inadequate pasdage through the bladder detrusor. Causes upper UTI
|
|
|
What is meant by functional bladder abnormality
|
Factors such as Parkinson's, "hanging on" by kids or cauda equina syndrome can result in urinary constipation, high pressure bladder and UTI. Also neurogenic bladder due to diabetes.
|
|
|
What is the risk of uti's in diabetics
|
Neuropathic bladder causing VUR and incomplete emptying, high pressure bladder and ureteric reflux. Glucose in urine promotes bacterial culturing. Decreased IgA due to depressed immunity.
|
|
|
How does pregnancy cause UTIs
|
Compression of ureters causes ureteric reflux and risk of complicated UTIs
|
|
|
What are the clinical features of nephritic syndrome
|
Heralded by malaise, fever, nausea followed by
1) Oligourea 2) Azotemia 3) Haematurea 4) Hypertension |
|
|
Describe acute postinfectious glomerulonephritis
|
Generally 3 weeks post B haemolytic Group A strep. C3 (serum complement levels fall) initially deposits in the BM causing deposition of IgG immune complexes resulting in acute inflammation, cellularity (mesangial cells and neutrophils) and nephritic syndrome and possibly crescentic (rapidly progressing) glomerulonephritis. ESRD can develop.
|
|
|
What are the principal causes of nephritis
|
1) Post infectious nephritis
2) IgA nephropathy 3) Alport syndrome (or hereditary nephritis caused by type IV collagen defect) 4) Rapidly progressing crescentc glomerulonephritis (includes Goodpasture's where anti-GBM IgG attacks the GBM and alveolar basement membrane) |
|
|
Over the last 3 months a patient's eGFR dropped from 65 to 58 mLs/min. Is this definitively chronic kidney disease. If not what else would be needed.
|
Chronic disease defined as GFR < 60 for 3 months or 3 months producing: glomerular haematuria, proteinuria, microalbuminuria, imaging or biopsy abnormalities (eg polycystic disease)
|
|
|
What are the 3 main causes of chronic kidney disease
|
1) tubulointerstital disease eg PCKD
2) glomerulonephritis (ie deposition of immune complexes) 3) vascular (hypertension, diabetes) |
|
|
What is the most significant risk posed by CKD on a person's health
|
Death from CVD (increased 20x)
|
|
|
What are the significant modifiable risk factors for developing CKD
|
1) smoking
2) diabetes 3) hypertension 4) obesity |
|
|
Once CKD is detected, what steps can be taken to slow rate of decline in renal function
|
1) quit smoking
2) treat hypertension with ACEI which decreases efferent arteriole constriction, MAP and, hence, reduces glomerular pressure and proteinuria 3) Lifestyle: weight loss, diet ,modification (reduce protein, salt and fat) |
|
|
given urine creatinine is 6mmol/L and urine protein is 900mg/L, what is the ACR. Is this value a concern. When to refer to nephrologist?
|
ACR=900/6 x 10 = 1500 mg/ 24hrs or 1.5g / 24hrs
This level is macroalbuminuria necessitating referral to nephrologist. An ACR 2.5-25 is micro (GP managed if GFR > 30) and ACR > 30 or GFR < 30 then refer |
|
|
What further investigations are required if a dipstick reveals haematuria
|
1) urine microscopy to determine origin of blood. Repeat between periods (ie 2 weeks) and confirm.
2) If glomerular, refer 3) If non-glomerular then spira CT. If lesion then refer to urologist. If negative then cytology x3. If positive (ie dysplastic cells) then urologist |
|
|
In stage 3 CRF, what complications are expected
|
CVD
Anaemia Osteodystrophy Restless legs Malnutrition |
|
|
A patient awaiting a cystoscopy for BPH experiences pain at the costovertebral angle, has fever, malaise and experiences painful burning urination. What is happening and how did this occur
|
Complicated UTI. Infection occurs via ascenting (catheters, VUR) or haematogenous route.
|
|
|
Describe the histology of pyelonephritis
|
IF acute, small yellow microabcesses. Interstitium and tubular lumen infiltrated with neutrophils. Tubular epithelium is necrotic
|
|
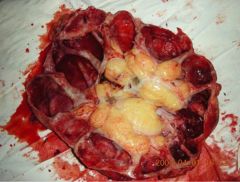
What is happening in this kidney and how did it arise
|
Pyonephrosis (puss trapped within in the pelvis) - complication of pyelonephritis
|
|
|
Explain the pathogenesis of papillary necrosis caused by infection
|
Pyelonephritis causing boggy interstitium swollen with neutrophils compresses medullary vasculature causing ischaemia and necrosis of the papilla, ultimately fibrosis
|
|
|
What is the difference between pyonephrosis and a perinephritic abcess
|
Pyonephrosis: puss trapped within the kidney (tubules, caliyces, pelvis)
Perinephric abcess: outside of the kidney |
|
|
What are the different types of pyelonephritis
|
Acute bacterial pyelonephritis
Pyonephrosis (infection of hydronephrotic, obsatructed kidney usually causing sepsis) Chronic: 1) caused by VUR resulting in reflux nephropathy. 2) Xanthogranulomatous pyelonephritis (usually from obstruction) - foamy macrophages infiltrate collecting system 3) |
|
|
What are the patterns of glomerular disease
|
Non proliferative (nephrotic, non-inflammatory)
i) minimal change GN ii) focal segmental GN iii) membranous GN Proliferative (nephritic, inflammatory) i) IgA nephropathy ii) membranoproliferative (SLE, post viral hepatitis) iii) Rapidly progressing Goodpasture's - anti basement membrane, Wegener's - anti neutrophil cytoplasmic antibodies adhee to endothelium and damage it |
|
|
List the ways in which autoregulation can fail
|
1) Perfusion pressure falls below 80mm by shock: hypovolaemic (bleeding, diarrhoea, vomiting, burns), distributive (sepsis, burns), cardiogenic (CHF), hypotensive crisis
2) >200mm hypertension |
|
|
What is the main regulator of Na homeostasis
|
RAAS: renin is secreted by the juxtaglometular apparatus in response to hyponatremia>aldosterone and angiotensin
|
|
|
What are the 3 endocrine hormones produced within the kidney
|
1) EPO
2) Renin 3) Calcitriol |
|
|
What are the 3 broad pathologies of the kidney
|
1) Glomerular disease (nephrotic: MCD, FSGS, MN, MPGN) (nephritic focal: IgA (HS, post strep), nephritic diffuse: rapidly progressing GN)
2) Tubular disease (congenital, MM or ATN) 3) Post renal obstruction: calculi, tumour, infection (pyonephritis, pyelonephritis, congenital) |
|
|
What are the aetiologies of the principal signs and symptoms of renal failure
|
Azotemia: pruritis, nausea, vomiting, lethargy, paraesthesia, cognitive and sensorymotor impairment, seizures, coma
Protein loss: oedema Acidosis: tachypnoea Endocrine: anaemia, bone pain Fluid and electrolyte imbalance: anuria, hypo/hyperkalemia, CHF |
|
|
What are the 2 main processes within the kidney
|
Glomerulus producing an ultrafiltrate based on a pressure & osmotic gradient
Tubular reabsorption of salt and water plus other substances |
|
|
Describe the main process of dialysis
|
1) Diffusion is the older process where solutes move down their concentration gradient. The concentrations of the dialysate are mostly iso with plasma except for potassium, calcium and bicarb. Glucose is added for ill patients
2) ultrafiltration where an osmotic or hydrostatic pressure gradient is created to remove water. 3) sorbents used to adsorb (chemical, ionic, complexing) substances from water |
|
|
Describe peritoneal dialysis. What is its limitation and who is not suitable.
|
A tube is inserted into the peritoneal cavity (through the parietal peritoneum and outside the visceral peritoneum) is filled with dialysate containing high concentrations of glucose to create an osmotic gradient. The glucose causes fibrosis over time, limiting its use to less than 10 years. Not suitable if fibrosed or past major abdominal surgery
|
|
|
What are the forms of dialysis
|
Incentre, satellite, home haemodyalisis
Peritoneal: continuous ambulatory PD (manual exchanges of fluid) Automated (machine does exchanges overnight). |
|
|
What are the problems with all forms of dialysis
|
50% mortality in 5 years with peritoneal dialysis. 15% overall annual mortality rate
|
|
|
What are the complications of a bifid ureter
|
Ectopic ureter - can cause incontenance
Ureteric reflux and dilatation |
|
|
Multicystic dysplastic kidney
|
Entire kidney is made up of big cysts, lack of ureter and no function
|
|
|
Polycystic kidney disease
|
Abnormal proteins form preventing signalling to filtrate flow in tubules causing abnormal proliferation of tubular cells.
In autosomal recessive form, many die at birth due to lung hypoplasia. Remember the berry aneurisms and SAH. |
|
|
Describe Wegners granulomatosis
|
1) Formation of ANCA (anti neutrophil cytoplasmic antibodies) caused by incomplete apoptosis of neutrophils.
2) antibodies bind to neutrophils causing degranulation, endothelial damage and vasculitis 3) formation of granulomas forming cutaneous and pulmonary nodules (coin lesions) 4) Nephritic syndrome (RBC casts, azotemia) caused by rapidly progressing glomerulonephritis |
|
|
Describe the
1) syndrome caused 2) pathophys 3) risk factors 4) histological changes of membranous nephropathy |
1) Causes nephrotic syndrome
2) Antibodies to unknown antigens (eg thyroid, Hep-B, bacterial) deposit in the sub-epithelial space causing complement formation triggering podocytes to release proteases. These proteases damage endothelium causing protein leakage. 3) Risk factors are infections (Hep B, syphilis, endocarditis), toxins and autoimmune disease 4) Histology: sub-epithelial antibody deposits cause thickening of the GBM in a spike (subepithelial antibody deposits) and dome (filling in) pattern. A granular pattern appears on immunohistochemistry |
|
|
Describe the
1) syndrome caused 2) pathophys 3) risk factors 4) histological changes of membranoproliferative glomerulonephritis |
1) Nephrotic syndrome
2) Type 1: Circulating antibodies form subendothelial deposits causing increase in the classical complement pathway. The excess complement causes a mesangial reaction (proliferation and processes splitting "tram tracks" within the GBM), damage to the endothelium and thickening of the GBM 3) Risk factors are factor H deficiency or C3 abnormality preventing its breakdown, SLE, Hep B, bacteria;l infections, |
|
|
Describe the
1) syndrome caused 2) pathophys 3) risk factors 4) histological changes of poststreptococcal glomerulonephritis |
1) nephritic syndrome with fever, malaise and nausea, 1-3 weeks following a beta haemolytic GAS infection
2) Antibodies against strep antigen are trapped within the glomerulus as immune complexes together with C3. A mesangial reaction occurs, together with neutrophil infiltration. 3) Risk factors: infection of pharynx or skin of nephritogenic group A Strep. Other infections including Hep B and C, measles, mumps, staph and strep can cause a symilar response 4) Hypercellularity with mesangial cells and neutrophils, formation of crescents (parietal epithelial cells, fibroblasts in the Bowman's space) and a granular pattern onf immunofluorescence |
|
|
Describe the
1) syndrome caused 2) pathophys 3) risk factors 4) histological changes of IgA nephropathy |
1) Nephritic syndrome 1-2 days following URTI
2) Inadequate clearance of IgA results in high levels nad deposition in the mesangium, causing mesangial reaction, complement activation and inflammation resulting in hypercellularity and rapidly progressive glomerulonephritis and Henoch-Schonlein purpura 3) risk factors: susceptible children and young adults 1-2 days following an URTI 4) Histology: hypercellularity of mesangium with crescent formation. Mesangial infiltration of IgA shown on immunofluorescence |
|
|
What are the three broad types of crescentic glomerulonephritis
|
1) Anti GBM (idiopathic and Goodpastures)
2) Immune complex mediated (post-infectious, IgA, SLE) 3) ANCA: Wegeners |
|
|
What is VUR
|
Retrograde urine flow along the ureters caused by
1) Primary: insufficient submucosal length at the vesicoueteral junction 2) Secondary: neurogenic bladder, meatal stenosis, posterior urethral valve |
|
|
What are the features of acute pyelonephritis? How is it different in diabetics?
|
1) Suppritive necrosis and abcess formation within the parenchyma. Infiltration of neutrophils into tubules resulting in white cell casts. The pelvis fills with puss due to obstruction, resulting in pyonephrosis
2) Diabetics get papillary necrosis (ischaemic and supprative necrosis of the papillae) |
|
|
What are the risk factors for pyelonephritis
|
1) Age and sex (females up to 40YO)
2) Urinary obstruction by VUR, enlarged prostate, tumour 3) Pregnancy 4) Immunosuppression 5) Sepsis 6) Catheterisation |

