![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
109 Cards in this Set
- Front
- Back
|
Three weeks after a meal at the Trucker's Cafe, a 28 year old man develops malaise, fatigue, and loss of appetite. Mild scleral icterus. AST 62, ALT 58, total bili 3.9, direct bili 2.8. Symptoms abate over the next 3 weeks. The cafe is closed by the health department. What serologic test will be positive in this patient
|
IgM anti-HAV. This man developed a mild, self-limited liver disease after a meal at a restaurant. He most likely developed HAV infection by consumption of contaminated food or water. The presence of IgM anti-HAV indicates recent infection. The IgM antibody is replaced within a few months by IgG antibodies, to give lifelong immunity to reinfection. The incubation period for HAV infection is short, and the illness is short and mild, with no significant tendency to develop chronic hepatitis. The most common mode of infection for HAV is via the fecal-oral route
|
|
|
41 year old woman who works as a tatto artist has had increasing malaise and nausea for the past 2 weeks. Icterus and mild right upper quadrant tenderness. AST 79, ALT 85, total bili 3.3, direct bili 2.5. Continues to have malaise for the next year. Biopsy shows minimal hepatocyte necrosis, mild steatosis, and minimal portal bridging fibrosis. An infection with what virus is most likely to produce these findings
|
HCV. Necrosis with portal bridging suggests chronic hepatitis. Mild steatosis is seen in HCV infection. The incidence of chronic hepatitis is highest with HCV infection. More than 50% of those infected with this virus develop chronic hepatitis, and many cases progress to cirrhosis. This is in part because the IgG antibodies against HCV that develop after acute infection are not protective
|
|
|
17 year old woman gives birth to a term infant after an uncomplicated pregnancy. The infant does well for three weeks, but then begins to have abdominal enlargement, light colored stools, and dark urine. The infact is icteric. Hepatomegaly, but no splenomegaly or lymphadenopathy. AST 101, ALT 112, glucose 81, creatinine 0.4. Biopsy show lobular disarray with focal hepatocyte necrosis, giant cell transformation, chelestasis, portal mononuclear cell infiltrates, Kupffer cell hyperplasia, and extramedullary hematopoiesis. The infant recovers in 1 month, and by the age of 1 year all laboratory findings are normal. Diagnosis?
|
Idiopathic neonatal hepatitis. Neonatal hepatitis is most often idiopathic, and most infants recover without specific therapy. Some cases are caused by alpha1-antitrypsin deficiency, and some are due to extrahepatic biliary atresia. However, patients with extrahepatic biliary atresia require surgery to anastomose extrahepatic ducts and prevent progressive liver damage.
|
|
|
Patients with what disease will have hydrops and icterus at birth because of maternal IgG antibody directed at fetal RBCs, leading to hemolysis
|
Erythroblastosis fetalis
|
|
|
What disease is an inborn error of metabolism in which deficiency of a certain enzyme damages cells of the kidney, liver, and brain; there is hepatomegaly, splenomegaly, hypoglycemia, and eventual cirrhosis
|
Galactosemia. The deficient enzyme is galactose 1-phosphate uridylyl transferase
|
|
|
Primary biliary cirrhosis affects what age group
|
Adults
|
|
|
What disease results from deficiency of glucose-6-phosphatase, and affected infants develop hypoglycemia, lactic acidosis, hyperuricemia, and hyperlipidemia
|
Von Gierkel disease
|
|
|
48 year old man has noticed increasing abdominal girth and yellowish color to his skin over the past 5 months. Scleral icterus and generalized jaundice. Abdomen is distended, and a fluid wave is present. Total bili 5.2, direct bili 4.2, AST 380, ALT 158, Alk Phos 95, total protein 6.4, albumin 2.2. PT 18 sec, PTT 30 sec. Blood ammonia 105. Diagnosis
|
Alcoholic liver disease. This patient has liver cell injury (indicated by elevated transaminase levels), some loss of liver function (indicated by the abnormal PT time), and cholestasis. These findings are not specific for a given type of liver injury. However, an AST level that is higher than the ALT level is characterisitc of liver cell injury associated with chronic alcoholism. In this patient, the disease is decompensating, as evidenced by the elevated blood ammonia level.
|
|
|
Choledocholithiasis results in what abnormal lab values
|
Conjugated hyperbilirubinemia, but without the high ammonia level that is evidence of liver failure
|
|
|
What lab value is characteristic of primary biliary cirrhosis
|
A very high alkaline phosphatase level
|
|
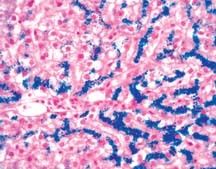
A 44 year old man has developed increasing arthritis pain, swelling of the feet, and reduced exercise tolerance over the past 3 years. He has smoked for 20 years. Glucose 201, creatinine 1.1, ferritin 893. CXR bilateral pleural effusions, pulmonary edema, and cardiomegaly. Liver biopsy shown. Diagnosis?
|
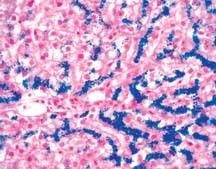
This patient has clinical, histologic, and laboratory features of genetic hemochromatosis. In this condition, iron overload occurs because of excessive absorption of dietary iron. The absorbed iron is deposited in many tissues, including the heart, pancreas, and liver, giving rise to heart failure, diabetes, and cirrhosis. It appears blue with Prussian blue stain, as seen in this figure. High serum ferritin concentration is an indicator of a vast increase in body iron. Genetic hemochromatosis is an autosomal recessive condition; hence, siblings are at risk of developing the same disease
|
|
|
12 year old boy with Down syndrome who lives in a residential care facility with other special needs children is brought in because of listnessless, malaise, and mild fever of 3 days duration. Dark urine is observed by one of the caregivers. Mild scleral icterus and mild right upper quadrant tenderness
Total protein 6.5 Albumin 4.4 AST 337 ALT 338 Alk Phos 178 Total bili 5.0 Direct bili 3.1 HBsAg negative Anti-HBs positive Anti- HBc positive Anti-HBc, IgM negative Anti-HAV, IgM positive Anti-HAV, IgG positive Anti-HCV negative Anti HDV negative Diagnosis? |
Acute HAV infection. This patient has a short history of jaundice, with evidence of acute hepatitis and significant transaminase elevations. The serologic findings support a diagnosis of acute HAV, because he has anti-HAV IgM antibodies. This indicates recent infection, because these antibodies form during recovery. In contrast, the patient has antibodies against HBcAg that do not type as IgM. By inference, he has IgG antibodies against HBcAg, which are indicative of previous HBV infection. Absence of HBsAg supports this conclusion. HAV infections are acquired via the fecal-oral route and are likely to occur in institutions such as those for mentally retarded children
|
|
|
52 year old woman has experienced malaise that has worsened during the past year. Mild scleral icterus. No ascites or splenomegaly. Positive IgG anti HCV and HCV RNA, negative anti-HAV, HBsAg, ANA, antimitochondrial antibody. AST 88, ALT 94. Condition remains stable for months. What will her liver look like morphologically
|
Piecemeal hepatocellular necrosis. This patient has evidence of HCV infection and has had symptoms of liver disease for 1 year. Clinically, she has chronic hepatitis (>6 months) that may have followed an asymptomatic acute HCV infection. The anti-HCV IgG antibody is not protective. This is supported by continued HCV viremia. Approximately 85% of cases of HCV progress to chronic hepatitis, but fulminant hepatitis is uncommon. Chronic hepatitis is characterized by necrosis of hepatocytes at the interface between portal tracts and the liver lobule. This eventually leads to bridging necrosis and, finally, to cirrhosis with portal bridging fibrosis and nodular regeneration. At this time, however, the patient has no signs or symptoms of cirrhosis
|
|
|
Concentric bile duct fibrosis occurs in what disease, which may be idiopathic or, more commonly, is associated with inflammatory bowel disease
|
Sclerosing cholangitis
|
|
|
Copper deposition is characteristic of what diease, which may be associated with chronic hepatitis and cirrhosis, but is not related to the common HCV infection
|
Wilson disease
|
|
|
Granulomatous bile duct destruction suggests what disease
|
Primary biliary cirrhosis
|
|
|
What syndrome in hepatic venous thrombosis leads to hepatic enlargement and necrosis as well as to ascities
|
Budd-Chiari syndrome
|
|
|
Microvesicular steatosis of the liver is characteristic of what two conditions
|
Acute fatty liver of pregnancy and Reye syndrome in children
|
|
|
36 year old woman has become increasingly icteric for 1 month. In the past 3 years, she has had several bouts of colicky, midabdominal pain. Generalized jaundice with scleral icterus. Tenderness in the right upper quadrant, and the liver span is normal. Liver biopsy shows bile duct proliferation and intracanalicular bile stasis but no inflammation or hepatocyte necrosis. What abnormal lab value will be present
|
Elevated alkaline phosphatase level. The findings suggest obstructive jaundice from biliary tract disease (eg gallstones). Elevation of the serum alkaline phosphatase level is characteristic of colestasis. The alkaline phosphatase comes from bile duct epithelium and hepatocyte canalicular membrane.
|
|
|
Increased antimitochondrial antibody titer, which eventually leads to bile duct destruction, is characteristic of what disease
|
Primary biliary cirrhosis
|
|
|
Most cases of active HCV infection are accompanied with what liver morphology
|
Increased inflammation with fibrosis
|
|
|
In obstructive biliary tract disease, which bilirubin value will be elevated
|
The direct bilirubin level
|
|
|
Increasing blood ammonia level is indicative of what
|
Worsening liver failure. When hepatic failure is sufficent to cause hyperammonemia, mental obtundation is seen
|
|
|
56 year old man from China has experienced fatigue and 10kg weight loss over the past 3 months. No remarkable physical findings. Positive HBsAg, negative anti-HCV and anti-HAV. CT shows 10cm solid mass in the left lobe of a nodular liver. Liver biopsy indicates hepatocellular carcinoma. What mechanism caused this lesion
|
Repeated cycles of liver cell necrosis and regeneration caused by HBV infection. There is a long-term risk of hepatocellular carcinoma in patients infected with HBV. This infection is more common (often from vertical transmission) in Asia than in North America and Europe, and it accounts for more cases of primary liver cancer worldwide than other causes such as chronic alcoholism. HBV does not encode any oncogene, nor does it integrate next to a known oncogene, such as C-MYC. Most likely, neoplastic transformation occurs because HBV induces repeated cycles of liver cell death and regeneration. This increases the risk of accumulating mutations during several rounds of cell division. Hepatic carcinomas do not develop from adenomas
|
|
|
Infection with the liver fluke Clonorchis sinensis predisposes to what disease
|
Bile duct carcinoma
|
|
|
42 year old woman has had fever, chills, and bouts of colicky right upper quadrant pain for the past week. Skin is icteric and there is scleral icterus. Total bili 7.1, direct bili 6.7. Ultrasound shows cholelithiasis, dilation of the common bile duct, and two cystic lesions, .8cm and 1.5cm, in the right lobe of the liver. What infectious agent produced these findings
|
Escherichia coli. This patient has a history of gallstones and has developed an ascending cholangitis caused by E. coli. These bacteria reach the liver by ascending the biliary tree. Obstruction from lithiasis is the most common risk factor. Development of cystic lesions in the right lobe of the liver suggests that the patient has developed liver abscess
|
|
|
Clonorchis sinensis is a risk factor for what disease
|
Biliary tract cancer
|
|
|
Seven years ago, a 30 year old man saw a physican because he had experienced malaise, fever, and jaundice for 2 weeks. There were needle tracks in the L antecubital fossa and a murmur of mitral regurgitation. Positive HBsAG, HBV DNA, anti-HBc IgG. Two year later he was seen at the ER for hematemesis and ascites. Serologic tests were the same as previously. He was treated with sclerotherapy for esophageal varices. Five years later he now sees the physican for 5kg weight loss, worsening ab pain, and rapid enlargement of the ab over the past month. Has increased liver span. What laboratory test will most likely be diagnostic of this last phase of his disease
|
Elevated serum alpha-fetoprotein level. This IV drug abuser developed chronic HBV infection, as evidenced by the persistence of HBsAG, HBV DNA, and IgG anti-HBc. Up to 80-90% of persons with a history of IV drug abuse are found to have serologic evidence of HBV or HCV infection. Ruptured varices and ascites suggest that this patient subsequently developed cirrhosis and portal hypertension. His final presentation of weight loss and rapid enlargement of the ab suggests that a hepatocellular carcinoma has developed. In most cases, this can be confirmed by an elevated alpha-fetoprotein level. Other test findings, including prolonged PT time, increased ALT, and increased ferritin are all indicative of chronic liver disease. Any mass lesion is associated with elevated alkaline phosphatase. Increased ammonia indicates liver failure
|
|
|
Over the past 4 days, a previously healthy 38 year old woman has become increasingly obtunded. Scleral icterus. Afebrile, BP 110/55. PT 38sec, ALT 1854, AST 1621, albumin 1.8, total protein 4.8. What additional abnormal lab value is likely to be present in this patient
|
Increased ammonia level. The patient's history points to acute fulminant hepatitis with massive hepatic necrosis. The loss of hepatic function from destruction of 80-90% of the liver results in hyperammonemia from the defective hepatocyte urea cycle.
|
|
|
What does an elevated alkaline phosphatase level suggest
|
Extrahepatic or intrahepatic biliary obstruction
|
|
|
An elevated amylase level suggests what
|
Pancreatitis
|
|
|
58 year old woman has experienced gradually increasing malaise, icterus, and loss of appetite for the past 6 months. Generalized jaundice and scleral icterus. Mild right upper quadrant tenderness; liver span normal. Total bili 7.8, AST 190, ALT 220, alk phos 26. Liver biopsy shows piecemeal necrosis of hepatocytes at the limiting plate, with portal bridging fibrosis and a mononuclear infiltrate in the portal tracts. Diagnosis?
|
HCV infection. This patient has clinical evidence of liver disease that has persisted for 6 months, and histologic evidence of hepatic necrosis with portal inflammation and fibrosis. These are features of chronic hepatitis. Of all the hepatitis viruses, HCV is most likely to produce chronic disease
|
|
|
Hepatic congestion with right-sided heart failure produces what liver morphology
|
Centrilobular necrosis, but not portal fibrosis
|
|
|
Choledocholithiasis leads to what liver morphology and lab values
|
Extrahepatic biliary obstruction and an elevated alkaline phosphatase level. It is not likely to produce hepatocellular necrosis
|
|
|
How will the liver cells appear in hemochromatosis
|
They will show prominent accumulation of golden-brown hemosiderin pigment
|
|
|
Metastases that produce focal obstruction in the liver will have what abnormal lab values
|
Increased alkaline phosphatase level but not the bilirubin concentration
|
|
|
Sclerosing cholangitis leads to what bile duct morphology
|
Inflammation and obliterative fibrosis
|
|
|
53 year old man comes to ER because of marked hematemesis that has continued for 3 hours. 35.9C, pulse 112, resp 26, BP 90/45. Distended abdomen with a fluid wave, and the spleen tip is palpable. What liver disease is most likely present in this patient
|
Cirrhosis. The findings point to portal hypertension with bleeding esophageal varices. Cirrhosis alters hepatic blood flow to produce portal hypertension
|
|
|
40 year old woman is found to have HBsAg. She feels fine. No physical findings. Lab values all normal. Negative IgM anti-HAV, anti-HBc, anti-HCV. Repeat testing 6 months later yields the same results. How is this possible
|
The patient is probably a chronic carrier from vertical transmission. Persistence of HBsAg in serum for 6 months or more after initial infection denotes a carrier state. Worldwide, most persons with a chronic carrier state for HBV acquired this infection in utero or at birth. Only 1-10% of adult HBV infections yield a chronic carrier state. The carrier state is stable in most persons, although carriers become a reservoir for infection in others
|
|
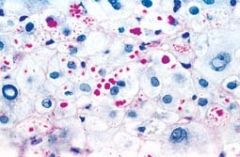
28 year old man has had increasing shortness of breath for the past year. Afebrile and normotensive. Breath sounds are decreased in all lung fields. Marked icterus as a neonate, but has been healthy since. Family history of liver disease. Biopsy stained with PAS shown above. This patient is at high risk for developing what disease
|
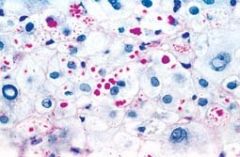
Pulmonary emphysema. The PAS positive globules in the liver seen here are characteristic of alpha1-antitrypsin (AAT) deficiency. Approximately 10% of persons with the homozygous deficiency (PiZZ phenotype) of AAT deficiency will develop significant liver disease, including neonatal hepatitis and progressive cirrhosis. Deficiency of AAT also allows unchecked action of elastases in the lung, which destroys the elastic tissue and causes emphysema
|
|
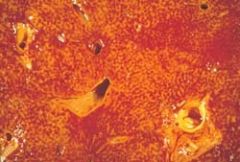
A 70 year old woman has had increasing swelling of the lower legs and difficulty breathing for the past 5 years. Irregular pulse, and there is dullness to percussion at the lung bases. The liver span is increased, and her neck veins are distended. CXR large, bilateral pleural effusions. Dies of cardiac dysrhythmia. Liver at autopsy shown. It is enlarged and tense with a blunted edge. What underlying condition caused this
|
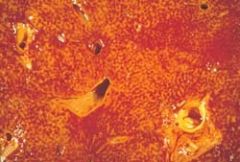
Cor pulmonale. This figure shows the classic "nutmeg" appearance of the liver caused by chronic passive congestion from right-sided heart failure. Several forms of obstructive and restrictive lung diseases can cause cor pulmonale.
|
|
|
Polyarteritis nodosa can lead to what liver pathology
|
Focal hepatic infarction
|
|
|
Chronic alcoholism results in what liver pathology
|
Hepatic steatosis, cirrhosis, or both
|
|
|
What is the most common cause of Budd-Chiari syndrome.
|
Polycythemia vera. In this disease, hepatic vein thrombosis is followed by rapid hepatic congestion. It is a rare condition.
|
|
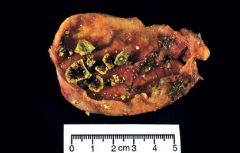
50 year old Native-American woman has had colicky right upper quadrant pain for the past week. Nausea, but no vomiting or diarrhea. Afebrile. Marked tenderness of the right upper quadrant. BMI 33. Ultrasound shows calculi within the lumen of the gallbladder, and the gallbladder wall appears thickened. Intrahepatic and extrahepatic bile ducts appear normal. Gallbladder removed and shown above. What mechanism most likely played the greatest role in development of this disease
|
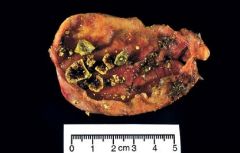
Biliary hypersecretion of cholesterol. The figure shows cholesterol gallstones. These stones are pale yellow but acquire a variegated appearance by trapping bile pigments. In comparison, pigment stones are uniformly dark. Risk factor for cholesterol stones include Native american descent, female, obesity, and increasing age. These factors cause secretion of bile that is supersaturated in cholesterol.
|
|
|
Patients with RBC hemolysis develop what type of gallbladder stones, whether the hemolyis is antibody-mediated (autoimmune hemolytic anemia) or whether it is caused by intrinsic RBC abnormalities (hemoglobinopathies such as sickle cell anemia)
|
Pigment stones
|
|
|
Infection of the biliary tract (E coli, Ascaris worms, liver flukes) can lead to what type of gallstones
|
There is increased release of Beta-glucuronidases that hydrolyze bilirubin glucuronides, favoring pigment stone formation
|
|
|
Severe ileal dysfunction, as occurs in Crohn disease, can predispose to what type of Gallstones
|
Pigment stones
|
|
|
Renal failure with phosphate retention can be a cause of secondary hyperparathyroidism with hypercalcemia, which increases the risk of what type of gallstones
|
Mixed stones
|
|
|
Does diet play a direct role in gallstone formation
|
Fatty foods may trigger biliary colic, but diet does not play a direct role in stone formation
|
|
|
60 year old man with a 30 year history of drinking alcohol to excess sees the physician because of hematemesis. Ascites, mild jaundice, enlarged spleen. Gynecomastia, spider telangiectasias of the skin, and testicular atrophy. Prominent hemorrhoids and a normal-sized prostate. Dilated, bleeding blood vessels in the esophagus
Na 136 K 6 Cl 92 CO2 23 Total prot 5.8 Alb 3.4 AST 137 ALT 108 Alk phos 181 Total bili 5.4 Direct bili 3.0 PT 20 sec Hct 25% WBC count 12,790 What morphologic changes will be found in the liver at autopsy |
Liver is diffusely nodular with small, uniform nodules and microscopically shows diffuse fibrosis encircling nodules of regenerative hepatocytes; liver cells contain fat globules. Portal fibrosis with nodular hepatocyte regeneration and steatosis are typical features of chronic alcohol abuse. Spider telangiectasis (angiomas) refer to vascular lesions in the skin characterized by a central, pulsating, dilated arteriole from which small vessels radiate. These lesions result from hyperestrogenism (which also contributes to the testicular atrophy). The failing liver is unable to metabolize estrogens normally. Therefore, spider angiomas are a manifestation of hepatic failure. Ascites, splenomegaly, hemorrhoids, and esophageal varices are all related to portal hypertension and the resultant collateral venous congestion and dilation
|
|
|
In what disease is the liver shrunken with a wrinkled capsular surface and microscopically shows massive irregular areas of necrosis without any obvious pattern
|
Acute fulminant hepatitis
|
|
|
In what disease is the liver diffusely nodular with small, uniform nodules and microscopically shows diffuse fibrosis encircling regenerative nodules; liver cells contain PAS-positive, globular cytoplasmic inclusions
|
Alpha1-antitrypsin deficiency
|
|
|
In what disease is the liver markedly enlarged, yellow, and greasy and microscopically shows preservation of the architecture and marked fatty change
|
Alcoholic fatty liver
|
|
|
In what disease is the liver diffusely nodular and intensely green with small, uniform nodules and microscopically shows prominent bile stasis and fibrous bridging between portal areas
|
Biliary cirrhosis
|
|
|
19 year old mother notices that her 3 week old neonate has increasing jaundice. Uncomplicated pregnancy. Generalized jaundice, hepatomegaly, acholic stool. Total bili 10.1, AST 123, ALT 140, glucose 77, creatinine 0.4. Liver biopsy shows marked proliferation of bile ducts, portal tract edema and fibrosis, and extensive intrahepatic and canalicular bile stasis. Infant develops progressively worsening jaundice and dies of liver failure at 9 months age. Diagnosis?
|
Biliary atresia. Extrahepatic biliary atresia is a rare condition in which some or all of the bile ducts are destroyed. If the disease spares a large enough bile duct to anastomose around the obstruction, the problem may be correctable. However, in many cases, such as this, obstruction of bile ducts occurs above the porta hepatis and the only option for treatment is liver transplantation
|
|
|
What is a congenital lesion that produces dilations of the common bile duct, and may cause biliary colic in children
|
A choledochal cyst
|
|
|
Over the past 6 months, a 68 year old woman has become increasingly tired and reports 3kg weight loss without dieting. Stool sample positive for occult blood. Protein 6.1, albumin 3.9, total bili 1.1, AST 38, ALT 44, Alk phos 294, glucose 70, creatinine 0.9. CBC hemoglobin 8.9, hct 26.7%, MCV 75, platelets 198,400, WBC 5520. PT 13sec, PTT 25sec. Negative Hep A,B,C. CXR normal. Diagnosis?
|
Metastatic adenocarcinoma. An elevated alkaline phosphatase level suggests obstruction of the biliary tract, but this case must be focal, because the bilirubin is not elevated. The microcytic anemia and the blood in the stool suggest gastrointestinal tract hemorrhage, and a colonic adenocarcinoma should be suspected. Hepatic metastases from colon cancer are common. They appear as multiple masses within the hepatic parenchyma
|
|
|
What syndrome predisposes to thrombosis with venous obstruction, in which case hepatic enzyme levels should be high, and PT times should be prolonged
|
Antiphospholipid syndrome
|
|
|
Ascending cholangitis is typically caused by bacteria such as E coli or Klebsiella, and presents how
|
Acutely with fever, chills, jaundice, and abdominal pain
|
|
|
In patients with gallstones, a subset have decreased urobilinogen excretion in urine and increased fecal bile acids. Despite normal values for serum bilirubin, albumin, haptoglobin, and calcium, many of these patients have a macrocytic anemia. Ab CT shows the liver and spleen are normal. What condition is most likely present in this subset of patients
|
Crohn disease. These findings indicate decreased bile acid and urobilinogen reabsorption in the ileum, which reduces the enterohepatic circulation and favors the formation of pigment stones. Crohn disease often involves the terminal ileum, and this also disturbs absorption of vitamin B12 complexed with intrinsic factor, leading to macrocytic anemia.
|
|
|
61 year old man has has ascites for the past year. Paracentesis removes 1 L of slightly cloudy, serosanguineous fluid. Firm, nodular liver. Positive serum HBsAg and anti-HBc. Markedly elevated alpha-fetoprotein level. What hepatic lesion is most likely present
|
Hepatocellular carcinoma. The elevated alpha-fetoprotein (AFP) level is most suggestive of hepatocellular carcinoma, which arises in cirrhosis. The presence of HBsAg and anti-HBc indicates chronic infection with HBV, which gave rise to cirrhosis and, ultimately, to liver cell cancer.
|
|
|
50 year old man has massive hematemesis. History of chronic alcoholism but he stopped drinking ethanol 10 years ago. Takes no meds. Afebrile, hypotensive, pale. Ab not enlarged, no tenderness. Liver span normal. Hep A,B,C negative. Hct 19%. What will this patient's liver look like morphologically
|
Portal bridging fibrosis with nodular hepatocyte regeneration. Portal bridging fibrosis and nodular hepatocyte regeneration are features of cirrhosis. The massive upper gastrointestinal bleeding suggests esophageal varices as a consequence of portal hypertension from cirrhosis. If the patient is currently not drinking alcohol, no fatty change (steatosis) will be present. The architectural changes of cirrhosis persist for decades after cirrhosis develops.
|
|
|
Concentric "onion skin" bile duct fibrosis is seen in what disease
|
Primary sclerosing cholangitis, which may be idiopathic or may appear is association with inflammatory bowel disease
|
|
|
Massive hepatocellular necrosis may occur rarely as a complication of what two things
|
HAV infection or ingestion of massive amounts of acetaminophen
|
|
|
44 year old woman has noticed increasingly severe generalized pruritus for the past 8 months. Serum levels of alkaline phosphatase and cholesterol are elevated; antimitochondrial antibody titer is elevated, but ANAs are not present. Total bili concentration increases. Liver biopsy shows nonsuppurative, granulomatous destruction of medium-sized bile ducts. Diagnosis?
|
Primary biliary cirrhosis. The prescence of obstructive jaundice, granulomatous destruction of bile ducts, and elevated titers of antimitochondrial antibodies is characteristic of primary biliary cirrhosis. This is an autoimmune condition that may be associated with other autoimmune phenomena (scleroderma, thryoiditis, glomerulonephritis). Cirrhosis is a late complication of this disease that can persist for 20 years or more
|
|
|
36 year old woman is in the sixth month of her first pregnancy, but she is unsure of her dates because she was taking oral contraceptives at the time she became pregnant. She experiences sudden onset of severe ab pain. Afebrile and normotensive. Right upper quadrant tenderness on palpation. Ultrasound shows well-circumscribed, 7cm subcapsular hepatic mass. Paracentesis yields bloody fluid. At laparotomy, the mass in the right lower lobe, which has ruptured through the liver capsule, is removed. The remaining liver parenchyma appears to be of uniform consistency, and the liver capsule is otherwise smooth. Diagnosis?
|
Hepatic adenoma. This patient has a circumscribed mass in the liver, suggesting a benign tumor such as hepatic adenoma. These tumors, which may develop in young women who have used oral contraceptives, can enlarge and rupture from estrogenic stimulation during pregnancy.
|
|
|
What are choledochal cysts of the biliary tract
|
Rare embryonic remnants that typically become symptomatic in childhood, along with biliary colic
|
|
|
In what age group are hepatoblastomas found
|
These are rare liver neoplasms found in children
|
|
|
19 year old woman is bothered by a tremor at rest, which becomes progressively worse over the next 6 months. Begins acting strangely and is diagnosed with an acute psychosis. Slight scleral icterus. Slit-lamp examination shows corneal Kayser-Fleischer rings. Total protein 5.9, albumin 3.1 total bili 4.9, direct bili 3.1, AST 128, ALT 157, Alk phos 56. What additional serologic test finding will most likely be reported in this patient
|
Decreased serum ceruloplasmin level. This patient has Wilson disease, an inheritied disorder in which toxic levels of copper accumulate in tissues, particulary the brain, eye, and liver. The gene for Wilson disease encodes a copper-transporting ATPase in the hepatocytes. With mutations in this gene, copper cannot be secreted into plasma. Ceruloplasmin is an alpha2-globulin that carries copper in plasma. Because copper cannot be secreted into plasma, ceruloplasmin levels are low
|
|
|
55 year old man has developed ab pain and jaundice over a period of several weeks. Right upper quadrant pain but no abdominal distension. Ab CT shows a markedly thickened gallbladder wall. Cholecystectomy shows a slightly enlarged gallbladder containing a fungating, 4x7cm firm, lobulated, tan mass. What is most likely associated with this mass
|
Cholelithiasis. Almost all gallbladder carcinomas are adenocarcinomas, and most are found in gallbladders that also contain gallstones
|
|
|
47 year old man has experienced intermittent upper ab pain for several weeks. Total protein 7.3, alb 5.2, total bili 7.5, direct bili 6.8, AST 35, ALT 40, Alk phos 207. Liver biopsy shows intracanalicular cholestasis in the centrilobular regions, swollen liver cells, and portal tract edema. No necrosis and no fibrosis. No increase in stainable iron. Diagnosis
|
Choledocholithiasis. The intermittent upper ab pain is a nonspecific symptom that often occurs in patients with gallstones. When a stone slips into the common bile duct, intrahepatic cholestasis occurs. This explains the conjugated hyperbilirubinemia and the increased alkaline phosphatase level
|
|
|
42 year old woman has had generalized pruritus for several months. Not relieved by application of topical corticosteroid-containing creams. Total bili 1.8, direct bili 1.2, AST 55, ALT 58, Alk phos 289, total prot 6.8, alb 3.4, total cholesterol 344. What serologic test will most likely be positive in this patient
|
Antimitochondrial antibody. This patient has findings characteristic of primary biliary cirrhosis, which has a peak incidence in middle-aged women. Later in the disease, jaundice may increase with progressive destruction of intrahepatic bile ducts. Positivity for antimitochondrial antibody is a characteristic finding in most cases
|
|
|
In what disease is anti-parietal cell antibody found
|
Chronic atrophic gastritis, and gives rise to pernicious anemia
|
|
|
Anticentromeric antibody typically occurs in what disease
|
Systemic sclerosis
|
|
|
Anti-ribonucleoprotein antibodies can occur in what diseases
|
A variety of connective tissue diseases, including mixed connective tissue disease
|
|
|
Anti-double-stranded DNA antibodies are diagnostic of what disease
|
Systemic lupus erythematosus
|
|
|
35 year old woman consults her physician because she has noticed an increasing yellowish hue to her skin for the past week. No ab pain or tenderness, liver span is normal. Hgb 11.7, hct 35.2, MCV 98, platelet 207,600, WBC 6360, alb 3.5, total prot 5.5, total bili 8.7, direct bili 0.6, AST 39, ALT 24, Alk phos 35. Diagnosis?
|
Hemolytic anemia. This patient has an unconjugated hyperbilirubinemia, which can result from hemolysis. With increased RBC destruction, there is more bilirubin than can be conjugated by the hepatocytes.
|
|
|
Obstructive jaundice with biliary tract lithiasis results in an increase of what type of bilirubin
|
Increase in conjugated bilirubin
|
|
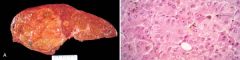
41 year old woman experienced increasing malaise and a 10kg weight loss in the last year of her life. She became increasingly obtunded, lapsed into a coma, and died. Liver at autopsy shown. Ingestion of what substance likely played a role in the development of this condition
|
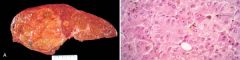
A hepatoxin such as Aflatoxin. Aflatoxin is the product of the fungus Aspergillus flavus, which grows on moldy peanuts. Aflatoxin can be carcinogenic, leading to hepatocellular carcinoma, as shown in the figure
|
|
|
Ingestion of raw oysters can result in infection with which hepatitis virus
|
HAV
|
|
|
Aspirin has been implicated in causing what syndrome in children, which results in extensive microvesicular steatosis of the liver
|
Reye syndrome
|
|
|
Nitrites have been linked with cancers in what part of the body
|
Cancers in the upper gastrointestinal tract
|
|
|
Ingestion of large amounts of acetaminophen leads to what liver pathology
|
Hepatocellular necrosis
|
|
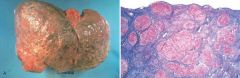
56 year old man has had increasing ab enlargement for 6 months. During the past 2 days, he developed a high fever. 38.5C. Ab enlarged, diffusely tender, and there is a fluid wave. Paracentesis yields 500mL of cloudy yellowish fluid. Cell count 532/uL with 98% neutrophils and 2% mononuclear cells. Escherichia coli present. Patient dies, liver shown above. What underlying condition most likely caused these findings
|
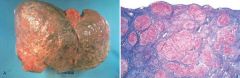
Chronic alcoholism. The diffuse nodularity with depressed scars between the nodules is characteristic of cirrhosis, which led to his ascites complicated by spontaneous bacterial peritonitis and septicemia. The most common cause of cirrhosis in the Western world is alcohol abuse
|
|
|
In what liver disease is there portal fibrosis but not much nodular regeneration, so the liver is green and hard and has a finely granular surface
|
Primary sclerosing cholangitis
|
|
|
41 year old man has experienced progressive fatigue, pruritus, and icterus for several months. A colectomy was performed 5 years ago for treatment of ulcerative colitis. Now has generalized jaundice. Ab not distended; no ab pain and no masses. Alk phos 285. Cholangiography shows widespread obliteration of intrahepatic bile ducts and a beaded apperance in the remaining ducts. What morphologic feature will most likely be present in this patient's liver
|
Concentric "onion skin" bile duct fibrosis. This patient has primary sclerosing cholangitis; ulcerative colitis coexists in 70% of these cases. The major targets in primary sclerosing cholangitis are intrahepatic bile ducts. They undergo a destructive cholangitis that leads eventually to periductal fibrosis and cholestatic jaundice. Eventually, cirrhosis and liver failure can occur.
|
|
|
Granulomatous bile duct destruction occurs in what disease
|
Primary biliary cirrhosis
|
|
|
Portal bridging fibrosis with nodular regeneration of the liver defines what disease
|
Cirrhosis
|
|
|
31 year old woman has experienced increasing malaise for the past 4 months. Physical exam reveals no remarkable findings. Total protein 6.4, albu 3.6, total bili 1.4, AST 67, ALT 91, alk phos 99. Negative hep A,B,C. Positive ANA and anti-smooth muscle antibody, rheumatoid factor level is elevated. Liver biopsy shows minimal portal mononuclear cell infiltrates with minimal piecemeal necrosis and mild portal fibrosis. Diagnosis?
|
Autoimmune hepatitis, a chronic liver disease of unknown cause in which antibodies to hepatocyte structural components cause progressive necrosis of hepatocytes, leading to cirrhosis and liver failure. Patients tend to improve with glucocorticoid therapy
|
|
|
In HBV infection, there is an association between the carrier state and what mode of transmission of HBV
|
Vertical transmission during childbirth. HBV infection from blood transfusion is rare because of screening of blood products. Transmission of HBV via sexual contact is not common and induces a carrier state in a minority of cases; in most cases, an immune response is elicited. The risk of acquiring HBV through needlestick injury is 1-6%. In regions where HBV is endemic, vertical transmission produces a carrier rate of 90-95%. Development of viral hepatitis requires an immune response against virus-infected cells. In immunocompetent persons, HBV induces T cells specific for HBsAg that cause apoptosis of infected liver cells. During the neonatal period, immune responses are not fully developed; hence, hepatitis does not occur. The high carrier rate is medically significant, because it increase the risk of hepatocellular carcinomas 200-fold. In populations with a high carrier rate, coexistent cirrhosis may be absent in up to 50% of patients. In contrast, in Western countries, where HBV is not endemic, cirrhosis is present in 80-90% of patients who develop liver cancer
|
|
|
On the day of the final exam in anatomy, a 26 year old med student notices her sclerae have a slight yellowish color. She has never had a major illness. No major physical findings. Total prot 7.9, alb 4.8, AST 48, ALT 19, Alk phos 32, total bili 4.9, direct bili 0.8. Scleral icterus resolves within 2 days. Diagnosis?
|
Gilbert syndrome. This patient has Gilbert syndrome, which results from decreased levels of uridine diphosphate glucuronosyl-transferase (UGT). Up to 7% of persons in the general population may have decreased levels of this enzyme, and the condition is often never diagnosed. Stress may cause transient unconjugated hyperbilirubinemia to a point that scleral icturus is detectable, when the serum bilirubin reaches about 2 to 2.5 mg/dL.
|
|
|
48 year old man sees his physician because he has had nausea and colicky right upper ab pain for the past 2 days. 38.8C, WBC 11,200, 71% neut, 9% bands, 13% lymphs, 7% monos. Diagnosis?
|
Acute cholecystitis. These symptoms are typical of acute calculous cholecystitis. Hepatitis is unlikely to produce acute pain and leukocytosis
|
|
|
46 year old man has had gradually increasing abdominal distension for the past 7 months, along with decreased libido. Excessive skin pigmentation in sun-exposed areas. Ab fluid wave and modest splenomegaly. Fasting glucose 200, creatinine 0.8, ferritin 650, total prot 6.3, alb 2.2. Total bili,AST,ALT,Alk phos normal. Hgb 13.5, hct 40.6, MCV 94, platelets 200,000, WBC 6570. PT 20sec, PTT 65 sec. A mutation in what gene is most likely to explain his disease
|
HFE gene, preventing the sensing of circulating iron levels by crypt enterocytes. This patient has ascites, splenomegaly, impaired liver function, diabetes mellitus, skin pigmentation, and elevated ferritin which all point to excessive hepatic iron storage and consequent hemochromatosis. Since there are no predisposing causes for increased iron absorption, the most likely diagnosis is primary, or genetic, hemochromatosis. This disease results from a mutation in the HFE gene that encodes for an HLA class I-like molecule that binds Beta2-microglobulin. HFE is expressed on the basolateral surface of the small intestinal crypt epithelial cells, where it is complexed with transferrin receptor and senses the levels of plasma transferrin. Through this sensing mechanism, HFE regulates the levels of several other proteins such as DMT-1 that are involved in iron absorption. Mutant HFE fails to exert such an influence, thereby causing excessive iron absorption and accumulation of iron in liver and other organs, leading to hemochromatosis.
|
|
|
28 year old woman, G3P2, is in the third trimester of a previously uncomplicated pregnancy when she develops increasing lethargy with nausea, vomiting, and jaundice over a 10-day period. Generalized jaundice and scattered ecchymoses over the trunk and extremities. Fetal age 35 weeks. Total bili 5.8, AST 122, ALT 131, Alk phos 125. What histologic feature is most likely to be found in a liver biopsy specimen
|
Marked microvesicular steatosis. This patient has acute fatty liver of pregnancy, an uncommon condition of varying severity. Accumulation of small droplets of fat in hepatocytes (microvesicular steatosis) is the typical histologic finding. The condition may occur because of a defect in intramitochondrial fatty acid oxidation.
|
|
|
A study is conducted of patients who are infected with hepatis A,B,C,D,E,F, or G. A subset of patients developed antibodies but subsequently were reinfected with the same type of hepatitis virus. What virus were they infected with
|
HCV. Antibodies to hepatitis C do not confer protection against reinfection. HCV RNA remains in the circulation, despite the presence of neutralizing antibodies. In other hepatitis infections, development of IgG antibodies offers lifelong immunity. A HBV vaccine exists for this purpose
|
|
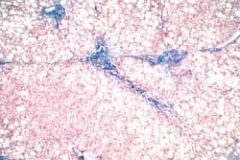
51 year old man has had increasing malaise and swelling of the lower legs for the past 4 months. Afebrile and normotensive. There is pitting edema to the knees. Ab slightly distended with a fluid wave, but there is no tenderness. Liver span is increased. Lab studies show total protein 5.0, alb 2.2, AST 65, ALT 65, Alk pho 93, total bili 1.8. Liver biopsy shown. Ingestion of what caused this illness
|
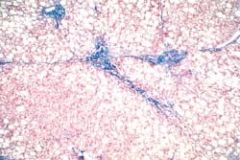
Alcohol. This patient has macrovesicular steatosis (fatty change) of the liver with early fibrosis. The most common cause of fatty liver and fibrosis is chronic alcoholism. In patients with no history of significant ethanol ingestion, a nonalcoholic steatohepatitis may be considered, with obesity, diabetes mellitus, or both, as possible causes
|
|
|
Allopurinol toxicity can cause what liver morphology
|
Granuloma formation
|
|
|
Chlorpromazine can lead to what liver pathology
|
Cholestasis
|
|
|
Ferrous sulfate ingested in excess can promote what disease
|
Hemochromatosis
|
|
|
Acetominophen ingestion in excess can cause what liver morphology
|
Centrilobular necrosis or diffuse necrosis
|
|
|
After experiencing malaise and increasing icterus for 6 weeks, a 42 year old man sees his physician. Jaundice, but no other significant findings. Negative IgM anti-HAV and anti HCV, positive HBsAg and IgM anti HbC. What will be the most likely outcome of this disease
|
Complete recovery without sequelae is most probable. The patient has serologic markers for HBV (HBsAg positive), and the detection of IgM anti-HBc indicates acute infection. Most cases of HBV infection do not progress to chronic hepatitis, but a small number of cases are complicated by fulminant hepatitis or by progression to cirrhosis. In some patients, cirrhosis progresses to hepatocellular carcinoma, but given that most patients with HBV recover, the risk of liver cancer in a specific person is very small
|
|
|
51 year old man has a lengthy history of chronic alcoholism and comes to the physician because of increasing malaise for the past year. Hospitalized 1 year ago because of upper gastrointestinal hemorrhage. Firm, nodular liver. Serum alb 2.5, PT 28sec. What additional physical exam finding is most likely to be present
|
Caput medusae. This patient has alcoholic cirrhosis with portal hypertension. Venous collateral flow can be increased in esophageal submucosal veins, producing varices, and in the ab wall, producing caput medusae
|
|
|
45 year old woman has had increasing pruritis and icterus for several months. Generalized jaundice. Total prot 6.3, alb 2.7, total bili 5.7, direct bili 4.6, AST 77, ALT 81, Alk phos 221. Liver biopsy shows destruction of portal tracts and loss of bile ducts as well as lymphocytic infiltrates. What additional lab finding is most likely to be reported
|
Positive antimitochondrial antibody. This patient has primary biliary cirrhosis, an uncommon autoimmune disorder that causes progressive intrahepatic bile duct destruction. Pruritus, conjugated hyperbilirubinemia, and increased alk phos levels are indicative of obstructive jaundice resulting from bile duct destruction. About 90% or more of patients with this disease have antimitochondrial antibodies in the serum
|
|
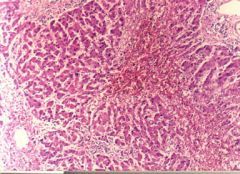
50 year old man has increasing dyspnea as a consequence of idiopathic pulmonary fibrosis, which was diagnosed 18 months ago. Elevated jugular venous pressure and pedal edema. AST 221, ALT 234, Alk phos 48, lactate dehydrogenase 710, total bili 1.2, alb 3.5, total prot 5.4. Liver shown above. What term best describes these liver findings
|
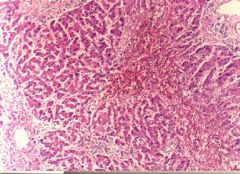
Centrilobular congestion. The restrictive lung disease leads to cor pulmonale with right-sided congestive heart failure. This causes passive venous congestion in the liver that is most pronounced in the centrilobular areas. When congestion is severe, the anoxia can cause centrilobular necrosis with transaminase elevation. The microscopic appearance is that of intense centrilobular congestion. Notice that the area around the portal tract is less congested.
|
|
|
How is cholestasis marked in the liver
|
Plugs of yellow-green bile in canaliculi
|
|
|
What are Mallory bodies
|
Globular red cytoplasmic structures most characteristic of alcoholism, and acute alcoholic hepatitis in particular.
|
|
|
27 year old man with history of IV drug use is seen in the ER because he has experienced nausea, vomiting, and passage of dark-colored urine for the past week. Scleral icterus and mild jaundice. Recent and healed track marks in the right antecubital fossa. Confused, somnolent man oriented only to person. Exhibits asterixis.
Total prot 5.0 Alb 2.7 AST 2342 ALT 2150 Alk phos 233 Total bili 8.3 Direct bili 4.5 HBsAG positive Anti-HBs negative Anti-HBc positive Anti-HBc, IgM negative Anti-HAV, IgG positive Anti-HAV, IgM negative Anti-HCV negative Anti-HDV positive Diagnosis? |
Superinfection of chronic HBV with HDV. This patient has serologic evidence of superinfection of HDV on chronic hepatitis caused by HBV. The evidence for chronic hep B is the presence of HBsAg and anti-HBc IgG antibody. The evidence of recent HDV infection is the presence of anti-HDV antibodies. HBV and HDV infections are likely to occur in drug users who inject parenterally. HDV cannot replicate in the absence of HBV; hence, isolated HDV infection does not occur. When HDV infection is superimposed on chronic HBV, three outcomes are possible: mild HBV hepatitis may be converted to fulminant disease; acute hepatitis may occur in an asymptomatic HBV carrier; or chronic progessive disease may develop, culminating in cirrhosis
|
|
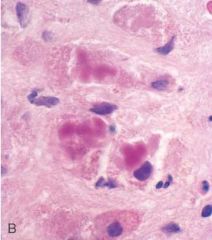
After a heavy bout of drinking over the weekend, a 38 year old man feels acutely ill with nausea, upper abdominal pain, and jaundice. Right upper quadrant tenderness. WBC 16,120 with 82% neut, 8% bands, 8% lymphs, 2% mono. Total bili 4.9, AST 542, ALT 550, alk phos 118. Liver biopsy shown. What best describes the findings in this biopsy
|
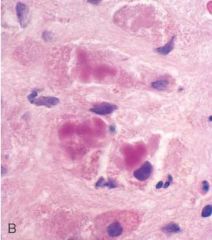
Mallory bodies. This is a classic case of acute alcoholic hepatitis. The figure shows globular eosinophilic cytoplasmic inclusions called Mallory bodies. These inclusions are characteristic of, but not specific for, alcoholic hepatitis. There are also areas of hepatocyte necrosis surrounded by neutrophils. Some neutrophils can be seen in the figure.
|

