![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
35 Cards in this Set
- Front
- Back
|
Functions
|
Substrates and oxygen carried to call cells
Metabolites and CO2 carried from all cells Flow to skin and extremities is regulated (thermoregulation) Hormone distribution Body defense mechanisms are carried by CVS Fluid movement is essential for living cells to exchange materials with their environment |
|
|
Total body water=
|
extracellular fluid ( plasma +interstitial fluid) + intracellular fluid
|
|
|
The extracellular fluid compartments are:
|
Blood plasma
Interstitial fluid, which is the ECF outside the capillaries and the site of metabolic exchange |
|
|
The extracellular fluid compartments require two interconnected system:
Cardiovascular system for Lump-vascular system for |
blood plasma
interstitial fluid |
|
|
The interstitial fluid (site of metabolic exchange) is released from the
|
arterial ends of the capillaries as an ultafiltrate of blood
|
|
|
Bulk transport
|
Substances carried between organs
|
|
|
TRANSPORT RATE =
|
FLOW RATE X CONCENTRATION
|
|
|
The velocity of blood at any level =l
|
total flow divided by cross sectional area at that leve
|
|
|
Therefore blood flow is slowest at the
|
capillaries, favoring gas and nutrient exchange.
|
|
|
Most substances cross capillary walls by ...
Called ... |
PASSIVE DIFFUSION
TRANSCAPILLIARY SOLUTE DIFFSION |
|
|
Four factors determine diffusion rate
|
Concentration difference
Surface area for exchange Diffusion distance Permeability of wall to diffusing substance |
|
|
Diffusion distance
Diffusion is very slow over distances of |
1 cm but very rapid over distances of 4-7 micrometers
|
|
|
Basic design for tubes delivering fluid metabolites to interstitial fluid is:
|
Very thin walled tube
As close as possible to every cell in body |
|
|
Tissue barrier at level of the capillary is a single squamous epithelial cell called an
|
ENDOTHILIAL CELL
|
|
|
Pump- the heart
|
Contracts and propels blood out to the body
|
|
|
Arterial system
|
Conveys blood from heart to the capillaries
|
|
|
Venous system
|
Conducts blood from capillaries back to heart
|
|
|
Lymph-vascular system
|
Carries lymph from the interstitial fluid spaces of the body back into the blood vascular system
|
|
|
... is the driving force for the flow
|
PRESSURE DIFFERENCE
|
|
|
VASCULAR RESISTANCE is
|
a measure of how difficult it is to make blood flow through a tube
I.e. the pressure required to make a given volume over a certain distance |
|

|

|
|
|
Therefore there are only two ways that blood flow through any organ can be changed
|
Changing pressure difference across the vascular bed
Changing vascular resistanc |
|
|
Therefore blood flow depends on:
PRESSURE DIFFERENCE TOTAL PERIPHERAL RESISTANCE VISCOSITY |
Mean arterial pressure minus central venus pressure
Small changes in radius have powerful effects on flow When radius or diameter of a blood vessel doubles, the flow increases by 16 This is not a variable that is easily changed but it may influence vascular resistance |
|
|
The greatest drop will occur in a area of greatest resistance
This occurs in |
ARTERIOLES
|
|
|
blood flow to a particular organ can be altered by adjusting the resistance of the arterioles without greatly affecting
|
pressures and flows in other organs
|
|
|
Four forces influence fluid movement across capillary walls
|
Capillary blood pressure (Pc)
Plasma colloic osmotic pressure (oncotic pressure πp) Interstitial fluid hydrostatic pressure (Pif) Interstitial fluid colloid pressure πif) |
|
|
net exchange pressure =
|
(Capillary blood pressure + Interstitial fluid colloid pressure) - (Plasma colloic osmotic pressure +Interstitial fluid hydrostatic pressure )
|
|
|
THERE IS A SLIGHT PREDOMINANCE OF
|
FILTRATION OVER REABSOTPTION
|
|
|
Left side of the heart pumps
|
oxygenated blood to the Systemic circulation- high pressure/ high resistance
|
|
|
Right side of the heart pumps
|
deoxygenated blood to the Pulmonary system- low pressure/low resistance
|
|
|
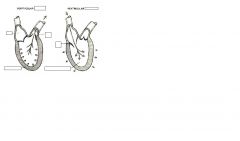
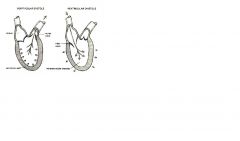
FROM THE HEART TO THE BLOOD VESSELS, this is called
|
SYSTOLE
|
|
|
When the ventricle relaxes, pressure within the ventricle falls below that in the atrium, and AV valve opens and the ventricle fills with blood. THIS IS CALLED
|
DISATOLE.
|
|
|
Three features of the hear t are very important features for effective functioning
|
Conductivity
Contractility Autorhythmicity |
|
|
|
|
|
Requirements for effective cardiac pumping
|
Contraction of individual cardiac muscles must be regular and synchronized
Valves must be open fully Valves must not leak Ventricles must fill adequately during diastole |

