![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
49 Cards in this Set
- Front
- Back
|
Brutons tyrosine kinase (BTK) |
Genetic mutation prevents B cells from developing X-linked agammaglobulinemic (XLA) |
|
|
Tx of BTK |
Infusion of human antibody |
|
|
Pathogens |
Microbial agents that cause disease infect a wide range of animals and humans |
|
|
Ways animals fight pathogens |
First line of defense help prevent pathogens from gaining entry Then Cells that interact with pathogen and destroy it |
|
|
Molecular recognition of nonself |
Immune system must distinguish invaders from its own cells This is accomplished by receptors that bind specifically to molecules from foreign cells and viruses |
|
|
Immunity |
Body’s capability of removing or killing foreign substances pathogens and cancer cells to avoid and limit infection |
|
|
2 types of molecular recognition |
Innate Adaptive |
|
|
Innate immunity |
Present before exposure to pathogens Effective from the time of birth Respond to a broad range of pathogens: small preset group of receptor proteins bind to molecules or structures that are common to a group of viruses, bacteria, or other pathogens |
|
|
Adaptive immunity (acquired) |
Activated after innate immune defense (Slower response) Develops after exposure to agents like micorbe, toxins, and other foreign stuff Very specific response to pathogens (has large number of receptors recognizing a feature on a particular molecule in pathogen and knows how to destroy it) Adaptive defenses are enhanced by previous experience |
|
|
Innate is in both invertebrates and vertebrates |
All animals and plants In vertebrates, first response and serves as foundation of adaptive immunity |
|
|
Innate immunity of invertebrates includes: |
Exoskeleton Lysosome Phagocytosis Hemocytes |
|
|
Exoskeleton |
In insects Made of chitin and forms first barrier to pathogens |
|
|
Lysozyme |
Enzyme that breaks down bacterial cell walls Digested system is chitin-protected and had lysozyme also |
|
|
Hemocytes |
Hemocytes circulate in hemolymph and carry out phagocytosis Also secrete antimocrobial peptides that disrupt the plasma membranes of fungi and bacteria |
|
|
Phagocytosis |
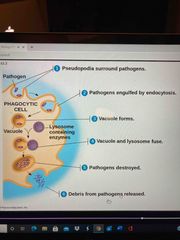
Back (Definition) |
|
|
Transmembrane receptor (toll) |
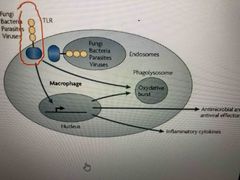
Immune system recognizes specific bacteria and fungi by structures on their cell walls Binding to fungi activated molecules of toll which then activated production and secretions of antimicrobial peptides that kill fungi cells and inflammatory cytokines |
|
|
Dicer -2 enzyme |
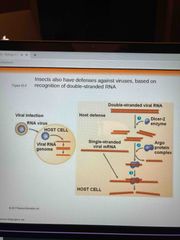
Breaks down RNA with argo protein complex |
|
|
Barrier defenses |
Skin and mucus membranes of digestive, urinary, and reproductive tracts: -Mucus traps and allows for the removal of microbes -Ciliated epithelial cells of trachea |
|
|
Natural killer cells (NK) |
Circulate throughout the body Determine proteins of viruses and cancers (cells lacking MHC-1) Release chemicals leading to cell death, inhibiting the further of virally infected or cancerous cells |
|
|
Body fluids in addition to the barrier defenses |
Saliva, mucus, tears (contain lysozymes) attacks microbes Low pH of skin from sweat Low pH of gastric glands in digestive system prevents growth of bacteria |
|
|
Cellular innate defenses |
Detect devour and destroy invading pathogens through Phagocytosis Phagocyctic cells recognize groups of pathogens using toll-like receptors (TLR)-a receptor protein TLRs recognize fragments of molecules belonging to a particular pathogen |
|
|
4 Toll-like receptors (TLR) types |
1. TLR4-Recognize lipopolysaccharide (surface of gram positive bacteria) 2. TLR5-recognize falgellin (bacteria flagella) 3. TLR3- inner surface of endocyctic vesicles recognize double stranded RNA viruses 4. TLR9-recognize CpG (DNA unlethylated CG sequences) |
|
|
How are pathogens destroyed in cellular innate defenses? |
Destroyed within lysosomes in 2 ways 1. Gases produced by lysosome poisens, engulf pathogens 2. Lysosomes and other enzymes degrade pathogen components |
|
|
Phagocytic cells in mammals |
Neutrophils Macrophages Dendritic cells Eosinophils |
|
|
Neutrophils |
Circulate in blood Engulf and destroy |
|
|
Macrophages |
Big eaters Migrate through the body or reside permanently in organs and tissues Mainly reside in lymph nodes where they encounter pathogens that flowed in from interstitial fluid |
|
|
Dendritic cells |
Skin, contact external environment Stimulate development of adaptive immunity Reside outside lymphatic system but migrate to lymph nodes after interaction with pathogen to interact with other immune cells (adaptive immunity) |
|
|
Eosinophils |
Beneath mucosal surfaces Discharge destructive enzymes |
|
|
Barrier defenses |
Skin and mucus membranes of digestive, urinary, and reproductive tracts: -Mucus traps and allows for the removal of microbes -Ciliated epithelial cells of trachea |
|
|
Natural killer cells (NK) |
Circulate throughout the body Determine proteins of viruses and cancers (cells lacking MHC-1) Release chemicals leading to cell death, inhibiting the further of virally infected or cancerous cells |
|
|
Body fluids in addition to the barrier defenses |
Saliva, mucus, tears (contain lysozymes) attacks microbes Low pH of skin from sweat Low pH of gastric glands in digestive system prevents growth of bacteria |
|
|
4 Toll-like receptors (TLR) types |
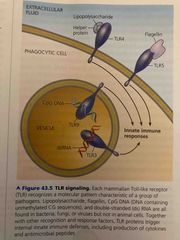
1. TLR4-Recognize lipopolysaccharide (surface of gram positive bacteria) 2. TLR5-recognize falgellin (bacteria flagella) 3. TLR3- inner surface of endocyctic vesicles recognize double stranded RNA viruses 4. TLR9-recognize CpG (DNA unlethylated CG sequences) |
|
|
4 Toll-like receptors (TLR) types |
1. TLR4-Recognize lipopolysaccharide (surface of gram positive bacteria) 2. TLR5-recognize falgellin (bacteria flagella) 3. TLR3- inner surface of endocyctic vesicles recognize double stranded RNA viruses 4. TLR9-recognize CpG (DNA unlethylated CG sequences) |
|
|
How are pathogens destroyed in cellular innate defenses? |
Destroyed within lysosomes in 2 ways 1. Gases produced by lysosome poisens, engulf pathogens 2. Lysosomes and other enzymes degrade pathogen components |
|
|
Phagocytic cells in mammals |
Neutrophils Macrophages Dendritic cells Eosinophils |
|
|
Neutrophils |
Circulate in blood Engulf and destroy |
|
|
Macrophages |
Big eaters Migrate through the body or reside permanently in organs and tissues |
|
|
Dendritic cells |
Skin, contact external environment Stimulate development of adaptive immunity |
|
|
Natural killer cells (NK) |
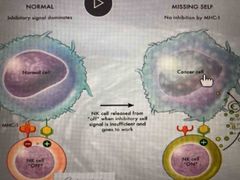
Circulate throughout the body Determine proteins of viruses and cancers (cells lacking MHC-1) Release chemicals leading to cell death, inhibiting the further of virally infected or cancerous cells |
|
|
Antimicrobial peptides and proteins |
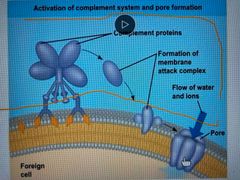
Peptides and proteins function in innate defense by attacking pathogens or impeded reproduction About 30 proteins (often inactive until needed) make up complement system Cause lysis in an pathogen cell and triggers inflammation Damage broad groups of pathogens by disrupting membranes |
|
|
Interferon (antimicrobial peptide and protein) |
Proteins provide innate defense Help activate macrophages -Proteins are secreted by virus-infected body cells -tell neighboring cells to produce substances (cytokine) that inhibit viral reproduction -produced by recombinant DNA technology (tx hepatitis C) |
|
|
Innate inflammatory response to wounds in dermis |
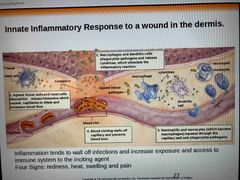
Inflammation tends to wall off infections and increase exposure/access to immune system 4 signs: redness, heat, swelling, pain |
|
|
Inflammatory response to wound in dermis step by step |
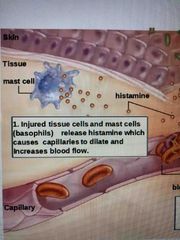
1. Injured tissue and mast cells (basophils) release histamine which causes vasodilation to increase blood flow Activate complement proteins which promote further release of histamine, attracting more phagocytic cells |
|
|
Step 2 |
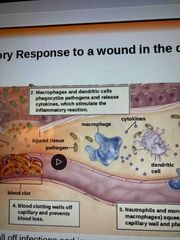
Macrophages and dendritic cells phagocytize pathogens and release cytokines which stimulate inflammatory reaction This reaction increases local blood supply (redness and heat of inflammation) Blood engorged capillaries leak fluid into other tissues causing swelling |
|
|
Step 3 |
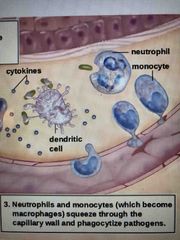
Neutrophils and monocytes (become macrophages) squeeze through the capillary wall and phagocytize pathogens Due to all phagocytic cells in tissue, pus is created (fluid rich in white blood cells, dead pathogens, and cell debris from damage tissues) |
|
|
Step 4 |
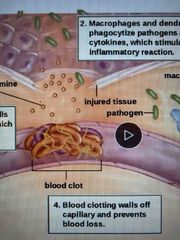
Blood clotting walls off capillary and prevents blood loss and blocking pathogens Nearby endothelial cells secrete signals that attract neutrophils and macrophages (step 3) |
|
|
Systemic inflammatory response |
Local or throughout whole body (systemic) Additional neutrophils can be released from bone marrow WBC increases significantly within hours Fever triggered by substances released by macrophages increase body’s set point (hypothalamus) which then enhances phagocytosis and tissue repair |
|
|
Septic shock |
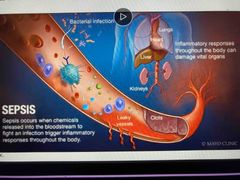
Caused by overwhelming inflammatory response High fever, low blood pressure, reduced blood flow through capillaries Fatal in more than 1/3 cases |
|
|
Evasion of innate immunity by pathogens |
Some avoid destruction Modify their outer capsule surface to prevent molecular recognition and resist breakdown from lysosomes after phagocytosis Include streptococcus pneumoniae (causes pneumonia and meningitis) Tuberculosis-kills more than a million people a year |

