![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
39 Cards in this Set
- Front
- Back
|
What are the functions of joints? |
1. Give skeleton mobility 2. Hold skeleton together |
|
|
What are the classifications of bone? |
1. Fibrous 2. Cartilagenous 3. Synovial |
|
|
What structural components do all synovial joint have in common? |
1. Articular Cartilage 2. Joint Cavity 3. Articular Capsule 4. Synovial Fluid 5. Reinforcing Ligaments |
|
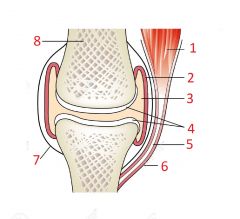
Label: |
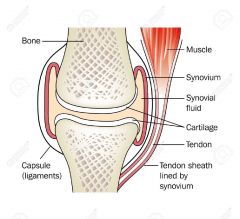
1. Muscle 2. Synovium 3. Synovial Fluid 4. Cartilage 5. Tendon 6. Tendon sheath lined by synovium 7. Capsule (ligaments) 8. Bone |
|
|
What is the role of: 1. Ligaments 2. Cartilage |
1. Ligaments stabilise the joint 2. Cartilage cushions the joint |
|
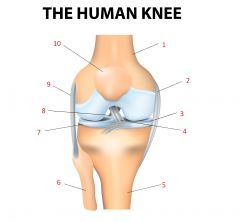
Label: |
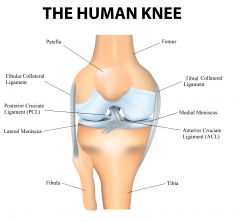
1. Femur 2. Tibial collateral ligament 3. Medial meniscus 4. Anterior cruciate ligament 5. Tibia 6. Fibula 7. Lateral meniscus 8. Posterior cruciate ligament 9. Fibular collateral ligament 10. Patella |
|
|
How does joint tissue composition vary between connective tissues? |
Vary based on function: 1. Tendon / Ligament : Dense, fibrous, strong in tension, transmits force 2. Cartilage: Resists compression - hydrated meshwork 3. Bone: Provides support and protection - Rigid Mineralised sheets. |
|
|
What is the cellular composition of connective tissues? What types of cells exist? What does each type synthesise? |
All joint tissues are mainly extracellular matrix. The cells which do exist, do so as they synthesise extracellular matrix: 1. Fibroblasts - Synovium, tendon etc 2. Chondrocytes - Cartilage 3. Osteocytes - Bone 4. Stem cells - New ECM synthesising cells |
|
|
What are the main varieties of molecules which make up the extracellular matrix of connective tissue? |
1. Collagens 2. Proteoglycans 3. Glycoproteins |
|
|
What are proteoglycans important for? Give 2 examples. |
Important for connective tissue material properties - hold water in tissues and thus convey vasoelasticity. Also important for interactions with cells, cytokines and collagen. Aggrecan, Decorin. |
|
|
1. What molecule types are 'Biolubricants'? 2. What are they important for? 3. Give 3 examples of biolubricants. |
1. Glycosaminoglycans and Proteoglycans 2. Essential for lubricating joint function 3. i) Hyduronan ii) lubrican / Proteoglycan 4 ii) Aggrecan |
|
|
What are bursae? |
Bursae are small synovial fluid filled sacs which are lined with synovium. They are found in and around most synovial joints. |
|
|
What is the function of bursae? |
Bursae function to facilitate movement. |
|
|
What is the pathology which affects the bursae? |
Bursitis - inflammation of the bursae. |
|
|
What are the two types of synovial cells? What are the functions of each? |
Type A (macrophage like) synovial cells - phagocytic immune function
Type B (Fibroblast like) produce synovial fluid. |
|
|
What is the role of synovial fluid? |
Lubricates the joints. |
|
|
What is the main structural component of connective tissue? |
Collagen. |
|
|
Describe the tertiary structure of collagen. |
1. 3 alpha chains (each a single gene product) are arranged in a triple helix. |
|
|
What is a crucial feature of the primary sequence? |
Glycine every 3 residues |
|
|
What is the hallmark structural motif of collagen? |
Gly - X - Y Where: X = Usually a proline Y = Usually a hydroxyproline |
|
|
What are the major structural collagens? |
Types I, II and III |
|
|
What is the first stage of collagen synthesis? |
Synthesised as an inactive procollagen molecule in the cell and then exocytosed into the ECM |
|
|
How is procollagen activated? |
N + C terminals cleaved by pro collagen peptides |
|
|
What is the extracellular matrix molecule compositions of: 1. Bone 2. Cartilage 3. Tendon / Ligaments |
1. 90% Type I collagen, 5% Type V collagen - arranged in sheets which are mineralised 2. 90% Type II collagen, 10% aggrecans - arranged in a meshwork 3. 90-95% type I collagen, 5% type II collagen, 0.5% DSPG - arranged in parallel fibres. |
|
|
What is the key determinant of tendon tensile strength? |
The Parallel type I collagen fibril bundles. |
|
|
How is constant fluid flow in tendon fibril bundles ensured? What is the effect of this process? |
The ebb and flow of proteoglycan swelling. Collagen resists the swelling and thus acts like a pump which forces fluid through the tendon. Allows renewal of nutrition for chondrocytes, removal of waste products and thus synthetic activity. |
|
|
How is extracellular matrix turnover in connective tissues mediated? |
Mediated through the secretion of secreted proteases. |
|
|
What are the key secreted proteases? |
1. MMPs - Matrixmetalloproteinases 2. ADAMTs (A disintegrin and metalloproteinase with thrombospondin motifs) |
|
|
How many MMPs are there? What are the important MMPs which act as collagenases? |
23 in total 1, 2, 8, 13, 14 |
|
|
How many ADAMTs are there? How is their activity regulated? |
19 in total Inhibited by TIMP-3 |
|
|
What are the different types of MMP? |
1. Archetypal - i) Collegenases ii) Stromelysins 2. Gelatinase 3. Furin Activated 4. Matrilysins |
|
|
What are the different types of ADAMTs? |
1. Angioinhibitory 2. Pro collagen N-Peptidase (cleaves the N terminal of procollagen) |
|
|
How is the activity and function of an MMP regulated throughout its life cycle? |
1. Before formation - translation / transcription 2. Produced in inactive form 3. Activation of zymogen 4. Inhibition when acting on target ECM component |
|
|
How is the secretion of MMPs controlled? |
a) transcriptionally controlled - cytokines, growth factors, mechanical load b) IL-1 c) Tumour necrosis factor |
|
|
How are MMP zymogens activated? |
1. By other MMPs 2. Other enzymes |
|
|
How are active MMP's regulated? |
By TIMPs which bind with MMPs to produce an inactive complex. Also by alpha 2 macroglobulin |
|
|
What does TIMP stand for? |
Tissue Inhibitor of Metallo Proteinases |
|
|
What diseases are associated with altered ECM turnover? |
1. Osteoarthiritis - degeneration of cartilage / bone - increased matrix degradation 2. Rheumatoid arthiritis - increased matrix degradation & reduced synthesis - systemic 3. Tendinopathy - Increased matrix degradation and synthesis |
|
|
What will SEVERE osteoarthiritis result in? |
Severe OA will result in a loss of proteoglycan and collagen fibrillation. |

