![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
171 Cards in this Set
- Front
- Back
|
What secretes ADH? What effect does it elicit?
|
Posterior Pituitary Gland ; increases water reabsorption in distal convoluted tubules and collecting ducts
|
|
|
Where is aldosterone secreted? What effect does it elicit?
|
Adrenal cortex
Sodium reabsorption in exchange for potassium or hydrogen |
|
|
Functions of the urinary system
|
- remove metabolic wastes (nitrogenous and acidic)
- remove hormones, drugs, and acid-base balance in the body -secrete erythropoietin -activate Vitamin D - regulate blood pressure through the renin-angiotensin-aldosterone system (RAS) |
|
|
Where are the kidneys located?
|
Retroperitoneally on the posterior abdonminal wall
|
|
|
What protects the kidneys from injury?
|
Fibrous capsule
Fat that surrounds it Lower ribs |
|
|
What is the outer layer of the kidney called? Inner layer?
|
Cortex
Medulla |
|
|
which layer is the renal pelvis in?
|
Medulla
|
|
|
Which layer is the calyces in?
|
Medulla
|
|
|
What is the functional unit of the kidney?
|
Nephron
|
|
|
What is superior to the kidney?
|
Adrenal gland
|
|
|
Two types of nephrons
|
Cortical and Juxtamedullary
|
|
|
blind end of the proximal convulated tubule
|
Bowman's capsule
|
|
|
During filtration, what passes from the blood into the tubule? What stays in the blood?
|
Large volume of fluid (wastes, nutrients, electrolytes, and other dissolved substance);
CELLS AND PROTEIN REMAIN IN THE BLOOD |
|
|
Where does reabsorption of essential nutrients, water, and electrolyes occur?
|
Proximal convoluted tubule (has brush border of microvilli)
does most reabsorption. Glucose, AAs, water, Na+ (and Cl-) loop of Henle (especially the long loops in JG produces hypertonic urine by reabsorbing water from the filtrate (due to high osmotic pressure) Distal convoluted tubule: Actively reabsorbs sodium ions (aldosteron effect) and excretes hydrogen, potassium ions, and drugs into the filtrate Collecting ducts: reabsorb water (ADH effect) |
|
|
What transports urine to the renal pelvis?
|
Collecting ducts
|
|
|
Reabsorption of nutrients and electrolytes involves the use of __________ transport
|
Active
|
|
|
Sodium reabsorption may be linked to the ____________ of the molecules, such as _________ and amino acids. There is a limit on reabsorption, called the _________ or ___________ maximum. What is this max for glucose?
|
Cotransport
glucose transport or tubular maximum 310 mg/min for glucose |
|
|
What causes glucosuria? What is it an indication of?
|
Excess quantity of glucose in the filtrate, with inadequate carrier molecules for reabsorption (so glucose gets peed out);
indication of hyperglycemia associated with diabetes mellitus |
|
|
How is water reabsorbed?
|
Osmosis
|
|
|
What controls the reabsorption of fluid and electrolytes?
|
Hormones
|
|
|
How does ADH control reabsorption of water?
|
By increasing the permeability of the distal convoluted tubule and collecting ducts
|
|
|
Where does atrial natriuretic hormone come from? What is its effect?
|
Heart ; reduces sodium and fluid reabsorption in the kidneys
|
|
|
How much of the CO enters the renal artery from the aorta?
|
20-25% (hence, the kidneys are always processing a very large volume of blood at any given time)
|
|
|
What is the alternative blood supply available to a lobe of the kidney deprived of oxygen supply? What would happen in the case of an embolus?
|
NONE. Anastomoses between the interlobar and arcuate arteries are NOT present.
In the case of an embolus (or any obstruction of blood flow) that lobe would undergo necrosis and infarction |
|
|
Is there regeneration of the nephrons?
|
NO
|
|
|
What is the vasa recta?
|
Peritubular capillaries
|
|
|
How many arterioles and how many capillaries are assocciated with each nephron?
|
Two arterioles and two capillaries
|
|
|
Summarize the blood flow through the kidney
|
Renal artery --> interlobar artery --> arcuate artery --> interlobular artery--> afferent arteriole --> glomerulus --> efferent arteriole --> peritubular capillaries--> interlobular vein --> arcuate vein --> interlobar vein--> renal vein
|
|
|
What is the purpose of the dual arteries of Bowman's capsule?
|
To control the pressure in the glomerular capillaries (GFR)
|
|
|
If the afferent arteriole is dilated and the effernt arteriole is constricted, what will happen to the hydrostatic pressure in the glomerular capillaries? GFR?
|
increase; increase
|
|
|
Loss of voluntary control of the bladder
|
Incontinence
|
|
|
Involuntary urination by a child age 4+ years. What is the often related to?
|
Enuresis
Often related to developmental delay, sleep pattern, psychosocial aspect |
|
|
What is stress incontinence? Who is it most common in? What are the "triggers"?
|
When increased intra-abdominal presure forces urine through the sphincter.
Most common in pregnant (esp multiparity) triggers= coughing.lifting, laughing |
|
|
What are JG cells? Where are they? What do they secrete?
|
Juxtaglomerular cells;
Modified smooth muscle cells in the wall of the afferent arteriole, just before it enters Bowman's capsule; Renin |
|
|
What makes up the juxtglomerular apparatus?
|
JG cells and macula densa.
|
|
|
What are the macula densa? Where are they located? what is their function?
|
A group of modified distal convoluted tubule cells;
Right next to the JG cells near the vascular pole; Act as baroreceptors and chemoreceptors- JG cells respond to changes in systemic blood pressure and macula densa responds to changes in sodium chloride concentration |
|
|
What stimulates the release of renin from the JG cells?
|
decrease in systemic blood pressure (blood volume) or decrease in sodium concentration in the filtrate.
|
|
|
What does renin do?
|
Converts angiotensinogen (plasma protein) to angiotensinogen I, which is then converted to angiotensinogen II by the ACE enzyme in the endothelial cells of the lung capillaries
|
|
|
What effect does angiotensinogen II elicit?
|
Powerful vasoconstrictor;
Stimulates the release of aldosterone from the adrenal gland cortex (increases water reabsorption by increasing sodium reabsorption) |
|
|
The RAS system causes (vasoconstriction / vasodilation)? What effect does this have of the GFR?
|
Vasoconstriction
Increases GFR |
|
|
In the absence of ADH, the collecting tubules remain (permeable / impermeable) to water. What is the result of this?
|
Impermeable
Increased volume of water in the urine |
|
|
Autoregulation, SNS innervation, and RAS system are all mechanism for _______________.
|
Vasoconstriction
|
|
|
What are the "renin-blocking" drugs?
|
beta-adrenergic blocking drugs
|
|
|
Where does "filtrate" become "urine"?
|
In the collecting ducts
|
|
|
Explain the pathway urine takes during excretion
|
Collecting ducts --> renal calyces --> renal pelvis --> ureter --> urinary bladder --> urethra
|
|
|
What assists movement of urine from the ureters to the urinary bladder?
|
Peristaltic movement by smooth muscles
|
|
|
The urinary bladder is surrounded in ___________, with _______ for expansion
|
Smooth muscle
Rugae |
|
|
The urinary bladder and two ureters make up the ____________.
|
trigone
|
|
|
what effect does hypertrophy of the prostate gland (common in older men) have on urine flow?
|
Decreases it (due to obstruction)
|
|
|
What is micturition? What stimulates it?
|
Urination, voiding;
Stimulated by the increased pressure as the bladder distends, PNS innervation |
|
|
______________________ results from an incompetent bladder sphincter. What causes this in older people?
|
Overflow incontinence;
A weakedn detrusor muscle (prevents complete emptying of the bladder, leading to frequency and incontinence) |
|
|
Overflow incontinence results from ...
|
... an incompetent bladder sphincter.
|
|
|
What causes neurogenic bladder?
|
interference with the CNS and ANS(for example, by injury)
|
|
|
What are the two types of neurogenic bladder?
|
Spastic or flaccid
|
|
|
Inability to empty the bladder?
|
Retention
|
|
|
What is retention typically accompanied by?
|
Overflow incontinence
|
|
|
Spinal cord injury at the ______ level blocks the micturation reflex. This leads to _______ .
|
sacral; retention
|
|
|
What urinary defect might occur after anethesia? Does this occur during general or spinal?
|
Retention ; can be both
|
|
|
Describe normal urine in terms of color, odor, and specific gravity
|
Clear
straw-colored mild odor sp gr 1.010 - 1.050 |
|
|
What does "cloudy" urine indicate?
|
Presence of large amounts of protein, blood, bacteria, and pus
|
|
|
How would you expect urine that has large amounts of protein, blood, bacteria, and pus to look?
|
Cloudy
|
|
|
What might dark, "coca-cola or tea-colored" urine indicate?
|
hematuria
excessive bilirubin highly concentrated urine |
|
|
How would you expect urine that contained blood or excessive bilirubin to look?
|
dark, "coca-cola or tea-colored"
|
|
|
Unpleasant or unusual odor of urine may result from...
|
...infection or result from certain dietary components or medication
|
|
|
What would small amount of hematuria indicate?
|
infection, inflammation, or tumors in the urinary tract
|
|
|
What would large amounts of hematuria indicate?
|
increased glomerular permeability (as in glomerulonephritis or nephrosis) or hemorrhage
|
|
|
What does hematuria mean in men?
|
Cancer
|
|
|
Leakage of albumin into filtrate
|
Albuminuria
|
|
|
Leakage of mixed plasma proteins into filtrate
|
Proteinuria
|
|
|
Presence of bacteria in urine? What does this indicate?
|
Bacteriuria ; infection in the urinary tract
|
|
|
Another name for small amounts of blood in the urine? Another name for large amounts of blood in the urine?
|
Microscopic hematuria
Gross hematuria |
|
|
Infection in the urinary tract is indicated by the presence of ___________ and __________ organisms in the urine
|
gram + and gram -
|
|
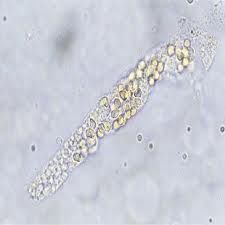
What is this a picture of? What does it indicate?
|
Urinary casts (microscopic molds of tubules consisting of one or more cells)
Indicates inflammation in the kidney tubules |
|
|
What does specific gravity of urine indicate?
|
The ability of tubules to concentrate urine
|
|
|
What type of specific gravity (high, low) would dilute urine with normal hydration have? What might this indicate?
|
low ; renal failure
|
|
|
What type of specific gravity (high, low) would concentrated urine with normal hydration have?
|
High
|
|
|
What would be found in the urine when diabete mellitus is not well controlled?
|
Glucose and ketones
|
|
|
Another name for ketoacids?
|
Ketones
|
|
|
What blood test would you expect to be elevated if your kidney fails to excrete nitrogen wastes during protein metabolism?
|
Elevated serum urea (BUA) and elevated serum creatinine or nitrogen (BUN) ;
also, metabolic acidosis possibly because nitrogen will bind with H ions |
|
|
What would elevated BUA and BUN serum levels indicate? What is this due to?
|
Failure to excrete nitrogen wastes during protein metabolism;
decreased GFR |
|
|
What does metabolic acidosis indicate?
|
decreased GFR;
failure of the tubules to control acid-base balance |
|
|
Decreased serum pH would indicate
|
Metabolic acidosis
|
|
|
decreased serum bicarbonate would indicate
|
metabolic acidosis
|
|
|
A low hemoglobin level would indicate? This would suggest that production of ___________ has (increased / decreased) or depression of the _________________.
|
Anemia ; erythropoietin ; bone marrow
|
|
|
A blood test that depends on related fluid balance
|
Serum electrolytes
|
|
|
A test to diagnose poststreptococcal glomerulonephritits
|
Antibody level- ASO titer (antistreptolysin O) or ASK titer (antistreptokinase O)
|
|
|
What test could prove that the kidney was the cause of hypertension?
|
Elevated levels of renin
|
|
|
Why might you perform a culture and sensitivity test on the urine?
|
-to identify the causative organism of infection
- select the appropriate treatment |
|
|
Why would you perform a radiological test (such as radionuleotide imaging, angiography, ultrasound, CT, MRI, or intravenous pyelography)?
|
To visualize structures and possible abnormalities, flow patterns, and filtration rates
|
|
|
What is are two examples of clearance tests? What do they assess?
|
Creatin or inulin clearance ; Used to assess GFR
|
|
|
What is a test that could be used to assess GFR?
|
Clearance test (creatine or inulin)
**inulin is the best test, because our body cannot use inulin, so ALL of it should be excreted out-- it it's not there's a problem |
|
|
Test that visualizes the lower urinary tract? When might this be used?
|
Cystoscopy ; could be used during biopsy or to remove kidney stones
|
|
|
Test that is used to acquire tissue specimens ?
|
Biopsy
|
|
|
What do diuretics remove from the body?
|
Electrolytes and water
|
|
|
What drug could you give to increase excretion of water through the kidneys?
|
Diuretic
|
|
|
Name some disorders for which a duretic might be utlized
|
Pulmonary edema (or just edema in general)
Hypertension Renal failure Liver disease Congestive heart failure |
|
|
What do "loop diuretics" do?
|
Inhibit reabsorption of NaCl in the renal tubules
|
|
|
What is the major side effect of using a diuretic? what might this cause?
|
Hypokalemia ; cardiac arrythmias and muscle weakness
|
|
|
What should a patient eat while on a diuretic?
|
Bananas
|
|
|
Which diuretic spares potassium?
|
Aldactone (Spiranolactone)
|
|
|
What are the two types of dialysis?
|
Hemodialysis and peritoneal dialysis
|
|
|
Which type of dialysis can only be perfomed at a hospital, dialysis center, or home with special equipment and training?
|
Hemodialysis
|
|
|
Dialysis provides __________ and __________ across a semipermeable membrane
|
filtration ; reabsorption
|
|
|
Process that sustains life during kidney failure. Name two situations in which this would be used
|
Dialysis ;
1. Acute renal failure (until problem is reversed) 2. End stage renal failure (until transplant organ becomes available) |
|
|
Which type of dialysis is required for a patient with chronic renal failure?
|
Hemodialysis
|
|
|
What device does blood move through during to hemodialysis to reach the machine
|
Shunt or catheter
|
|
|
What is dialysis fluid called?
|
Dialysate
|
|
|
Explain what happens with wastes, electrolyes, blood cells, proteins, and bicarbonate ions during dialysis
|
Blood --> dialysate
wastes electrolytes dialysate--> blood bicarbonate stays in blood blood cells proteins |
|
|
How often is hemodialysis required and how long does it typically last? What are the potential complications?
|
Every three weeks and lasts for 3-4 hours
complications Blood clots Infection of shunt Blood vessels involved in the shunt become sclerosed or damaged (have to find new site) Increased risk of parenteral infections (Hep B, Hep C, HIV) |
|
|
which type of dialysis is typically done on an outpatient basis?
|
Peritoneal dialysis
|
|
|
In peritoneal dialysis, the ___________ serves as the semipermeable membrane
|
Peritoneal membrane
|
|
|
During peritoneal dialysis, dialysate is instilled into the ____________ and drained via ___________ .
|
peritoneal cavity ; gravity
|
|
|
Which type of dialysis takes longer? What is a major complication of this type?
|
Peritoneal dialysis ; Infection leading to peritonitis
|
|
|
Since transient bacteremia is a risk in dialysis. To prevent this risk _____________ are given.
|
prophylactic antibiotics
|
|
|
What is the major concern we have as pharmacists in drug administration to a patient on dialysis?
|
Caution with dosage because toxic-level buildup can occur
|
|
|
Why are UTIs so common?
|
-urine is excellent growth medium
- E coli is common causative agent |
|
|
Examples of lower urinary tract infections?
|
Cystitis (inflammation of the urinary bladder) and Urethritis (inflammation of the urethra)
|
|
|
example of upper urinary tract infection?
|
Pyelonephritis
|
|
|
Examples of lower urinary tract infections
|
Urethritis and cystitis
|
|
|
Example of upper UTI
|
pyelonephritis, glomerulonephritis
|
|
|
Most common to develop UTI?
|
Women (chocolate factory so close to the water factory)
Older men (Prostatic hypertrophy and urine retention- any problem with the reproductive system poses risks to urniary system in men since they're shared) |
|
|
Congenital abonormalities, incontinence, retention of urine, or direct contamination with fecal matter could cause
|
UTI
|
|
|
Inflammation of the bladder wall and urethra
|
Cystitis
|
|
|
Cystitis
|
Inflammation of the bladder wall and urethra
|
|
|
Painful urination
|
Dysuria
|
|
|
Dysuria
|
Painful urination
|
|
|
Nocturia
|
Need for urination during sleep period
|
|
|
How does the urine look with cystitis?
|
Cloudy and unusual odor
|
|
|
what is most likely to cause hyperactive bladder and reduced capacity?
|
Cystitis
|
|
|
Where is the infection in pyelonephritis?
|
From the ureter into the kidney (including the renal pelvis and the medullary area)
|
|
|
In pyelonephritis, what fills the renal pevis and calyces? If the infection is severe, how does this effect the renal artery and vein and urine flow?
|
Purulent exudate ; Sever infection could compress the renal artery and vein, obstruct urine flow to the ureter
|
|
|
What are the signs and symptoms of pyelonephritis?
|
Same as cystitis because infection will also be present in the bladder wall and urethra, but in addition:
Dull, aching, flank pain (in the lower back) FEVER |
|
|
Diagnose.
Urinary casts found during urinalysis. What does this presence reflect? |
Pyelonephritis ;
Presence of renal casts reflect tubule involvement |
|
|
Why does flank pain occur in pyelonephritis?
|
The inflammation streches the renal capsule
|
|
|
What is hydronephrosis?
|
An enlargement of the kidney due to the accumulation of urine
|
|
|
What are complications of pyelonephritis?
|
- Loss of tubule function (due to medullary involvement)
- Hydronephrosis (due to obstruction of urine flow, which leads to collection of filtrate) - Chronic renal failure (due to excessive scar tissue and necrosis if it is left untreated) |
|
|
How would you treat pyelonephritis?
|
Antibacterials
|
|
|
What does APSGN stand for?
|
Acute poststreptococcal glomerulonephritis
|
|
|
Diagnose.
Kidney Disorder in which antigen-antibody complexes are formed, leading to an inflammatory response. |
APSGN (a form of glomerulonephritis)
|
|
|
Explain the inflammatory response associated with APSGN
|
Presence of anti-streptococcal (ASO) antibodies form complexes with the antigens, then are deposited into the lumen of the glomerulus, causing an inflammatory response. This causes increased capillary permeability --> leakage of proteins and rbcs
|
|
|
What causes the negative effect of strept on the kidney and the heatr?
|
strong exotoxin produced by strept organism causes antigen-antibody complex formation and DEPOSITION INTO THE TISSUE--> SEVERE INFLAMMATION and NECROSIS
|
|
|
What the the effect of glomerulonephritis on GFR?
|
Decreased
|
|
|
Where would you find congestion and cell proliferation in the glomerulus?
|
Severe inflammatory response associated with glomerulonephritis
|
|
|
How would you expect the urine to look in glomerulonephritis? What about the quantity?
|
Dark and cloudy (due to blood and proteins);
Oliguria, due to decreased GFR |
|
|
Diagnose.
Facial and periorbital edema and flank pain with fever. |
glomerulonephritis
|
|
|
explain the effects of glomerulonephritis on blood pressure
|
Because of edema, the macula densa cells are not detecting a high blood volume, therefore, the JG cells will release increased levels of renin, leading to further edema because increased hydrostatic pressure, but with limited osmotic pressure. This increases the blood pressure. eventually, as kidney fails, renin secretion will slow and blood pressure will drop.
|
|
|
What do you expect to see in renal failure?
|
Anemia (decreased erythropoietin secretion)
|
|
|
glomerulonephritis would cause metabolic (acidosis / alkalosis)
|
acidosis
|
|
|
What might be wrong with a a person whose urinalysis showed proteinuria, hematuria, and erythrocyte casts with no evidence of infection?
|
glomerulonephritis
|
|
|
What might treatment for glomerulonephritis include?
|
Sodium restriction and antihypertensives (to lessen the workload of the kidney)
Glucocorticoids (to reduce inflammation) Decrease fluid and protein intake (in severe cases) |
|
|
1 tsp = _____ mL
|
5
|
|
|
What does the abnormality in nephrosis cause?
|
Escape of large amounts of plasma proteins to escape into the filtrate
|
|
|
What causes nephrosis?
|
In children 2-6 usually idiopathic
in adults, usually secondary to an autoimmune disease (such as SLE) or to exposure of nephrotoxins or drugs |
|
|
What would you expect in nephrotic syndrome, hypo or hyperalbuminemia? What does this cause?
|
Hypoalbuminemia
Decreased osmotic pressure and increased edema |
|
|
What effect would you expect nephrotic syndrome to have on blood pressure?
|
Low or normal (due to extreme fluid loss... may be elevated depending on angiotensin II levels)
|
|
|
What hormone secretions would you expect to see in nephrosis?
|
Aldosterone (to increase sodium reabsorption and increase blood volume)
Maybe renin (to vasoconstrict) |
|
|
Why is lipiduria associated with nephrosis?
|
Not totally clear- probably a response of the liver to high protein loss
|
|
|
Diagnose.
proteinuria, lipiduria, casts, massive edema, sudden increase in girth |
Nephrosis
|
|
|
How would you treat nephrosis?
|
All treatments aimed at decreasing inflammation
-Glucocorticoids - decreasing sodium reabsorption - ACE inhibitors (to decrease hydrostatic pressure and to decrease aldosterone secretion) |
|
|
Another name for a stone?
|
Calculi
|
|
|
Where can calculi form in the urinary tract?
|
anywhere
|
|
|
What do you call a large calculi that forms in the renal pelvis and calyces?
|
"Staghorn" calculi (because looks like deer antlers)
|
|
|
Under which conditions do urinary calculi form?
|
- Insufficient fluid intake
-When there is excessive amounts of solutes in the filtrate -urinary tract infection |
|
|
Calculi themselves are not dangerous.... what causes the manifestations? what can it cause?
|
Obstruction of urine flow;
Causes: Infection Hydronephrosis with dilation of the calyces Atrophy of renal tissue (if located in the kidney or ureter) |
|
|
What is the formation of calculi in the urinary system called?
|
Urolithiasis
|
|
|
What are common components of calculi? What does stone formation depend on?
|
Calcium (due to alkaline urine)
Uric acid stones (Due to acidic urine and hyperuricemia associated with gout, high-purine diets [red meats], and cancer chemotherapy) Struvite Cysteine Stone formations depend on Predisposing factors (diet, genetics, etc) |
|
|
What type of stone would a person who eats a diet rich in red meats likely form?
|
Uric acid
|
|
|
Diagnose.
Renal colic |
Urolithiasis
|
|
|
Intense spasms of pain in flank area that radiates into the groin area
|
Renal colic (associated with urolithiasis)
|
|
|
what is ESWL? When is it used?
|
Extracorporeal shock-wave lithotripsy ;
Used to break up calculi |
|
|
What can a person do to prevent urolithiasis?
|
Maintaint high fluid intake
Adjustment of urine pH through dietary modifications (cranberry juice, vitamins, antioxidants) |

