![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
38 Cards in this Set
- Front
- Back
|
Define the Equilibrium Potential
|
It is the value of the membrane potential where there is not net positive transport of a permeant ion into or out of a cell.
|
|
|
The direction of current in an ionic solution follows the movement of these ions
|
It follows the movement of cations in an electric field
|
|
|
The equilibrium potential can vary based on these factors (2)
|
Temp and [ionic]
|
|
|
The equilibrium potentials for the following ions in a neuron:
Ca2+: Na+: Bicarbonate: Cl-: K+: |
The equilibrium potentials for the following ions in a neuron:
Ca2+: +123 Na+: +62 Bicarbonate: -14 Cl-: -65 K+: -80 |
|
|
The equilibrium potentials for the following ions in a muscle cell:
Na+ K+ Cl- Ca2+ Bicarbonate |
The equilibrium potentials for the following ions in a muscle cell:
Na+: +65 K+: -95 Cl-: -90 Ca2+: +132 Bicarbonate: -26 |
|
|
General description of an ion channel (3 components)
|
1. Consists of protein subunits surrounding
2. a central aqueous pore 3. with an ion selectivity filter |
|
|
An example of a symport at the synaptic cleft
|
Neurotransmitters use the energy created by Na+ to re-enter nerve terminals
|
|
|
An example of an antiport with synaptic vesicles
|
Neurotransmitters are allowed to enter the vesicle in exchange for Na+
|
|
|
Typical mean values of Vm for:
• Photoreceptors: • Neurons: • Skeletal muscle fibers: |
Typical mean values of Vm for:
• Photoreceptors: - 40mv • Neurons : - 65mv • Skeletal muscle fibers: - 90mv |
|
|
Compare/Contrast the relative number of K+, Cl- and Na+ channels open in the Neurons and Skeletal muscle and why this is significant
|
---------------- K+ Cl- Na+
Neurons Large some Few Skeletal Large Large Few The significance is K+ contributes greatly to the Vm of neurons where as in Skeletal muscle, both K+ and Cl- are contributing |
|
|
A stable resting membrane potential is dependent on this (2)
|
Ion pump activity and Ion channels
|
|
|
All excitable cells have resting membrane potentials dependent on this
|
Outside [K+]
|
|
|
The reason why raising outside [K+] causes depolarization and possible subsequent signaling failure in excitable cells
|
• Raising outside [K+] causes less K+ to flow out of the cell
• This leads to a less negative cell interior (Vm becomes less negative) • The depolarization and can lead to a "depolarization-induced closure" of voltage-sensitive Na+ channels ---> this closure is called inactivation |
|
|
In the scenario of depolarization-induced closure of voltage-sensitive Na+ channels, which gate on the channel is closed?
|
The inactivation gate
|
|
|
These factors will affect the cell's transmembrane potential (4)
|
• The type of open ion channels
• The number of open ion channels • The amount of current passing through the channel when it is open • The time the channel spends in an open state |
|
|
Define Po and how it is measured
|
Po is the probability of a channel opening
It is calculated as a fraction of the observed time a channel is open. Another way to look at it is: Po = (the # of open ion channels in a time period) / (the total # channels available for opening at that same time period) |
|
|
The relationship of conductance and resistance and their units
|
Conductance (g) is the inverse of Resistance (r).
Conductance is measured in Siemens Resistance is measured in Ohms |
|
|
Ohm's Law
|
V = Ir = I/g
|
|
|
The total membrane conductance for an ion is dependent on this
|
The number of open channels for the ion, Nx
|
|
|
Calculating the membrane conductance, g(x), for an ion X
|
g(x) = Nx (γx)
where γ = the single channel conductance for that ion |
|
|
Voltage-gated channels and transmitter-gated channels have there Po values dependent on this (one each)
|
V-gated: Po dependent on Vm
Transmitter- gated: Po dependent on [transmitter] in their vicinity |
|
|
Electrochemical gradients drive this type of flux
|
Passive ion
|
|
|
What is the general form of the Nernst equation and what does it tell us
|
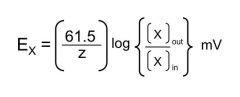
It tells us the value of the Vm that exactly counterbalances the ion's [gradient] across the membrane
|
|
|
The only ion that has an equilibrium potential close to Vm for neurons and skeletal muscle
|
Chloride (-65mV)
|
|
|
The relationship btwn the equilibrium potential for an ion and its concentration gradient
|
The equilibrium potential and the concentration gradient is equal and opposite
|
|
|
Calculating the Electrochemical gradient for an ion
|
(Vm - Ex) mV
|
|
|
The significance of calculating the electrochemical gradient using the equilibrium potential of an ion
|
The value calculated gives the driving force as produced by the electrochemical gradient that an ion would use to passively leave/enter a cell. However, an equal and opposite force will be matching this value which represents what an active (ATP-driven) pump is doing to ensure there is no net flux of the ion
|
|
|
Equating a cell to a circuit, this represents the capacitor and conductor
|
Capacitor = plasma membrane
Conductor = open ion channel |
|
|
The value of the total ionic current, Im, when the cell is at rest
|
Im = zero, ** however, its components are non-zero
|
|
|
How the resting membrane potential is calculated when there are >1 ion channels present
|

The Potential is the weighted sum of all the equilibrium potentials
|
|
|
Channelopathies:
• definition • what the episodes involves • how it can be acuired (3 possible sources) |
Channelopathies:
• d/o caused by dysfxnal ion channel activity • episodes of disturbed nerve or muscle cell excitability • autoimmune attack, nerve damage, after use of drug tx or toxins |
|
|
Ischaemic cerebral edema:
• what it can cause • another name for this type of edema • why the edema occurs • the secondary edema that can follow |
Ischaemic cerebral edema:
• irreversible cellular damage due to cellular swelling • cytotoxic edema • Na/K pump is no longer supplied w/ ATP and the gradient dissipates. The influx of Na and Cl into the cell leads to cellular swelling from water • Vasgogenic edema - blood vessels become more permeable and water flows out of them and into the extra cellular space |
|
|
Aquaporins:
• their fxn • two prominent fxns in the CNS • The name of the primary channel in the brain and where its found (2 sites) |
Aquaporins:
• selectively allow water through the plasma membrane • production of CSF, regulation of water at the BBB • AQP-4 > astrocyte foot processes at the BBB > brain-CSF interface |
|
|
Relationship of Lethal injection and cardiac muscle
|
The increase in extracellular [K+] causes many muscles, particularly cardiac, to fail to generate APs because v-gated Na+ channels become inactivated (depolarization-induced closure)
|
|
|
Channelopathies:
• definition • what the episodes involves • how it can be acuired (3 possible sources) |
Channelopathies:
• d/o caused by dysfxnal ion channel activity • episodes of disturbed nerve or muscle cell excitability • autoimmune attack, nerve damage, after use of drug tx or toxins |
|
|
Ischaemic cerebral edema:
• what it can cause • another name for this type of edema • why the edema occurs • the secondary edema that can follow |
Ischaemic cerebral edema:
• irreversible cellular damage due to cellular swelling • cytotoxic edema • Na/K pump is no longer supplied w/ ATP and the gradient dissipates. The influx of Na and Cl into the cell leads to cellular swelling from water • Vasgogenic edema - blood vessels become more permeable and water flows out of them, into the extra cellular space |
|
|
Aquaporins:
• their fxn • two prominent fxns in the CNS • The name of the primary channel in the brain and where its found (2 sites) |
Aquaporins:
• selectively allow water through the plasma membrane • production of CSF, regulation of water at the BBB • AQP-4 > astrocyte foot processes at the BBB > brain-CSF interface |
|
|
Relationship of Lethal injection and cardiac muscle
|
The increase in extracellular [K+] causes many muscles, particularly cardiac, to fail to generate APs because v-gated Na+ channels become inactivated (depolarization-induced closure)
|

