![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
31 Cards in this Set
- Front
- Back
|
what is a complement?
|
Complement is:
-system of plasma proteins some of which are INACTIVE proteases activate by cleavage -a triggered enzyme cascade with downstream amplification -components are cleaved into 2 pieces -- 'b' (binding- BIG) -- 'a' (soluble mediator-smalle) chemotactic |
|
|
what are the functions of a complement system? (list of 6)
|
1. phagocytosis by opsonization
-coats the pathogen with a molecule (b) that will facilitate uptake of that pathogen by phagocytic cells 2. promote inflammation -recruits inflammatory cells by liberated soluble chemotactic factors (a) 3. kills microorganisms -forms a membrane attack complex that inserts a pore into the pathogen's membrane leading to death by osmotic lysis (can also kill host cells-pathological) 4. B cell activation and maturation 5. Immune complex removal -solubilizes and facilitates the removal of antibody attached to foreign molecule complex, filtered by the kidney 6. T cell activity modulation/maturation |
|
|
The 3 Pathways and noteworthy characteristics
|
Classical Pathway
-ONLY one of these that is acquired* and therefore initiated by antibody participation 2. MB-Lectin Pathway 3. Alternative Pathway All 3 use the same TWO amplification steps, C3 and C5 convertase -BUT, the alternative pathway uses a slightly structurally different C3 convertase Upon generation of the C3 convertase, the 3 pathways converge into a common pathway until their termination |
|
|
Classical/Acquired Pathway Initiation
|
requires deposition of IgM or IgG antibody on the surface of a pathogen
C1 is the first component of the complement that binds. Then it undergoes a conformational change, and generates an active serene protease that cleaves C4 into C4a (soluble) and C4b (binds to surface of pathogen) |
|
|
C1q
|
first component of complement classical pathway to bind
binds to IgM Fc and IgG Fc but also directly to some bacterial surfaces to initiate pathway activates serine proteases to cleave C4 and C2 |
|
|
MB-Lectin Pathway Initiation
|
mannose-binding lectin binds mannose on pathogen surfaces
uses MASP-1 and MASP-2 instead of C1, which cleave C4 and C2 |
|
|
What can antibodies do and what can't they do?
|
they have no inartistic killing activity!
this is where the complement cascade comes in |
|
|
what classes of antibody activate complement?
|
IgM, IgG3, IgG1, IgG2
|
|
|
why doesn't complement function at mucosal surfaces?
|
don't want to damage our barrier epithelial
-a consequence of complement activation is tissue damage -this is also why the primary antibody that protects surfaces (IgA) is noninflammatory complement only functions inside the body (blood, interstitial space) -inactivated in tears, saliva, mucins |
|
|
IgM and IgG initiation of the classical pathway
|
although they are found circulating in the blood, they re unable to activate complement there. In solution, IgM is planar. In this conformation the complement binding site on the Fc region is masked and IgM cannot fix complement.
it is not until the antibody binds a pathogen and undergoes a conformational change, from planar to more crab-like, that the C1 binding site is exposed ONLY ONE IgM is required for activation, while TWO are required for IgG (and the 2 IgG molecules must be sufficiently close enough to be bridged to each other. |
|
|
activation of alternative pathway
|
very different from the other 2 pathways
most primitive and undergoes constant turnover activation is triggered by pathogen surface recognition spontaneous hydrolysis of C3 |
|
|
where do all 3 pathways converge?
|
C3
|
|
|
what does the assembly of the C3 Convertase generate?
|
1. Chemotactic factors (C3a, C5a, and C4a)- peptide mediators of inflammation, phagocyte recruitment
2. Opsonin (C3b)- aids in phagocytosis 3. Terminal Complement Components- lead to formation of the membrane attack complex that creates pores in the pathogen envelope resulting in osmotic lysis |
|
|
C3 Convertase
|
converts C3 into C3a and C3b
-this step can be repeated thousands of times for amplification cleavage produces 3 powerful chemotactic factors (C3a, C5a, C4a), which act on vascular epithelium to recruit neutrophils from the blood to the site of infection also produces C3b, an opsonin |
|
|
opsonins
|
molecules that bind antigens and make them a target of the immune system
|
|
|
C5 convertase
|
generate if C3b binds to the C3 convertase itself
makes C5a and C5b -this is the 2nd amplification step in the pathway C5b is deposited onto the pathogen's cell membrane and together wight he other terminal components of the cascade (C6-C9), inserts a ring structure into the membrane |
|
|
opsonins: C3b
|
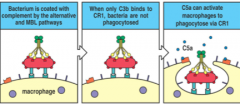
C3b and IgG
pathogen membrane bound C3b binds to its receptor located on macrophages and other phagocytic cells when only C3b binds to CR1, bacteria are not phagocytksed phagocytosis requires the binding of both C3b AND C5a (second signal) |
|
|
opsonins: IgG
|
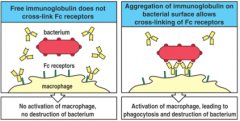
there are IgG-Fc receptors on the surface of macrophages to recognize IgG antibodies bound to specific pathogens
aggregation of immunoglobulin on bacterial surface allows cross-linking of Fc receptors -IgG Ab binds its epitope on bacterium and IgG also binds to its Fc receptor on the macrophage requires minimum of 2 IgG molecules |
|
|
synergistic opsonization
|
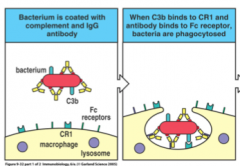
deposition of BOTH C3b and IgG on the surface provides a synergistic effects and is the best way to promote phagocytosis
|
|
|
MAC assembly
|
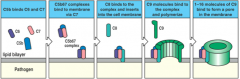
termination of the complement cascade involves assembling a Membrane Attack Complex (MAC)
-begins with the C5 convertase that generates C5b -C5b binds C6 and C7 followed by C8, which is inserted into the membrane instead of simply binding the surface -finally, up to 16 molecules of C9 polymerize in a circle to form a pore |
|
|
Removal of immune complexes
|
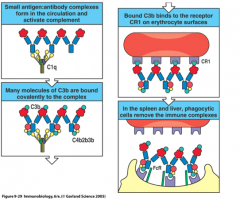
during an immune response, pathogen antigens and their pathogen-specific IgG antibodies form complexes that bind the C3b
RBC's have complement receptors (CR2) for C3b, which capture these large antibody:antigen complexes and remove them from circulation as they pass through the spleen and liver resident macrophages in these areas destroy the complexes and dispose of them |
|
|
complement cascade's role in adaptive immunity
|
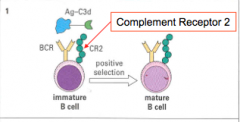
one of the receptors for complement, CR2, is part of the B-Cell signaling mechanism
BCR bridging to Ag via CR2 delivers a powerful activation and maturation signal to the B-cell in the periphery upon complement receptor activation, a T-cell is driven to become a regulatory T-cell |
|
|
deficiency in compliment proteins
|
results in increased susceptibility to extracellular bacterial infections
deficiencies in earlier steps (leading up to generation of C3b) give rise to immune complex diseases (like lupus), where one is unable to remove immune complexes -this should make sense since removal requires C3b |
|
|
deficiencies in terminal components of complement (C6-C9)
|
make people susceptible to recurrent nisserial infections (bacterial infections)
|
|
|
deficiencies in regulatory proteins
|
would lead to uncontrolled activation of the complement system and hereditary angioedema (uncontrolled activation of complement cascade, leading to extreme inflammation)
|
|
|
C4a
|
chemotactic factor
peptide mediator of inflammation (weak activity) |
|
|
C3a
|
chemotactic factor
early promotor of acute inflammation (intermediate activity act on mast cells (degranulation) and tissues around blood vessels (recruit histamine) |
|
|
C3b
|
many molecules of C3b bind to pathogen surface and act as opsonins
initiates amplification via the alternative pathway binds C5 for cleavage by C2b |
|
|
C5a
|
chemotactic factor
early promotor of acute inflammation act on mast cells (degranulation) and tissues around blood vessels (recruit histamine) |
|
|
specific C3 convertase for classical and alternative pathways
|
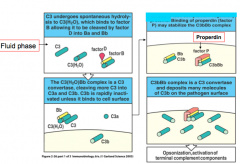
Classical: C4b2b and C4b2a
(made from binding of C2b onto C4b) Alternative: C3bBb |
|
|
specific C5 convertase used
|
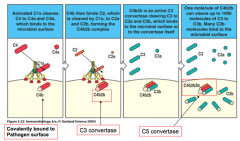
C4b2b3b
(created when C3b binds to the C3 convertase (C4b2b)) |

