![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
26 Cards in this Set
- Front
- Back
|
General Features of Complement
|
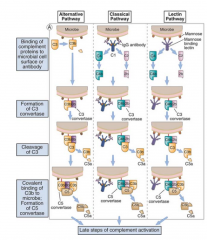
- A family of ~30 activation and regulatory proteins found either bound to the cell membrane or in circulation
- Synthesized mainly by the liver - Many circulating proteins are pro-enzymes whose activation requires their proteolytic hydrolysis - 2 pathways: 1. the alternative and 2. the classical - Both pathways generate “C3b” |
|
|
Complement Function
|
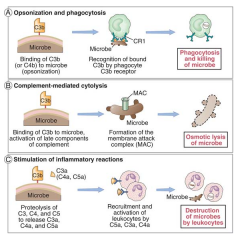
1. Facilitate the interaction of phagocytes to induce opsonin-mediated phagocytosis
2. Induce osmotic lysis of microbes 3. Enhance vascular permeability by inducing degranulation of mast cells/ basophils 4. Induce chemotaxis of neutrophils 5. Facilitate immune complex elimination |
|
|
C3b
|
- Bind to immune complexes in circulation
- They can be eliminated by neutrophils (opsonin mediated phagocytosis) or be transported to the liver and/or spleen via red blood cells (erythrocytes) |
|
|
Classical Complement Pathway
|
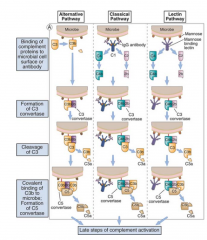
- The classical pathway is triggered when IgM or certain subclasses of IgG (IgG1 and IgG3 in humans) bind to antigens (e.g., on a microbial cell surface)
- Fc regions of the antibodies become accessible to complement proteins and 2 or more Fc regions come close together - When this happens, the C1 complement protein binds to two adjacent Fc regions - Attached C1 becomes enzymatically active, thus resulting in the binding and cleavage of two other proteins, C4 and C2. - The resultant C4b2b complex becomes covalently attached to the antibody and to the microbial surface where the antibody is bound - This complex is the “classical pathway C3 convertase,” which functions to break down C3, and the C3b that is generated again becomes attached to the microbe - Some of the C3b binds to the C4b2b complex, and the resultant C4b2b3b complex |
|
|
C3a and C5a (C4a)
|
- C3a and C5a are anaphylatoxins generated by the action of the C3 and C5 convertases
- Bind to cognate receptors on mast cells and basophils inducing degranulation, resulting in the release of histamine and other inflammatory mediators - Histamine increases vascular permeability - C5a is also chemotactic for phagocytes, recruiting these cells to the site of infection - Both the induction of histamine release and chemotaxis of neutrophils contribute to the initiation of the inflammatory response - The anaphylatoxin C4a is generated only following activation of the classical pathway |
|
|
C3b
|
- Serves as an opsonin on microbial surfaces
- On immune complexes it facilitates the elimination of immune complexes - C3b is a component of the alternative pathway C3 convertase (C3bBb) - Component of the C5 convertases of both the alternative (C3bBbC3b) and the classical (C4b2a3b) complement pathways |
|
|
C2b
|
- C2b is produced by C1 acting on C2 in the classical pathway
- A weak kinin that increases vascular permeability and contributes to the genesis of inflammation |
|
|
C2a and C4b
|
- Form the C3 convertase Classical Pathway (C4bC2a)
- They are also components of the C5 convertase classical pathway (C4b2a3b) |
|
|
C5b
|
- Generated by the action of C5 convertases on the complement protein, C5.
- Formation and deposition of the proteolytically derived C5b proteolytic fragment onto cell surfaces serves as the stimulus for the formation of the membrane attack complex |
|
|
C4b2a
|
C3 convertase, classical pathway
|
|
|
C3bBb
|
C3 convertase, alternative pathway
|
|
|
C4b2aC3b
|
C5 convertase, classical pathway
|
|
|
C3bBbC3b
|
C5 convertase, alternative pathway
|
|
|
C5b
|
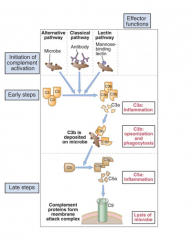
- Activation of either the alternate or the classical complement pathways generates C5b
- Initiator molecule for the formation of the membrane attack complex (MAC) in the terminal complement pathway (MAC= C5b, C6, C7, C8, C9) - Insertion of the MAC into the target membrane induces osmotic lysis and death of the microbe (or cell) |
|
|
Alternative Complement Pathway
|
- C3b prompts the mobilization of the alternative pathway
- Derived from circulating C3 - In the absence of microbial infection, the spontaneously generated C3b is rapidly inactivated - In presence of bacteria, C3b binds to microbial surfaces activates complement - Factor B hydrolyzed to Ba and Bb by Factor D - C3bBb complex generated by C3 convertase - C3 convertase stabilized by a tetrameric protein, properdin, that extends its half-life 6 to 10-fold - C3b is required for the formation of the alternative pathway C5 convertase (C3bBbC3b), which cleaves C5 to generate C5a and C5b - Formation of C5b = initiating step for the formation of the membrane attack complex |
|
|
C1 INH
|
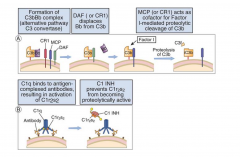
Classical Pathway Regulator:
- C1 INH (C1 esterase inhibitor (C1 INH)) forms a complex with C1, preventing the spontaneous activation of the classical complement pathway - Inactivates the protease, kallikrein. |
|
|
DAF
|
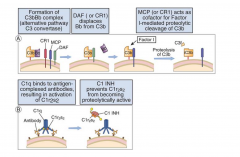
Classical & Alternative Pathway Regulator:
Decay accelerating factor (DAF) binds to membrane bound C4b and C3b, blocking the formation of the alternative and classical pathway C3 convertases |
|
|
C4bp
|
Classical Pathway Regulator:
- C4 binding protein (C4bp) binds to fluid phase C4b, preventing its attachment to cells. - When the classical C3 convertase has already formed, C4bp competitively binds with C4b, promoting its dissociation |
|
|
Factor I
|
Classical Pathway Regulator:
Cleaves C4b (bound or soluble) to its inactive form, C4bi, in the presence of one of several cofactors |
|
|
AI
|
Classical & Alternative Pathway Regulator:
Anaphylatoxin inhibitor (AI) binds to C3a, C4a, and C5a, inhibiting their binding to receptors on mast cells and basophils |
|
|
Factor H
|
Alternative Pathway Regulator:
- Binds to C3b in the fluid phase thus preventing C3b from binding to the cell surface. - When the alternative pathway C3 convertase has formed, Factor H competitively binds with C3b, inducing the dissociation of this convertase |
|
|
Factor I
|
Alternative Pathway Regulator:
Cleaves C3b (soluble or membrane bound) to yield the inactive form, C3bi. |
|
|
Terminal Pathway
|
MAC inhibitors (MAC INH) include homologous restriction factor (HRF), S-protein, and CD59. These inhibit formation of MAC on autologous cells
|
|
|
Kallikrein
|
- Links the complement and the contact intrinsic coagulation systems
- Enhance the intrinsic coagulation pathway by proteolytically converting Factor XII to Factor XII(a) in the presence of a cofactor, kininogen |
|
|
Bradykinin
|
potent vasodilator that increases vascular permeability
|
|
|
Complement Test
|
- Tests for (a) the classical pathway (CH50) and (b) the alternative pathway (AH50) measure overall complement activity.
- Tests for C3 and C4 are often used if the CH50 test is abnormal. |

