![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
89 Cards in this Set
- Front
- Back
|
free air w/in peritoneal cavity
|
pneumoperitoneum
|
|
|
types of pneumoperitoneum
|
laparotomy w/in 3-7 days
spontaneuous traumatic |
|
|
m/c cause is perforation of gastric or duondenal ulcer
|
spontaneous pneumoperitoneum
|
|
|
secondary to diagnostic studies
perforation fm barium enema/colonoscopy severe external trauma |
traumatic pneumoperitoneum
|
|
|
free air under hemidiaphragm
|
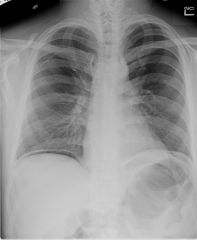
radiographic signs of a pneumoperitoneum
|
|
|
intraluminal and extraluminal air outlining both surfaces of bowel wall
|
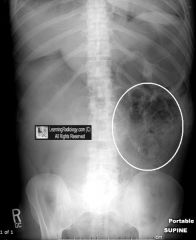
double wall sign AKA Rigler's sign
|
|
|
triangular gas density projected over superior margin of right kidney
represents air trapped dorsally under liver |
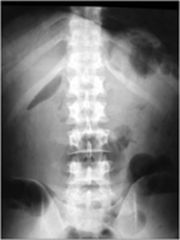
Morrison's pouch sign
|
|
|
two closely approximated loops of bowel mimic a Rigler sign
|
double wall finding
|
|
|
gas filled loop on intestine between liver and diaphragm
|
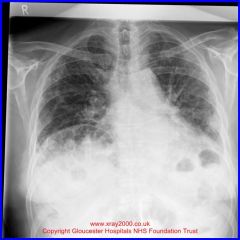
Chilaiditis syndrome
|
|
|
gastric air bubble is under right hemidiaphragm
|
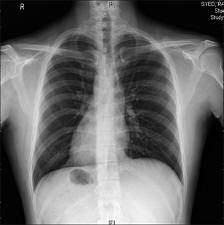
situs inversus
|
|
|
fat under diaphragm
|
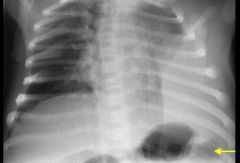
subdiaphragmatic fat or extraperitoneal fat
|
|
|
Mucosal folds in sm intestine normally 1-2mm in width & regularly spaced
|
valvulae conniventes
|
|
|
small bowel rule of 3
|
no more than 3 air/fluid levels
no more than 3 cm of bowel distention no more than 3 mm between folds |
|
|
small bowel obstruction clinical findings
|
nausea, vomiting, cramping, abdominal pain, distention
|
|
|
may be partial or complete
adhesions fm surgery m/c hernias neoplasms intussusception strictures fm Crohn's disease volvulus |
mechanical bowel obstruction
|
|
|
sm bowel tries to force obstruction out by strong peristaltic contractions
may be seen as dynamic motion on surface of abdomen |
Dynamic Ileus
|
|
|
bowel becomes exhausted and stops peristalsis
air collects in dilated loops of bowel |
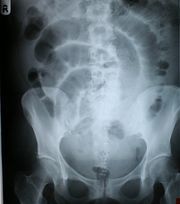
Adynamic Ileus
|
|
|
fairly common in adults occasionly children
indirect>direct M>F presence of enlarged scrotum that contains multiple loops of air filled bowel |
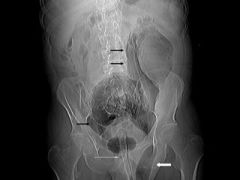
Inguinal hernia
|
|
|
common in adults
stomach herniates thru diaphragmatic hiatus |
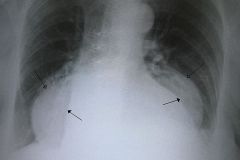
hiatal hernia
|
|
|
gastroesophageal junction remains fixed and gastric fundus herniates
|
Paraesophageal (1%) hiatal Hernia
|
|
|
m/c (95%) gasatroesophageal junction slides upward
|
Sliding hiatal hernia
|
|
|
three types of hiatal hernia
|
sliding
paraesophageal mixed |
|
|
gastroesophageal junction at 2 cm above diaphragm
soft tissue mass or air fluid level in middle/posterior mediastinum (retrocardiac region) |
radiographic findings for hiatal hernia
|
|
|
two types of pathological calcifications
|
metastatic
dystrophic |
|
|
refers to calcium deposition in normal tissue
result of hypercalcemia/elevated pH not frequent in abdomen apppears as a cloud of calcium deposits described as tumoral calcinosis |
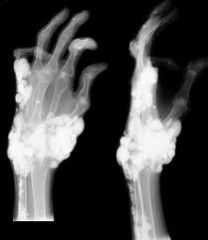
metastatic calcification
|
|
|
occurs in local tissue damage or stone formation
normal calcium/pH very common in abdomen |
Dystrophic calcification
|
|
|
dystrophic calcification classifications
|
morphological features
location mobility |
|
|
radiographic features of dystrophic calcifications
what to look for |
shape, border sharpness, marginal continuity, internal architecture
|
|
|
four types of dystrophic calcifications
|
concretions
conduit wall cyst wall mass |
|
|
called stone or calculus
calcified mass that forms inside tubular or hollow structures forms like pearl |
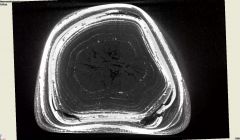
concretion
|
|
|
sharp
clearly defined external margins continuous internal architecture:laminations, eccentric area of lucency, homogenously dense |
radiographic appearance of concretions
|
|
|
found in appendix
associated w/current or future perforation associated w/pain 90% chance of acute appendicitis |
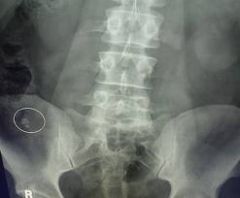
appendocolith
|
|
|
RUQ
solitary or multiple "bag of Diamonds" only 10-15% calcify & show up on xray can be multifaceted |
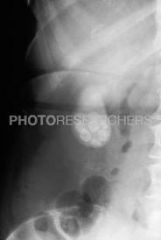
cholelithiasis
gallstones |
|
|
m/c associated w/pancreatitis d/t alcoholism
caused by long standing ductal obstruction/inflammation multiple,tiny, dense,discreet opacities cross midline at L1-2 |
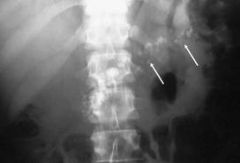
pancreatic calculi
|
|
|
m/c calcification in pelvis
calcified thrombus w/vein normal variant multiple/bilateral do not cross midline |
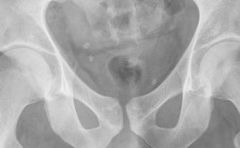
phleboliths
|
|
|
multiple calcifications ,various sizes, behind pubic symphysis in males
prior prostatitis asymptomatic usually |
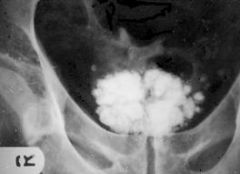
prostatic calculi
|
|
|
seen in: renal calyces, renal pelvis, ureters, bladder
most calcify 85-95% visualized on xray chronic low-level dehydration/infection mineral deposit embedded in inorganic material asymptomatic til obstruct calcium phosphate, calcium oxalate, magnesium phosphate (struvite) m/c |
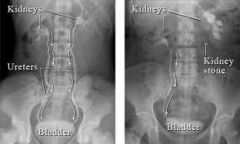
urinary tract calculi
|
|
|
large stone occupies renal collecting system forming cast of major calyces and renal pelvis
usually struvite (triphosphate) may cause chronic hydronephrosis leading to renal failure |
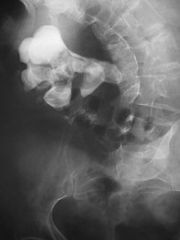
staghorn calculus
|
|
|
seen on plain film present w/ low back pain, flank/groin pain
look in kidney, ureters, bladder m/c lodged in uteropelvic junction, bifurcation of iliac vessels, uterovesical junction |
radiographic findings for renal stones
|
|
|
round
central lucency below ischial spine DOES NOT MOVE |
phlebolith
|
|
|
irregular shape
uniformly dense above ischial spine Moves w/time |
renal stone
|
|
|
caused by obstruction/infection
may be migrant renal stone 50% may be seen on plain film stellate referred to as "jackstone" |
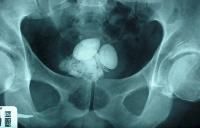
bladder stone
|
|
|
stellate bladder stone
|
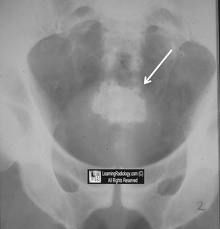
jackstone
|
|
|
tubular structures thru which fluids are conducted
calcifications confined to tubular walls m/c arterial walls |
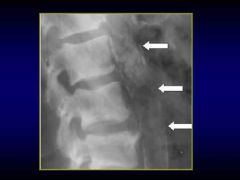
conduit wall calcifications
|
|
|
parallel, linear opacities (tract-like)
dot-dash appearance may see vessel branch pattern seen on end appear as ringlike |
radiographic finding for conduit wall
|
|
|
m/c result of atherosclerosis
*smoking, diabetes,hypertension m/c below renal arteries NOT contraindication to manipulation Not always an aneurysm |
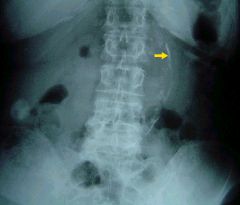
Abdominnal aorta calcification
|
|
|
m/c athersclerosis
M 4:1 older pts 95% 60-80yrs asymptomatic pain in low back,buttock, down leg abdominal mass or pulsation abdominal pain |
aneurysms
|
|
|
3cm-3.8cm=dilation
>3.8-suggests aneurysm 4.5cm-6cm=surgical consult >7cm=immediate consult |
Abdominal aortic size
|
|
|
abdominal ultrasound
CT |
diagnostic for aneurysms
|
|
|
second m/c site for arterial calcification
easy to recognize may undergo aneurysmal changes second to abdominal aorta |
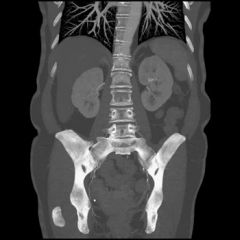
iliac artery calcification
|
|
|
arise fm abdominal aorta at or near L1 and extend laterally
athersclerosis or diabetes typically aorta calcified as well |
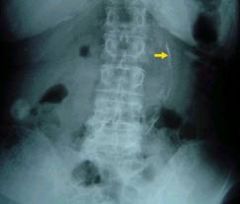
renal artery calcification
|
|
|
frequently calcifies
serpentine course in LUQ very tortuous (may appear ringlike) may be dilated or aneurysmal |
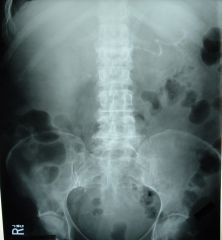
splenic artery
|
|
|
duct that carries sperm fm epididymis to urethra
m/c associated w/diabetes bilateral/symmetric forms "V" shape parallels pubic rami |
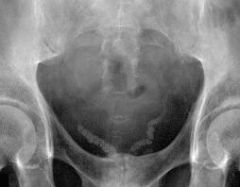
vas deferens calcification
|
|
|
calcium deposition w/in wall of abdominal fluid filled structure
smooth, curvilinear rim opacity complete or incomplete borders displace or distort adjacent vessels/organs |
cyst wall calcifications
|
|
|
2/3 splenic cysts caused by echinoccocus (hydatid cyst disease)
uncommon in US accidental oral ingestion of eggs cysts form in solid organs:liver, spleen, lung, brain may have daughter cyst |
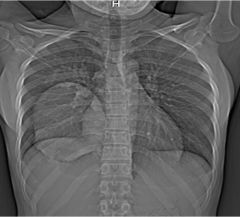
echinococcal cyst (hydatid)
|
|
|
calcification of gallbladder wall
d/t chronic inflammation females ages 38-70yrs 10-20% develop gallbladder carcinoma usually aggressive poor prognosis |
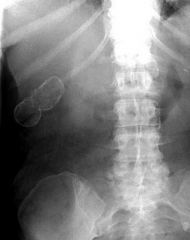
porcelain gallbladder
|
|
|
most diverse presentation of abdominal calcifictions
irregularly calcified borders & complex internal architecture may occur anywhere in abdomen central or peripheral , adjacent to or w/in organs |
solid mass calcification
|
|
|
4 standard differential for masses
|
calcified mesenteric lymph nodes
leiomyoma dermoid cyst (teratoma) injection granulomas |
|
|
occur along broad arch fm LUQ to RLQ w/in small bowel mesentery
multiple of varied sz TB and Histoplasmosis m/c causes |
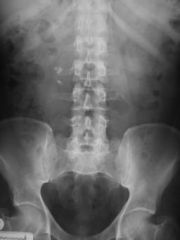
Mesenteric lymph node calcification
|
|
|
m/c women
usually occur in uterus can be anywhere benign tumor of smooth muscle whorled type of calcification or flocculant may demonstrate prominent bordering rim |
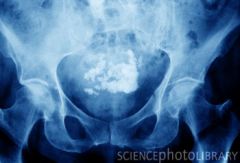
Leiomyomas
|
|
|
subcutaneous fat necrosis secondary to intramuscular injections
m/c in hip soft tissue solitary or multiple calcific spheres |
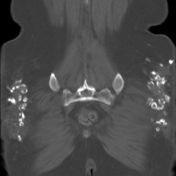
injection granulomas
|
|
|
stone baby
calcified fetus body could not resorb |
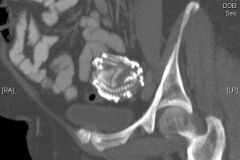
lithopedion
|
|
|
Stands for kidneys, ureters and bladder
Represents the “standard” radiograph Sometimes referred to as a flat plate 70kVp if looking for calcification 90kVp if looking for a mass |
KUB study
|
|
|
Taken with the same parameters as the KUB
Only the patient is lying on the abdomen (prone) PA is anterior anatomy while a KUB is designed for the posterior anatomy |
PA abdominal study
|
|
|
The very best to demonstrate free intra-abdominal air is the PA chest (erect)
Air will travel to the location of least resistance Fluid will gather in the most gravity dependent area |
pneumoperitoneum study
|
|
|
Patient lays on their side with their back up against the film
Patient should be on their side for a minimum of 5 minutes before exposure Left Best demonstrates free air within the abdominal cavity in the area of the liver in the RUQ |
Lateral Decubitus Position
|
|
|
Taken just like an AP lumbar film
70 kVp for calcifications 90 kVp for masses Fluid sinks down to the pubic area Air travels up to the diaphragms |
AP Abdomen—Erect
|
|
|
Patient lays on their back with their side up against the film
Looks just like a lateral lumbar Asses for free air/fluid and aneurysms |
Dorsal Decubitus
|
|
|
Abnormal gas and mucosal patterns
Morphological abnormalities of the anatomy Abnormal calcifications Abnormal fluid (ascites) Bone and joint abnormalities Post-operative changes |
Pathological Considerations of abdomen
|
|
|
Mostly located in the LUQ
Identified by the gas content or meganblase (gastric air bubble) Relatively fixed position at the gastroesophageal junction while the rest is fairly mobile |
stomach
|
|
|
Duodenum is primarily a fixed retroperitoneal structure
The descending (2nd) portion is closely associated with the head of the pancreas Typically does not contain enough air to be visualized on plain film radiographs Valvulae conniventes– are the circular folds |
small intestine
|
|
|
Relatively well visualized because of its gas content
Haustra (semilunar folds) Cecum usually found in the RLQ Can be mobile Ascending and descending portions are retroperitoneal The rectum typically is seen with air within it Presacral space—the distance between the anterior cortex of the sacrum to the posterior margin of the recutum Should not exceed 2cm in adults Exception in the extremely obese Causes for increased: inflammation, ascites, blood, neoplasm Seen on a lateral image |
large intestine
|
|
|
Generally not seen unless pathological
Diagnostic ultrasound is the preferred method of investigation CT has also been shown to be more sensitive and accurate Traditional located in the RLQ |
appendix
|
|
|
RUQ
Homogenous water density There should be no gas separation between the liver and right hemidiaphragm or within the liver Reidel’s lobe: Congenital anomaly Vertical elongation of the inferior margin May extend down to the iliac crest Common in tall thin females (3-30%) |
liver
|
|
|
Closely associated with the anteroinferior aspect of the liver
One of the more common sites for abnormal abdominal calcifications (cholelithiasis) wall calcification may result in carcinoma Not always visualized RUQ There is some variability |
gallbladder
|
|
|
One of the more difficult organs to visualize
Head lies within the duodenal loop The tail projects posteriorly and to the left Chronic pancreatitis may demonstrate calcficiations |
pancreas
|
|
|
Located within the LUQ
Superiorly it is bordered by the left hemidiaphragm Only the lower pole casts a shadow on the radiograph Vertical Height (8-12cm) Measure 2cm up from the inferior pole for the horizontal measurement Measurement should be no more than 4cm When enlarges it will travel in an anterior and inferior direction Measurements on plain film radiographs are not completely accurate |
spleen
|
|
|
Bean-shaped
Located with in the retroperitoneum Slight medial inclination towards the upper poles Patient position and respiration can change the position Superior pole is found at T12/L1 The length is no more than the combined height of 3.5 vertebral bodies Left sits higher than right by 1-2cm Dromedary Hump: Seen on the left Caused by the spleen pushing on the side creating a “hump” |
kidneys
|
|
|
Bilateral V-shaped organs
Superior and somewhat anterior to the superior poles of the kidneys Not demonstrated on plain film normally |
adrenal glands
|
|
|
Not normally seen on plain film
Retroperitoneal Most common site for symptomatic calculi Three common sites for calculi to lodge Ureteropelvic junction The point where they cross the bifurcation of the iliac artery Ureterovesicular junction |
ureters
|
|
|
Comes off the transverse processes of T12 and descends to the iliac crest
What is actually seen is the interface between the actual muscle and the fat surrounding it Non-visualization may reflect serious disease like inflammation or ascites as well as benign reasons Excessive overlying gas Curvature of the spine Lack of surrounding fat |
Psoas shadow
|
|
|
Outlines the margins of the abdomen lateral to the ascending and descending colon
It appears as a lucent line separating the soft tissues of the skin from the abdominal cavity This line is often obliterated in inflammatory conditions of the abdomen such as Appendicitis Peritonitis |
flank stripes
|
|
|
Seen as a water density immediately superior to the pubic symphysis
In females, the uterus may lay against the superior aspect causing an indentation |
bladder
|
|
|
Located in the pelvic bowel
Between the rectum and bladder Seen only if it indents the bladder May contain calcifications within uterine fibroids |
uterus
|
|
|
Located in the pelvic bowel
Exact location varies Not typically seen on plain film |
ovaries
|
|
|
Located with in the pelvic bowel
Not visualized unless calcified Most often seen in diabetic patients male |
vas deferens
|
|
|
Lies just above the pubic symphysis
Normally not seen Calcifications from prior inflammation male |
prostate
|
|
|
Runs along the left anterolateral aspect of the lumbar spine
Bifurcates into the iliac arteries at approximately L4/L5 Calcification more common in elderly Upper limits of normal is 3.5cm |
abdominal aorta
|
|
|
Branch at L4/L5
Extend down and out to the groin Common site for calcification |
common iliac
|

