![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
107 Cards in this Set
- Front
- Back
|
Delivery system that begins and ends at heart |
Blood vessels |
|
|
Arteries |
Carry blood away from the heart |
|
|
Capillaries |
Contact tissue cells that directly serve cellular needs |
|
|
Veins |
Carry blood towards the heart |
|
|
Central blood containing space in the blood vessels |
Lumen |
|
|
3 wall layers in blood vessels |
Tunica intima Tunica media Tunica externa |
|
|
Capillaries have ____ with sparse basal lamina. |
Endothelium |
|
|
Tunica that contains the endothelium. |
Tunica intima |
|
|
Tunica media |
- smooth muscle and elastin |
|
|
Smooth muscle of Tunica media is regulated by _______. For what? |
Sympathetic vasomotor nerve fibers to allow Vasoconstriction or Vasodilation. |
|
|
Tunica externa |
-Collagen fibers (anchors) -Contains nerve fibers & lymphatic vessels - Vasa vasorum |
|
|
How do vessels vary? |
- length - Diameter - wall thickness - tissue makeup |
|
|
The blood vessels of the blood vessels |
Vasa Vasorum |
|
|
When vascular smooth muscle contracts, what happens to the diameter of the blood vessel? what is this called? |
vasoconstriction |
|
|
Types of arteries |
1. Elastic arteries 2. muscular arteries 3. arterioles |
|
|
What are the elastic arteries? |
- large thick-walled arteries with large lumen - contain elastin in all three tunics - Aorta and its major branches |
|
|
T or F Elastic arteries act as pressure reservoirs |
True smooth pressure downstream |
|
|
T or F Elastic arteries are active in vasoconstriction. |
False, they can't because aorta feeds all of body. |
|
|
Muscular arteries |
- deliver blood to body organs - thick Tunica intima with more smooth muscle |
|
|
T or F Muscular arteries are active and vasoconstriction |
True |
|
|
Smallest arteries |
Arterioles |
|
|
Arterioles |
Control flow into capillary beds via vasodilation and vasoconstriction |
|
|
Microscopic blood vessels |
Capillaries |
|
|
cells that stabilize the capillary wall and help control capillary permeability |
Pericytes |
|
|
Most tissues have capillaries, except: |
Cartilage (avascular) Epithelia Cornea & lens of eye |
|
|
T or F Capillaries provides direct access to almost every cell |
True |
|
|
Function of capillaries |
Exchange between blood and interstitial fluid |
|
|
Types of capillaries |
1. Continuous capillaries 2. Fenestrated capillaries 3. Sinusoid capillaries |
|
|
Capillaries abundant in skin and muscles |
Continuous capillaries |
|
|
Continuous capillaries are joined together by ______, which leave gaps called _____. |
Tight junctions Intercellular cleft |
|
|
Continuous capillaries in the brain. |
Have complete tight junctions That form the blood-brain barrier. |
|
|
Where are fenestrated capillaries found? |
In areas where active capillary Absorption or Filtrate formation occurs. (Ex: kidneys, Intestines, Endocrine glands)
|
|
|
Sinusoid capillaries characteristics. |
larger lumen Fenestrated Fewer tight junctions Larger Intercellular clefts |
|
|
which capillaries has the most leakage ? |
Sinusoid capillaries |
|
|
Where can you find sinusoid capillaries |
Liver Bone marrow spleen adrenal medulla |
|
|
Sinusoid capillaries have a lot of cells called_____. |
Macrophage |
|
|
Interwoven networks of capillaries between arterioles and venules |
Microcirculation |
|
|
Vascular shunt |
Directly connects terminal arterial and postcapillary venule |
|
|
True capillaries |
- Turn 10 - 100 exchange vessels per capillary bed - branch off metarteriole or terminal arteriole |
|
|
Regulate blood flow into true capillaries. How? |
Precapillary sphincters Through vascular shunt or into true capillaries |
|
|
Precapillary sphincters are regulated by what |
Local chemical conditions and vasomotor nerves |
|
|
Venules characteristics |
-Very porous -allow fluids and WBC into tissues -endothelium -few pericytes |
|
|
Veins are called _________, because they can hold up to 65% of blood supply. |
Capacitance vessels |
|
|
T or F The blood pressure, in veins is higher than arteries. |
False, it's lower |
|
|
T or F Adaptations ensure return of blood to heart despite low pressure in veins. |
True |
|
|
Venous valves are most abundant in _____. |
Veins of limbs. |
|
|
Venous sinuses |
Flattened veins with extremely thin walls (Ex: coronary sinus of heart) |
|
|
* Arterial anastomoses |
Interconnection of blood vessels which provides alternate pathways |
|
|
Where would you find arterial anastomoses? |
Joints Abdominal organs Brain Heart |
|
|
T or F arteries that supply the retina kidneys and spleen have arterial anastomoses. |
False They do not have arterial anastomoses |
|
|
What is an example of arteriovenous anastomoses. |
vascular shunt of capillaries |
|
|
T or F Venous anastomoses are very common |
True |
|
|
Volume of blood flowing through vessel, organ, or entire circulation in a given period. |
Blood flow |
|
|
Blood pressure |
Force per unit area exerted on wall of blood vessel by blood |
|
|
Instrument used to take BP. |
* Sphygmomanometer |
|
|
Place in order: ___ elastic artery ___ Veins ___ venules ___ capillary ___ arterioles ___ muscular artery |
Heart Elastic artery (aorta) muscular artery arterioles capillary beds venules veins Back to heart |
|
|
Peripheral resistance |
(Opposition of flow ) Measure of amount of friction blood encounters with vessel walls. |
|
|
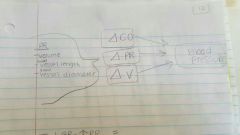
Three sources of resistance in blood flow. |
- Blood viscosity - total blood vessel length - blood vessel diameter |
|
|
Is blood pressure increases then blood flow _____. |
Increases |
|
|
If resistance increases, then blood flow_____. |
Decreases |
|
|
generates blood flow |
Pumping of heart |
|
|
T or F Blood pressure results when flow is opposed by resistance |
True |
|
|
Systemic pressure is highest in the ______, but drops steeply in the _______. |
Aorta Arterioles |
|
|
Types of blood pressure |
Arterial capillary venous |
|
|
What 2 factors do Arterial blood pressure in arteries close to the heart reflect.? |
1. Elasticity 2. Volume of blood forced in them |
|
|
Blood pressure near the heart is _______. |
Pulsatile |
|
|
Pressure exerted in your to dream ventricular contraction. |
Systolic pressure |
|
|
Diastolic pressure |
Lowest level of aortic pressure |
|
|
The difference between systolic and diastolic pressure. |
Pulse pressure |
|
|
Mean arterial pressure (MAP) |
Pressure that propels blood to tissues |
|
|
______ and ________ both decline with increasing distance from heart. |
MAP Pulse pressure |
|
|
Throbbing of arteries |
Pulse pressure |
|
|
What would happen to a capillary if the BP was high. |
High BP would rupture capillaries |
|
|
T or F Venous blood pressure is very high due to resistance. |
False, BP is very low |
|
|
Factors that increase venous return |
1. muscular pump 2. respiratory pump 3. Venoconstriction |
|
|
Main factors that influence BP |
- Cardiac output (CO) - peripheral resistance (PR) - Blood volume |
|
|
What affects blood pressure? |
PR blood volume Co |
|
|
Short term control of blood pressure |
Neural and hormonal controls How: counteract fluctations in BP by altering peripheral resistance and CO |
|
|
long term control of BP |
Altering blood volume Ex: hydrated= more blood volume VS |
|
|
Neural controls operate via ____. |
Reflex arcs |
|
|
Locations of Baroreceptors |
- carotid sinuses - Aortic arch - walls of large arteries of neck and thorax. |
|
|
How do baroreceptors work if there's an increase in BP. |
- stimulate cardioinhibitory center - increase input of vasomotor center for vasodilation = decreased BP |
|
|
Detect abnormal BP |
Baroreceptors |
|
|
Decrease in Blood pressure is due to ... |
- arteriolar vasodilation - venodilation - decreased CO |
|
|
If MAP is low what happens? |
Reflex to vasoconstriction ➡ Increased CO➡ Increased BP |
|
|
T or F Baroreceptors are never ineffective. |
False, ineffective if altered BP sustained |
|
|
Detect increase in CO2 or drop in pH or 02 |
Chemoreceptors in aortic arch and large arteries of neck. |
|
|
How do chemoreceptor reflexes increase blood pressure? |
- Signal cardioaccelatory center (⤴CO) - Signal vasomotor center (⤴vasoconstriction) |
|
|
T or F The hypothalamus and cerebral cortex modify arterial pressure via relays to medulla. |
True |
|
|
☺ |
|
|
Hormonal controls of BP through adrenal glands. |
Release of epinephrine & norepinephrine = vasoconstriction & increased CO |
|
|
Angiotensin II stimulates _____ |
Vasoconstriction |
|
|
How does atrial natriuretic peptide (ANP) cause a decreased blood volume? |
By antagonizing aldosterone |
|
|
2 ways kidneys regulate arterial blood pressure. |
1. Direct renal mechanism (independent of hormones) 2. Indirect renal mechanism ( renin-angiotensin-aldosterone) |
|
|
Prolong hypertension leads to |
Heart failure vascular disease renal failure stroke |
|
|
Secondary hypertension is caused by: |
- obstructed renal arteries - kidney disease - endocrine disorders (Cushing & hyperthyroidism) |
|
|
Low blood pressure |
Hypotension |
|
|
T or F Acute hypertension is an important sign of circulatory shock that could be a threat for surgical patients. |
False, acute hypotension |
|
|
Hint of poor nutrition and warning sign for Addison's disease or hypothyroidism |
Chronic hypotension |
|
|
Orthostatic hypotension |
Temporary low BP and dizziness when suddenly rising from sitting or reclining position |
|
|
High ADH levels cause _____. |
Vasoconstriction |
|
|
High ADH cause an increase in the number of ____. |
Aquaporins |
|
|
What hormone lowers blood pressure and how.? |
Atrial natriuretic peptide (ANP) Decreases blood volume by antagonizing aldosterone. |
|
|
If BP is high are we going to eliminate or retain water? |
Eliminate. And vs |
|

|
Pic |
|
|
4 functions of angiotensin II |
1. Increases blood volume. - stimulates aldosterone secretion - causes ADH release - triggers hypothalamic thirst center 4. causes vasoconstriction directly increasing BP |
|
|
The protein that converts angiotensin 1 |
Renin ** |

