![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
20 Cards in this Set
- Front
- Back
|
B cell Activation
|
- Antigen-dependent B cell differentiation/activation is a process by which antigen encounter, in the presence of appropriate T cell help, leads to isotype switching, affinity maturation (somatic mutation), differentiation to antibody secreting plasma cells, and memory B cell formation
|
|
|
Antigen Recognition and Processing
|
- Initiating stimulus for B cell activation is antigen-induced crosslinking of the B cell receptor complex, followed by its endocytosis in a cytosolic endosome
- Endosomes fuse with cytosolic vesicles containing class II major histocompatibility complex molecules (MHC), a peptide/class II MHC complex is formed. - This chimeric endosome translocates to the B cell surface resulting in the display of Class II MHC/peptide on the cell surface. |
|
|
Role of CD4+ T cells
|
- Class II MHC/peptide complex is recognized by activated CD4+ T cells and resulting in a T cell/B cell conjugate that is further stabilized by adhesion molecules
|
|
|
Clonal Expansion
|
- Activated naive B cells undergo clonal expansion that is detectable within 24 hours of immunization.
- Following the initial burst of proliferation, activated B cells and T cells migrate to primary follicles where enhanced proliferation of B cells leads to the formation of germinal centers, the hallmark of secondary follicles |
|
|
Germinal Centers
|
- Associated with B cell clonal expansion, isotype switching, affinity maturation, differentiation to plasma cells, and differentiation to memory B cells
|
|
|
CD40/CD40 ligand interaction
|
- Delivers an essential signal
- Disruption of the T cell gene for the CD40 ligand, or injection of CD40 - prevents steps in the differentiation pathway that results in hyper IgM syndrome (i., there is no isotype switching) |
|
|
Plasma Cells
|
- B cells = antigen specific antibodies as cell surface receptors; plasma cells = antibodies
- Differentiation to the plasma cell stage occurs 4 days after immunization, and is marked by secretion of IgM antibodies |
|
|
Isotype switching (switch recombination)
|
- Cells expressing IgM and IgD are modified at the genomic level such that they produce antibodies of different isotypes (IgA, IgE, or IgG)
- Occurs in germinal centers approximately 1 week after initial B cell activation by T-dependent antigen - Irreversible - Gene encoding the heavy chain constant region is modified |
|
|
Affinity maturation (somatic maturation)
|
- Process that leads to the gradual accumulation, with time after immunization, of higher affinity antibodies for the immunizing antigen
- Gives rise to point mutations -VDJ gene region of both light and heavy chains - Occurs in germinal center 7-10 days following B cell activation |
|
|
Generation of Memory B cells
|
- Differentiation of activated B cells to memory cells occurs in germinal centers, beginning approximately one week after antigenic challenge with a T dependent antigen
- Some memory B cells colonize the secondary lymphoid tissues - Most join the pool of recirculating B cells that circulate from blood, lymph, and tissues that were the primary sites of previous antigen encounter |
|
|
BLyS (B cell stimulator)
|
- Plays a critical role in B cell selection and survival
- BLyS is expressed first as a cell surface protein - upon cell activation, it is cleaved and released as a soluble molecule, which is the more biologically active form - Release of BLyS from monocytes/macrophages and dendritic cells is triggered by cytokines, or by crosslinking of Fc R by IgG, an opsonin. - Signaling via BR3 leads to B cell survival by preventing apoptosis |
|
|
Receptors for BLyS
|
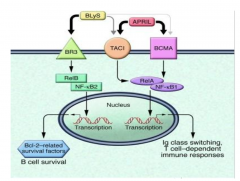
BLyS binds to three different receptors (BR3, BCMA, and TACI) which are present on most peripheral B cells, albeit with different affinities, with interaction with BR3 providing the greatest affinity
|
|
|
Abnormal BLyS
|
- Abnormal production of BLyS alters immune tolerance by allowing the survival of autoreactive B cells, thus triggering autoimmune disorders.
- Serum levels of BLyS have been reported in patients with rheumatoid arthritis (RA), systemic lupus erythematosus (SLE), or multiple sclerosis. |
|
|
B cell Regulation
|
Down regulation of B cell activation has been shown to require colligation of Fc RIIB-IgG/antigen
|
|
|
Negative Signaling in B cells
|
- Inhibition of B cells following antigen induced activation
- Negative signaling occurs when secreted IgG crosslinks the membrane bound antibodies (same specificity) with the integral membrane receptor, FcγR (the low affinity FcγR ) |
|
|
B cell Activation: Secondary Responses
|
- Secondary exposure to the same antigen induces the activation and differentiation of memory B cells, generating a secondary immune response
- Secondary immune responses may be initiated outside of secondary lymphoid tissues. - During secondary responses, B cell proliferation is detected much sooner, and the number of progeny is nearly one log greater than that generated in a primary immune response |
|
|
B cell Responses to T-independent Antigens
|
T independent (T-indep) antigens are antigens that can induce naive B cell activation in the absence of cognate interaction with T cells (i.e., T cell help). B cell activation, in response to T-indep antigens, leads mainly to IgM production
- e.g. lipopolysaccharide (LPS) |
|
|
Adjuvants: Enhancing Immunogenicity of Monoclonal Activators
|
- Alum precipitate, a suspension of aluminum hydroxide mixed with antigen, is used in human vaccines to enhance immunogenicity.
- Alum is thought to cause the slow release of antigen, such that the presentation of antigen to T cells is prolonged. - A common adjuvant used in studies with laboratory animals is Freund’s complete adjuvant (water in oil emulsion and killed Mycobacterium tuberculae). |
|
|
Polyclonal Activators
|
- Mitogens are naturally occurring molecules that have the capacity to bind to, and trigger proliferation of many clones of lymphocytes.
- B cells mitogens: pokeweed mitogen, high concentrations of lipopolysaccharide (important: at low concentrations it is a T-independent antigen) - T cell mitogens: concanavalin A (Con A), phytohemagglutinin (PHA), and pokeweed mitogen (PWM). Con A and PHA are plant glycoproteins, more commonly called lectins that bind carbhydrate molecules (sugars). |
|
|
Oligoclonal Activators
|
- Superantigens activate subsets of T cells
- Antigen specific but non-polyclonal (oligoclonal) fashion on T cells - These molecules bind specifically to regions of the T cell receptor termed Vβ |

