![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
25 Cards in this Set
- Front
- Back
|
what is the function of bone |
Structural -support -protection -movement Mineral storage -Calcium -Phosphate |
|
|
does cortical/compact/tubular bone have a low or high metabolic activity/turn over rate |
low metabolic activity and turn over rate |
|
|
does cancellous/spongy/trabecullar bone undergo more or less remodelling than cortical/compact/tubular bone |
more |
|
|
does cancellous/spongy/trabecullar bone have a low or high metabolic activity/turn over rate |
high metabolic activity and turn over rate |
|
|
what are the different section that make up bone |
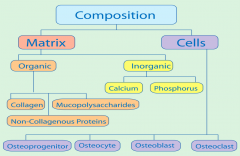
|
|
|
what is another name for the epiphyseal growth plate |
physis |
|
|
what is the structural advantage of having a physis |
Allows remodelling of angular deformity after fracture |
|
|
if the physeal blood supply is damaged what will this result in |
will lead to growth arrest (either partial or complete) |
|
|
what are the 2 types of fracture healing |
direct (primary) indirect (secondary) |
|
|
what is direct fracture healing |
‘Direct formation of bone, without the process of callus formation, to restore skeletal continuity’ ‘Direct formation of bone, without the process of callus formation, to restore skeletal continuity’ |
|
|
what are the 4 steps of indirect fracture healing |
-Haematoma +Inflammation -Soft Callus -Remodelling |
|
|
how does indirect fracture healing occur |
via callus formation, through IRR
‘Formation of bone via a process of differential tissue formation until skeletal continuity is restored’ |
|
|
what is the first step of fracture healing |
1. Fracture haematoma and inflammation – blood from broken vessels forms a clot. – 6-8 hours after injury – swelling and inflammation to dead bone cells at fracture site |
|
|
what is the second step of fracture healing |
Fibrocartilage (SOFT) callus (lasts about 3 weeks) – new capillaries organise fracture hematoma into granulation tissue - ‘procallus’ – Fibroblasts and osteogenic cells invade procallus. – Make collagen fibres which connect ends together – Chondrocytes begin to produce fibrocartilage, |
|
|
what happens when the bony (HARD) callus formation |
occurs during week 3 and lasts 3-4 months basically.....osteoblasts make woven bone |
|
|
what happens during the bone remodelling stage of indirect fracture healing |
Osteoclasts remodel woven bone into compact bone and trabecular bone |
|
|
do bones need a blood supply to heal |
YES...obviously |
|
|
does a fracture injure the bone blood supply |
yes |
|
|
does surgery damage the bone blood supply |
yes |
|
|
what portions of the bone do the endostium and periosteum supply |
Endosteal Periosteal |
|
|
give an example of a place where a problem with the blood supply leads to necrosis (bone death) |
Proximal pole of scaphoid fractures Talar neck fractures Intracapsular hip fractures Surgical neck of humerus fractures |
|
|
what factors inhibit fracture healing |
Patient Factors: Medication: (remember these INHIBIT healing) * |
|
|
why are NSAIDs said to inhibit fracture healing |
they reduce vascularity at the sight of fracture helaing |
|
|
are cox-2 NSAIDs thought to be more on less inhibitive than other non-specific NSAIDs |
more inhibitive |
|
|
how do biphosphonates inhibit fracture healing |
they inhibit osteoclastic activity and therefore delay fracture healing as a result
btw biphoshonates have a long half life...js |

