![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
56 Cards in this Set
- Front
- Back
|
General description of vitamins (Purpose/Structure/Function) |
-Support nutritional health (small amts needed for proper body function) -Organic, macronutrients -Work as individual units (don't form polymers) -Assist other enzymes (No E received from their catalysis) |
|
|
1) What is one way that vitamins are categorized? 2) Why is this important? |
1. Solubility. -Water Soluble (B Vits & C Vits) -Fat Soluble (Vits DEAK) 2. Solubility affects absorption, transport, excretion, and storage -Water soluble: Move directly into blood, excess is peed out -Fat soluble: Enter lymph, then blood (many require transport protein in blood). Require bile for digestion & absorption Fat soluble is stored in liver and adipose tissue more than water sol., so water sol. must be eaten more regularly (Fat sol. will lead to more toxic outcomes b/c we already have a certain amt stored) |
|
|
B1 |
Thiamine Needs to be pyrophosphorylated to be functional (Funct. form=Thiamine pyrophosphate (TPP)) |
|
|
What are 4 types of rxns is Thiamine involved in? |
-Carboxylase/decarboxylase rxns (most important) -Transferase rxns -Synthesis of acetylcholine and GABA (GABA binds to receptor stimulating IPSP, hyperpol) -Important in conversion of pyruvate to acetyl-CoA |
|
|
How can we become deficient in B1? |
Malnourished, alcoholic (ethanol inhibits absorption and TPP formation), prolonged cooking destroys thiamine, thiamine leaches into H2O when boiling food |
|
|
What 2 diseases are associated with Thiamine deficiency? |
1.Wernicke-Korsakoff Syndrome shows up in alcoholics (Sxs: loss of appetite, depression, unsteadiness, memory loss, abnormal walk/stance) 2. Beriberi (2 forms) -Dry: effects PNS (sensory, motor, reflex impairment) -Wet: effects cardiovascular system (one form is rarely seen w/out the other) |
|
|
B2 |
Riboflavin -Flavin aspect of: FMN (Flavin Mononucleotide) FAD (Flavin adenine dinucleotide) |
|
|
What type of rxns is Riboflavin involved in? |
Redox rxns, 2 e-s transferred |
|
|
What happens if there's a deficiency in B2? |
-Oral, ocular, genital manifestations (Angular chelitis (inflammed around mouth), photophobia (sensitivity to light), scrotal dermatitis) |
|
|
What can destroy Riboflavin? |
-Ultraviolet light and irradiation (Ex. Milk in opaque containers) -Not destroyed by cooking |
|
|
B3 |
Niacin -Found in 2 structural forms: Nicotinic acid and Nicotinamide (<-one normally found in blood) Both forms can be converted into the other -Niacin is used in metabolic rxns (redox rxns, transfer of 1e-) Ex: NAD, NADP -Niacin is made by consumption and by our body ONLY after protein synthesis needs are met, b/c it's made from tryptophan in the liver (B3 is needed from diet, bodily production is NOT enough) |
|
|
1. What are the cofactors needed for our body to make niacin from tryptophan? 2. How is this related to Niacin deficiency? |
1. Thiamine, Riboflavin, Iron, Vit B6 2. If you're deficient in any one of these, Niacin deficiency can occur IF you aren't getting B3 through diet or supplements |
|
|
What happens if we don't have enough Niacin?
|
-Pellagra: (4Ds) Diarrhea, Dermatitis, Dementia, Death -Hartnup's Disease: Defect in the kidneys and intestines - they can't absorb or reabsorb tryptophan -Other sxs: nausea, Skin&mouth lesions, anemia, tiredness (B3 is involved in NAD, which is involved in E production) |
|
|
B3 Toxicity |
Niacin Flush -Red rash -Itchy tingly sensation -W/prolonged B3 consumption, it can be painful Toxicity caused by supplements that cause high levels of nicotinic acid |
|
|
B5 |
Pantothenic Acid -Part of Coenzyme A (CoA) chem. structure -Very rare to have deficiency & toxicity |
|
|
Which vitamin is directly effected by alcohol consumption? |
B1 (Thiamine) |
|
|
B6 |
Pyridoxine (3 forms - all can be phosphorylated) -Pyridoxal (Functional one) -Pyridoxine (Most common in diet) -Pyridoxamine Functional form: PLP (pyridoxal phosphate) |
|
|
What types of rxns is Pyridoxine involved in? |
-a.a. metab. (Transamination/deamination, transfer/removal of a.a. groups) -Glycogen metabolism -Conversion of tryptophan to niacin or serotonin -Synthesis of heme, nucleic acids, & some lipids |
|
|
How can [B6] be effected?/What can B6 deficiency cause? |
-Dietary deficiency is rare -B/c B6 is important for trans & deamination, if we consume a high protein diet, we'll need to take in more B6 (need more pyridoxine) If you don't consume more B6, you experience depression, irritability, and confusion -Alcohol & isoniazid (med for TB) effect ability to take up B6 -Low B6 can cause low B3 |
|
|
B6 toxicity |
Only comes from supplementation, which can cause irreversible nerve degradation causing pain and numbness in extremities |
|
|
B7 |
Biotin Coenzyme that carries activated CO2 |
|
|
What rxns is Biotin involved in? |
-Carboxylase & decarboxylase rxns -TCA cycle/citric acid cycle -Gluconeogenesis -Fatty acid synthesis -Participates in synthesis of isoleucine and valine |
|
|
Biotin deficiency |
-Very rare -Can be induced. Eat 2 raw egg whites daily for several months. Egg whites have a protein that binds biotin -Sterile intestinal tract can cause it (GI bacteria produce biotin) |
|
|
B9 |
Folate/Folic Acid (2 active forms) -Dihydrofolate (DHF) and tetrahydrofolate (THF) -Transfers single carbon componenents during metabolism (Ex: methyl groups) |
|
|
What rxns is folate involved in? |
-Converting B12 to active coenzyme form -Production of nucleotides -Aids in cell division, specifically of fetus -Important in RBC formation (b/c they require a lot of DNA) |
|
|
What happens if not enough B9 around? |
Since it usually prevents neural tube defects (Spina Bifida), folate supplementation should be taken 1 month before conception -However ~50% of pregnancies are unplanned, so US gov fortified grain products w/folic acid -Fortification did lower Spina Bifida occurrence, but can mask VitB12 deficiency (usually B12 helps activate folate) |
|
|
B12 |
Colbalamin -Usually B12 is w/in a protein. To get B12 out of protein to be absorbed/used, our stomach acid denatures protein -In the small intestine, cells release intrinsic factor protein that binds B12. ONLY upon binding can our cells take up B12 -B12 is recycled; if we stopped eating meat today, we could last about 6 yrs before seeing a deficiency -We store some B12 in liver (one of the only water soluble vits that is stored) |
|
|
What rxns is B12 involved in? |
-B12 & Folate depend on each other for activation (Unactive forms: B9 methyl., B12 unmethyl; so B9 can give a methyl to B12 and they both become activated) However, B9 can be activated through interaction w/other molecules, while B12 can ONLY be activated by folate. So, if you have a B9 deficiency, you'll have a B12 deficiency -Regeneration of methionine -Synthesis of fatty acids -Synthesis of DNA & RNA |
|
|
Why do vegans need supplementation for B12? |
No B12 is made by plants. B12 can't be received from their diet b/c we only get it from animal sources whose bacteria in their digestive system made B12 |
|
|
Cobalamin deficiency |
Pernicious anemia (type of megloblastic anemia/RBCs look huge); one cause is that B12 isn't there to help activate folate (needed for RBC production) |
|
|
How can you get B12 deficiency? |
-Inadequate absorption/lack of HCL or intrinsic factor -Vegan diet -Excessive alcohol intake (dec. GI absorp.) -Tape worms -Folate supplementation can mask B12 deficiency |
|
|
If someone is B12 deficient because they can't produce intrinsic factor, would giving them B12 supplement help? |
No, b/c they still can't bind B12 to allow it to absorb in small intestine |
|
|
Vitamin C, what rxns is it involved with? |
-#1 role: antioxidant (inhibits ox. of molecules) defends against ROS - reactive oxidation species -Involved in redox rxns (protects against free rads by grabbing extra e- from them) -Deactivates histamine |
|
|
What happens if you have a VitC deficiency? |
-ROS present at high levels -Scurvy (could take 1-6 months to appear): Gum bleeding around teeth and capillaries under skin break easily -Smokers require more VitC |
|
|
Vitamin C |
Ascorbic Acid -Cofactor in collagen formation (matrix for bone and tooth formation) -Cofactor in other rxns Conversion of tryptophan to serotonin Conversion of tyrosine to NE |
|
|
Vitamin A |
-Stored in the liver (1-2yrs worth) -Precursor form = beta carotene (cutting beta carotene in half produces 2 VitAs, spec. Retinal) -There are 3 forms: Retinol, Retinal, Retinoic Acid (together called the retinoids, each has a diff. bodily function) Retinol: supports reproduction Retinal: Vision Retinoic acid: growth regulation |
|
|
Vitamin A in animals/plants vs our body |
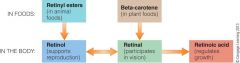
We get VitA from animals in more stable form, retinyl esters. We store it as retinyl esters in our body also. Beta-carotine is the plant form. Our body converts rentinyl esters to retinol and beta carotine to retinal. Retinol & retinal can be converted into one another. Retinal can convert into retinoic acid, can't go back. |
|
|
Describe vitA in blood |
-Needs a transport protein=retinol binding protein (RBP) -Cell receptors for vitA take them from blood to cell as it circulates |
|
|
Retinal |
-Form of vitA -Helps maintain a clear cornea/crystal clear window -Helps with retina (photosenstive cells, made up of rhodopsin = opsin & retinal, when light hits rhodopsin, it goes from cis conf. to trans/linear form, this causes opsin to change shape and opsin interacts w/cell membrane, stimulates signal sent to brain to say we say light/have vision) |
|
|
Retinoic Acid |
-Form of VitA -Binds to cytoplasmic retinoic acid receptor after entering cell, together they act as a transcription factor (can turn on genes-retinoic acid response elements) -Important in making and producting skin and mucosal cells |
|
|
Retinol |
-Important in reproduction & growth, spec. sperm dvlmnt, normal fetal dvlmnt, growth of children (bone remodeling=VitA helps in dismantling) |
|
|
Beta-caotene |
-Precursor of VitA -By itself, has antioxidant function, helps to protect from ROS |
|
|
VitA deficiency |
-More susceptible to infectious diseases (b/c its important in protein synthesis, antibodies) -Night blindness (not enough retinal to retina, ppl don't quickly recover from bright flash) -Blindness/xerophthalmia (lack of VitA to front of eye - opaque, cloudy cornea) |
|
|
VitA Toxicity |
-Only develops when our retinol binding protein is full, then the other VitA is free floating, which acts as an oxidant and damages cells -Comes from supplements, foods high in VitA, fortified foods, pre-formed vitA from animal sources (already converted to retinal) -Wknd bone (VitA promotes dismantling/VitA can interfere with VitD) -Birth defects (cell death in spinal cord; ppl using actutane/Retin-A need to have preg. test before) -Usually conversion of beta-carotene to VitA is insufficient for toxicity, but if we overconsume beta-carotene in supplements, it can go from antioxidant to pro-oxididant (it can produce O2 radicals). If we overconsume from food, we can have yellow skin (not harmful) -Children are more vulnerable (they're small) |
|
|
Vitamin D |
-Non-essential nutrient -Two things needed to start VitD production: 1. Sunlight starts process of turning 7-DHC in skin to pre-VitD 2. Add some OH groups ( 2 hydroxylation rxns), occurs in liver and kidneys |
|
|
VitD toxicity |
-No toxicity can come from too much sun b/c sunlight degrades VitD precursor w/prelonged exposure (will degrade pre-VitD) -We only need 5-10 mins in summer sun 2-3 times/wk; what can effect time? Skin color, latitude, season, time of day |
|
|
What does VitD do in our body? |
-Works as a hormone -If blood Ca2+ levels low>PTH activated>VitD activated>VitD goes stimulates (1)Kidney Ca reabsorption (2)Intestines: absorb Ca (3)Dismantles bone to release Ca -If high blood Ca2+>activates calcitonin>blocks VitD>(1)Kidneys pee out Ca (2)Intestines don't need to absorb Ca (3)Bone reassembles - Ca added to bone |
|
|
Causes of VitD deficiency |
-Common, but hard to detect by visual obs. -Contributing factors: dark skin, breast feeding w/out supplementation (giving vitD to baby), lack of sunlight, not using fortified milk (vitD helps Ca absorb) |
|
|
What can vitD deficiency lead to? |
-VitD deficiency causes a Ca2+ deficiency -In children, Rickets: bones don't calcify normally (bones bend) -In adults, Osteomalacia: soft, brittle bones (leads to osteoporosis) |
|
|
VitD toxicity |
-Most likely to have toxic effects, esp. in children -Cause: Supplements -Too much vitD, raises blood Ca conc. (leads to formation of kidney stones, hardened BVs, can cause death) |
|
|
Which form of VitA are animal derived vitA precursors converted to? |
Retinol |
|
|
Vitamin E |
-Part of cmpd group tocopherol -There are 4 types, only alpha form is active in humans -Acts as antioxidant, esp. for lipids-stops free radicals from producing more radicals, protects cells and their membranes, Helps w/heart disease-protects against LDL & reduces inflammation -Liver regualates VitE concentration |
|
|
VitE deficiency |
- Primary deficiency is rare (from diet) - Secondary deficiency can occur (Ex. can't absorb fat b/c of cystic fibrosis) - RBCs can break open (erythrocyte hemolysis) b/c lipids in membrane are damaged -Thrombocytosis due to cell lysis -Edema - water flows to solutes released from cell lysis |
|
|
VitE toxicity |
-Comes from supplementation -Extremely high doses can interfere with VitK which can lead to hemorrhages (VitK usually stops hemorrhages) |
|
|
Vitamin K |
-Helps with blood clotting (activates some clotting factors 2, 7, 9, 10, and thrombin). To activate, Glutamate residues of factors must be carboxylated (CO2 added). VitK helps w/addition -Metab. of bone proteins, spec. osteocalcin, which helps with amt of Ca in bones (must have CO2 added to Glu to be functional) If low in VitK, you'll have a low bone density b/c not enough Ca put into bones |
|
|
VitK deficiency |
-Primary deficiency is rare b/c GI bacteria make half of our daily amt -Secondary deficiency possible 1. Ex. fat absorption prob. - can't make bile 2. Ex. Some drugs disrupt VitK synthesis & action A) antibiotics (can destroy bacteria making VitK) B) anticoagulants (Warfarin example: warfarin blocks VKORC1-VitK epoxide reductase- so that it can't turn ox. VitK to reduced form = less available vitK/VitK can't be recycled) |

