![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
37 Cards in this Set
- Front
- Back
|
what kind of virus is herpes? what are its general features? what drugs affect herpes? |
enveloped double stranded DNA virus cause acute disease upon infection and then set up a latent state that can become reactivated. immune response will temper primary infection but doesnt stop reactivaton. severity depends on immune status of host no cure but most successful antivirals are nucleic acid analogues |
|
|
which herpes are neurotropic? which are B cell tropic (most people infected)? which are lymphoid tissue tropic? which are lymphocytotropic? |
neurotropic- 1 2 3 (simplex, 2, VZV)- set up latent infections in nerve cells b-cell tropic- 4 (EBV)- hides out in b-lymphocytes lymphoid tissue tropic- 5 (HCV)- hide in lymphoid tissue lymphocytotropic- 8 (KSAV) |
|
|
whats HSV-1? whats the incubation period? what are the symptoms? who does it affect (primary secondary attacks)? |
primary herpetic gingivostomatitis 5 days asymptomatic or tired, unwell, aching muscles, sore mouth and throat, lymphadenopathy, ulceration, gingivitis, crusting lips 1- fit and well usually children if you get it first as an adult more severe 2- immunocompromised |
|
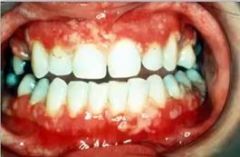
whats this |
HSV 1- primary herpetic gingivostomatitis |
|
|
how do you diagnose and treat HSV-1 and whats the prognosis? |
diag- clinical manage- rest, fluid, anti-pyretics, CHX or chlortetracycline MW, systemtic antivirals only for immunocompromised resolve 10-14 days |
|
|
what do you get is HSV 1 is reactivated? what are the features? how common is it? what are the triggers |
herpes labialis prodromal itch then vesicles burst to form a scab can occur in any pt once infected 3-=40% will have recurrences sunlight, trauma, stress |
|
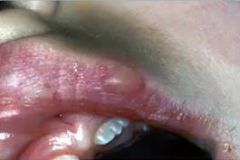
whats this |
herpes labialis |
|
|
how is herpes labialis diagnosed and managed |
clinical avoid predisposing factors topical aciclovir or penciclovit in prodromal phase |
|
|
what is HSV 2? |
can give herpes labialis but more likely to be associated with genital herpes |
|
|
whats HHV3? what are its primary and secondary infections? |
varicella zoster 1- chicken pox 2- herpes zoster |
|
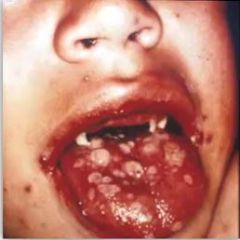
whats this |
chickenpox |
|
|
whats the incubation period of chickenpox and how does it present |
14-21 days itchy rash, sore mouth, malaise, maculopapular rash, ulcers, lymphadenopathy, fever |
|
|
how do you diagnose and treat chickenpox? what advice should you give? whats the prognosis? |
diag clinical manage- rest, fluid, anti-pyretics, antiseptic MW avoid contact with immunocompromised, spread by droplet infection and pt infectious until skin lesions have healed adults more severely infected rare complications are encephalitis and pneumonia |
|
|
what happens when HHV 3 reactivates? who does it affect? has does it present (inc. prodromal phase)? |
shingles over 50s can occur in fit and well and immunocompromised prodromal phase of severe pain 2-3 days then rash (skin) or soreness (mouth) vesicles burst and create ulcers IO or skin rash consistent with distribution of sensory never unilaterally |
|
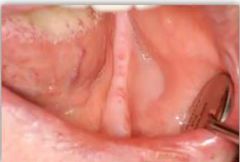
whats this and what nerve |
shingles and trigeminal |
|
|
hows shingles diagnosed and managed? whats the prognosis? whats the condition called that gives persistant facial nerve weakness? |
clinical (mainly, start treatment straight away) or serology manage- high dose systemic aciclovir, referral to ophthamologist (if V1 of trigeminal affected), chlortetracycline MW prognosis- may get post herpetic neuralgia (painful), persistant weakness of facial nerve can occur in ramsey hunt syndrome |
|
|
what causes infectious mononucleosis? who does it affect? whats the incubation period? how does it present? |
epstein barr virus/ HHV4 young adults asymptomatic or feels unwell, tired, fever, tonsilitis, lymphadenopathy, sometimes ulcers |
|
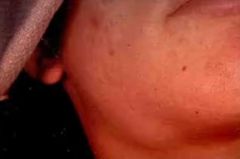
whats this |
infectious mononucleosis |
|
|
how is infectious mononucleosis diagnosed and managed? |
monospot blood test symptomatic only- fluid, antipyretic... |
|
|
what 4 things does EBV/HHV4 cause? |
infectious mononucleosis oral hairy leukoplakia burkitts lymphoma (oncogenic) nasopharyngeal carcinoma (oncogenic) |
|
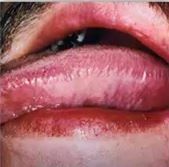
whats this? is it premalignant? |
hairy leukoplakia HHV4 EBV no but is a marker of pt being immunocompromised |
|
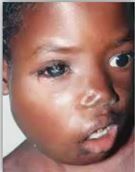
whats this |
burkitts lymphoma HHV4 EBV |
|
|
whats HHV5? what does it cause? who does it usually affect? |
cytomegalovirus rare cause of ulcers but common in AIDS pts |
|
|
whats HHV8? who does it affect? what does it look like? |
kaposi sarcoma (malignant lymphoma) HIV pos or certain groups of ethnic elderly people esp MSM pt often asymptomatic, pigmented nodular appearance often in palate |
|
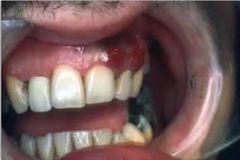
whats this |
kaposi sarcoma HHV8 |
|
|
is coxsackie a herpes virus? what does it cause? what type causes hand foot and mouth? what type causes herpangina? what kind of virus is it? how is it spread? whats the incubation period? |
no hand foot and mouth, herpangina HFM- A 4,5,9,12 herpangina- A 2,4,5,8 positive single stranded RNA faeco-orally 5-7 days |
|
|
what causes hand foot and mouth? who does it affect? whats the incubation period? how does it present |
coxsackie childhood (epidemic outbreaks) 5-7 days ulcers, macith vesiculation on palmer surfaces of hands and feet, malaise |
|
|
how is hand foot and mouth diagnosed and treated? whats the prognosis? |
clinical symptomatic resolves is 7 days |
|
|
what causes herpangina? who does it affect? whats the incubation period? how does it present? |
coxsackie 2-3 days malaise sore mouth and throat, oropharynx ulcerates |
|
|
how is herpangina diagnosed and managed? whats the prognosis? |
clinical symptomatic resolves in 3-5 days |
|
|
what diseases does paramyxovirus cause? what type of virus is it? what treatment is there? |
measles- childhood illness, serious complications of blindness and SSPE, fatality 0.1-10% mumps- childhood illness, serious complications of male sterility, miscarriage in 1st trimester, meningitis, encephalitis and deafness negative single stranded RNA virus effective vaccine (need more than 1 dose) no anit-viral therapy avaliable |
|
|
who does measles affect? how does it present? |
children runny nose, intraoral kopliks spots, bluish grey last 3-4 days followed by maculopapular rash and high fever |
|
|
how is measles managed? whats the prognosis? |
symptomatic rarely encephalitis and pneumonia |
|
|
who does mumps infect? whats the incubation period? how does it present? |
children 14-21 days bilateral parotitis |
|
|
how is paramyxovirus managed? whats the prognosis? |
symptomatic rare complications of pancreatitis, encephalitis, orchitis, oophoritis and deafness |
|
|
what are papillomas? what kind of virus is it? is it destroyed by soap and why? what infect hands and soles of feet? which cause condyloma accuminata? which cause cervical cancer? what do the exclusively replicate in? |
tumour causing viruses (warts) associated with some cancers non-enveloped (lack lipid bilayer, soap normally breaks this but doesnt for papilloma so cant stop infectivity) double stranded DNA hands and feet- 1, 2 condyloma accuminata aka genital warts- 6, 11 cervical cancer (vaccine targets)- 16, 18, 31 replicate in keratinocytes |
|
|
whats verruca vulgaris? whats hecks disease? is there an oral cancer link? |
single common wart (HPV) multiple warts (HPV) no only associated with cancer in the cervix |

