![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
48 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Diffentiate between:
1. Central Nervous System 2. Peripheral nervous system |
CNS is composed of the brain and spinal cord. Peripheral nervous system is the rest of the body, including limbs and dermatome. The basic distinction between the CNS and PNS is that :
1.a) - The CNS is the nerve cells from axon to axon terminal entirely enclosed in a bony cavity – skull or vertebral canal. 1.b) - CNS tissues once damaged do not regenerate 2.a) The PNS has a portion of themselves within the CNS but then exit through the intervertebral foramina and either attach to sensory receptors or to muscles. 2.b) Those tissues of the PNS do regenerate. NOTES: The human nervous system is made up of the following components: * Central Nervous System * Peripheral Nervous System The central nervous system (CNS) comprises the brain and the spinal cord, and controls the vast majority of bodily functions. The peripheral nervous system (PNS) is connected to the CNS, but lies beyond it – it provides a nerve supply to the rest of the body, and relays messages to and from the CNS. |
|
|
|
What is a mixed spinal nerve?
|
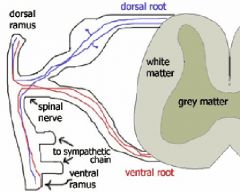
The term spinal nerve generally refers to the mixed spinal nerve, which is formed from the dorsal and ventral roots that come out of the spinal cord. The spinal nerve is the bit that passes out of the vertebrae through the intervertebral foramen.
Mixed nerves have many functional components both somatosensory with links to the sensory endings in tissue. The somatomotor which are motor axons ending on muscle and causing muscle contraction. Associated with each level is a spinal nerve that goes out and with regards to that sensory nerve innervates a band of skin at that level – sensory only. |
|
|
|
How are spinal nerves or mixed spinal nerves formed?
|
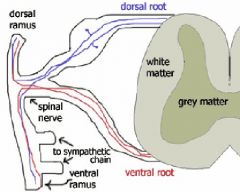
Inside the spinal cord, there is grey matter, surrounded by white matter. From out of the grey matter, two dorsal roots (one on the left side, and one on the right side) and two ventral roots emerge. The dorsal roots contain afferent sensory axons, and the ventral roots contain efferent motor axons.
Dorsal means back, ventral means front. As the body is symmetrical, the same thing happens on both the left and right side of the body. This happens in each vertebra of the spine. The dorsal roots of each side continue outwards, along the way forming a dorsal root ganglion (also called a spinal ganglion). The ventral roots similarly continue out from the spinal column, and meet and mix with their corresponding dorsal nerve root at a point after the ganglion. At this point they are called a mixed spinal nerve |
|
|
|
What is a dermatome?
|
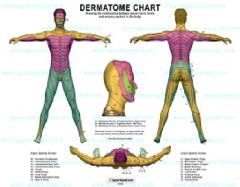
The dermatome is a slice of skin innervated by a nerve. Because of the arrangement of the spinal nerves and innervation of the skin of the body – it is a very important concept.
Dermatomes are the area of skin innervated by a particular dorsal root. The dorsal root is a collection of the sensory neurons for that given peripheral nerve and can contain hundreds of thousands of neurons. A single axon only gets information from a tiny patch from within the dermatome (receptive field). The receptive field is the portion of the dermatome that activates a particular axon. The size of these receptive fields vary for different parts of the body. NOTES: Dermatomic area (also known as a dermatome) is an area of skin that is supplied by a single pair of dorsal roots. An area innervated by peripheral nerves is a peripheral nerve field. The body can be divided into regions that are mainly supplied by a single spinal nerve. There are eight cervical (one for the head, and one for each cervical vertebra), twelve thoracic, five lumbar and five sacral spinal nerves. This innervates the body in a patterned form. Along the thorax and abdomen it is simply like a stack of discs forming a human, each supplied by a different spinal nerve. Along the arms and the legs, the pattern is different: the dermatomes run longitudinally along the limbs. Dermatomes are useful in neurology for finding the site of damage to the spine. |
|
|
|
Why is the dermatomal organization of the spinal cord important?
|
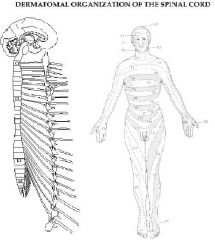
The dermatomal organization of the spinal cord is important because this organization is maintained to the highest levels of the Nervous system i.e. primary somatosensory cortex of the postcentral gyrus also holds this dermatomal organization
|
|
|
|
1. Why is it important to do staining for the spinal cord.
2. What are the 2 types of staining methods used? |
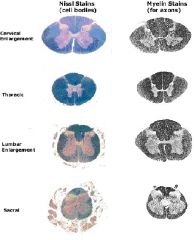
1. Stains are used in order to trace pathways throughout the body.
2. The two types are: A. Myelin stains for axons B. Nissl stains for nissl bodies (discrete granular bodies of variable size that occur in the perikaryon and dendrites, but not axons of neurons) in the cell bodies of the spinal cord |
|
|
|
What is unque about mylein staining?
|

White matter is treated with silver nitrate and this turns the myelin to black even though normally this tissue would appear white
|
|
|
|
Describe the gray matter of the spinal cord?
|
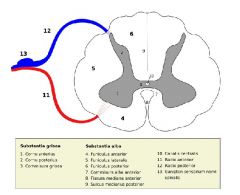
It is located centrally within the spinal cord and it is the butterfly of H-shaped in configuration that varies according to spinal cord level. It is divided into 3 horns or cell coulmns in each side: Dorsal horn, Lateral horn, and Ventral horn. Cell bodies lie in the grey matter at the center – the butterfly.
|
|
|
|
Why is there enlargement of the ventral and dorsal horns?
|
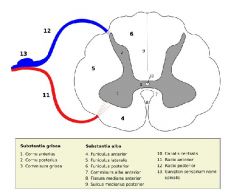
The enlargement of the ventral and dorsal horns is due to increase in number of cell bodies. Innervation of the hands and fingers have many many axons.
NOTES: The actual cord is approxiamately cylindrical in shape, but the diameter varies at different vetebral levels. There are two enlargements, cervical and lumbar. The cervical enlargement is due to the cord segments from C5 to T1 which innervates the upper limb via the brachial plexus. The lumbar enlargement arise from segments L1 to S3 (only the region around L1/L2 is part of the spinal cord proper) and innervates the lower limbs via the lumbar and sacral plexi. |
|
|
|
What is the role of the septum in the spinal cord?
|
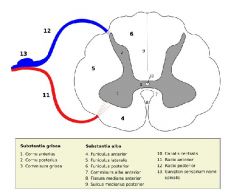
A septum, in general, is a wall separating two cavities or two spaces containing a less dense material. The word is Latin and literally means "something that encloses". (plural: septa). The spinal septum lies between the dorsal and ventral horn and separates the two pathways.
|
|
|
|
What is unique about the thoracic grey matter?
|
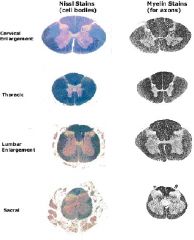
The thoracic grey matter is smaller and rounder due to fewer sensory and motor axons innervating the dermatomes of the thorax. Another features is the medial lateral cell column where the cell bodies are located. The whole thorax comes off the intermediate cell column from T1-T12.
The lumbar enlargement is due to increased cell bodies due to the legs, feet and toes innervation. |
|
|
|
What are nodes of Ranvier and saltatory conduction?
|
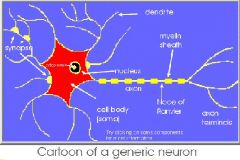
Nodes of Ranvier are regularly spaced gaps in the myelin sheath around an axon or nerve fiber. Saltatory conduction is a means by which action potentials are transmitted along myelinated nerve fibers.
Because the cytoplasm of the axon is electrically conductive, and because the myelin inhibits charge leakage through the membrane, depolarization at one node of Ranvier is sufficient to elevate the voltage at a neighboring node to the threshold for action potential initiation. Thus in myelinated axons, action potentials do not propagate as waves, but recur at successive nodes and in effect hop along the axon, by which process they travel faster than they would otherwise. This process is outlined as the charge will passively spread to the next node of Ranvier to depolarize it to threshold which will then trigger an action potential in this region which will then passively spread to the next node and so on. |
|
|
|
Describe dorsal root ganglion?
|
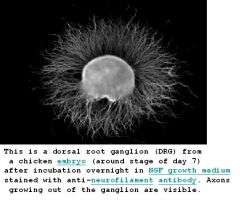
The dorsal root ganglion is a nodule on a dorsal root that contains cell bodies of neurons in afferent spinal nerves. All of the axons in the dorsal root convey somatosensory information, bringing sensory information into the brain and spinal cord. These neurons are of the unipolar type, meaning they have only one projection.
|
|
|
|
What is a peripheral nerve?
|
Peripheral nerves consist of hundreds or thousands of axons whose cell bodies are located either in the dorsal root ganglia (sensory, afferents) or in the central nervous system (motor, afferents).These axons do
not have a uniform population. |
|
|
|
What are 7 characteristic differences in the population of axons in a peripheral nerve?
|
1. axon diameter
2. degree of myelination 3. conduction velocity 4. susceptibility to anesthesia and asphyxia 5. site of termination in the central nervous system 6. function 7. physiological characteristics such as spike duration and absolute refractory period |
AMCAS Form Paper
|
|
|
Axon diameter is:
1. Positively correlated with? 2. Negatively correlated with? |
1. positively
correlated with degree of myelination and conduction velocity 2. negatively correlated with susceptibility to anesthesia |
PMC
|
|
|
What is the difference between a pain neuron and a touch neuron?
|
Pain neurons are unmyelinated and susceptible to anesthesia; touch neurons are not susceptible to anesthesia because they are myelinated;
|
|
|
|
Differentiate btw:
1. Epineurium 2. Perineurium 3. Endoneurium |
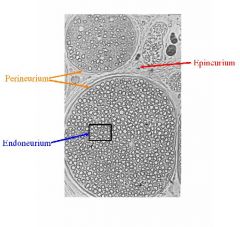
1. Epineurium: the external connective tissue sheath of a nerve trunk
2. Perineurium: the connective tissue sheath that surrounds a bundle of nerve fibers 3. Endoneurium: the connective tissue sheath holding together the individual fibers of a nerve trunk |
|
|
|
WHAT ARE THE 5 SUBPOPULATIONS OF AXONS WITHIN A PERIPHERAL NERVE?
|
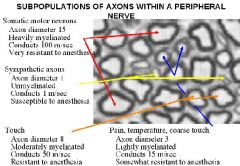
SEE PIC
|
|
|
|
Afferents of spinal and cranial nerves are classified into what 2 categories?
|
1. Fine touch and pressure.
2. Pain, temperature and crude touch. |
Full Pass
|
|
|
How do afferents carrying information from one side of the body and head project, get to terminal locations on the opposite side of the central nervous system?
|
Via a series of relays, their touch, pressure/pain, temperature, crude touch information
|
|
|
|
What happens to relays of the two functional categories of the somatosensory system ?
|
They synapse initially at different sites in the CNS, cross the midline at different locations, ascend in different pathways, and finally end in different CNS structures.
|
|
|
|
List 3 characteristics of the postcentral gyrus?
|
1. The relays of the 2 pathways of the somatosensory pathway synapse at different sites in the CNS before they all arrive at the postcentral gyrus of the opposite hemisphere.
2. The postcentral gyrus is functionally organized by dermatome. 3. The distortion of the homunculus of the postcentral gyrus reflects the number of axons/receptive fields within a dermatome. |
|
|
|
What is a Receptive field?
|
The set of points at which specific stimuli can influence the excitability of an individual neuron. For the somatosensory system it is the area of skin which can affect the single afferent neuron supplying it. "The peripheral receptive fields of sensory units innervating a sensory surface vary greatly in size. The numbers of innervating nerve fibers per unit area of a body part vary also, usually inversely with the sizes of peripheral receptive fields.” (Mountcastle, Medical Physiology, Vol.II.
|
|
|
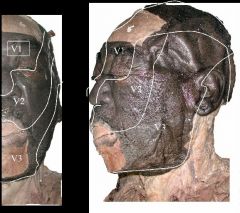
What does this represent?
|
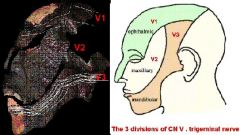
Dermatomes of the face – lateral and frontal views. Note area covered by V1, V2 and V3 in slide 13– each represents a dermatome for the face.
|
|
|
|
Compare the three branches of the trigeminal nerve, V1 to V3,in terms of:
1. Receptor fields. 2. Number of axons |

The receptor fields of the individual axons are smaller going from V1 to V3, with V3 having the smallest receptor fields. Going from V3-V1 you have a decrease in the number of axons, with V1 have the lowest number of axons.
|
|
|
|
What is the Two point discrimination threshold (TPDT)and how does it relate to V1 TO V3?
|

Two point discrimination threshold (TPDT) is the point at which two points (from a caliper) can be distinguished accurately. TPDT is large in V1, quite small within the lips of V3 due to the prescence of so many receptor fields.
NOTE: - point at which two pin-pricks are felt as one is your two-point discrimination threshold - it is largest at V1, smaller and V2 and smallest at V3 because there are so many receptive fields - some areas of skin have many receptors with smaller receptive fields so you can discriminate finer and finer textures and other things there |
|
|
|
What is the significance of having smaller receptive fields?
|

Some areas of skin have many more sensory axons, with more sensory fields so, smaller receptive fields means being able to distinguish textures.
NOTE: - thorax = large dermatomes and smaller fibers-- can't perceive small differences in areas of the back - lips and finger tips have very small two-point discrimination threshold - axons demand a certain amount of cotical space (same for all; differs for areas based on NUMBER of axons present) |
|
|
|
Discuss the lips and the fingertips in terms of two point discrimination thresholds and the significance of this?
|

The lips and the fingertips have very small two point discrimination thresholds, because of the tasks associated with those structures; like discrimination is necessary for speech so the lips have high TPDT. Each axon demands a certain amount of space in the cortex. Collectively a lot of cortex is needed for the V3 region versus for the V1, which has a lot less cortex.
NOTE: - thorax = large dermatomes and smaller fibers-- can't perceive small differences in areas of the back - lips and finger tips have very small two-point discrimination threshold - axons demand a certain amount of cotical space (same for all; differs for areas based on NUMBER of axons present) |
|
|
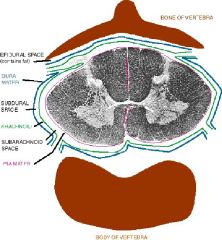
Discuss this picture in terms of:
1. coverings 2. enlargements 3. vasculature |
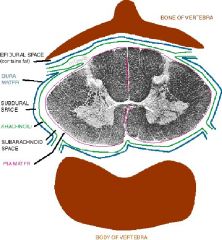
The large ventral and dorsal horns with septum indicates the cervical enlargement. under the arachnoid space lies the vasculature of the brain – primarily located in the subarachnoid space.
NOTES: cervical enlargement-- see septums at top - spinal cord is covered with the three meninges - dura mater = tough mother - under arachnoid is all the vasculature of the brain x: circle of willis and them |
|
|
|
What is:
1. White matter of spinal cord 2. Gray matter of spinal cord |
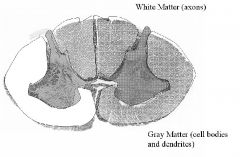
1. White matter is the axonal matter (bundles of myleinated fiber) that surround the central gray matter in the spinal cord and it consists of ascending and descending fiber pathways called tracts.
2. Gray matter consists of cell bodies and dendrites and it is located centrally within the spinal cord and it is butterfly or H shaped in a configuration that varies according to spinal cord level . |
|
|
|
1. What are the 2 major divisions of the GRAY MATTER?
2. What are the 3 major division of WHITE MATTER? |
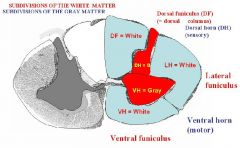
1. The 2 major divisions of the GRAY MATTER are:
-Dorsal horn (sensory) -Ventral horn (motor) 2. The 3 major division of WHITE MATTER are: -Doral funiculus -Lateral funiculus -Ventral funiculus NOTES: -Funiculus means “large bundle of sticks” and it is found within the white matter and contains the axons; -The dorsal horn is sensory only. It contains axons that respond only to pain, touch and temperature only. - The ventral horn is motor only. Respond only to chemical or electrical stimulation, leading to a motor twitch. -Dorsal funiculus contains axons that are sensory and ascend to the brain. -- Dorsal funiculus (dorsal columns) is a bundle of sticks and it has two subdivisions: A. Fasciculus gracilis = all cord levels. B. Fasciculus cuneatus = only at upper thoracic and cervical cord levels - Incoming sensory information is the division between the dorsal and lateral funiculi - other division is not as clear - lateral funiculi is mix of sensory and motor - dorsal funiculus = sensory info only |
|
|
|
Describe:
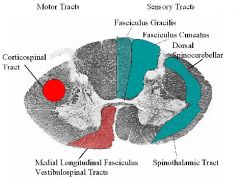
1. The 2 motor tracts in white matter of the spinal cord 2. The 2 sensory tracts in white matter of the spinal cord |
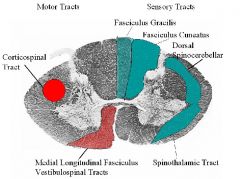
1. The 2 motor tracts in white matter of the spinal cord are:
A.) CORTICOSPINAL TRACT: The corticospinal or pyramidal tract is a massive collection of axons that travel between the cerebral cortex of the brain and the spinal cord. The corticospinal tract contains exclusively motor axons. About 85% of the axons cross over in the medulla oblongata (at a point known as the pyramidal decussation). This explains why movement of one side of the body is controlled by the opposite side of the brain. The cell bodies of the axons of the corticospinal Tract are located in the precentral gyrus. B.) MEDIAL LONGTITUDINAL FASCICULUS VESTIBULOSPINAL TRACT: These are tracts that their cell bodies are located in the vestibular nuclei of the medulla (brainstem) and travel to the spinal cord. 2. The 2 sensory tracts in white matter of the spinal cord are : A.) DORSAL SPINOCEREBELLAR TRACT: Anatomically the cerebellum has great neuronal trees. The dorsal spinocerebellar tract conveys proprioceptive information from the body to the cerebellum. It is part of the somatosensory system and runs in parallel with the ventral spinocerebellar tract. Both these tracts involve two neurons and end up on the same side of the body. B. SPINOTHALAMIC TRACT: It is responsive to touch and it is a very general and not specific transmission of the pain and temperature axons. If selected damage occurs within the STT there will be no deficits because they are not localizing. NOTES: 1B.) The medial longitudinal fasciculus (MLF) is a pair of crossed fiber tracts (group of axons), one on each side of the brainstem, that carry information about the direction that the eyes should move. It connects the cranial nerve nuclei III, IV and VI together, as well as the gaze centres and information about head movement (from cranial nerve VIII). It also descends into the cervical spinal cord, and innervates some muscles of the neck. The MLF arises from the Vestibular Nucleus (VN) and is thought to be involved in the maintenance of gaze. This is achived by inputs to the VN from 1. the Vestibulocochlear (8th cranial) nerve about head movements, 2. gain adjustments from the flocculus of the cerebellum, 3. head and neck propioceptors and foot and ankle muscle spindle, via the fastigial nucleus. Lesions of the MLF produce internuclear ophthalmoplegia. 2B. The spinothalamic tract is the sensory pathway in the body that transmits pain, temperature, itch and crude touch. These types of sensation cross over to the other side of the body at the spinal cord, not in the brainstem like the posterior column-medial lemniscus pathway and corticospinal tract. The name spinothalamic tells us sensation runs up the spinal cord to the thalamus; this is true but misleading, as all sensory pathways synapse at the thalamus with the exception of the olfactory sensory pathway. There are two main parts of the spinothalamic tract (STT): The lateral spinothalamic tract transmits pain and temperature, the anterior (or ventral in animals) spinothalamic tract transmits touch. The types of sensory information trasmitted via the STT are described as affective sensation. This means that the sensation is accompanied by a compulsion to act. For instance an itch is accompanied by a need to scratch, and a painful stimulus makes us want to withdraw from the pain. |
|
|
|
What are the two divisions of the dorsal funiculus?
|
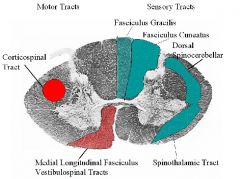
1. Fasciculus gracilis
2. Fasciculus cuneatus. The two pathways are the same sensory modality, fine touch and pressure from different dermatomes. Remember that pain is a localizer of problem location but there are no pain fibers n the dorsal column but they contain many fine touch sensations and knowlesge of spinal cord anatomy helps localize damage to spinal cord - laminations = gray matter! |
|
|
|
Define these terms:
1. Dorsal root ganglion 2. Dorsal root 3. Mixed spinal nerve 4. Ventral root 5. Motor neurons of the ventral horn |
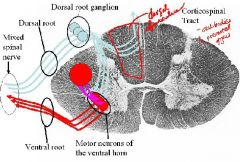
1. Dorsal root ganglion: A ganglion on the dorsal root of each spinal nerve that is one of a series containing cell bodies of sensory neurons
2. Dorsal root: The one of the two roots of a spinal nerve that passes posteriorly to the spinal cord separating the dorsal funiculus and lateral funiculus and consists of sensory fibers. 3. Mixed spinal nerve: a spinal nerve containig both sensory and motor fibers. Also,peripheral nerves connected to the spinal cord in a mixed spinal nerve 4. Ventral root: The ventral root arises from the ventral aspect of the spinal cord segment. All motor fibres (somatic and autonomic) leave the cord via the ventral roots. The ventral roots from T1 - L2 carry sympathetic fibres. 5. Motor neurons of the ventral horn : A neuron that passes from the CNS to a muscle and conducts an impulse that causes movement and motor neurons in different parts of the spinal cord (ventral horn) innervate different parts of the body. EXTRA NOTES: When a spinal nerve enters the vertebral canal, the sensory fibers peel off and go ventrally in the spinal cord and the motor fibers go into the ventral root - separation of dorsal and ventral roots into sensory and motor-- Bell-Mangende law - therefore problem in dorsal root only = sensory problem only on the associated dermatome (looking at one spinal level) |
|
|
|
Differentiate between:
1. Disease of the dorsal root 2. Disease of dorsal root and dorsal root ganglion |
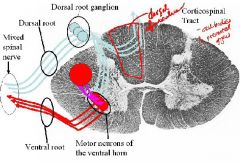
1. Disease of the dorsal root would be limited to sensory deficits and the deficits exist on the associated dermatome.
2. Disease of the dorsal root and dorsal root ganglion is limited to sensory but not motor deficits on the same side of the body. |
|
|
|
Describe Poliomyelitis ?
|
It is a disease of the ventral root ganglion, axons selectively die and the deficits are motor only and preserve the sensory.
NOTES: Poliomyelitis ("polio"), or infantile paralysis, is a viral paralytic disease. The causative agent, a virus called poliovirus (PV), enters the body orally, infecting the intestinal wall. It may proceed to the blood stream and into the central nervous system causing muscle weakness and often paralysis. |
|
|
|
Distinguish between:
1. Corticospinal tract neurons 2. Peripheral motor neurons 3. Central motor neurons |
There are Axon collatorals ascend from the primary axons without synapse to the dorsal columns – the cuneatus and gracilis and here are the diff btw the neurons:
1. Corticospinal tract neurons are CNS upper motor neurons. They have cell bodies that originate in the precentral gyrus and coarse all the way down from the gyrus to terminate on the motor neurons of the ventral horn in the spinal cord. 2. Peripheral motor neurons consist of the upper and lower motor neurons 3. Central motor neurons - remain within a bony cavity Selective destruction of either one of these leads to different deficits. |
|
|
|
Describe the disease of lower motor neurons and its 3 characteristics?
|
The lower motor neurons are the motoneurons which synapse on striated muscle and their disease is poliomyelitis (flaccid paralysis) and it is characterized by:
1. Atonia (limb is limp and dead) 2. Atrophy of associated muscles 3. Areflexia: no reflexes are possible |
Low = TRiP
|
|
|
Describe the disease of upper motor neurons and its 2 characteristics?
|
This is a disease of the corticospinal system and it is characterized by :
1. Hypertonia 2. Hyperreflexia,where reflexes are possible but no behavior out of it in the muscle(controlled behavior) NOTE: Upper motor neurons, or Betz cells, are pyramidal neurons located in the primary motor cortex. The cell bodies of these neurons are some of the largest in the brain, approaching nearly 100μm in diameter. These neurons connect the brain to the spinal cord, from which point nerve signals continue to the muscles by means of the lower motor neurons. Damage to upper motor neurons is indicated by spasticity and exaggerated reflexes. Damage to lower motor neurons is indicated by fasciculations, weakening of muscles, and muscular atrophy. |
UPPER = HIGH
LOWER = WEAK |
|
|
What does this illustrate?
|
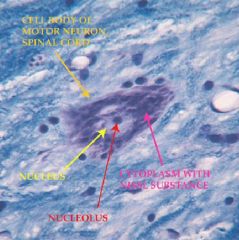
This shows the ventral horn with motor neuron cell bodies and the cell bodies are large in motor neurons because they have to travel long distances.
|
|
|
|
What is a motor end plate?
|
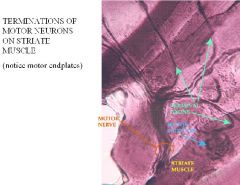
A motor end plate is the axon terminal secreting ACh flowing over 150microns (or nm?) to attach to receptors on striated muscle to allow for contraction-- muscle shortening and this occurs by the axons branching out and terminating on the motor endplate at the axon terminal then the axon secretes the acetylcholine leading to depolarization and contraction of the muscle. The picture above is a silver nitrate stain that shows the motor end plate in the blue arrow.
NOTES: A motor end plate is the distal (farthest from the nerve body) end of the nerve where the nerve impulse causes emission of acetylcholine molecules into the synaptic cleft to innervate muscle fibers triggering muscle contraction. A motor (efferent) nerve axon loses its myelin sheath and branches into multiple endings, which occupy depressions in the sarcolemma. Motor neurons can innervate from one to over 100 muscle fibers. |
|
|
|
What is unique about Striated muscle fibers ?
|
They have sensory components to them
|
|
|
|
Describe monosynaptic reflex?
|
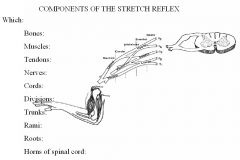
The mixed nerves enter the spinal grey through C6 which activates the ventral horn cell and triggers contraction of the muscle.
NOTES: If the sensory neuron comes in and directly synapses on the motor neuron, that is called a monosynaptic reflex. Monosynaptic means "one synapse." So, in the monosynaptic reflex, there is only one synapse that occurs in the spinal cord: SN -----< MN (the line with the "<" represents an axon with axon terminals). This reflex is quick: it only takes as long to respond as it takes for the sensory neuron to carry the information to the spinal cord, cross the synapse to the motor neuron, run back out the motor neuron axon to the muscle, and cause contraction. Not even one second is necessary. |
|
|
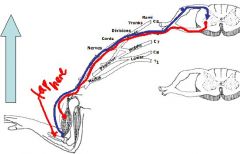
Use this illustration to describe the antagonistic reflex?
|
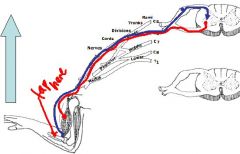
This shows that striated muscle fibers have receptors that are sensitive to stretch
and you have dorsal/ ventral primary rami involved in this. The red line contracts the muscle to draw the limb up but this doesn't happen because in doing so it stretches the opposing muscle (agonist activates the antagonist) and this sets off an antagonistic relfex to contract opposing muscle to pull limb down |
|
|
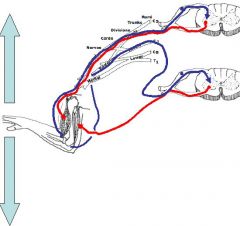
Explain this picture?
|
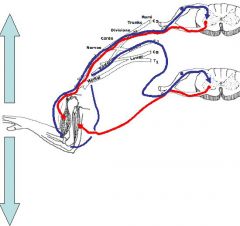
This picture shows that no movement of the arm can occur if the agonist muscle to the movement is stimulated to action as well, therefore, opposing reflexes prevent movement.
|
|
|
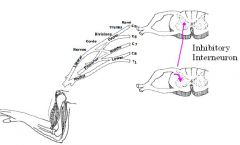
Explain the effect of an inhibitory interneuron with this diagram?
|
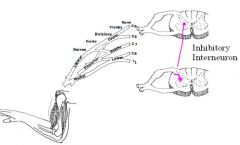
The purple line are cells descending ipsilaterally to terminate on ventral cells of opposing relfex and these are inhibitory interneurons that inhibits cells they synapse on.
|
|
|
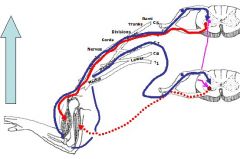
What does this illustrate and why is it significant in a clinical basis??
|
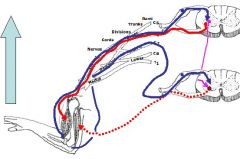
-The agonist muscle (biceps) has been activated, setting off a motor neuron which then starts to operate and stretches the opposing muscle and goes in.
-However, the inhibitory interneuron has inhibited the opposing neuron associated with the opposing muscle (triceps) rendering the input there unresponsive. -There is both a monosynaptic and disynaptic relay allowing this reflex to work. It can occur either way, favoring either muscle. -You need both sensory and motor neurons to trigger a reflex, without one or the other you have areflexia. NOTE: The limb is lifted where you have the monosynaptic and disynaptic relay, allowing the reflex to work by inhibiting the action of the opposing muscle. - In upper motor neuron disease, these reflexes are still there and are hyperreflexive - Also, you need sensory and motor limbs to have a reflex otherwise you have areflexia |
|

