![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
84 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Skeletal system |
Bones, cartilage, ligaments, other CT that attach bones to each other |
|
|
|
Bone |
Each is an organ w/ CT, blood vessels, nerves, lymph vessels, cartilage, CT coverings |
|
|
|
Skeletal system fn |
Support Protection Mineral storage Triglyceride storage Red & white blood cell formation (hemopoiesis) Leverage (assist in mvmt) |
|
|
|
Periosteum |
CT membrane covering external surface of bone Cont w/ tendons, CT of joints Attached to bone matrix via perforating fibers 2 layers: outer fibrous & inner osteogenic |
|
|
|
Endosteum |
Lining inner surface of bone including marrow cavity, trabecullae of spongy bone, canals of compact bone Contains osteogenic cells-important for bone growth & remodeling |
|
|
|
Osteogenic cells |
Stem cells formed from mesenchyme (embryonic CT) |
|
|
|
Osteoblasts |
Cells build bone=bone formation Syn organic components of matrix Initiate calcification-take Ca from blood & deposit w/in matrix by exocytosis Immature cells |
|
|
|
Osteocytes |
Mature cell involved in maintenance of bone tissue Sense bone microdamage & mechanical forces on bone & signals for repair |
|
|
|
Osteoclasts |
Break down bone=bone resorption Release proteolytic enzymes & acids to degrade collagen & release minerals to blood Derived from myloid stem cells |
|
|
|
Bone modeling |
Bone formed by osteoblasts w/out prior bone resorption Happens during growth Produces chg in bone size & shape |
|
|
|
Bone remodeling |
Bone first resorbed by osteoclasts & then formed in same location by osteoblasts Happens throughout life |
|
|
|
Goal of modeling/remodeling |
Achieve strength for loading & lightness for mobility |
|
|
|
Extracellular matrix |
Organic- ground sub & collagen fiber Inorganic- water & hydroxyapatite |
|
|
|
Organic components |
Ground sub- GAG Glycoproteins-polysaccaride + protein Negatively charged Collagen fiber Fibrous protein arranged in helical form Resistant to pulling forces Provides flexibility & framework for deposition of Ca crystals |
|
|
|
Inorganic components |
Water- attracted to ground sub Makes up 25% of extracellular matrix Hydroxyapatite- Ca phosphate & Ca hydroxide + other minerals & ions Forms mineral plates called hydroxyapatite platelets |
|
|
|
Organization of organic/inorganic components |
Salts (hydroxyapatite) deposited w/in collagen fiber As hydroxyapatite condenses, other inorganic salts & ions percipitate in matrix to fill spaces w/in collagen fiber |
|
|
|
Collagen & minerals |
Collagen- flexibility Minerals- firmness |
|
|
|
Rickets |
Inorganic component deficient Ca deficiency due to lack of vitamin D leads to flexible bones |
|
|
|
Scurvy |
Organic component deficient Prob w/ collagen syn due to vitamin C deficiency leads to brittle bones that can fracture easily |
|
|
|
Spongy bone |
Irregular lattice of thin plates (trabecullae) Osteocytes housed in lacunae Epiphysis of long bone, surrounding marrow cavities, flat, short, Irregular bones W/stand force from many directions Lightens skeleton Contains red marrow from hemopoiesis |
|
|
|
Compact bone |
Solid network of bone organized in concentric ring structures (osteon) External layer of all bones, diaphysis of long bones Gives long bones ability w/stand forces along longitudinal axis |
|
|
|
Infant Bone formation |
Fontanels (soft spot) Epiphyseal of long bone made of cartilage Epiphyseal plates stay cartilage until adulthood |
|
|
|
Fetus bones |
Composed of loose CT (mesenchyme) & hyaline cartilage |
|
|
|
Ossification |
Replacement of CT by bone Begins during 2nd month of develop Intramembranous & endochondral |
|
|
|
Intramembranous |
W/in membrane Mesenchyme--->bone Cranial bones, mandible, sternum, clavicle Develop ossification center Calcification Form trabecullae (spongy bone) Develop periosteum |
|
|

Endochondral ossification |

Inside cartilage Mesenchyme-->cartilage-->bone Most bones in body Growth in length at epiphyseal plate |
|
|
|
Calcification |
Deposition of Ca |
|
|
|
Growth of cartilage |
Interstitial growth Appositional growth |
|
|
|
Interstitial growth |

W/in cartilage Length at epiphyseal plate |
|
|
|
Appositional growth |
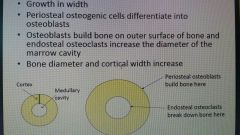
Outer surface Width |
|
|
|
Fractures |
Break in continuity of bone rendering structurally incompetent |
|
|
|
Traumatic fracture |
Normal bone experiencing abnormal forces |
|
|
|
Pathologic fracture |
Abnormal bone experiencing normal forces |
|
|
|
Gross incomplete fracture |
Bone partially broken in continuity Greenstick-incomplete results in bent bone in child/youths |
|
|
|
Gross complete fracture |
Loss in continuity |
|
|
|
Gross non-displaced fracture |
Complete fracture result in speration of broken bone pieces from ea other |
|
|
|
Gross displaced fracture |
Complete fracture result in seperation of 1 broken piece from other |
|
|
|
Gross simple (closed) fracture |
Complete, displaced neither broken piece of bone breaks skin |
|
|
|
Gross open (compound) fracture |
Complete, displaced 1 or more broken pieces of bone break skin |
|
|
|
Repair for bone fractures |
Formation of fracture hematoma Fibrocartilage callus formation Bony callus formation Bone remodeling |
|
|
|
Treatmemt for bone fractures |
Immobilization Reduction Closed-setting&splinting bone for natural healing Open-surgical use of rods, plates, pins,etc position bone & bone fragments correctly for proper healing |
|
|
|
Factors that influence bone |
Dietary:minerals & vitamins Hormones Exercise |
|
|
|
Dietary |
Minerals: Ca & P (also Mg, F, Mn) Vitamins: A-stim osteoblast activ C- needed for collage syn D- stim Ca absorption K,B12- need for syn bone proteins |
|
|
|
Ca homeostasis |
Goal: reg blood Ca w/in norm range (8.5-11.0 mg/dl) Why- Ca important physiological role: membrane excitability(blood clotting) & intercellular activ(2nd messenger) How- control Ca entry into & exit from blood: bone storage, intestinal absorption, kidney excretion |
|
|
|
Hormones involved in Ca homeostasis |
Calcitonin Parathyroid hormone Calcitriol (vitamin D) |
|
|
|
Calcitonin |
Stim: high blood Ca Source: thyroid gland (parafollicular cell) Target tissue: bone, kidney, intestine Actions (goal to decrease bone resorption): inhibit osteoclast activity, increase excretion of Ca at kidney, inhibit absorption of Ca at intestine End result: decrease blood Ca |
|
|
|
Parathyroid hormone |
Stim: low blood Ca Source: parathyroid gland Target tissue: bone, kidney, intestine Actions (goal to increase Ca): stim osteoclast activity, decrease excretion of Ca at kidney, stim intestinal absorption of Ca & promote calcitriol (vit D) action End result: increase blood Ca |
|
|
|
Vitamin D |
Calcitriol: active form of vit D 1,25 dihydroxycholecalciferol or 1,25 dihydroxy vitamin D3 Vit D steroid hormone- derived from cholesterol (lipophilic/hydrophobic) |
|
|
|
Actions of calcitriol (active form of vit D) |
Stim osteoclast activ (increase bone resorption) Decrease Ca excretion at kidney Increase Ca absorption at intestine (works well with PTH stim absorption) End result: increase blood Ca |
|
|
|
How much Ca should you have per day? |
Young adults(19-50) need 1000mg Ca from diet&sup to avoid bone loss |
|
|
|
Hormones that influence bone |
Calcitonin & PTH = osteoclasts Growth hormone(somatotropin) & estrogen/testosterone = osteoblasts |
|
|
|
Growth hormone (somatotropin) |
Stim cell growth & protein syn (collagen) Stim form of insulin like growth factors (IGFs) --> stim osteoblast activ --> stim bone form |
|
|
|
Skeletal disorders associated w/ GH |
Pituitary dwarfism Pituitary giantism Acromegaly |
|
|
|
Pituitary dwarfism |
Children w/ low levels of growth hormone--> slow epiphyseal growth (short stature) |
|
|
|
Pituitary giantism |
Hypersection of growth hormone in childhood--> accelerated epiphyseal growth (tall stature) |
|
|
|
Acromegaly |
Hypersecretion of growth hormone after puberty--> appositional growth (thickening of bones) in skull, hands, feet--> epiphyseal plates of long bones already closed |
|
|
|
Estrogen/testosterone |
Both stim osteoblast activity--> stim bone form Levels increase at puberty: bone growth/height spurts, eventually cause closure of epiphyseal plates because osteoblast/osteoclast activity slightly greater than chondrocyte activ Levels decrease w/ older age |
|
|
|
Effect of exercise on bone |
Bone will chg in response to stresses 1. Muscle pulling on bone --> joint rxn forces 2. Impact --> ground rxn forces |
|
|
|
Spongy vs compact |
Spongy- more metabolically active- can respond to chgs in mechanical loading more readily Most likely sites of fracture areas w/ high spongy bone content (hip, wrist, spine) |
|
|
|
Role of exercise |
Goal: reach fracture threshold later in life Early- increase peak bone mass Later- prevent bone loss Other benefits- fall prevention - improved strength, balance, coordination |
|
|
|
Bone estrogen strength training (BEST) study |
Postmenopausal women (N=266) Split into exercise & control groups Exercisers trained 3x per week, 2 sets of 8-10 reps for ea exercise at 70-80% rep max All subjects took Ca supplements |
|
|
|
BEST study strength training exercises |
Wall squat/ smith squat One arm military press Leg press Lat pull down Seated row Back extension |
|
|
|
Effects of exercise on bone |
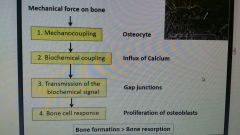
|
|
|
|
Osteoporosis |
Porous bone--> increased fracture risk Proportion of collagen & minerals norm but decrease in mass |
|
|
|
What causes reduced bone mass? |
Any factor stimulates bone resorption or inhibits formation Ostoclast activ>osteoblast activ (Bone resorp) (bone form) |
|
|
|
Osteoporosis risk factors |

|
|
|
|
Articulation |
Point of contact between: 1. Bones (elbow) 2. Bones & cartilage (epiphyseal plates) 3. Bones and teeth |
|
|
|
Structural classification of joints based on anatomical structure |
Fibrous, cartilaginous, synovial |
|
|
|
Functional classification of joints based on amount of mvmt at joint |
Immovable-->synarthrosis Slightly movable--> amphiarthrosis Freely movable-->diarthrosis |
|
|
|
Types of synarthroses |
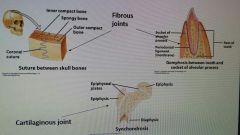
|
|
|
|
Types of amphiarthrosis |
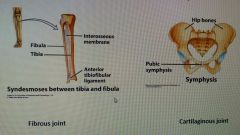
|
|
|
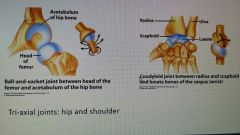
Types of diarthrosis |
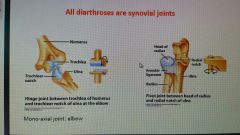
|
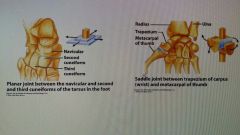
|
|
|
Structure of diarthrosis (synovial joint) |
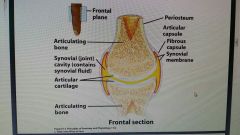
|
|
|
|
Functions of synovial fluid |
1. Lubricates joint 2. Provides nutrients to articular cartilage (avascular) 3. Shock absorption |
|
|
|
Accessory structures of synovial joint |
Ligaments:intracapsular & extracapsular Tendons Bursae Meniscus Labrum |
|
|
|
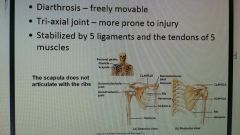
Shoulder joint |
|
|
|
|
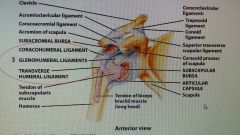
Shoulder joint ligaments |
|
|
|
|
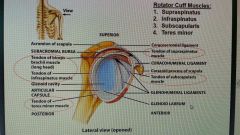
Shoulder joint tendons |
|
|
|
|
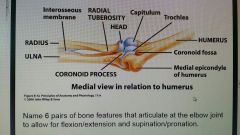
Elbow joint |
|
|
|
|
Knee joint |
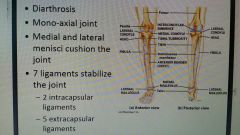
|
|
|
|
Knee joint extracapsular ligaments |
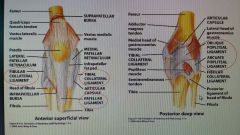
|
|
|
|
Knee joint intracapsular ligament |
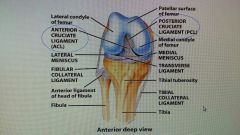
|
|
|
|
Temporomandibular joint |
Only moveable joint of skull Mandibular condyle of mandible & mandibular fossa of temporal bone TMJ syndrome- pain associated w/ muscle spasm (muscles pull joint out of alignment) |
|
|
|
Articulations of thoracic vertebrae |
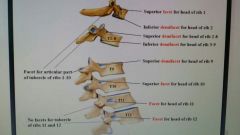
|
|

