![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
61 Cards in this Set
- Front
- Back

Benign and Malignant Disorders of the Breast and Pelvis |

Benign and Malignant Disorders of the Breast and Pelvis |
|
|
271. A 50-year-old woman is diagnosed with cervical cancer. |
271. The answer is d.
The main routes of spread of cervical cancer include vaginal mucosa, myometrium, paracervical lymphatics, and direct extension into the parametrium. The prevalence of lymph node disease correlates with the stage of malignancy. Primary node groups involved in the spread of cervical cancer include the paracervical, parametrial, obturator, hypogastric, external iliac, and sacral nodes, essentially in that order. Less commonly, there is involvement in the common iliac, inguinal, and para-aortic nodes. In stage I, the pelvic nodes are positive in approximately 15% of cases and the para-aortic nodes in 6%. In stage II, pelvic nodes are positive in 28% of cases and para-aortic nodes in 16%. In stage III, pelvic nodes are positive in 47% of cases and para-aortic nodes in 28%. |
|
|
272. A 21-year-old woman presents with left lower quadrant pain. An anterior 7-cm firm adnexal cyst is palpated. Ultrasound confirms a complex left adnexal mass with solid components that appear to contain bone and teeth. |
272. The answer is c.
Benign cystic teratomas (dermoids) are the most common germ cell tumors and account for about 20% to 25% of all ovarian neoplasms. They occur primarily during the reproductive years, but may also occur in postmenopausal women and in children. Dermoids are usually unilateral, but 10% to 15% are bilateral. Usually the tumors are asymptomatic, but they can cause severe pain if there is torsion or if the sebaceous material perforates, spills, and creates a reactive peritonitis. |
|
|
273. A 54-year-old woman undergoes a laparotomy because of a pelvic mass. At exploratory laparotomy, a unilateral ovarian neoplasm is discovered that is accompanied by a large omental metastasis. Frozen section diagnosis confirms metastatic serous cystadenocarcinoma.
Which of the following is the most appropriate intraoperative course of action? a. Excision of the omental metastasis and ovarian cystectomy b. Omentectomy and ovarian cystectomy c. Excision of the omental metastasis and unilateral oophorectomy d. Omentectomy and bilateral salpingo-oophorectomy e. Omentectomy, total abdominal hysterectomy, and bilateral salpingo-oophorectomy |
273. The answer is e.
The survival of women who have ovarian carcinoma varies inversely with the amount of residual tumor left after the initial surgery. At the time of laparotomy, a maximum effort should be made to determine the sites of tumor spread and to excise all resectable tumor. Although the uterus and ovaries may appear grossly normal, there is a relatively high incidence of occult metastases to these organs; for this reason, they should be removed during the initial surgery. Ovarian cancer metastasizes outside the peritoneum via the pelvic or paraaortic lymphatics, and from there into the thorax and the remainder of the body. |
|
|
274. A 58-year-old woman is seen for evaluation of a swelling in her right vulva. She has also noted pain in this area when walking and during coitus. At the time of pelvic examination, a mildly tender, fluctuant mass is noted just outside the introitus in the right vulva in the region of the Bartholin gland.
Which of the following is the most appropriate treatment? a. Marsupialization b. Administration of antibiotics c. Surgical excision d. Incision and drainage e. Observation |
274. The answer is c.
Although rare, adenocarcinoma of the Bartholin gland must be excluded in women more than 40 years of age who present with a cystic or solid mass in this area. The appropriate treatment in these cases is surgical excision of the Bartholin gland to allow for a careful pathologic examination. In cases of abscess formation, both marsupialization of the sac and incision with drainage as well as appropriate antibiotics are accepted modes of therapy. In the case of the asymptomatic Bartholin cyst, no treatment is necessary. |
|
|
275. A 51-year-old woman is diagnosed with invasive cervical carcinoma by cone biopsy. Pelvic examination and rectal-vaginal examination reveal the parametrium to be free of disease, but the upper portion of the vagina is involved with tumor. Intravenous pyelography (IVP) and sigmoidoscopy are negative, but a computed tomography (CT) scan of the abdomen and pelvis shows grossly enlarged pelvic and periaortic nodes. This patient is classified at which of the following stages?
a. IIa b. IIb c. IIIa d. IIIb e. IV |
275. The answer is a.
Cervical cancer is still staged clinically. Physical examination, routine x-rays, barium enema, colposcopy, cystoscopy, proctosigmoidoscopy, and IVP are used to stage the disease. CT scan results, while clinically useful, are not used to stage the disease. Stage I disease is limited to the cervix. Stage Ia disease is preclinical (ie, microscopic), while stage Ib denotes macroscopic disease. Stage II involves the vagina, but not the lower one-third, or infiltrates the parametrium, but not out to the pelvic side wall. Stage IIa denotes vaginal but not parametrial extension, while stage IIb denotes parametrial extension. Stage III involves the lower one-third of the vagina or extends to the pelvic side wall; there is no cancerfree area between the tumor and the pelvic wall. Stage IIIa lesions have not extended to the pelvic wall, but involve the lower one-third of the vagina. Stage IIIb tumors have extension to the pelvic wall and/or are associated with hydronephrosis or a nonfunctioning kidney caused by tumor. Stage IV is outside the reproductive tract. |
|
|
276. A 35-year-old G3P3 with a Pap smear showing high-grade squamous intraepithelial lesion of the cervix (CIN III) has an inadequate colposcopy. Cone biopsy of the cervix shows squamous cell cancer that has invaded only 1 mm beyond the basement membrane. There are no confluent tongues of tumor, and there is no evidence of lymphatic or vascular invasion. The margins of the cone biopsy specimen are free of disease.
How should you classify or stage this patient’s disease? a. Carcinoma of low malignant potential b. Microinvasive cancer, stage Ia1 c. Atypical squamous cells of undetermined significance d. Carcinoma in situ e. Invasive cancer, stage IIa |
276. The answer is b.
Microinvasive carcinoma of the cervix includes lesions within 3 mm of the base of the epithelium, with no confluent tongues or lymphatic or vascular invasion. The overall incidence of metastases in 751 reported cases is 1.2%. Simple hysterectomy is accepted therapy. |
|
|
277. A 35-year-old G3P3 with a Pap smear showing high-grade squamous intraepithelial lesion of the cervix (CIN III) has an inadequate colposcopy. Cone biopsy of the cervix shows squamous cell cancer that has invaded only 1 mm beyond the basement membrane. There are no confluent tongues of tumor, and there is no evidence of lymphatic or vascular invasion. The margins of the cone biopsy specimen are free of disease.
The patient above now asks you for your advice on how to treat her cervical disease. Your best recommendation is for the patient to undergo which of the following? a. Treatment with external beam radiation b. Implantation of radioactive cesium into the cervical canal c. Simple hysterectomy d. Simple hysterectomy with pelvic lymphadenectomy e. Radical hysterectomy |
277. The answer is c.
Microinvasive carcinoma of the cervix includes lesions within 3 mm of the base of the epithelium, with no confluent tongues or lymphatic or vascular invasion. The overall incidence of metastases in 751 reported cases is 1.2%. Simple hysterectomy is accepted therapy. |
|
|
278. A woman is found to have a unilateral invasive vulvar carcinoma that is 2 cm in diameter but not associated with evidence of lymph node spread. Initial management should consist of which of the following?
a. Chemotherapy b. Radiation therapy c. Simple vulvectomy d. Radical vulvectomy e. Radical vulvectomy and bilateral inguinal lymphadenectomy |
278. The answer is e.
Women who have invasive vulvar carcinoma usually are treated surgically. If the lesion is unilateral, is not associated with fixed or ulcerated inguinal lymph nodes, and does not involve the urethra, vagina, anus, or rectum, then treatment usually consists of radical vulvectomy and bilateral inguinal lymphadenectomy. If inguinal lymph nodes show evidence of metastatic disease, bilateral pelvic lymphadenectomy is usually performed. Radiation therapy, though not a routine part of the management of women who have early vulvar carcinoma, is employed (as an alternative to pelvic exenteration with radical vulvectomy) in the treatment of women who have local, advanced carcinoma. |
|
|
279. A patient is receiving external beam radiation for treatment of metastatic endometrial cancer. The treatment field includes the entire pelvis.
Which of the following tissues within this radiation field is the most radiosensitive? a. Vagina b. Ovary c. Rectovaginal septum d. Bladder e. Rectum |
279. The answer is b.
Different tissues tolerate different doses of radiation, but the ovaries are by far the most radiosensitive. They tolerate up to 2500 rads, while the other tissues listed tolerate between 5000 and 20,000 rads. Acute evidence of excessive radiation exposure includes tissue necrosis and inflammation, resulting in enteritis, cystitis, vulvitis, proctosigmoiditis, and possible bone marrow suppression. Chronic effects of excessive radiation exposure are manifest months to years after therapy and include vasculitis, fibrosis, and deficient cellular regrowth; these can result in proctitis, cystitis, fistulas, scarring, and stenosis. Successful radiation depends on (1) the greater sensitivity of the cancer cell compared with normal tissue and (2) the greater ability of normal tissue to repair itself after irradiation. The maximal resistance to ionizing radiation depends on an intact circulation and adequate cellular oxygenation. Resistance also depends on total dose, number of portions, and time intervals. The relative resistance of normal tissue (cervix and vagina) in cervical cancer allows high surface doses approaching 15,000 to 20,000 rads to be delivered to the tumor with intracavitary devices, and, because of the inverse square law, significantly lower doses of radiation reach the bladder and rectum. The greater the fractionalization (number of portions the total dose is broken into), the better the normal tissue tolerance of that radiation dose; hence 5000 rads of pelvic radiation is usually given in daily fractions over 5 weeks, with approximately 200 rads being administered each day. |
|
|
280. An intravenous pyelogram (IVP) shows hydronephrosis in the workup of a patient with cervical cancer otherwise confined to a cervix of normal size. This indicates which one of the following stages?
a. Microinvasive stage b. I c. II d. III |
280. The answer is d.
By definition, an IVP showing hydronephrosis would mean the cancer has extended to the pelvic side wall and thus a stage III carcinoma, specifically stage IIIb. Such staging applies even if there is no palpable tumor beyond the cervix. IVP, cystoscopy, and proctosigmoidoscopy are diagnostic tests used to stage cervical cancer along with pelvic examination. However, it is important to understand that while the results of only certain tests are used to stage cervical cancer, this does not limit the physician from performing other diagnostic tests (such as CT scans of the abdomen, pelvis, or chest) that in his or her judgment are required for appropriate medical care and decision making. |
|
|
281. A pregnant 35-year-old patient is at highest risk for the concurrent development of which of the following malignancies?
a. Cervix b. Ovary c. Breast d. Vagina e. Colon |
281. The answer is a.
Cervical cancer is a more common gynecologic malignancy in pregnancy than ovarian or breast cancer attributed to the fact that it is a disease of younger women. Management of cervical intraepithelial lesions is complicated in pregnancy because of increased vascularity of the cervix and because of the concern that manipulation of and trauma to the cervix can compromise continuation of the pregnancy. A traditional cone biopsy is indicated only in the presence of apparent microinvasive disease on a colposcopically directed cervical biopsy. Otherwise, more limited procedures such as shallow cervical biopsies are more appropriate. If invasive cancer is diagnosed, the decision to treat immediately or wait until fetal viability depends in part on the gestational age at which the diagnosis is made, and the severity of the disorder. Survival is decreased for malignancies discovered later in pregnancy. Radiation therapy almost always results in spontaneous abortion, in part because the fetus is particularly radiosensitive. Chemotherapy is associated with higher than expected rates of fetal malformations consistent with the antimetabolite effects of agents used. Specific malformations depend on the agent used and the time in pregnancy at which the exposure occurs. |
|
|
282. Stage Ib cervical cancer is diagnosed in a young woman who wishes to retain her ability to have sexual intercourse. Your consultant has therefore recommended a radical hysterectomy. Assuming that the cancer is confined to the cervix and that intraoperative biopsies are negative, which of the following structures would not be removed during the radical hysterectomy?
a. Uterosacral and uterovesical ligaments b. Pelvic nodes c. The entire parametrium on both sides of the cervix d. Both ovaries e. The upper third of the vagina |
282. The answer is d.
Radical hysterectomy was popularized by Meigs in the 1940s and has become a very safe procedure in skilled hands. It is most often used as primary treatment for early cervical cancer (stages Ib and IIa), and occasionally as primary treatment for uterine cancer. In either case, there must be no evidence of spread beyond the operative field, as suggested by negative intraoperative frozen section biopsies. The procedure involves excision of the uterus, the upper third of the vagina, the uterosacral and uterovesical ligaments, and all of the parametrium, and pelvic node dissection including the ureteral, obturator, hypogastric, and iliac nodes. Radical hysterectomy thus attempts to preserve the bladder, rectum, and ureters while excising as much as possible of the remaining tissue around the cervix that might be involved in microscopic spread of the disease. Ovarian metastases from cervical cancer are extremely rare. Preservation of the ovaries is generally acceptable, particularly in younger women, unless there is some other reason to consider oophorectomy. |
|
|
283. A 24-year-old woman presents with new-onset right lower quadrant pain, and you palpate an enlarged, tender right adnexa.
Which of the following sonographic characteristics of the cyst in this patient suggests the need for surgical exploration now instead of observation for one menstrual cycle? a. Lack of ascites b. Unilocularity c. Papillary vegetation d. Diameter of 5 cm e. Demonstration of arterial and venous flow by Doppler imaging |
283. The answer is c.
Approximately 20% of ovarian neoplasms are considered malignant on pathologic examination. However, all must be considered as placing the patient at risk. Given that most ovarian tumors are not found until significant spread has occurred, it is not unreasonable to attempt to operate on such patients as soon as there is a suspicion of tumor. Papillary vegetation, size greater than 10 cm, ascites, possible torsion, or solid lesions are automatic indications for exploratory laparotomy. In a younger woman, a cyst can be followed past one menstrual cycle to determine if it is a follicular cyst, since a follicular cyst should regress after onset of the next menstrual period. If regression does not occur, then surgery is appropriate. Doppler ultrasound imaging allows visualization of arterial and venous flow patterns superimposed on the image of the structure being examined; arterial and venous flow are expected in a normal ovary. |
|
|
284. A 70-year-old woman presents for evaluation of a pruritic lesion on the vulva. Examination shows a white, friable lesion on the right labia majora that is 3 cm in diameter. No other suspicious areas are noted. Biopsy of the lesion confirms squamous cell carcinoma. In this patient, lymphatic drainage characteristically would be first to which of the following nodes?
a. External iliac lymph nodes b. Superficial inguinal lymph nodes c. Deep femoral lymph nodes d. Periaortic nodes e. Internal iliac nodes |
284. The answer is b.
An important feature of the lymphatic drainage of the vulva is the existence of drainage across the midline. The vulva drains first into the superficial inguinal lymph nodes, then into the deep femoral nodes, and finally into the external iliac lymph nodes. The clinical significance of this sequence for patients with carcinoma of the vulva is that the iliac nodes are probably free of the disease if the deep femoral nodes are not involved. Unlike the lymphatic drainage from the rest of the vulva, the drainage from the clitoral region bypasses the superficial inguinal nodes and passes directly to the deep femoral nodes. Thus, while the superficial nodes usually also have metastases when the deep femoral nodes are implicated, it is possible for only the deep nodes to be involved if the carcinoma is in the midline near the clitoris. |
|
|
285. A 17-year-old girl is seen by her primary care physician for the evaluation of left lower quadrant pain. The physician felt a pelvic mass on physical examination and ordered a pelvic ultrasound. You are consulted because an ovarian neoplasm is identified by the ultrasound.
Which of the following is the most common ovarian tumor in this type of patient? a. Germ cell b. Papillary serous epithelial c. Fibrosarcoma d. Brenner tumor e. Sarcoma botryoides |
285. The answer is a.
The most common ovarian neoplasms in young women in there teens and early twenties are of germ cell origin, and about half of these tumors are malignant. Functioning ovarian tumors have been reported to produce precocious puberty in about 2% of affected patients. Epithelial tumors of the ovary, which are quite rare in prepubertal girls, are benign in approximately 90% of all cases. Papillary serous cystadenocarcinoma is an example of such a malignant epithelial tumor. Stromal tumors (such as fibrosarcoma) and Brenner tumors are not seen in this age group. Sarcoma botryoides, a tumor seen in children, is a malignancy associated with Müllerian structures such as the vagina and uterus, including the uterine cervix. |
|
|
286. A 41-year-old woman undergoes exploratory laparotomy for a persistent adnexal mass. Frozen section diagnosis is serous carcinoma.
Assuming that the other ovary is grossly normal, what is the likelihood that the contralateral ovary is involved in this malignancy? a. 5% b. 15% c. 33% d. 50% e. 75% |
286. The answer is c.
Serous carcinoma is the most common epithelial tumor of the ovary. On histologic examination, psammoma bodies can be seen in approximately 30% of these tumors. Bilateral involvement characterizes about one-third of all serous carcinomas. Although mesonephroid carcinomas tend to be associated with pelvic endometriosis, a similar association has not been demonstrated for serous carcinomas. |
|
|
287. A postmenopausal woman presents with pruritic white lesions on the vulva. Punch biopsy of a representative area is obtained.
Which of the following histologic findings is consistent with the diagnosis of lichen sclerosus? a. Blunting or loss of rete pegs b. Presence of thickened keratin layer c. Acute inflammatory infiltration d. Increase in the number of cellular layers in the epidermis e. Presence of mitotic figures |
287. The answer is a.
Lichen sclerosus was formerly termed but recent studies have concluded that atrophy does not exist. Patients with lichen sclerosus of the vulva tend to be older; they typically present with pruritus, and the lesions are usually white with crinkled skin and well-defined borders. The histologic appearance of lichen sclerosus includes loss of the rete pegs within the dermis, chronic inflammatory infiltrate below the dermis, the development of a homogenous subepithelial layer in the dermis, a decrease in the number of cellular layers, and a decrease in the number of melanocytes. Mechanical trauma produces bullous areas of lymphedema and lacunae, which are then filled with erythrocytes. Ulcerations and ecchymoses may be seen in these traumatized areas as well. Mitotic figures are rare in lichen sclerosus, and hyperkeratosis is not a feature. While a significant cause of symptoms, lichen sclerosus is not a premalignant lesion. Its importance lies in the fact that it must be distinguished from vulvar squamous cancer. |
|
|
288. A 21-year-old woman returns to your office for evaluation of an abnormal Pap smear. The Pap smear showed a squamous abnormality suggestive of a high-grade squamous intraepithelial lesion (HGSIL). Colposcopy confirms the presence of a cervical lesion consistent with severe cervical dysplasia (CIN III).
Which of the following human papilloma virus (HPV) types is most often associated with this type of lesion? a. HPV type 6 b. HPV type 11 c. HPV type 16 d. HPV type 42 e. HPV type 44 |
288. The answer is c.
The human papillomaviruses (HPV) are a group of double-stranded DNA viruses that infect epithelial cells. They do not cause systemic infection. There are numerous viruses within the group, and they are named by number according to the order of their discovery. Human papilloma viruses are sexually transmitted. HPV, in particular types 16, 18, and 31, have been linked to cervical neoplasia. HPV types 6 and 11 are associated with benign condyloma. |
|
|
289. A 20-year-old woman presents complaining of bumps around her vaginal opening. The bumps have been there for several months and are getting bigger. Her boyfriend has the same type of bumps on his penis. On physical examination the patient has multiple 2- to 10-mm lesions around her introitus consistent with condyloma. Her cervix has no gross lesions. A Pap smear is done. One week later, the Pap smear returns showing atypical squamous cells of undetermined significance (ASCUS). Reflex HPV typing showed no high-risk HPV. |
289. The answer is a.
The human papillomaviruses (HPV) are a group of double-stranded DNA viruses that infect epithelial cells. They do not cause systemic infection. There are numerous viruses within the group, and they are named by number according to the order of their discovery. Human papilloma viruses are sexually transmitted. HPV, in particular types 16, 18, and 31, have been linked to cervical neoplasia. HPV types 6 and 11 are associated with benign condyloma. |
|
|
290. Select the ovarian tumor from below that is most likely to be associated with the clinical picture:
A 26-year-old G2P1 presents to the gynecologist complaining of increasing hair growth on her face, chest, and abdomen, but the hair on her head is receding in the temporal regions. She also has had problems with acne. On physical examination the patient has significant amounts of coarse, dark hair on her face, chest, and abdomen. On pelvic examination she has an enlarged clitoris. She has a 7-cm left adnexal mass. a. Granulosa tumor b. Sertoli-Leydig cell tumor c. Immature teratoma d. Gonadoblastoma e. Krukenberg tumor |
290. The answer is b.
Sertoli-Leydig cell tumors, which represent less than 1% of ovarian tumors, may produce symptoms of virilization. Histologically, they resemble fetal testes; clinically, they must be distinguished from other functioning ovarian neoplasms as well as from tumors of the adrenal glands, since both adrenal tumors and Sertoli-Leydig tumors produce androgens. The androgen production can result in seborrhea, acne, menstrual irregularity, hirsutism, breast atrophy, alopecia, deepening of the voice, and clitoromegaly. |
|
|
291. Select the ovarian tumor from below that is most likely to be associated with the clinical picture:
A 56-year-old postmenopausal female presents complaining of vaginal bleeding. Her uterus is slightly enlarged and she has a 6-cm right adnexal mass. Endometrial biopsy shows adenocarcinoma of the endometrium. a. Granulosa tumor b. Sertoli-Leydig cell tumor c. Immature teratoma d. Gonadoblastoma e. Krukenberg tumor |
291. The answer is a.
Granulosa and theca cell tumors are often associated with excessive estrogen production, which may cause pseudoprecocious puberty, postmenopausal bleeding, or menorrhagia. These tumors are associated with endometrial carcinoma in 15% of patients. Because these tumors are quite friable, affected women frequently present with symptoms caused by tumor rupture and intraperitoneal bleeding. |
|
|
292. Select the ovarian tumor from below that is most likely to be associated with the clinical picture:
A 67-year-old woman is found to have bilateral adnexal masses while undergoing evaluation of her recently diagnosed colon cancer. a. Granulosa tumor b. Sertoli-Leydig cell tumor c. Immature teratoma d. Gonadoblastoma e. Krukenberg tumor |
292. The answer is e. |
|
|
293. Select the ovarian tumor from below that is most likely to be associated with the clinical picture:
A 17-year-old woman is referred by her primary care physician for the evaluation of primary amenorrhea. On physical examination, the patient has evidence of virilization. She also has a pelvic mass. During the workup of the patient, she is found to have sex chromosome mosaicism (45,X/46,XY). a. Granulosa tumor b. Sertoli-Leydig cell tumor c. Immature teratoma d. Gonadoblastoma e. Krukenberg tumor |
293. The answer is d. |
|
|
294. Select the ovarian tumor from below that is most likely to be associated with the clinical picture: |
294. The answer is c.
The malignant potential of immature teratomas correlates with the degree of immature or embryonic tissue present. The presence of choriocarcinoma can be determined histologically as well as by human chorionic gonadotropin (hCG) assays. The presence of choriocarcinoma in an immature teratoma worsens the prognosis. |
|
|
295. A 51-year-old menopausal woman is undergoing exploratory laparotomy for bilateral adnexal masses. A frozen section is performed on the excised ovaries and shows significant numbers of signet cells.
a. Granulosa tumor b. Sertoli-Leydig cell tumor c. Immature teratoma d. Gonadoblastoma e. Krukenberg tumor |
295. The answer is e.
Sertoli-Leydig cell tumors, which represent less than 1% of ovarian tumors, may produce symptoms of virilization. Histologically, they resemble fetal testes; clinically, they must be distinguished from other functioning ovarian neoplasms as well as from tumors of the adrenal glands, since both adrenal tumors and Sertoli-Leydig tumors produce androgens. The androgen production can result in seborrhea, acne, menstrual irregularity, hirsutism, breast atrophy, alopecia, deepening of the voice, and clitoromegaly. Granulosa and theca cell tumors are often associated with excessive estrogen production, which may cause pseudoprecocious puberty, postmenopausal bleeding, or menorrhagia. These tumors are associated with endometrial carcinoma in 15% of patients. Because these tumors are quite friable, affected women frequently present with symptoms caused by tumor rupture and intraperitoneal bleeding. Gonadoblastomas frequently contain calcifications that can be detected by plain radiography of the pelvis. Women who have gonadoblastomas often have ambiguous genitalia. The tumors are usually small, and are bilateral in one-third of affected women. The malignant potential of immature teratomas correlates with the degree of immature or embryonic tissue present. The presence of choriocarcinoma can be determined histologically as well as by human chorionic gonadotropin (hCG) assays. The presence of choriocarcinoma in an immature teratoma worsens the prognosis. Krukenberg tumors are typically bilateral, solid masses of the ovary that nearly always represent metastases from another organ, usually the stomach or large intestine. They contain large numbers of signet ring adenocarcinoma cells within a cellular hyperplastic but nonneoplastic ovarian stroma. |
|
|
296. Match the chemotherapeutic agent with the most common side effects.
Cyclophosphamide a. Hemorrhagic cystitis b. Renal failure c. Tympanic membrane fibrosis d. Necrotizing enterocolitis e. Pulmonary fibrosis f. Pancreatic failure g. Ocular degeneration h. Cardiac toxicity i. Peripheral neuropathy j. Bone marrow depression |
296. The answer is a.
Cyclophosphamide is an alkylating agent that cross-links DNA and also inhibits DNA synthesis. Hemorrhagic cystitis and alopecia are common side effects. |
|
|
297. Match the chemotherapeutic agent with the most common side effects.
Cisplatin a. Hemorrhagic cystitis b. Renal failure c. Tympanic membrane fibrosis d. Necrotizing enterocolitis e. Pulmonary fibrosis f. Pancreatic failure g. Ocular degeneration h. Cardiac toxicity i. Peripheral neuropathy j. Bone marrow depression |
297. The answer is b.
Cisplatin causes renal damage and neural toxicity. Patients must be well hydrated. Its mode of action does not fit a specific category. |
|
|
298. Match the chemotherapeutic agent with the most common side effects. |
298. The answer is j.
Taxol can produce allergic reactions and bone marrow depression. |
|
|
299. Match the chemotherapeutic agent with the most common side effects. |
299. The answer is e.
Bleomycin is an antibiotic whose side effect is pulmonary fibrosis |
|
|
300. Match the chemotherapeutic agent with the most common side effects. |
300. The answer is h.
Doxorubicin is an antibiotic whose side effect is cardiac toxicity |
|
|
301. Match the chemotherapeutic agent with the most common side effects. |
301. The answer is i.
Vincristine arrests cells in metaphase by binding microtubular proteins and preventing the formation of mitotic spindles. Peripheral neuropathy is a common side effect. |
|
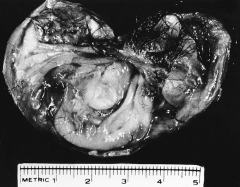
302. Match the figure with the correct description: |
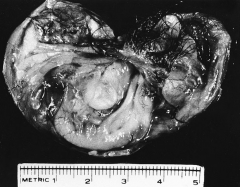
302. The answer is f. |
|
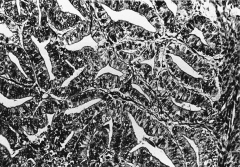
303. Match the figure with the correct description: |
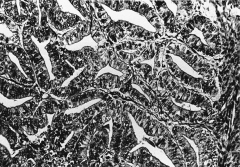
303. The answer is a. |
|
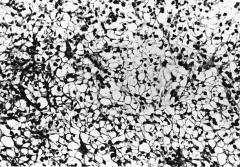
304. Match the figure with the correct description: |
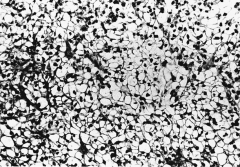
304. The answer is g. |
|
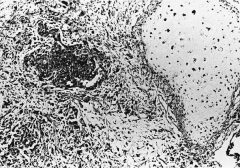
305. Match the figure with the correct description: |
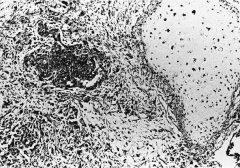
305. The answer is e. |
|
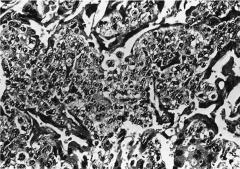
306. Match the figure with the correct description: |
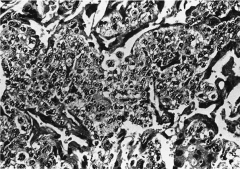
306. The answer is c. |
|
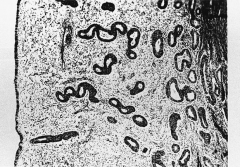
307. Match the figure with the correct description: |
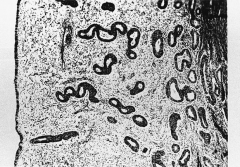
307. The answer is b. |
|
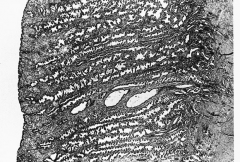
308. Match the figure with the correct description: |
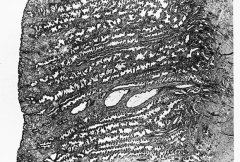
308. The answer is d. |
|
|
309. A patient is diagnosed with carcinoma of the breast. |
309. The answer is c. |
|
|
310. A 25-year-old woman presents to you for routine well-woman examination. She has had two normal vaginal deliveries and is healthy. She smokes one pack of cigarettes per day. She has no gynecologic complaints. Her last menstrual period was 3 weeks ago. During the pelvic examination, you notice that her left ovary is enlarged to 5 cm in diameter.
Which of the following is the best recommendation to this patient? a. Order CA-125 testing b. Schedule outpatient diagnostic laparoscopy c. Return to the office in 1 to 2 months to recheck the ovaries d. Schedule a CT scan of the pelvis e. Admit to the hospital for exploratory laparotomy |
310. The answer is c.
In young, menstruating women the most common reason for an enlargement of one ovary is the presence of a functional ovarian cyst. Functional cysts are physiologic, forming during the normal functioning of the ovaries. Follicular cysts are usually asymptomatic, unilateral, thin-walled, and filled with a watery, straw-colored fluid. Corpus luteum cysts are less common than follicular cysts. They are usually unilateral, but often appear complex, as they may be hemorrhagic. Patients with a corpus luteum cyst may complain of dull pain on the side of the affected ovary. Theca lutein cysts are the least common of the three types of functional ovarian cysts. They are almost always bilateral and are associated with pregnancy. Since the most common cause of a unilateral, asymptomatic ovarian cyst in a young, menstruating woman is a functional cyst, it is most reasonable to follow the patient conservatively and have her return after 1 to 2 months to recheck her ovary. More aggressive primary management with surgery is not indicated in a young, asymptomatic patient. CT scanning or pelvic ultrasonography may be indicated if the cyst is persistent. CA-125 is a cancer antigen expressed by approximately 80% of ovarian epithelial carcinomas. CA-125 testing is not very specific in women of childbearing age and is not useful for primary evaluation of an ovarian cyst in a young, asymptomatic patient. CA-125 testing is valuable in evaluating postmenopausal women with pelvic masses and in assessing treatment response in women undergoing treatment for CA-125 producing ovarian cancers. |
|
|
311. A 23-year-old woman presents to your office complaining of growths around her vaginal opening. Recently, the growths have been itching and bleeding. On physical examination she has several broad-based lesions measuring 2 to 4 cm in diameter along the posterior fourchette. Although there is no active bleeding, the largest lesion appears to have been bleeding recently.
Which of the following is the best way to treat this patient? a. Weekly application of podophyllin in the office b. Injection of 5-fluorouracil into the lesions c. Self-application of imiquimod to the lesions by the patient d. Weekly application of trichloroacetic acid in the office e. Local excision |
311. The answer is e.
The lesions are most likely condyloma acuminata, also known as venereal warts. Condyloma acuminata are squamous lesions caused by a human papillomavirus (HPV). The lesions reveal a treelike growth microscopically with a mantle that shows marked acanthosis and parakeratosis. Treatment options include local excision, cryosurgery, application of podophyllin or trichloroacetic acid, and laser therapy, although podophyllum is not recommended for extensive disease because of toxicity (peripheral neuropathy). For intractable condyloma of the vagina, 5-fluorouracil can be employed. Medical treatment with podophyllum, imiquimod, trichloroacetic acid, and 5-fluorouricil requires weeks or months of therapy to be effective. As this patient has large, bleeding lesions, local excision is the best treatment option. |
|
|
312. At the time of annual examination, a patient expresses concern regarding possible exposure to sexually transmitted diseases. During your pelvic examination, a single, indurated, nontender ulcer is noted on the vulva. Venereal Disease Research Laboratory (VDRL) and fluorescent treponemal antibody (FTA) tests are positive.
Without treatment, the next stage of this disease is clinically characterized by which of the following? a. Optic nerve atrophy and generalized paresis b. Tabes dorsalis c. Gummas d. Macular rash over the hands and feet e. Aortic aneurysm |
312. The answer is d.
Syphilis is a chronic disease produced by the spirochete Because of the spirochete’s extreme thinness, it is difficult to detect by light microscopy; therefore, spirochetes are diagnosed by use of a specially adapted technique known as dark-field microscopy. Clinically, syphilis is divided into primary, secondary, and tertiary (or late) stages. In primary syphilis a hard chancre develops. This is a painless ulcer with an indurated base that is usually found on the vulva, vagina, or cervix. Secondary syphilis is the result of hematogenous dissemination of the spirochetes and thus is a systemic disease. There are a number of systemic symptoms depending on the major organs involved. The classic rash of secondary syphilis is red macules and papules over the palms of the hands and the soles of the feet. The manifestations of late syphilis include optic atrophy, tabes dorsalis, generalized paresis, aortic aneurysm, and gummas of the skin and bones. |
|
|
313. A 24-year-old patient recently emigrated from the tropics. Four weeks ago she noted a small vulvar ulceration that spontaneously healed. Now there is painful inguinal adenopathy associated with malaise and fever. You are considering the diagnosis of lymphogranuloma venereum (LGV).
The diagnosis can be established by which of the following? a. Staining for Donovan bodies b. The presence of serum antibodies to Chlamydia trachomatis c. Positive Frei skin test d. Culturing Haemophilus ducreyi e. Culturing Calymmatobacterium granulomatis |
313. The answer is b.
Lymphogranuloma venereum (LGV) is a chronic infection produced by It is most commonly found in the tropics. The primary infection begins as a painless ulcer on the labia or vaginal vestibule; the patient usually consults the physician several weeks after the development of painful adenopathy in the inguinal and perirectal areas. Diagnosis can be established by culture or by demonstrating the presence of serum antibodies to The Frei skin test is no longer used because of its low sensitivity. The differential diagnosis includes syphilis, chancroid, granuloma inguinale, carcinoma, and herpes. Chancroid is a sexually transmitted disease caused by that produces a painful, tender ulceration of the vulva. Donovan bodies are present in patients with granuloma inguinale, which is caused by Therapy for both granuloma inguinale and LGV is administration of tetracycline. Chancroid is successfully treated with either azithromycin or ceftriaxone. |
|
|
314. One day after a casual sexual encounter with a bisexual man recently diagnosed as antibody-positive for human immunodeficiency virus (HIV), a patient is concerned about whether she may have become infected. A negative antibody titer is obtained.
To test for seroconversion, when is the earliest you should reschedule repeat antibody testing after the sexual encounter? a. 1 to 2 weeks b. 3 to 4 weeks c. 4 to 10 weeks d. 12 to 15 weeks e. 26 to 52 weeks |
314. The answer is c.
Persons at high risk for infection by HIV include homosexuals, bisexual males, women having sex with a bisexual or homosexual male partner, intravenous drug users, and hemophiliacs. The virus can be transmitted through sexual contact, use of contaminated needles or blood products, and perinatal transmission from mother to child. The antibody titer usually becomes positive 4 to 10 weeks after exposure, and the presence of the antibody provides no protection against AIDS. Because of occasional delayed appearance of the antibody after initial exposure, it is important to follow up patients for 1 year after exposure. |
|
|
315. A 22-year-old G3P0030 obese female comes to your office for a routine gynecologic examination. She is single, but is currently sexually active. She has a history of five sexual partners in the past, and became sexually active at age 15. She has had three first-trimester voluntary pregnancy terminations. She uses Depo-Provera for birth control, and reports occasionally using condoms as well. She has a history of genital warts, but denies any prior history of abnormal Pap smears. The patient denies use of any illicit drugs, but admits to smoking about one pack of cigarettes a day. Her physical examination is normal. However, 3 weeks later you receive the results of her Pap smear, which shows a high-grade squamous intraepithelial lesion (HGSIL).
Which of the following factors in this patient’s history does not increase her risk for cervical dysplasia? a. Young age at initiation of sexual activity b. Multiple sexual partners c. History of genital warts d. Use of Depo-Provera e. Smoking |
315. The answer is d.
The occurrence of cervical squamous dysplasia/carcinoma is caused by infection with the HPV, which is sexually transmitted. HPV causes genital warts as well. Women who begin sexual activity at a young age, have multiple sexual partners, do not use condoms, and have a history of sexually transmitted diseases are at an increased risk for cervical neoplasia. Alterations in immune function (such as in patients with HIV or on immunosuppressive therapy) place a patient at an increased risk of cervical neoplasia. Women who smoke tobacco have an increased risk of developing cervical neoplasia. There is no known increased risk of cervical dysplasia caused by use of Depo-Provera. However, some studies support an association of increased risk of cervical adenocarcinoma with oral contraceptive use. |
|
|
316. A 22-year-old woman presents for her first Pap smear. She has been sexually active with only one boyfriend since age 19. Her physical examination is completely normal. However, 2 weeks later her Pap smear results return showing HGSIL. There were no endocervical cells seen on the smear.
Which of the following is the most appropriate next step in the management of this patient? a. Perform a cone biopsy of the cervix b. Repeat the Pap smear to obtain endocervical cells c. Order HPV typing on the initial Pap smear d. Perform random cervical biopsies e. Perform colposcopy and directed cervical biopsies |
316. The answer is e.
Any patient with a Pap smear result that suggests dysplasia of the cervix should undergo colposcopy. The colposcope is a type of microscope that allows the physician to examine the cervix at a magnification of 10 to 16 times. The Pap smear is a cytological screening test for cervical neoplasm. A Pap smear result of high-grade squamous intraepithelial lesion (HGSIL) may be caused by moderate or severe cervical dysplasia or carcinoma in situ of the cervix. During colposcopy, 3% acetic acid is applied to the cervix. This allows the colposcopist to visualize abnormal blood vessels or acetowhite areas that could represent areas of dysplasia. Abnormal areas are then biopsied for histologic analysis. In patients with an HGSIL Pap, there is no indication for repeating the smear or ordering HPV testing as the cytological test suggests the presence of cervical neoplasia. Repeating a Pap could produce a false-negative result, which can lead to a delay in treatment of the patient. Random cervical biopsies are not indicated because the actual abnormal tissue may be missed. The indications for a cone biopsy would be (1) unsatisfactory colposcopic examination (ie, the entire transformation zone cannot be seen); (2) a colposcopically directed cervical biopsy that indicates the possibility of invasive disease; (3) neoplasm in the endocervix; or (4) cells seen on cervical biopsy that do not adequately explain the cells seen on cytologic examination (ie, the Pap). The absence of endocervical cells in an otherwise normal Pap smear in a patient with no history of abnormal Pap smears is not an indication for a repeat smear. However, in this patient, because of the absence of endocervical cells on the Pap smear, endocervical curettage is indicated to evaluate the endocervical canal for the presence of neoplasia. |
|
|
317. A 32-year-old woman consults with you for evaluation of an abnormal Pap smear done by a nurse practitioner at a family planning clinic. The Pap smear shows evidence of a high-grade squamous intraepithelial lesion (HGSIL). You perform colposcopy in the office. Your colposcopic impression is of acetowhite changes suggestive of human papilloma virus infection (HPV). Your biopsies show chronic cervicitis but no evidence of dysplasia.
Which of the following is the most appropriate next step in the management of this patient? a. Cryotherapy of the cervix b. Laser ablation of the cervix c. Conization of the cervix d. Hysterectomy e. Repeat the Pap smear in 3 to 6 months |
317. The answer is c.
As discussed in question 316, one of the indications for a cone biopsy is a cervical biopsy or colposcopic impression which does not adequately explain the severity of the Pap smear. In about 10% of colposcopically directed cervical biopsies, there will be a substantial discrepancy between the Pap smear and the biopsy results (ie, the biopsy is normal but the Pap indicates severely abnormal cells). A conization of the cervix is required to rule out lesions higher in the endocervical canal. Merely repeating the Pap smear is incorrect, because you may be delaying treatment of a serious problem. Once cervical dysplasia has been established, cryotherapy and laser ablation are viable treatment options. However, these are destructive procedures (ie, no tissue is preserved for histological evaluation) which should not be performed until a diagnosis is made. A hysterectomy should not be performed in this patient without resolving the discrepancy between the Pap smear and the colposcopic findings. |
|
|
318. A 55-year-old postmenopausal female presents to her gynecologist for a routine examination. She denies any use of hormone replacement therapy and does not report any menopausal symptoms. She denies the occurrence of any abnormal vaginal bleeding. She has no history of any abnormal Pap smears and has been married for 30 years to the same partner. She is currently sexually active with her husband on a regular basis. Two weeks after her examination, her Pap smear comes back as atypical glandular cells of undetermined significance (AGUS).
Which of the following is the most appropriate next step in the management of this patient? a. Repeat the Pap in 4 to 6 months b. HPV testing c. Hysterectomy d. Cone biopsy e. Colposcopy, endometrial biopsy, endocervical curettage |
318. The answer is e.
Approximately 0.5% of Pap smears come back with glandular cell abnormalities. These abnormalities can be associated with squamous lesions, adenocarcinoma in situ, or invasive adenocarcinoma. Therefore, any patient with AGUS should undergo immediate colposcopy and endocervical curettage. In addition, postmenopausal women should have endometrial sampling as the abnormality may be within the uterine cavity. Hysterectomy or conization might be indicated based on results of the colposcopy; however, colposcopy must be performed prior to these surgical procedures to establish a diagnosis. |
|
|
319. A 24-year-old G0 presents to your office complaining of vulvar discomfort. More specifically, she has been experiencing intense burning and pain with intercourse. The discomfort occurs at the vaginal introitus primarily with penile insertion into the vagina. The patient also experiences the same pain with tampon insertion and when the speculum is inserted during a gynecologic examination. The problem has become so severe that she can no longer have sex, which is causing problems in her marriage. She is otherwise healthy and denies any medical problems. She is experiencing regular menses and denies any dysmenorrhea. On physical examination, the region of the vulva around the vaginal vestibule has several punctate, erythematous areas of epithelium measuring 3 to 8 mm in diameter. Most of the lesions are located on the skin between the two Bartholin glands. Each inflamed lesion is tender to touch with a cotton swab.
Which of the following is the most likely diagnosis? a. Vulvar vestibulitis b. Atrophic vaginitis c. Contact dermatitis d. Lichen sclerosus e. Vulvar intraepithelial neoplasia |
319. The answer is a.
Vulvar vestibulitis is a syndrome of unknown etiology. To make the diagnosis of this disorder, the following three findings must be present: (1) severe pain on vestibular touch or attempted vaginal entry, (2) tenderness to pressure localized within the vulvar vestibule, and (3) visible findings confined to vulvar erythema of various degrees. To treat vulvar vestibulitis, the first step is to avoid tight clothing, tampons, hot tubs, and soaps, which can all act as vulvar irritants. If this fails, topical treatments include lidocaine, estrogen, and steroids. Tricyclic antidepressants and intralesional interferon injections have also been used. For women refractory to medical therapy, surgical excision of the vestibular mucosa may be helpful. Valtrex (valacyclovir) is an antiviral medication used in the treatment of genital herpes and is not indicated for vulvar vestibulitis. Contact dermatitis is an inflammation and irritation of the vulvar skin caused by a chemical irritant. The vulvar skin is usually red, swollen, and inflamed and may become weeping and eczemoid. Women with a contact dermatitis usually experience chronic vulvar tenderness, burning, and itching that can occur even when they are not engaging in intercourse. Atrophic vaginitis is a thinning and ulceration of the vaginal mucosa that occurs as a result of hypoestrogenism; thus this condition is usually seen in postmenopausal women not on hormone replacement therapy. Lichen sclerosus is another atrophic condition of the vulva. It is characterized by diffuse, thin whitish epithelial areas on the labia majora, minora, clitoris, and perineum. In severe cases, it may be difficult to identify normal anatomic landmarks. The most common symptom of lichen sclerosus is chronic vulvar pruritus. Vulvar intraepithelial neoplasia (VIN) are precancerous lesions of the vulva that have a tendency to progress to frank cancer. Women with VIN complain of vulvar pruritus, chronic irritation, and raised lesions. These lesions are most commonly located along the posterior vulva and in the perineal body and have a whitish cast and rough texture. |
|
|
320. After making a diagnosis in the patient in question 319, you recommended that she wear loose clothing and cotton underwear and to stop using tampons. After 1 month she returns, reporting that her symptoms of intense burning and pain with intercourse have not improved.
Which of the following treatment options is the best next step in treating this patient’s problem? a. Podophyllin b. Surgical excision of the vestibular glands c. Topical Xylocaine d. Topical trichloroacetic acid e. Valtrex therapy |
320. The answer is c.
Vulvar vestibulitis is a syndrome of unknown etiology. To make the diagnosis of this disorder, the following three findings must be present: (1) severe pain on vestibular touch or attempted vaginal entry, (2) tenderness to pressure localized within the vulvar vestibule, and (3) visible findings confined to vulvar erythema of various degrees. To treat vulvar vestibulitis, the first step is to avoid tight clothing, tampons, hot tubs, and soaps, which can all act as vulvar irritants. If this fails, topical treatments include lidocaine, estrogen, and steroids. Tricyclic antidepressants and intralesional interferon injections have also been used. For women refractory to medical therapy, surgical excision of the vestibular mucosa may be helpful. Valtrex (valacyclovir) is an antiviral medication used in the treatment of genital herpes and is not indicated for vulvar vestibulitis. Contact dermatitis is an inflammation and irritation of the vulvar skin caused by a chemical irritant. The vulvar skin is usually red, swollen, and inflamed and may become weeping and eczemoid. Women with a contact dermatitis usually experience chronic vulvar tenderness, burning, and itching that can occur even when they are not engaging in intercourse. Atrophic vaginitis is a thinning and ulceration of the vaginal mucosa that occurs as a result of hypoestrogenism; thus this condition is usually seen in postmenopausal women not on hormone replacement therapy. Lichen sclerosus is another atrophic condition of the vulva. It is characterized by diffuse, thin whitish epithelial areas on the labia majora, minora, clitoris, and perineum. In severe cases, it may be difficult to identify normal anatomic landmarks. The most common symptom of lichen sclerosus is chronic vulvar pruritus. Vulvar intraepithelial neoplasia (VIN) are precancerous lesions of the vulva that have a tendency to progress to frank cancer. Women with VIN complain of vulvar pruritus, chronic irritation, and raised lesions. These lesions are most commonly located along the posterior vulva and in the perineal body and have a whitish cast and rough texture. |
|
|
321. A 29-year-old G0 comes to your office complaining of a vaginal discharge for the past 2 weeks. The patient describes the discharge as thin in consistency and of a grayish white color. She has also noticed a slight fishy vaginal odor that seems to have started with the appearance of the discharge. She denies any vaginal or vulvar pruritus or burning. She admits to being sexually active in the past, but has not had intercourse during the past year. She denies a history of any sexually transmitted diseases. She is currently on no medications with the exception of her birth control pills. Last month she took a course of amoxicillin for treatment of a sinusitis. On physical examination, the vulva appears normal. There is a discharge present at the introitus. A copious, thin, whitish discharge is in the vaginal vault and adherent to the vaginal walls. The vaginal pH is 5.5. The cervix is not inflamed and there is no cervical discharge. Wet smear of the discharge indicates the presence of clue cells.
Which of the following is the most likely diagnosis? a. Candidiasis b. Bacterial vaginosis c. Trichomoniasis d. Physiologic discharge e. Chlamydia |
321. The answer is b.
Bacterial vaginosis is a condition in which there is an overgrowth of anaerobic bacteria in the vagina, displacing the normal lactobacillus. Women with this type of vaginitis complain of an unpleasant vaginal odor that is described as musky or fishy and a thin, gray-white vaginal discharge. Vulvar irritation and pruritus are rarely present. To confirm the diagnosis of bacterial vaginosis, a wet smear is done. To perform a wet smear, saline is mixed with the vaginal discharge and clue cells are identified. Clue cells are vaginal epithelial cells with clusters of bacteria adherent to their surfaces. In addition, a whiff test can be performed by mixing potassium hydroxide with the vaginal discharge. In cases of bacterial vaginosis, an amine-like (ie, fishlike) odor will be detected. The treatment of choice for bacterial vaginosis is metronidazole (Flagyl) 500 mg given twice daily for 7 days. Pregnant women with symptomatic bacterial vaginosis (BV) should be treated the same way as nonpregnant women with BV. In cases of a normal or physiologic discharge, vaginal secretions are white and odorless. In addition, normal vaginal secretions do not adhere to the vaginal side walls. In cases of candidiasis, patients commonly complain of vulvar burning, pain, pruritus, and erythema. The vaginal discharge tends to be white, granular, and adherent to the vaginal walls. A wet smear with potassium hydroxide can confirm the diagnosis by the identification of hyphae. Treatment of candidiasis can be achieved with the administration of topical imidazoles or triazoles or the oral medication Diflucan. vaginitis is the most common nonviral, nonchlamydial sexually transmitted disease of women. It is caused by the anaerobic, flagellated protozoan Women with vaginitis commonly complain of a copious vaginal discharge that may be white, yellow, green, or gray and that has an unpleasant odor. Some women complain of vulvar pruritus, which is primarily confined to the vestibule and labia minora. On physical examination, the vulva and vagina frequently appear red and swollen. Only a small percentage of women possess the classically described strawberry cervix. Diagnosis of trichomoniasis is confirmed with a wet saline smear. Under the microscope, the organisms can be visualized; these organisms are unicellular protozoans that are spherical in shape with three to five flagella extending from one end. The recommended treatment for trichomoniasis is a one-time dose of metronidazole 2 g PO. is an intracellular parasite that can cause an infection that may be manifested as cervicitis, urethritis, or salpingitis. Patients with chlamydial infections may be asymptomatic. On physical examination, women with chlamydial infections may demonstrate a mucopurulent cervicitis. The diagnosis of chlamydia is suspected on clinical examination and confirmed with cervical cultures. Treatment for a chlamydial cervicitis is with oral azithromycin 1 g or doxycycline 100 mg twice daily for 7 days. |
|
|
322. A 29-year-old G0 comes to your office complaining of a vaginal discharge for the past 2 weeks. The patient describes the discharge as thin in consistency and of a grayish white color. She has also noticed a slight fishy vaginal odor that seems to have started with the appearance of the discharge. She denies any vaginal or vulvar pruritus or burning. She admits to being sexually active in the past, but has not had intercourse during the past year. She denies a history of any sexually transmitted diseases. She is currently on no medications with the exception of her birth control pills. Last month she took a course of amoxicillin for treatment of a sinusitis. On physical examination, the vulva appears normal. There is a discharge present at the introitus. A copious, thin, whitish discharge is in the vaginal vault and adherent to the vaginal walls. The vaginal pH is 5.5. The cervix is not inflamed and there is no cervical discharge. Wet smear of the discharge indicates the presence of clue cells.
Which of the following is the best treatment? a. Reassurance b. Oral Diflucan c. Doxycycline 100 mg PO twice daily for 1 week d. Ampicillin 500 mg PO twice daily for 1 week e. Metronidazole 500 mg PO twice daily for 1 week |
322. The answer is e.
Bacterial vaginosis is a condition in which there is an overgrowth of anaerobic bacteria in the vagina, displacing the normal lactobacillus. Women with this type of vaginitis complain of an unpleasant vaginal odor that is described as musky or fishy and a thin, gray-white vaginal discharge. Vulvar irritation and pruritus are rarely present. To confirm the diagnosis of bacterial vaginosis, a wet smear is done. To perform a wet smear, saline is mixed with the vaginal discharge and clue cells are identified. Clue cells are vaginal epithelial cells with clusters of bacteria adherent to their surfaces. In addition, a whiff test can be performed by mixing potassium hydroxide with the vaginal discharge. In cases of bacterial vaginosis, an amine-like (ie, fishlike) odor will be detected. The treatment of choice for bacterial vaginosis is metronidazole (Flagyl) 500 mg given twice daily for 7 days. Pregnant women with symptomatic bacterial vaginosis (BV) should be treated the same way as nonpregnant women with BV. In cases of a normal or physiologic discharge, vaginal secretions are white and odorless. In addition, normal vaginal secretions do not adhere to the vaginal side walls. In cases of candidiasis, patients commonly complain of vulvar burning, pain, pruritus, and erythema. The vaginal discharge tends to be white, granular, and adherent to the vaginal walls. A wet smear with potassium hydroxide can confirm the diagnosis by the identification of hyphae. Treatment of candidiasis can be achieved with the administration of topical imidazoles or triazoles or the oral medication Diflucan. vaginitis is the most common nonviral, nonchlamydial sexually transmitted disease of women. It is caused by the anaerobic, flagellated protozoan Women with vaginitis commonly complain of a copious vaginal discharge that may be white, yellow, green, or gray and that has an unpleasant odor. Some women complain of vulvar pruritus, which is primarily confined to the vestibule and labia minora. On physical examination, the vulva and vagina frequently appear red and swollen. Only a small percentage of women possess the classically described strawberry cervix. Diagnosis of trichomoniasis is confirmed with a wet saline smear. Under the microscope, the organisms can be visualized; these organisms are unicellular protozoans that are spherical in shape with three to five flagella extending from one end. The recommended treatment for trichomoniasis is a one-time dose of metronidazole 2 g PO. is an intracellular parasite that can cause an infection that may be manifested as cervicitis, urethritis, or salpingitis. Patients with chlamydial infections may be asymptomatic. On physical examination, women with chlamydial infections may demonstrate a mucopurulent cervicitis. The diagnosis of chlamydia is suspected on clinical examination and confirmed with cervical cultures. Treatment for a chlamydial cervicitis is with oral azithromycin 1 g or doxycycline 100 mg twice daily for 7 days. |
|
|
323. A 20-year-old G2P0020 with an LMP 5 days ago presents to the emergency room complaining of a 24-hour history of increasing pelvic pain. This morning she experienced chills and a fever, although she did not take her temperature. She reports no changes in her urine or bowel habits. She has had no nausea or vomiting. She is hungry. She denies any medical problems. Her only surgery was a laparoscopy performed last year for an ectopic pregnancy. She reports regular menses and denies dysmenorrhea. She is currently sexually active. She has a new sexual partner and had sexual intercourse with him just prior to her last menstrual period. She denies a history of any abnormal Pap smears or sexually transmitted diseases. Urine pregnancy test is negative. Urinalysis is completely normal. WBC is 18,000. Temperature is 38.8°C (102°F). On physical examination, her abdomen is diffusely tender in the lower quadrants with rebound and voluntary guarding. Bowel sounds are present but diminished.
Which of the following is the most likely diagnosis? a. Ovarian torsion b. Endometriosis c. Pelvic inflammatory disease d. Kidney stone e. Ruptured ovarian cyst |
323. The answer is c.
Ovarian torsion, appendicitis, and acute salpingitis are all commonly associated with fever, abdominal pain, and elevated white blood cell count. Ruptured ovarian cysts present with acute abdominal pain without fever. Ovarian torsion is usually associated with an adnexal mass. Pain from ruptured ovarian cysts may occur at any time throughout the menstrual cycle but often present around the time of ovulation. Although appendicitis is in the differential diagnosis in any woman presenting with abdominal pain and fever, it is unlikely in the patient in question 323 as she has had no nausea, vomiting, or anorexia. In cases of kidney stone, urinalysis usually indicates the presence of blood. In addition, the pain is usually in the flank areas. The timing of the symptoms of the patient in question 323 and her history of a new sexual partner make acute salpingitis the most likely diagnosis. A tubo-ovarian abscess (TOA) may form in a patient with untreated pelvic inflammatory disease. A patient with a tubo-ovarian abscess should be initially hospitalized and treated with intravenous antibiotics. Patients with TOAs, who does not improve on broad-spectrum antibiotics, may require drainage of the abscesses by laparotomy, laparoscopy, or percutaneously under CT guidance. The recommendation of Centers for Disease Control for inpatient management of PID includes the following: 1. Cefoxitin 2 g IV every 6 hours or cefotetan 2 g IV every 12 hours plus doxycycline 100 mg PO or IV twice daily 2. Clindamycin 900 mg IV every 8 hours plus gentamicin loading dose IV or IM (2 mg/kg) followed by maintenance dose (1.5 mg/kg) every 8 hours The recommendation of Centers for Disease Control for the outpatient management of PID includes the following: 1. Cefoxitin 2 g IM plus probenecid 1 g PO in a single dose concurrently or ceftriaxone 250 mg IM plus doxycycline 100 mg PO twice daily for 14 days 2. Ofloxacin 400 mg PO two times a day for 14 days plus either clindamycin 450 mg PO four times a day or metronidazole 500 mg PO two times a day for 14 days The decision for inpatient versus outpatient treatment of a patient with pelvic inflammatory disease depends upon several factors such as patient compliance, tolerance of oral medications, and certainty of diagnosis. |
|
|
324. A 32-year-old women presents to the emergency room complaining of severe lower abdominal pain. She says she was diagnosed with pelvic inflammatory disease by her gynecologist last month, but did not take the medicine that she was prescribed because it made her throw up. She has had fevers on and off for the past 2 weeks. In the emergency room, the patient has a temperature of 38.3°C (101°F). Her abdomen is diffusely tender, but more so in the lower quadrants. She has diminished bowel sounds. On bimanual pelvic examination, bilateral adnexal masses are palpated. The patient is sent to the ultrasound department, and a transvaginal pelvic ultrasound demonstrates bilateral tubo-ovarian abscesses.
Which of the following is the most appropriate next step in the management of this patient? a. Admit the patient for emergent laparoscopic drainage of the abscesses. b. Call interventional radiology to perform CT-guided percutaneous drainage of the abscesses. c. Send the patient home and arrange for intravenous antibiotics to be administered by a home health agency. d. Admit the patient for intravenous antibiotic therapy. e. Admit the patient for exploratory laparotomy, TAH/BSO. |
324. The answer is d.
Ovarian torsion, appendicitis, and acute salpingitis are all commonly associated with fever, abdominal pain, and elevated white blood cell count. Ruptured ovarian cysts present with acute abdominal pain without fever. Ovarian torsion is usually associated with an adnexal mass. Pain from ruptured ovarian cysts may occur at any time throughout the menstrual cycle but often present around the time of ovulation. Although appendicitis is in the differential diagnosis in any woman presenting with abdominal pain and fever, it is unlikely in the patient in question 323 as she has had no nausea, vomiting, or anorexia. In cases of kidney stone, urinalysis usually indicates the presence of blood. In addition, the pain is usually in the flank areas. The timing of the symptoms of the patient in question 323 and her history of a new sexual partner make acute salpingitis the most likely diagnosis. A tubo-ovarian abscess (TOA) may form in a patient with untreated pelvic inflammatory disease. A patient with a tubo-ovarian abscess should be initially hospitalized and treated with intravenous antibiotics. Patients with TOAs, who does not improve on broad-spectrum antibiotics, may require drainage of the abscesses by laparotomy, laparoscopy, or percutaneously under CT guidance. The recommendation of Centers for Disease Control for inpatient management of PID includes the following: 1. Cefoxitin 2 g IV every 6 hours or cefotetan 2 g IV every 12 hours plus doxycycline 100 mg PO or IV twice daily 2. Clindamycin 900 mg IV every 8 hours plus gentamicin loading dose IV or IM (2 mg/kg) followed by maintenance dose (1.5 mg/kg) every 8 hours The recommendation of Centers for Disease Control for the outpatient management of PID includes the following: 1. Cefoxitin 2 g IM plus probenecid 1 g PO in a single dose concurrently or ceftriaxone 250 mg IM plus doxycycline 100 mg PO twice daily for 14 days 2. Ofloxacin 400 mg PO two times a day for 14 days plus either clindamycin 450 mg PO four times a day or metronidazole 500 mg PO two times a day for 14 days The decision for inpatient versus outpatient treatment of a patient with pelvic inflammatory disease depends upon several factors such as patient compliance, tolerance of oral medications, and certainty of diagnosis. |
|
|
325. A 36-year-old woman presents to the emergency room complaining of pelvic pain, fever, and vaginal discharge. She has had nausea and vomiting and cannot tolerate liquids at the time of her initial evaluation. The emergency room physician diagnoses her with pelvic inflammatory disease and asks you to admit her for treatment.
Which of the following is the most appropriate initial antibiotic treatment regimen for this patient? a. Doxycycline 100 mg PO twice daily for 14 days b. Clindamycin 450 mg IV every 8 hours plus gentamicin 1 mg/kg load followed by 1 mg/kg every 12 hours c. Cefoxitin 2 g IV every 6 hours with doxycycline 100 mg IV twice daily d. Ceftriaxone 250 mg IM plus doxycycline 100 mg PO twice daily for 14 days e. Ofloxacin 400 mg PO twice daily for 14 days plus Flagyl 500 mg PO twice daily for 14 days |
325. The answer is c. Ovarian torsion, appendicitis, and acute salpingitis are all commonly associated with fever, abdominal pain, and elevated white blood cell count. Ruptured ovarian cysts present with acute abdominal pain without fever. Ovarian torsion is usually associated with an adnexal mass. Pain from ruptured ovarian cysts may occur at any time throughout the menstrual cycle but often present around the time of ovulation. Although appendicitis is in the differential diagnosis in any woman presenting with abdominal pain and fever, it is unlikely in the patient in question 323 as she has had no nausea, vomiting, or anorexia. In cases of kidney stone, urinalysis usually indicates the presence of blood. In addition, the pain is usually in the flank areas. The timing of the symptoms of the patient in question 323 and her history of a new sexual partner make acute salpingitis the most likely diagnosis. A tubo-ovarian abscess (TOA) may form in a patient with untreated pelvic inflammatory disease. A patient with a tubo-ovarian abscess should be initially hospitalized and treated with intravenous antibiotics. Patients with TOAs, who does not improve on broad-spectrum antibiotics, may require drainage of the abscesses by laparotomy, laparoscopy, or percutaneously under CT guidance. The recommendation of Centers for Disease Control for inpatient management of PID includes the following:
1. Cefoxitin 2 g IV every 6 hours or cefotetan 2 g IV every 12 hours plus doxycycline 100 mg PO or IV twice daily 2. Clindamycin 900 mg IV every 8 hours plus gentamicin loading dose IV or IM (2 mg/kg) followed by maintenance dose (1.5 mg/kg) every 8 hours The recommendation of Centers for Disease Control for the outpatient management of PID includes the following: 1. Cefoxitin 2 g IM plus probenecid 1 g PO in a single dose concurrently or ceftriaxone 250 mg IM plus doxycycline 100 mg PO twice daily for 14 days 2. Ofloxacin 400 mg PO two times a day for 14 days plus either clindamycin 450 mg PO four times a day or metronidazole 500 mg PO two times a day for 14 days The decision for inpatient versus outpatient treatment of a patient with pelvic inflammatory disease depends upon several factors such as patient compliance, tolerance of oral medications, and certainty of diagnosis. |
|
|
326. A 43-year-old G2P2 comes to your office complaining of an intermittent right nipple discharge that is bloody. She reports that the discharge is spontaneous and not associated with any nipple pruritus, burning, or discomfort. On physical examination, you do not detect any dominant breast masses or adenopathy. There are no skin changes noted. |
326. The answer is c.
Nipple discharge can occur in women with either benign or malignant breast conditions. Approximately 10% to 15% of women with benign breast disease complain of nipple discharge. However, nipple discharge is present in only about 3% of women with breast malignancies. The most worrisome nipple discharges tend to be spontaneous, unilateral, and persistent. The color of nipple discharge does not differentiate benign from malignant breast conditions. The most common breast disorder associated with a bloody nipple discharge is an intraductal papilloma. However, breast carcinoma must always be ruled out in any patient complaining of a bloody nipple discharge. Sanguineous or serosanguineous nipple discharges can also be seen in women with duct ectasia and fibrocystic breast disease. Women with hyperprolactinemia caused by a pituitary adenoma experience bilateral milky white nipple discharges. |
|
|
327. A 20-year-old G0, LMP 1 week ago, presents to your gynecology clinic complaining of a mass in her left breast that she discovered during routine breast self-examination in the shower. When you perform a breast examination on her, you palpate a 2-cm firm, non-tender mass in the upper inner quadrant of the left breast that is smooth, well-circumscribed, and mobile. You do not detect any skin changes, nipple discharge, or axillary lymphadenopathy.
Which of the following is the most likely diagnosis? a. Fibrocystic breast change b. Fibroadenoma c. Breast carcinoma d. Fat necrosis e. Cystosarcoma phyllodes |
327. The answer is b.
This patient’s breast mass is characteristic of a fibroadenoma. Fibroadenomas are the second most common benign breast disorder, after fibrocystic changes. Fibroadenomas are characterized by the presence of a firm, solid, well-circumscribed, nontender, freely mobile mass and have an average diameter of 2.5 cm. These lesions most commonly occur in adolescents and women in their twenties. Fibrocystic changes occur in about one-third to one-half of reproductive- age women and represent an exaggerated response of the breast tissue to hormones. Patients with fibrocystic changes complain of bilateral mastalgia and breast engorgement preceding menses. On physical examination, diffuse bilateral nodularity is typically encountered. Cystosarcoma phyllodes are rare fibroepithelial tumors that constitute 1% of breast malignancies. These rapidly growing tumors are the most frequent breast sarcoma and occur most frequently in women in the fifth decade of life. Trauma to the breast can result in fat necrosis. Women with fat necrosis commonly present to the physician with a firm, tender mass that is surrounded by ecchymosis. Occasional skin retraction can occur, making this lesion difficult to differentiate from cancer. It is unlikely that this patient who presents in her twenties has breast cancer. Fine-needle aspiration or excisional biopsy may be performed to rule out the rare chance of malignancy, but breast cancer is not the most likely diagnosis based on the patient’s age and lack of any other breast changes consistent with carcinoma (such as a fixed mass, skin retraction, or lymphadenopathy). |
|
|
328. You have a 32-year-old G1P0 patient who has undergone a routine obstetrical ultrasound screening at 20 weeks of gestation. The patient phones you immediately following the ultrasound because during the procedure the ultrasonographer commented that she noted several small fibroid tumors in the patient’s uterus. As this is the patient’s first pregnancy, she is concerned regarding the possible effects that the fibroid tumors may have on the outcome of her pregnancy.
As her obstetrician, which of the following should you tell her? a. Enlargement of the fibroids with subsequent necrosis and degeneration during pregnancy is common. b. Many women have fibroid tumors, but most fibroids are asymptomatic during pregnancy. c. Progression to leiomyosarcoma is more common in pregnancy attributed to the hormonal effects of the pregnancy. d. Preterm labor occurs frequently, even in women with asymptomatic fibroid tumors. e. She will have to have a cesarean delivery because the fibroid tumors will obstruct the birth canal. |
328. The answer is b.
Uterine fibroids or myomas are benign smooth muscle tumors of the uterus. They are present in about 30% to 50% of American women. In pregnancy, most women with fibroids are asymptomatic and do not require therapy. Uterine myomas are hormonally responsive and grow in response to estrogen exposure. Uncommonly, during pregnancy a woman with fibroids may have an increase in size of these fibroids to the point where they outgrow their blood supply and undergo carneous degeneration. Fibroid degeneration may lead to preterm labor. Uterine fibroids can also be associated with fetal malpresentation caused by distortion of the endometrial cavity. They may also contribute to postpartum hemorrhage caused by inability of the uterine muscle to contract normally after delivery. Uterine leiomyosarcomas are smoothmuscle malignancies characterized by more than 5 mitoses per 10 hpf on microscopic examination. These malignancies are not thought to arise from benign fibroids but occur de novo. Uterine leiomyosarcomas typically occur in postmenopausal women who present with a rapidly enlarging uterus. |
|
|
329. A 55-year-old G3P3 with a history of fibroids presents to you complaining of irregular vaginal bleeding. Until last month, she had not had a period in over 9 months. She thought she was in menopause, but because she started bleeding again last month she is not sure. Over the past month she has had irregular, spotty vaginal bleeding. The last time she bled was 1 week ago. She also complains of frequent hot flushes and emotional lability. She does not have any medical problems and is not taking any medications. She is a nonsmoker and denies any alcohol or drug use. Her gynecologic history is significant for cryotherapy of the cervix 10 years ago for moderate dysplasia. She has had three cesarean sections and a tubal ligation. On physical examination, her uterus is 12 weeks in size and irregularly shaped. Her ovaries are not palpable. A urine pregnancy test is negative.
Which of the following is the most reasonable next step in the evaluation of this patient? a. Schedule her for a hysterectomy. b. Insert a progesterone-containing intrauterine device (IUD). c. Arrange for outpatient endometrial ablation. d. Perform an office endometrial biopsy. e. Arrange for outpatient conization of the cervix. |
329. The answer is d.
Given this patient’s age and symptoms, she is probably menopausal. Women with postmenopausal bleeding should be evaluated with an endometrial biopsy prior to any medical treatment or surgical intervention (such as hysterectomy or endometrial ablation). A pelvic ultrasound would also be helpful in the management of this patient and would offer information regarding the size and location of any uterine fibroids or polyps. There is no indication for conization of the cervix in this patient. Conization of the cervix is done for evaluation and treatment of cervical dysplasia. Progesterone-containing IUDs are used in premenopausal women for contraception and some physicians use them 'off label' in the treatment of menorrhagia. There is no indication for inserting a progesterone-containing IUD in this patient. |
|
|
330. A 57-year-old menopausal patient presents to your office for evaluation of postmenopausal bleeding. She is morbidly obese and has chronic hypertension and adult onset diabetes. An endometrial sampling done in the office shows complex endometrial hyperplasia with atypia, and a pelvic ultrasound done at the hospital demonstrates multiple, large uterine fibroids. |
330. The answer is b. |

