![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
61 Cards in this Set
- Front
- Back
|
Divisions of the Extrinsic Nervous System
|
1) Parasympathetic 2) Sympathetic
|
|
|
GI and Parasympathetic Nervous System: Nerves
|
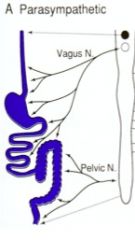
1) Vagus nerve 2) Pelvic nerve
|
|
|
Vagus Nerve Innervation
|
Innervates: 1) Esophagus 2) Stomach 3) Small intestine 4) Upper colon
|
|
|
Pelvic Nerve Innervation
|
Innervates: 1) Descending colon 2) Sigmoid colon 3) Rectum 4) Anal canal
|
|
|
Vagovagal Reflex
|
1) Information from receptors in mucosa and smooth muscle relayed to CNS via vagus nerve afferents 2) Triggers a response that is carried back to GI tract via vagus nerve efferents
|
|
|
GI and Sympathetic Nervous System: Innervation
|

1) Nerve fibers typically synapse outside GI tract in prevertebral ganglia 2) A few innervate blood vessels and secretory cells directly.
|
|
|
Enteric/Intrinsic Nervous System Function
|
1) Relay information to and from gut via extrinsic system 2) Stimulus in one part of GI tract can produce response in another part in absence
of extrinsic nervous system |
|
|
Enteric/Intrinsic Nervous System Structure
|
Networks formed by myenteric and submucosal plexuses
|
|
|
Enteric/Intrinsic Nervous System Innervation
|
Innervate: 1) Blood vessels 2) Smooth muscle 3) Secretory cells 4) Endocrine cells
|
|
|
G Cell Secretion
|
Gastrin
|
|
|
Parietal Cell Secretion
|
Gastric acid (HCl)
|
|
|
Steatorrhea
|
Excess fat in stools
|
|
|
CCK
|

1) Cholecystokinin 2) Secreted by I cells 3) Released in response to: A) Small peptides B) Amino acids C) Fatty acids D) Monoglycerides (containing 8 or more carbon atoms) 4) Stimulates: A) Gallbladder contraction B) Pancreatic enzyme secretion 5) Potentiates pancreatic bicarbonate secretion 6) Inhibits gastric emptying
|
|
|
I Cell Secretion
|
CCK
|
|
|
Reason Fatty Meals Empty More Slowly than Non-Fat Meals
|
CCK, released in response to fatty acids, inhibits gastric emptying
|
|
|
Secretin
|
1) Released by S cells 2) Stimulates: a) Bicarbonate b) Water secretion in: i) pancreas ii) liver 3) Increases bile production 4) Inhibits gastric acid secretion 5) Released in response to acid
|
|
|
S Cells
|
1) Duodenum 2) Secretes secretin in response to acid
|
|
|
GIP
|
1) Glucose-dependent insulinotropic peptide 2) Secreted by K cells 3) Released in response to: A) Fat B) Protein C) Carbohydrate 4) Stimulates insulin release from pancreas
|
|
|
K Cells
|
1) Duodenum and jejunum) 2) Secretes GIP in response to: A) Fat B) Protein C) Carbohydrate
|
|
|
Why Is Oral Glucose Load More Effective than IV Glucose in Causing Insulin Release?
|
1) IV glucose circulates through the blood and therefore fails to stimulate the GIP secreting K cells of the small intestine which stimulate insulin release from pancreas 2) Oral glucose passes through the small intestine, stimulating GIP and insulin release
|
|
|
Motilin
|
1) Released cyclically about every 90 minutes from upper small intestine (duodenum and jejunum) during fasting
2) Stimulates migrating myoelectric complex in: A) Stomach B) Small intestine 3) Release abolished by eating |
|
|
Gastrointestinal Peptides: Types
|

1) Hormones 2) Paracrines 3) Neurocrines
|
|
|
Gastrointestinal Peptides: Hormones
|
1) Gastrin 2) CCK 3) Secretin 4) GIP 5) Motilin
|
|
|
Gastrointestinal Peptides: Paracrines
|
1) Somatostatin 2) Histamine
|
|
|
Gastrointestinal Peptides: Neurocrines
|
1) VIP 2) GRP 3) Enkephalins
|
|
|
Somatostatin
|
1) Secreted by D cells 2) Inhibits: A) Gastric acid secretion B) Release of gastrin C) Release of all GI hormones
|
|
|
D Cells
|
1) Throughout GI tract 2) Release somatostatin in response to acid in lumen
|
|
|
Histamine
|
1) Secreted by ECL cells 2) Increases gastric acid secretion: A) Directly B) Potentiating effects of: a) gastrin b) ACh 3) Releaser: gastrin
|
|
|
ECL Cells
|
1) Enterochromaffin-like cells 2) Located in acid secreting portion of stomach 3) Secrete histamine in response to acid
|
|
|
VIP
|
1) Vasoactive intestinal peptide 2) Released from nerves in: A) Mucosa B) Smooth muscle of GI tract 3) Relaxes smooth muscle of GI 4) Stimulates: A) Intestinal secretion B) Pancreatic secretion 5) Secreted from pancreatic islet cell tumor
|
|
|
Gastrin
|
1) Secreted by G cells 2) Released in response to: A) Peptides B) Amino acids C) Distension of stomach D) Vagal stimulation 3) Stimulates HCl secretion 4) Increased in Zollinger-Ellison syndrome
|
|
|
Gastrinoma
|
1) Tumor in the pancreas or duodenum that secretes excess of gastrin 2) Implicated in Zollinger-Ellison syndrome
|
|
|
GRP
|
1) Gastrin-releasing peptide or bombesin 2) Released from nerves in gastric mucosa in response to vagal stimulation 3) Stimulates gastrin release
|
|
|
Gastric Mucosa
|
1) Contains nerves that release GRP 2) Responds to vagal stimulation
|
|
|
Enkephalins
|
1) Secreted from: A) Nerves of mucosa and smooth muscle of GI tract 2) Stimulate GI smooth muscle contraction: A) lower esophageal B) Pyloric C) Ileocecal sphincters 3) Inhibit intestinal secretion of: A) Fluid B) Electrolytes
|
|
|
Slow Wave Contraction Couplet
|
Slow waves without contractions, but not contractions without slow waves
|
|
|
Slow Waves
|
1) Smooth muscle cell potential rhythmically depolarizes and polarizes 2) Also called Basic Electrical Rhythm (BER) 3) Not action potentials
|
|
|
Cells of Cajal
|
1) Generate slow waves 2) Interstitial
|
|
|
Slow Wave Dispensation
|
1) Begin in cells of Cajal 2) Spread to other cells via gap junctions
|
|
|
Slow Wave Generation: Depolarization Phase
|
Ca++ influx
|
|
|
Slow Wave Generation: Plateau Phase
|
Ca++ influx
|
|
|
Slow Wave Generation: Repolarization Phase
|
K+ efflux
|
|
|
Slow Waves: Requirement for Contraction
|

Plateau phase must exceed threshold
|
|
|
Slow Waves: Plateau Exceeds Threshold
|
1) Voltage-gated Ca++ channels open 2) Ca++ enters 3) AP initiated
|
|
|
Slow Waves: Function of Action Potential
|
1) Increase strength and duration of contraction 2) Required for contraction everywhere except stomach
|
|
|
Slow Waves: Stomach Contractions and Action Potential
|
1) May occur in absence of AP 2) AP almost always present
|
|
|
Slow Waves: Affect of Neural and Hormonal Input on Frequency
|
Little affect on frequency of slow waves
|
|
|
Smooth Muscle Action Potentials: Neural and Hormonal Input
|
Influence variations in membrane potentials: 1) Produce AP, thus contractions 2) Inhibit AP 3) Determine strength of contractions
|
|
|
Slow Waves: Frequency
|
Sets maximum frequency for contraction of given part of GI tract
|
|
|
G Cell Location
|
Stomach
|
|
|
Parietal Cell Location
|
Stomach
|
|
|
Signals for CCK Release
|
1) Small peptides 2) Amino acids 3) Fatty acids 4) Monoglycerides (containing 8 or more carbon atoms)
|
|
|
CCK Stimulates
|
1) Gallbladder contraction 2) Pancreatic enzyme secretion
|
|
|
CCK Releasing Cell
|
I cell
|
|
|
CCK Inhibits
|
Gastric emptying
|
|
|
CCK Potentiates
|
Pancreatic bicarbonate secretion
|
|
|
I Cell Location
|
Proximal small intestine: duodenum and jejunum
|
|
|
Secretin Stimulates
|
Bicarbonate and water secretion in liver and pancreas
|
|
|
Secretin Increases
|
Bile production
|
|
|
Secretin Inhibits
|
Gastric acid secretion by parietal cells
|
|
|
Signals for Secretin Release
|
Acid
|

