![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
75 Cards in this Set
- Front
- Back
|
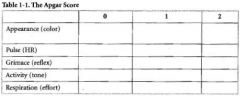
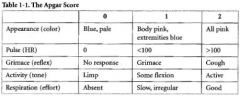
The APGAR helps identify infants who require what?
What does it stand for? |
Resuscitation
Appearance, Pulse, Grimace, Activity, Respiration |
|

-
|
-
|
|
|
A newborn infant has a blue-gray pigmented lesion on the sacral area. It is clearly demarcated & does not fade into the surrounding skin. What is the most likely diagnosis? What must you differentiate them from...how?
|
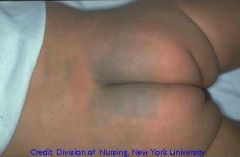
Mongolian Spots
Child Abuse = fade into surrounding skin & have different colors |
|
|
Describe Erythema Toxicum
1. when do they appear? 2. what are they full of when scraped? 3. what must you differentiate it from? |
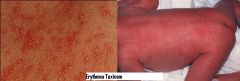
Small papules or pustules on a red base (50% of full-term babies have it!!!)
1. appear AFTER the 1st day & may last several weeks 2. Eosinophils 3. Staphylococcal Scalded Skin Syndrome = full of neutrophils, skin culture reveals S. aureus, & infant looks ill. |
|
|
Milia
Small inclusion cysts & are pearly white Epstein's Pearls **these benign lesions usually exfoliate & disappear within the first few weeks. No treatment necessary |
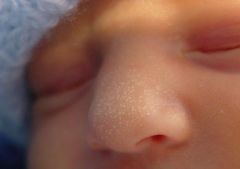
What are these called? What is their definition? What are they called if they are in the mouth?
|
|
|
Cutis Marmorata
|
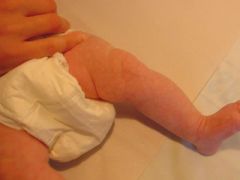
This is a vasomotor response to cold stress. The skin assumes a lacy pattern similar to cobblestones. A persistent form is seen in Trisomy 21 & 18
|
|
|
A newborn has a flat, salmon-colored lesion on the glabella, which becomes darker red when he cries. What is the best course of management? What must it be differentiated from?
|
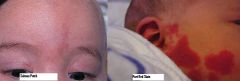
the SALMON PATCH is commonly seen over the eyelids, glabella, & in nuchal area. It is a flat vascular lesion that disappears with time, except for those in the Nuchal area, which may persist.
Port Wine Stains = permanent & unilateral |
|
|
Capillary Hemangioma
|
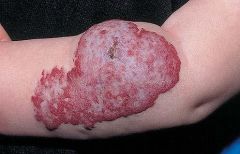
These skin lesions start out as macular lesions in the first few months & quickly grow in the first year of life. They can occur anywhere & are bright red, reminiscent of a strawberry. Rx is usually not necessary b/c they regress spontaneously
|
|
|
Nevus Sebaceus (of Jadossohn)
|

Seen in infancy, these are yellow-orange hairless plaques resembling flat warts located on the scalp. B/c they have a potential to become malignant, they are usually removed by adolescence
|
|
|
Cafe-au-lait spots
|
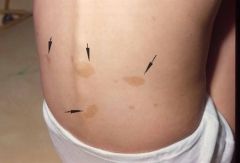
These are tan or light brown flat lesions. They can occur anywhere, vary in size, & are sharply demarcated
|
|
|
Cephalohematoma
Overlying nondepressed skull fracture Jaundice = may require phototherapy |
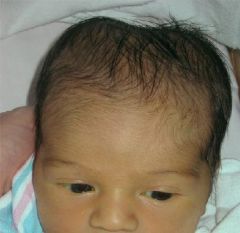
This is a subperiosteal bleed due to birth trauma. Because it is limited to bone, it DOES NOT CROSS the suture line
What can it be associated with? What can these be a common cause of? |
|
|
Caput Seccedaneum
|
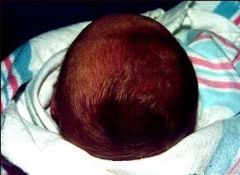
This is a swelling of the scalp, which involves the presenting part (often Occiput-Anterior). It is caused by the pressure exerted on that part during labor & delivery. Involving the SCALP only, the swelling crosses suture lines & resolves quickly over several days
|
|
|
Subcutaneous Fat Necrosis
|
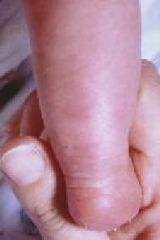
Look for a history of difficult labor & delivery, particularly forceps & vacuum extraction. Rubbery, firm nodules are palpated on the cheeks or buttocks but also the back or extremities. The majority of these lesions resolve spontaneously, although occasionally calcium deposits occur in the lesions
|
|
|
What nerve roots does Erb-Duchenne Palsy affect?
Describe the deficit |
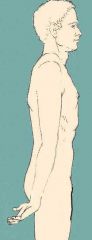
C5-C6
Arm is adducted & pronated & internally rotated |
|
|
What happens if only C4 is affected during traumatic delivery of a newborn?
|
Ipisilateral diaphragmatic paralysis
|
|
|
What nerve roots does Klumpke Paralysis involve? What deficit does it produce?
|
C7-T1
Paralysis of the intrinsic hand muscles ***Ipisilateral Horner Syndrome is seen if the sympathetic fibers of T1 are involved |
|
|
This is usually a peripheral palsy, again secondary to difficult delivery. B/c it is a flaccid paralysis, the AFFECTED SIDE DOES NOT MOVE when the baby cries
|
Facial palsy
|
|
|
Most commonly fractured bone during delivery & is associated with babies who are LGA & Shoulder Dystocia. What does PE reveal? What can be felt over the fracture? Is treatment usually indicated?
|
Clavicular Fracture
Fussy baby with asymmetric Moro reflex Crepitus Rx is usually not indicated |
|
|
What do Subconjunctival Hemorrhage usually result from?
|
Increased pressure during passage thru the birth canal
|
|
|
Coloboma
|
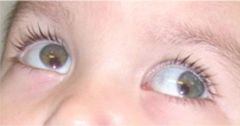
This is a congenital anomaly in the lid, ranging from a small notch to a large cleft. It can also involve the retina or iris
|
|
|
What is Aniridia associated with? What tumor do you always think of?
|
Hemihypertrophy
Wilm's tumor = kidney tumor |
|
|
What are Pre-auricular skin tags, pre-auricular pits, & malformed ears sometimes associated with?
|
hearing loss and/or GU anomaly
|
|
|
This congenital anomaly results from injury to the SCM during delivery, or less commonly from a congenital cervical anomaly. How is it usually treated?
|
Congenital Torticollis
Stretching exercises |
|
|
What is Breast Hypertrophy in the neonate due to?
|
temporary condition secondary to increased circulating hormones
|
|
|
What are Supernumerary Nipples (Polythelia) sometimes associated with?
|
Renal & CV anomalies
|
|
|
This syndrome has amastia, pectoralis muscle aplasia, rib deformities, webbed fingers, & radial nerve aplasia
|
Poland Syndrome
|
|
|
What are the causes of most Abdominal masses in the newborn?
|
Renal = hydronephrosis & Polycystic Kidney Disease
|
|
|
This arises from incomplete closure of the fascia of the umbilical ring.
What is it associated with? |
Umbilical Hernia
Diastasis Recti = separation of the rectus abdominis muscle into right and left halves **usually close spontaneously by 5 years of age |
|
|
What is an Omphalocele?
What is treatment? What is it associated with? |
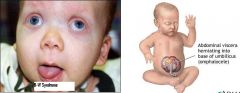
Herniation of peritoneum & abdominal contents into the base of the umbilical cord = abdominal viscera herniate thru the umbilical & supraumbilical portions of the abdominal wall into a sac covered by peritoneum & amniotic membrane
Immediate Surgical repair GI & congenital heart defects & Beckwith-Wiedemann's Syndrome (exophthalmos, macroglossia, gigantism, hyperinsulinemia, & hypoglycemia) |
|
|
Define Gastroschisis
|
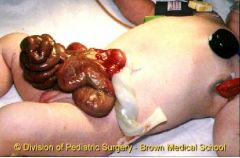
Contains no sac; the intestine is herniated thru the abdominal wall lateral to the umbilicus
|
|
|
What is the cause of Omphalocele?
|
results from arrested folding of the embryonic disc
|
|
|
Epispadia
|
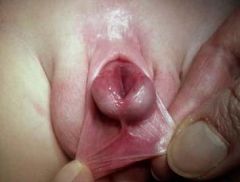
Condition in which the urethral opening is located on the dorsum of the penis shaft
|
|
|
Hypospadia
|
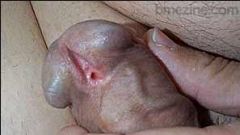
Condition in which the urethral opening is located on the ventral side of the penis shaft
|
|
|
What is sometimes associated with Hypospadia?
|
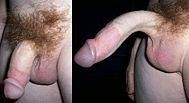
Chordee
|
|
|
What should be avoided in Hypospadia?
|
Circumcision b/c the foreskin is needed for repair
|
|
|
What must Cryptorchid testes be differentiated from?
|
Retractile Testes = result from an active cremasteric reflex & do not require treatment
-can be manipulated into the scrotum with gentle pressure...cryptorchid testes cannot be manipulated down |
|
|
1. This is a collection of fluid in the scrotum, specifically the tunica vaginalis.
2. What happens to most of them? 3. Reduction of these by compression should raise suspicion of what? 4. How is 1 diagnosed? |
1. Hydrocele
2. Involute by 1 year of age 3. Hernia 4. Transillumination |
|
|
A 1-month-old fair-skinned baby presents with projective vomiting of 4 days' duration. Physical exam reveals a baby with eczema & a musty odor. Which screening test would most likely be abnormal?
What does this disease result from a defect in? |
PKU
Hydroxylation of Phenylalanine to Tyrosine |
|
|
What are the symptoms of an affected PKU infant?
|
1. Mental retardation (most common)
2. Projectile vomiting which can be confused with Pyloric Stenosis 3. Fair-hair, fair-skinned, blue eyes 4. Eczematous rash & musty odor |
|
|
What are the blood levels of Phenylalanine & Tyrosine in an affected PKU infant?
|
Phenylalanine = high
Tyrosine = normal |
|
|
What do pregnant women with a high level of phenylalanine have a higher rate of?
|
Spontaneous Abortions
|
|
|
Galactosemia results from a deficiency of __1__. __2__ then accumulates, injuring the __3__, __4__, __5__
|
1. Galactose-1-phosphate uridyl transferase
2. Galactose-1-phosphate 3. kidney 4. liver 5. brain |
|
|
What is the presentation of Galactosemia?
|
1. jaundice
2. vomiting 3. hypoglycemia 4. seizures 5. cataracts 6. hepatosplenomegaly 7. poor weight gain **often times the initial presentation is E. coli sepsis |
|
|
You are called to see a 9.5 lb infant who is jittery. PE reveals a large plethoric (red-faced) infant who is tremulous. A murmur is heard. Blood sugar is low. What is the most likely cause?
|
Infant of Diabetic Mother
|
|
|
What is the presentation of Infants of Diabetic Mothers?
|
1. Ruddy, plethoric complexion
2. LGA -> birth trauma 3. Hypoglycemia -> jitters, tremors, & excitability 4. RDS -> Insulin can block surfactant production 5. Hypertrophic Cardiomyopathy, Hyperbilirubinemia, & Polycythemia 6. Congenital anomalies -> cardiac defects, lumbrosacral agenesis, small left colon |
|
|
Define SGA
|
babies whose birth weight falls below the 3rd percentile for their calculated gestational age
|
|
|
Define the 2 types of SGA
Which one is usually later onset? |
Symmetric = all growth variables (weight, length, HC) are equally affected
Asymmetric = relative sparing of the head Later onset -> Asymmetric |
|
|
How do you differentiate SGA babies from Preterm babies?
|
Preterm babies are proportionately small & their weights fall in the normal range for the GA
-use Ballard scoring system to determine GA |
|
|
What are 5 complications of SGA babies?
|
1. Fetal death
2. Asphyxia = deficiency of oxygen and excess of carbon dioxide in the blood and body tissues 3. Cold stress 4. Hypoglycemia 5. Polycythemia/Hyperviscosity from hypoxia |
|
|
Describe the risk factors for RDS
|
Immaturity of Surfactant due to Prematurity
-results in Atelectasis & V/Q mismatch |
|
|
What is the presentation of RDS?
|
manifest soon after birth
-tachypnea -nasal flaring -retractions -cyanosis -grunting -Apnea may occur as the infant tires Pt's condition peaks at about the 3rd day |
|
|
What signals improvement of RDS?
|
Spontaneous diuresis
|
|
|
What is the diagnostic test for RDS?
|
**Clinical presentation usually makes the diagnosis
CXR usually demonstrates a reticular-granular pattern "Ground-glass" with air bronchograms -Air bronchogram = pulmonary infiltration or edema in the tissues immediately adjacent to the bronchi |
|
|
A term neonate born by C-section has tachypnea, mild retractions, & grunting. O2 requirement is minimal. CXR shows fluid in the fissure & prominent vascular markings
|
Transient Tachypnea of the newborn
|
|
|
What is Persistent Fetal Circulation (Primary Pulmonary HTN of the Newborn)?
What is the treatment? |
Occurs when severe hypoxemia causes pulmonary vasoconstriction -> R-to-L shunting thru PDA or Patent Foramen Ovale
Treament -Hyperventilation to avoid acidosis -maintaining optimal oxygenation to decrease pulmonary vasoconstriction -Nitric Oxide to act as pulmonary vasodilators -Extracorporeal Membrane Oxygenation |
|
|
Describe the characteristics of Physiologic Jaundice
|
-NOT seen until AFTER the first day of life
-rarely exceeds 12.9-15 mg/dL -UNconjugated -resolves by 1 wk of age |
|
|
What are the risk factors for Neonatal Sepsis?
What are the common organisms? |
-Infection during pregnancy
-prematurity -prolonged rupture of membranes GBS, E.coli, Listeria HSV, Enteroviruses |
|
|
How is Toxoplasmosis transmitted?
|
ingesting undercooked or raw infected meat or from handling infected cat feces
|
|
|
What are the manifestations of Toxoplasmosis on the neonate? (6)
|
-Intracranial calcifications
-IUGR -Microcephaly -Seizures -Blindness -Hepatosplenomegaly |
|
|
What is the treatment of pregnant women with Toxoplasmosis infection?
|
Spiramycin during 1st trimester
Pyrimethamine & Sulfonamide afterward |
|
|
What is the treatment for the neonate with Toxoplasmosis infection?
|
Pyrimethamine, Sulfonamide, & Leucovorin (folinic acid)
Steroids for Chorioretinitis |
|
|
What are the signs & symptoms of CMV infection?
|
1. IUGR (most common)
2. Prematurity 3. Petechiae 4. Hepatosplenomegaly 5. Jaundice (Direct) 6. Hearing Loss 7. Chorioretinitis 8. Microcephaly 9. Periventrincular Calcifications (vs. Intracranial for Toxo) |
|
|
Occurs in 80% of babies if the mother is infected in the 1st trimester.
Manifestations -IUGR -cataracts -mental retardation -microcephaly -Heart defects = PDA, Pulmonary Stenosis -Hepatosplenomegaly -Deafness -BLUEBERRY Muffin Lesions |
Congenital Rubella
|
|
|
Under what time-frame should a neonate be treated when the mother develops Varicella?
|
If the mother develops Varicella 5 days before to 2 days after delivers
|
|
|
What are some associated conditions with TEF?
|
Congenital Heart Diseases
-PDA -Vascular rings -Coarctation of the aorta VACTERL -Vertebral abnormalities -Anal atresia -Cardiovascular tree -Trachea -Esophagus -Renal system -Limb buds |
|
|
Pt presents with bilious vomiting with every feed. "Double bubble" is seen on abdominal films
|
Duodenal Atresia
|
|
|
What is duodenal atresia associated with?
|
Downs Syndrome
|
|
|
This should be suspected in any newborn who fails to pass meconium in the first 24-48 h of life
|
Hirschsprung disease
|
|
|
MC medical & surgical GI emergency in the newborn. 90% of cases occur in Preterm infants, presenting in the first 2 wks of life
What are symptoms usually related to? What are the symptoms? |
Necrotizing Enterocolitis
Introduction of feeds Bloody stools, apnea, lethargy, & abdonimal distension once perforation has occurred |
|
|
What is pathognomonic of Necrotizing Enterocolitis on plain Abdominal film?
|
Pneumatosis Intestinalis = gas in the bowel wall
|
|
|
In the newborn ICU, an infant is noted to have sucking movements, tongue thrusting, & brief apneic spells. The blooc counts & chemistries are normal
|
Neonatal seizure
|
|
|
What are 2 possible metabolic causes of seizures?
|
Hypoglycemia & Hypocalcemia
|
|
|
What is the MCC of neonatal seizures?
|
Hypoxic-ischemic encephalopathy
|
|

-
|

-
|
|

-
|

-
|

