![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
20 Cards in this Set
- Front
- Back
|
1. Differentiate between:
a. Endocrine organs b. Exocrine organs 2. What are the 2 types of endocrine organs? |
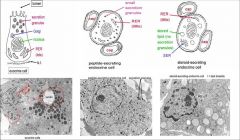
1. a
endocrine glands - lose contact with surface epithelium, non-polarized cells with non-polarized secretions (into surrounding blood capillaries) Note: the thyroid gland is one exception to this rule 1.b.exocrine glands - maintain continuity with surface epithelium, have polarized cells with polarized secretions 2. a. peptide-secreting endocrine cell b. steroid-secreting endocrine cell NOTES: Endocrine organs: -synthesis and secretion of chemical messengers – hormones -dissemination by bloodstream or specialized microcirculation -secretory cells of epithelial origin -support tissue, rich in blood and lymphatic capillaries -ductless glands -secretory cells with prominent nuclei, abundant mitochondria, ER, Golgi bodies, secretory vesicles -discrete organs or in association with exocrine gland (pancreas) -Endocrine glands are ductless glands. Secrete into the bloodstream Have secretory cells of epithelial origin -Anatomizing in between capillaries, the secretory cells in endocrine that contain and store hormone. The thyroid glands line follicles and the hormone is in the intercellular space Peptide endocrine: Important are the capillaries very near by. They have fenestrated capillaries Steroid endocrine: No secretion granules Lipid droplets are close by. Few mitochondria that has enzymes for steroid production Exocrine gland: -Hormone in lumen of duct |
|
|
1. What is the location of the thyroid gland?
2. Describe the thyroid follicular cells by mentioning the role of the colloid, and name the type of epithelium in these cells. 3. What is the function of the thyroid hormone? 4. What is the difference in appearance of the thyroid in comparison to the normal state when: a. there is excessive stimulation b. There is insufficient activity |
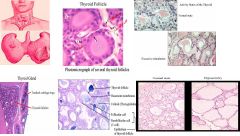
1. The thyroid gland consists of two lobules, encircling the trachea and located below the thyroid cartilages of the larynx
and it is butterfly shaped with a connective tissue called the capsule. Therefore, the thyroid follicle is in close proximity to the trachea. 2. The follicular cells basically form a wall and within the wall, you have the colloid that store the thyroid hormone. There are other secretory cells that store the hormone in the cytoplasm. Colloid is surrounded by follicular cells. The epithelium is simple cuboidal cells. 3. Function of thyroid hormone: key role in development during growth and functional activity of different organs and tissues. lack of TH in children can lead to poor development and growth and mental retardation…dwarfism in adults it regulates metabolic activity, the rate that the body transfers oxygen for nutrients. 4. a. In the normal state : 1. Size of the follicles is very irregular. Some are really small. Amount of colloid in lumen is reduced 2. Will have sharp edges., indicates that there colloid is being used for thyroid hormone 3. Epithelial cells are relatively tall in size, so cuboidal or columnar. When the thyroid is very active, there is less colloid and there is no colloid left in active use. Also, the epithelium is not always cuboidal because it depends on the thyroid secretion. b. In reduced activity or hypoactivity, the core is pressing against the follicular cells, making them look almost squamous. The cell is actually in a normal active state, but it is not releasing the hormone. Small follicles lined by tall epithelial cells in the normal state. In the hypoactive state, follicles are too filled with colloid, so you have squamous because the colloid is pressing on the follicles when there is no activity. More hormone is now in the colloid. |
|
|
1. Describe the regulation of TSH secretion?
2. Describe Synthesis & release of thyroid hormone by follicular cells? |
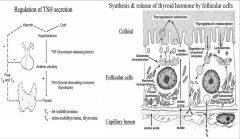
1. In a cold environment, we are less active. Results in more TH in the blood.
NOTES Size of follicle and lining cells vary, tall cuboidal or columnar, flattened if inactive and too much colloid. Thyroid has T3 and T4 Iodine is thyroxin. The regulation of TSH secretion is by a negative feedback circuit so amount of hormone in blood has influence on production So if low amounts of T3 or T4 in cold conditions, less active and metabolic rate is reduced, so the hypothalamus releases and acts on anterior pituitary, releases thyroptropin so thyroid releases more hormone and higher thyroid in blood, so you get negative feedback to stop too much. 2. Follicular cells are surrounded by capillaries, the follicular cells concentrate iodide thought the pump and iodide from blood go into the follicular cells and they are oxidized to iodine, transported through membrane and brought into the colloid and the follicular cells also make thyroglobulin, that goes through protein synthesis and through exocytosis goes into the lumen, combines with iodine, thyrogobulin iodination, this is the inactive form of the thyroid hormone if thyroid is stimulated the complex is reabsorbed and through endocytosis, and the vacuoles are formed and they fuse with lysosomal vacuoles with enzymes and then you release T3 and T4 and released through the plasma membrane and picked up by the blood stream. This is thyroid hormone synthesis. NOTES: Thyroid has colloid in the center surrounded by follicular cells, and you see the peptide secreting cells, the c cells, and have no access to the lumen, you see golgi, one of the thyrogobulin vacuoles in the cytoplasm and the lysozyme fuses with them to make T3 and T4, you see a basement membrane and then fenestrated capillaries. Microvilli are involved in exocytosis and endocytosis of the vacuoles. |
|
|
What are the 2 thyroid gland disorders?
|
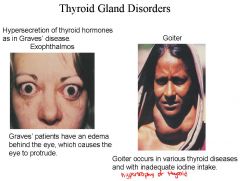
More core being accumulated in the lumen, but it’s not being taken out because there is not enough iodine. This leads to a hypertrophy of the thyroidgoiter
Goiter is hypertrophy of the organ, the follicular cells make thyrogobulin, that is pumped into lumen but its not taken out, and the colloid is accumulated cause not taken out Graves disease, because of excessive secretion of the hormone and there is an abnormal antibody that is produced that mimic the fxn of the thyroid stimulating hormone, due to inflammatory of the extrinsic eye muscles so protruding eyes |
|
|
1. Describe the appearance of the parafollicular cell (C cell)?
2. Describe the location of the parathyroid glands in comparison to the thyroid glands? |
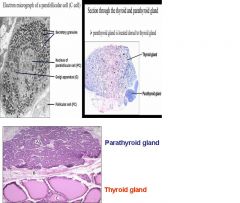
1. The parafollicular cell (C cell) looks like a secretory cell. It has lots of golgi, features of a protein hormone secreting cell. Parafollicular cells have no access to the lumen of the follicular cell. They produce calcitonin. They have no tubule lumen. Not make thyroid hormone. They are adjacent to the follicles and some call them C cells because they contain calcitonin, and they are “clear” in histological stain.
2. parathyroid gland is located dorsal to thyroid gland and it is more densely organized. |
|
|
Compare the functions of these hormones:
1. Calcitonin in the parafollicular cells of the thyroid gland 2. PARATHYROID HORMONE (PTH) secretion from the parathyroid gland |
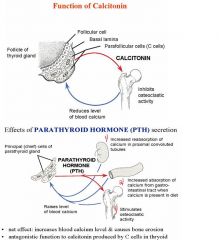
1. Calcitonin reduces level
of blood calcium. 2. Parathyroid hormone raises blood calcium levels by 3 mechanisms illustrated in the above diagram. |
|
|
What are the 2 cell types in the parathyroid gland?
|
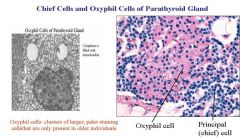
1. Principal (chief) cell
2. Oxyphil cell - abundant mitochondria NOTES: Don’t know the function of the oxyphil cells but principal (chief) cells produce parathyroid hormone and it is the most abundant. - Oxyphil cells have Very high packing density of mitochondria. Results in light staining cytoplasm. These cells are derived from chief cells and they also have a dark staining nucleus, |
|
|
1. What are the 2 divisions of the adrenal glands?
|
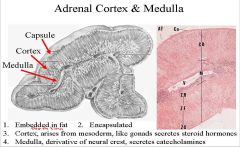
1. Adrenal cortex
2. Adrenal medulla NOTES: The adrenal glands are really two glands that work together with each other. They are the cortex and medulla. They are next to the kidney in upper pole of the kidney Dense irregular connective tissue Embed in fat These are 2 glands that work together Adrenal cortex and adrenal medulla Cortex is like the gonads and secretes steroid hormones related to cholesterol Medulla is like sympathetic nervous and from neural crest, secretes catecholamine, like epinephrine and norepinephrine. |
|
|
1. What are the 3 subdivisions of the adrenal cortex?
2. What are the 3 sources of vascular supply to the adrenal cortex? |
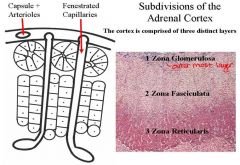
1. Histological zonation – Capsule (dense C.T.) surrounding three zones:
a. Zona glomerulosa b. Zona fasciculata - spongiocytes c. Zona reticularis 2. Vascular supply a. Capsular arterioles b. Fenestrated capillaries c. Arterioles penetrating cortex to supply medulla directly NOTES Cortex has 3 layers, the outer most…gas collecting of cells that look like glomerulus Parallel to fenestrated capillaries Reticular is irregular arrangement. |
|
|
What are the unique features of the 3 layers of the adrenal cortex?
|
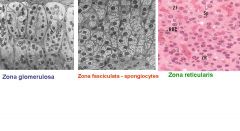
1. The Zona Glomerulosa:
These are steroid secreting cells. Have lipid droplets, RER, lipofuscin. Connective tissue capsule. This is an endocrine organ, no ducts Steroid cells, lipid droplets, lipofuscion in lipid metabolism breakdown. 2. The Zona Fasciculata: Distinct cause if you stain for lipids, you see it here, it looks like the cells are spongy. The steroid cells have lots of lipid vacuoles that gives them the spongy appearance. It has lipid-filled cells arranged in long rows between fenestrated capillaries. It has mostly sER since it is steroid secreting and not that much rER. The Spongiocytes from the zona fasciculata are filled with lipid vacuoles. Here are its 3 characteristics: Three characteristics: a. Lots of SER containing membrane associated proteins involved in the production of steroids. b. Mitochondria have tubular cristae, not the shelf-like cristae. C. Lipid droplets containing cholesteral. -The Fenestrated Capillaries of Zona Fasciculata are a meshwork of protein filaments forms the permeable diaphragm of a fenestra so they let large molecules go through. 3. The Zona Reticularis: It is Next to the medulla, and its structure is more irregular. Border Between the Zona Fasciculata and Zona Reticularis is indistinct. |
|
|
1. What are the 2 cell types in the adrenal medulla?
2. a. What are the 3 hormones secreted by the 3 different layers of the adrenal cortex? 2.b. What are the 2 hormones secreted by the adrenal medulla? |
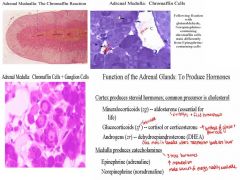
1. a. Chromaffin Cells: Chromaffin cells, undergo “chromaffin reaction” after perfusion with dichromate; secrete catecholamines: epinephrine (adrenalin), norepinephrine (noradrenalin). Because these neurotransmitters can be made to fluoresce, these cells show a formaldehyde-induced fluorescence.
After glutaraldehyde fixation, it may be possible to distinguish between these 2 type of chromaffin cells (norepinephrine stains darker). Enkephalins are peptides secreted from chromaffin cells simultaneously with norepinephrine and they have an opioid-like activity. b. Ganglion cells: The ganglion cells are like neurons, it is a clear appearance and they are regulating the function of blood vessels 2. The hormones are illustrated above: Each layer of the secrete a diff hormone they are all steroid hormone Aldostereone regulation of fluids. Glucocorticoids increases the blood glucose level. DHEA has a weak androgen activity. Not much in male but higher in female, for lactomerization. Less stimulation of adrenal have too muscle. Stress hormones are secreted in medulla. NOTES: Have dense core vesicles, but there are no axons leaving the tissue. Instead they secrete their neurotransmitters directly into the blood. Adrenal medulla does not secrete its hormones continuously the hormones are stored in membrane bound vesicles, that gives the cells the granular appearance There are enkephalins, opiods in the medulla that are secreted as well Ganglion cells are big! They are very rare, there are enlarged blood vessels Combination of darkly basophilic chromaffin cells and the ganglion cells The ganglion cells are like neurons, it is a clear appearance and they are regulating the function of blood vessels No axons leave the tissue, they secrete their neurotransmitter into the blood |
|
|
1. Differentiate between ISLETS of LANGERHANS and ACINAR cells?
2. What 4 hormones are present on the 4 cells of Islet of Langerhans? |
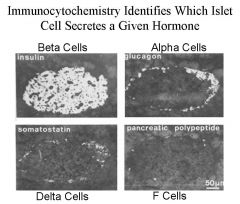
1. Highly vascularized balls of endocrine cells called
ISLETS of LANGERHANS and it is surrounded by more abundant ACINAR cells, which are the exocrine portion of the pancreas. 2. See diagram. Heavy vascularization in the endocrine glands. Each cell type can be distinguished by a stain. Each cell type has its own secretion of a polypeptide hormone. -Delta cells may inhibit glucagon secretion There are 4 cell types in the islet Most of the cells are the beta cells that secrete insulin Somatostain effects on GI function and inhbit insilin and glucagon. -Similar to peptide-secreting endocrine cells A and B cells are different in the structure and form of secretion granules– more irregular in deiter/delta? Cells and more round in the alpha cells These are peptide secreting endocrine cells Secretion granules A and b is the form of the secretion granules Fenestrated capillaries that lets the molecules get into the lumen. -Function – regulate blood glucose level by insulin & glucagons - somatostatin Control – negative feedback by blood glucose level - autonomic nerves |
|
|
1. Compare the roles of glucagon and insulin?
|
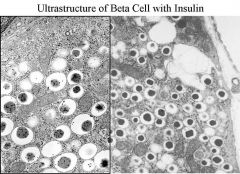
1a.Glucagon INCREASES blood glucose levels by stimulating the release of glucose from the liver
1b. Insulin DECREASES blood glucose levels by stimulating the uptake of glucose from the bloodstream into tissues like muscle and fat PICTURE ABOVE: Many secretion granules with insulin (very densely packed) On left shows that in the beta cells are little dots of secretion granules which stain. Electron dense granules bind to insulin in granules and we visualize that Lots of secretion granules Insuloin was labelerd, they stain positive and the granules bind to insulin |
|
|
1. Illustrate how islet cells Regulate Hormone Secretion in Response to Changes in Blood Glucose?
2. Describe diabetes and differentiate between the 2 types? |
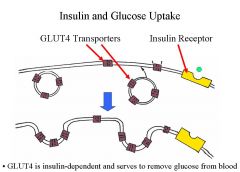
1. Islet cells possess unusual, high capacity glucose transporter proteins (GLUT2 transporters)
GLUT2 is insulin-independent and transports glucose to insular cells and hepatocytes. -After glucose is taken up it triggers the release and production of insulin into the blood stream and it binds to receptors (Ex: on muscle and fat) and the intracellular receptor part triggers changes in the cell– insertion of GLUT 4 into cell membrane of cells GLUT 4 pick up glucose from blood and take it up into muscle and fat GLUT 4 is insulin dependent and removes glucose from the blood It is a feedback mechanism so if you have high glucose in the blood you have uptake into beta cells NOTES: Glucose transporter 2 High level glucose in the blood stimulates insulin release and that stimulates glucose uptake into muscle and fat High glucose is taken up by beta cells with help of GLUT2 and it is insulin independent, transporting glucose into endocrine pancreas Beta cells and hepatocytes is where the glut 2 transports the glucose into! Skeletal muscle In the cell membrasne Insulin binds to the receptor and there ae many events See glucose being taken up After insulin binds to the muscle cells, it triggers the insertion of more glut transports to get glucose 2. Diabetes Mellitus -Type I—juvenile onset—due to an autoimmune attack upon islets. -Type II—adult onset—involves resistance of tissues to effects of insulin ~7 million US citizens have this form. Type II diabetes is the leading cause of blindness, renal failure, and amputations. |
|
|
1. Describe the development of the pituitary gland (hypophysis)?
2. What are the major divisions of the pituitary and the their contents? |
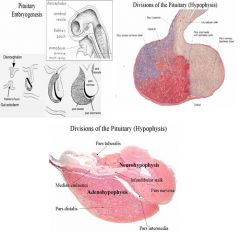
2. Development
Union of buccal ectoderm (Rathke’s pouch) with neuroectodermal infundibular process. Remnants of this process: pharyngeal hypophysis, other remnants that can form tumor – craniopharyngioma 2. Parts of Pituitary Gland a. Adenohypophysis, anterior pituitary i. Pars distalis ii. Pars tuberalis iii. Pars intermedia b. Neurohypophysis, posterior pituitary i. Infundibulum - Median eminence - Infundibular stalk ii. Pars nervosa NOTES; Pituitary is in the hypophyseal fossa and surrounded by the sella turcica Anterior is towards front of head It is hung off the bottom of the brain btw the sphenoid bone in a cup like Surrounded by a dense conec tissue capsule Extends down from the brain and it has a gland component and a big neuro component Here is a parasaggital section It has diff parts to it Portion that extends down from the brain Posterior lobe, true glandular is the pars distalis It is an extension of the brain as well as from ectoderm extending towards the brain (Rathke’s pouch) Pars tuberalis surrounds the infundibulum The pouch is gut ectoderm The pouch goes up to the brain and disconnects itself and moves further up The intermediate The open space Pars nervosa is all neuro tissue extending from the brain so neurohypophysis |
|
|
A. What are the 2 cell types of the anterior pituitary?
|
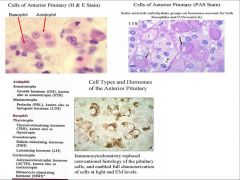
A.
(1) Chromophils (1.1) Acidophils – produce growth hormones, prolactin - Somatotrophs - Mammotrophs (1.2) Basophils – are PAS+ and produce glycosylated hormones all having identical α-subunits and different β-subunits - Thyrotrophs - Corticotrophs - Gonadotrophs (2) Chromophobes NOTES; -Pars distalis and pars intermedia line rathke's pouch. -Pars distalis has 2 parts, a. CHROMOPHILS, subdivided into basophils and acidophils b. CHROMOPHOBES do not stain at all, they have no affinity for the dyes or they have no granules in them PAS STAIN PICTURE (119): Different stain Shows basic cell types B = intensely staining and contain glycosylated hormones (FSH, etc) A = peptide hormones contained but are not glycosylated so they don’t stain as well here C = basal membrane/ lamina surrounding capillaries; they contain a lot of carbs and so stain how they do IN SILVER SATIN: of Pars Distalis = Fenestrated capillaries surround the cell clusters and enable easy access of secretory products into the blood supply. SINUSOIDAL CAPILLARIES -Cells are in clusters and are surrounded by fibers and sinusoidal capillaries Cannot see individual cell types and cannot see secretions There is a silver stain, reticular fibers You see the cells Many cell clusters Pas stains glycogen or polysaccharides, do these cells have glycosilated hormones like FSH, TSH Basal membrane with the lamina stains too |
|
|
Compare:
-Corticotrophs -Thytotrophs -Gonadotrophs -Somatotrophs -Lactotrophs |
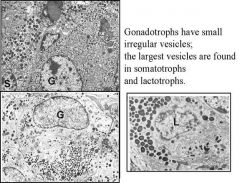
The corticotroph has medium
sized secretory vesicles, whereas the thyrotroph’s vesicles are very small. Gonadotrophs (next slide) have small irregular vesicles. The largest vesicles are found in somatotrophs and lactotrophs. Gonadotrophs have small irregular vesicles; the largest vesicles are found in somatotrophs and lactotrophs. |
|
|
What does pars intermedia secrete and why is it important?
|
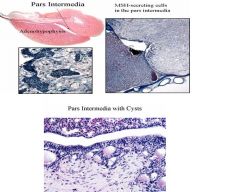
1. MSH-secreting cells
in the pars intermedia NOTES: Cell types found in the pars distalis There is a different cell type in the pars intermedia and is only one cell type– the one that makes MSH Bottom left are finger-like extensions of these cells It is rudimentary structure and is believed to not be there MSH in pars intermedia, they are enriched into the tissue and they are basophilic CYST: They contain cysts Don’t do a lot and not a problem– advantageuos in IDing the pars intermedia But if cysts go crazy and grow indefinitely so entire hypothalamus or pituitary is ablated and you don’t have enough secretions, so cranial pron They have some colloid in them They lets us identify |
|
|
1. What are the 2 main structures of the Neurohypophysis and their contents?
2. Describe the path of the hypothalamic neurons on their way to the pituitary? |
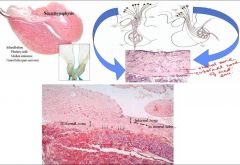
1.
a. Infundibulum i. Median eminence ii. Infundibular stalk b. Pars nervosa i. Nervous tissue (1) Unmyelinated axons from hypothalamus (2) Herring bodies (3) Pituicytes (4) Capillaries (fenestrated) 2. Cell bodies of the hypothalamic neurons are seen and they send axons Use median eminence as a roadway to get to the pituitary Internal and external zones of median eminence are functionally different Axons go into the median eminance or they continue to go down to the neural lobe Diff neurons secrete diff substances depending on where they go Some neurons in the external zone, internal zone to go to the neural lobe. -Some neurons terminate in external zone and release substances going to anterior pituitary = how it is regulated Cells terminating in median eminence do so in external zone Those neurons continuing down to the neural lobe (neurohypophysis), those with vasopressin and oxytocin, release the chemicals which then go to the area they need to go to . Capillary networks within the median eminence and thy drain down substances to the pars distalis, the anterior pituitary and it is regulated this way so external zone Other ones go to the neural lobe, this have ….the vasopressin gets picked up by the blood and then gets to its target organ NOTES: Fun part– neurohypophysis: important in body function Extends down from the brain so it is NEURAL TISSUE It is like other parts of the brain except it is mainly axons and not entire neurons coming down from the brain Cell bodies will be up in the hypothalamus Median eminence is seen below third ventricle VERY IMPORTANT The cell bodies are in the hypothalamus and stay high in the brain They send their axons down into 2 regions |
|
|
1. Describe the function of the 2 hormones stored in the neurohypophysis?
2. What are pituicytes? 3. What are Herring bodies? |
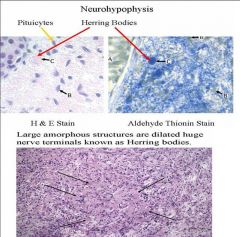
1.
a. Vasopressin (Anti-diuretic hormone, ADH): stimulates the kidney to produce a concentrated urine LACK of Vasopressin causes DIABETES INSIPIDUS b. Oxytocin: stimulates milk release from the mammary gland. 2. Neural lobe contains: - nerve terminals from Vasopressin and Oxytocin neurons - glia called pituicytes. 3. Herring bodies are large nerve terminals which store hormones (vassopressin (a lot)and oxytocin) if neurons stopped making vasopressin we would be okay for about a week. -Vasopressin is stored in Herring bodies and when needed is released -Oxytocin is found in a separate set of terminals in the posterior lobe. NOTES: Neural lobe of the pituitary– looks like peripheral nerves jumbled up Large amorphous structures are herring bodies They are large nerve terminals which store hormones (vassopressin (a lot)and oxytocin) if neurons stopped making vasopressin we would be okay for about a week Part coming from the brain and looks like brain tissue Herrinmg have so much vasopressin in tem stored -Neural lobe is a large container of nerve terminals On left is a drawing Electromicrograph is on the right If you don’t need a lot of vasopression pituicytes cover nerve endings of vasopressin neurons. When you need them then they retract Vasopressin is always continuously released Neural lobe is a filled up with synaptic vesicles at the nerve terminal Fenestra are here and you see the large core vesicles in the termial Pituicytes cover the vasopressin containing neeron So cover their terminals until there is a finctional emergency, then they retract so that vasopressin can ve released due to salt levels |

