![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
117 Cards in this Set
- Front
- Back
|
List 2 differences between the Parotid gland and the exocrine Pancreas
|
1. The Exocrine pancreas contains far fewer ducts
2. Pancreas has centroacinar cells while the Pancraes does not |
|
|
What is the function of the Centroacinar cells in the Pancreas and where are they located.
|
They are located adjacent to the acinar cells ( they come before the striated and intercalated duct).
Their function is to suck the secretions out of the cells upon stimulation and feed into the duct network |
|
|
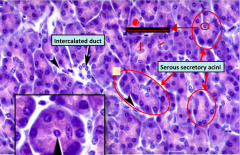
Histological slide of the exocrine pancreas. Features to note:
- Notice like all serous acini, the bottom of the cells is darker than top. Thats because, bottom contains active rER (basophillic) while the top contains proteinaceous vesicles (eosinophilic) -Note the centroacinar cells -Also note the LACK of ducts as compared to the salivary gland slide |
|
|
|
Another zoom up histological slide of the Exocrine acini.
Note that the centroacinar cells are much lighter. And also the darker shade bottom of acini cell and lighter top |
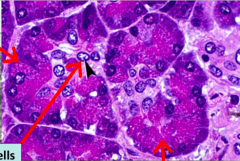
Know what the three arrows are pointing to
|
|
|
Name the 4 main structures the urinary system consist of?
* Hint think of acronym |
Acronym: KUBU
Kidney, Ureter, Bladder, Urethra |
|
|
Describe filtrate flow after it has entered the minor calyce at the bottom of the medulla
|
Renal papilla --> Minor calyx --> Major calyx --> Ureter
|
|
|
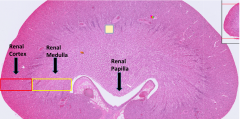
Histological slide of a cat kidney (humans have far more lobules).
Can tell its kidney due to the cortex/medulla difference and the renal papilla shaped like female repro tract |
|
|
|
Name the two structures that the uriniferous tubule consist of
|
Nephron(s) + Collecting duct
**remember that one collecting duct is attached to several nephron |
|
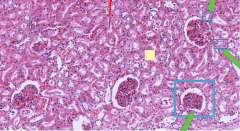
This is a section of a Kidney tissue. List what the three arrows are pointing to
|
Bottom-most arrow is pointing to a renal corpsucle (rememer not just glomerulus, cuz that would be excluding the BOWMANS space)
The middle arrow is pointing to the Proximal convoluted tubule (hazy lumen) The top most is labelling the DISTAL convoluted tubule |
|
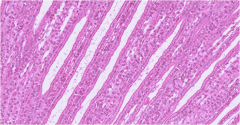
What is this a section of?
|
Renal medulla
|
|
|
What kind of epithelium is found at the Renal Papilla?
Which other parts of the Urinary system is this epithelium also found? Where is the one place it isnt found? |
The epithelium at the Renal Papilla is the transitional epithelium
It is also found in the ureter, bladder and urethra One place it isnt found is the kidney |
|
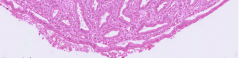
What is this a section of?
What is the name of the blank space underneath? Where will the fluid that drains into the blank space flow next? |
1. Section of a renal papilla
2. Blank space underneath is the Minor Calyx 3. The fluid (urine) will flow to the Major Calyx |
|
|
What does the vascular pole consist of?
What does the urinary pole consist of? |
1. Vascular Pole: Afferent and efferent arterioles, found at the front of the glomerulus (fenestrated capillary network)
2. Urinary pole: Proximal Convoluted tubule, because this is where the eventual urine is formign |
|
|
What is the function of mesangial cells in the Renal corpuscle
|
Mesangial cells have contractile ability and also phagocytose
|
|
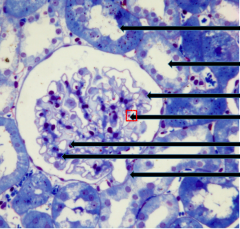
List what the top 2 arrows and the most bottom arrow are pointing to
|
1. Top arrow: Proximal convoluted tubule, darker cytoplasm with a slightly collapse lumen
2. Second arrow: Distal convoluted tubule,, more circular lumen 3. BOTTOMEST arrow = Vascular pole |
|
|
List the three barriers to filtration for blood coming from afferent arteriole trying to get into bowmans space
|
1. Fenestrated capillary endothelium
2. Double layered basement membrane (of both endothel and epithel) 3. Podocyte (visceral layer of bowmans capsule) |
|
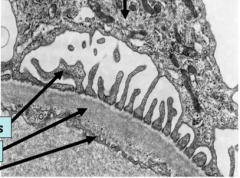
What is this a section of?
What are the three arrows pointing to |
This is the interface between afferent arteriole and the bowmans space.
1. Top most arrow = Foot processes of podocyte 2. Second arrow = Dual layered basement memb 3. Fenestrated endothelium of the afferent |
|
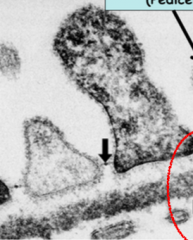
List the 3 layers of the dual basement membrane present at the filtration interface
|
The top white layer (arrow sorta pointing) = Lamina lucida externa
THe middle dark layer = Lamina densa The bottomest white layer in between those cells = Lamina lucida interna The lucidas are named such because its facing the inside of the afferent arteriole |
|
|
What is a medullary ray
Where is it found? |
Medullary ray consist of the uriniferous tubules (Collecting duct + attached nephrons)
It is located in the Renal cortex |
|
|
What is the duct of bellini
Where is it located |
Duct of bellini is the continuation of the collecting duct (which in the cortex called medullary ray)
It drains into the minor calyx and is found in the Renal Papilla |
|
|
Histological slide of a medullary rays
Key features to identify this is, first know that you are in the Renal cortex due to presence of Bowmans Capsule, then look if you can see cell borders in between cells = CD. Combination of border and cortex means MEDULLARY RAY |
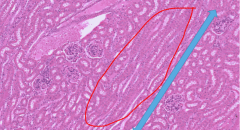
Uriniferous Tubules
Form the Renal Axis (1 CD with attached Nephrons) |
|
|
What are the two features that the secondary processes of podocyte filter by
|
1. Size (large molecules cant get in)
2. Charge (Anions cant get in) |
|
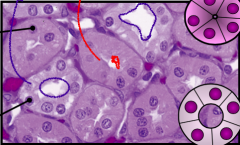
Identify the PCT and the DCT in the image.
**Also note sahil dont confuse these with acini, in acini u can barely ever see a lumen. Lumen = ductal system |
The Pct is the Red arrow, thats because it has a smaller more collapsed lumen with some hazinnss inside. Also its cells are darker
THe DCT is the blue arrow, larger lumen and lighter cellls |
|
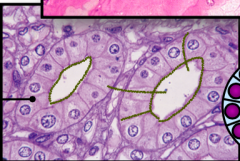
What are these?
|
Collecting Ducts
Because you can see Cell borders |
|
|
Name 3 important hormones for Kidneys Function.
Name where they act Name one important enzyme |
3 Hormones
- Aldosterone = DCT -ADH = Collecting duct water absorption is ADH DEPENDENT - Angiotensin 2 = PCT Enzyme = Renin |
|
|
Name the 2 cell types which are part of the JG apparatus.
Where they are located What is their function |
1. Macula Densa cells = Located in the DCT runs in between the afferent arteriole
2. Juxtaglomerular cells = Part of the afferent arteriole, modified Smooth Muscle cells, RELEASE RENIN The Macula densa cells detect abnormal NaCl The Juxtaglomerular cells detect Blood flow/Pressure |
|
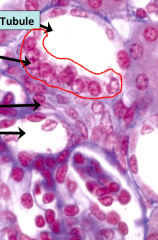
List what all the arrows are pointing to
|
Arrows (from top to bottom)
1. Distal convoluted tubule 2. Macula densa (obvi because they are part of DCT) 3. JG cells 4. Afferent arteriole (obvi because the JG cells are a part of them are directly above) |
|
|
List the pathway of response when Low Bp/Low Osmolarity detected by their respective cells (list which cells detect what first)
|
Low BP detected by JG cells (part of afferent arteriole), Low NaCl detected by Macula densa cells (transporters in DCT). If JG detect release renin directly if MD detect then indirect
Renin converts the constitualy made Angiotensinogen (made in liver) into Angiotensin 1 Angiotensin 1 floats through circulation and is cleaved to Angiostensin 2 by the enzyme ACE in the LUNG Angiotensin 2 now floats back and acts on the Proximal tubule to increase absorption of Na+. This also intiates a neural response of constriction and release of Aldosterone which acts at the DCT to further absorb Na/Cl at the DCT Note that Ang2 also activates ADH release which reabsorbs water from the CD |
|
|
Another histo slide of Cortex. Note the diff in lumens
|
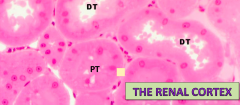
|
|
|
Why does the lumen of the PCT look filled or hazy as compared to the DCT?
|
The PCT contains Brush Border which are needed for absorption and collapse the lumen as compared to the DCT which does not
|
|
|
Histo image of the PCT.
Note the brush border |
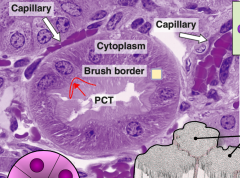
|
|
|
Which organelle is abundant in PCT. Where is majority of it located. Why is it abundant?
|
Mitochondria is abundant
It is abundant since you need to provide ATP to work all the transporters It is abundant in the Base of the cell (opposite to lumen and microvilli) since this is where most of these transporters are located |
|
|
List the 4 things that are identifiable in the Renam Medulla
|
1. Ascending LOH
2. Descrnding LOH 3. Vasa recta (very red blood supply) 4. CD |
|
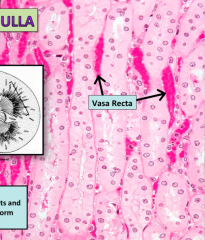
A section of the Renal medulla, see if you can spot the 4 things (including vasa recta) found in medulla
|
find em
|
|
|
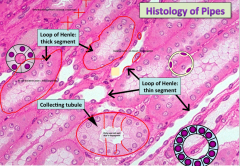
Histological slide of the Renal medulla
* remember that the Ascending LOH looks like DCT while the descending LOH looks like proximal, prolly wont be asked tho. Also there is a thick and thin LOH, should be easy to spot diff here |
|
|
|
Both Ducts of Bellini and CD contain cell borders. But what is the histological diff between them
|
CD cells are SIMPLE CUBOIDAL
The Ducts of Bellini are COLUMNAR |
|
|
Into which structure does the renal papilla (the tip of renal pyramid) drain into.
Where does the ultrafiltrate travel from here? |
1. Renal papilla drains into the Minor Calyx
2. Ultrafiltrate (urine) travels via the ureter |
|
|
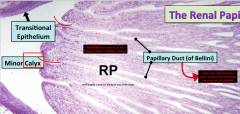
Histo slide of the Renal Papilla
Notice large lumen Ducts of Bellini and a pointy tip feature that give it away |
|
|
|
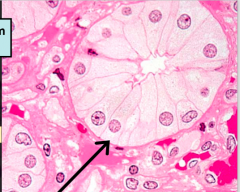
This and the next slide contain histo pics of ducts of bellini.
Remember located in Papilla NOT medulla Have columnar NOT Cuboidal |
|
|
|
What kind of epithelium does the Ureter contain.
What property of this epithelium classifies it as such? |
The Ureter contains TRANSITIONAL EPITHELIUM.
It is classified like this because the height of the epithelium changes depdning on what the pressure is in the lumen |
|
|
How does the Muscle layer of the Ureter differ from that most commonly found in GI Muscularis Externa
|
1. in the GI you had Inner circular OUTER longitudonal
2. In the Ureter you have Inner longitudonal, OUTER circular |
|
|
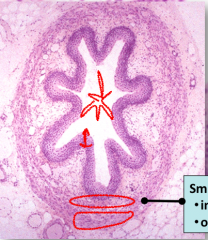
Histological slide of the bladder
**Note it looks very much like the esophagus. Ruffled border, Large Muscular layer and start shaped. Does not look like trachea due to absence of Cartilage |
|
|
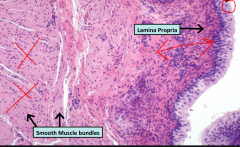
What is this a section of?
List distinguishing features |
This is the Ureter consisting of
* Transitional epithelium = DOME TOP, psuedostartified |
|
|
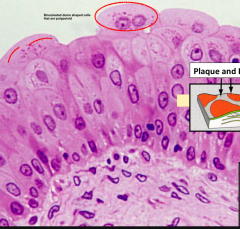
ANother slide of Urinary bladder
Easy to see BINCULEATE HERE the only other place we saw binculeate was the Liver, where it was in plates |
|
|
|
Where is the Adrenal gland located
|
The Adrenal gland is located on top of the Kidney
"Ad"= on top, "renal" = Kidney |
|
|
What is the difference in the product on the Renal Cortex and the Renal Medulla
What are the 3 layers of the Adrenal Cortex and which hormone is produced in each? |
1. Cortex produced CORTICOSTEROID hormones, the Medulla produces Catecholamines (amine = amino acid derivatives)
Z. Glomerulosa (Darker staining) = Mineralocorticoid (Aldosterone) Z. Fasiculata (Largest, Lighter staining part) = Glucocorticoids, Cortisol Z. Reticularis (closest to medulla, dark) = Gonadotrophins, sex hormones |
|
|
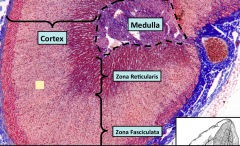
Histological slide of the Adrenal gland.
Always look out for the 3 zone distinction ALSO KNOW THAT THE TOP MOST LAYER above the Zona Glomerulosa is called the CAPSULE of the Adrenal gland |
|
|
|
Describe the blood supply(s) of the Adrenal gland
|
1. There is one blood supply which enters through the capsule located on TOP of the cortex, and goes through every capillary bed (one in each zone) all the way into the venous sinusoids located in the medulla through which it drains
2. A second blood supply comes directly to the medulla and it is called the Medullary Artery This means that the sinusoids in the REnal medulla contain blood that is both low in O2/ but high in corticosteroid hormones, but also blood that is fresh with O2 The reason for the first blood supply will be important later *this is very similiar to that seen in the Liver |
|
|
For each zone list the following
1. Why they are named glomerulosa/fasic etc. 2. What is their primary hormone 3. What are they stimulated by 4. What is their Target organ |
Glomerulosa
- Shape resembles circular glomerulosa's - Primary hormone is aldosterone - Stimulated by both ACTH, and ANG2 - Target organ is kidney where they uptake Sodium Fasiculata - Named because looks like long fasicles - Primary hormone is cortisol -Stimulated by ACTH - Target organ is primarily Liver Reticularis - Looks like convoluted reticular fibers -Primary hormone is Androgens (LH/FSH) - Stimulated by ACTH!! - Target organ is the gonads |
|
|
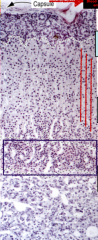
Histological Slide of the Adrenal Gland
- Try to note the 3 diff zones - Make sure you know where the medulla begins, and cortex ends |
|
|
|
Name the 3 cytoplasmic organelles important for the synthesis of Steroid Hormones , and why
|
1. Lipid droplets: Contain cholestrol, which is a precursor to all Steroid hormones
2. Mitochondria: Contains enzymes (StAR, and P450ssc) which are responsible for bringing in cholestrol and converting it 3. Smooth ER: Does the bulk of the modification for the Steroid hormones, contains lots of enyzmes |
|
|
What is the easiest feature to dinstinguish between a mucous acini like sublingual gland in the mouth or the sebaceous gland on skin and the acini found in the Adrenal Cortex
|
Glands in the Adrenal cortex
- Contain no associated Ductal system - Have no lumen themselves *basically, your not going to find large white spaces in lumen anywhere |
|
|
Histology of the Zona Glomerulosa. Notice the following things:
1. Circular shape of cells like a glomerulus 2. Note there is no lumen in any of them (secrete into adjacent capillary so no duct with lumen either) 3. Tons of lipid droplets so you know they are making a steroid hormone |
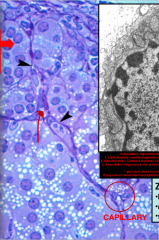
|
|
|
Which 2 organelles do modified steroid hormones keep going back n forth through and why?
|
Precursor hormones like Androstendione and Pregnonlone have to keep shuffling in between SMOOTH ER and the Mitochondria because certain enzyme for modification are contained in one and not the other.
Once final product is made it is released into adjacent capillary |
|
|
Histological slide of the Zona Fasiculata. Notice
- Long plate like cells rather than circular acini looking in glomerulosa - Still have abundance of Lipid droplets |
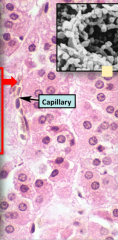
|
|
|
What is the 2 functions of Cortisol?
|
1. Raise glucose levels by causing its secretion from Hepatocytes of the liver
2. Supressing IMMUNE RESPONE |
|
|
What is the name of the cells found in the Adrenal Medulla.
What is their DOMINANT secretion What is their origin |
1. Chromaffin cells
2. Dominant secretion is Epinepherine (80%) secrete Epi 3 .They arose from NEUROECTODERMAL CELLS, they are part of the NERUOENDODERMAL tissues |
|
|
How can you distinguish the Adrenal Medulla from the Adrenal Cortex, given a picture of the whole gland
|
The adrenal gland on its own is not easily identificable
If shown next to cortex, it would be obvious because it is REALLY PALE STAINING, contains NO LIPID DROPLETS Be sure to see where you can spot three zones of the cortex, and the medulla would then be region underneath |
|
|
Chromffin cells are modified ________________
|
Post ganglion sympathetic fibers
|
|
|
What is the functional reason for that one blood supply that comes from the capsule INTO the Adrenal medulla and drains from the Venous sinusoid.
|
1. Glucorticoids produced in the Zona Fasiculata are needed for methylation of Norepi into epi for release
**this makes sense because Fasiculata make cortisol which is released during fear response, and at this time you have symp activity and chromaffin are modified post symp, so activating both in one response is beneficial |
|
|
Near which structures is the Thyroid gland/ Parathyroid gland found
|
It is located ABOVE the trachea and esophagus and under the larynx
|
|
|
What are the two hormones produced in Thyroid gland
|
T3 and T4 (Thyroxine)
Calcitonin |
|
|
What are the two functions of thyroid Hormones
Which cells have receptor for thyroid Hormones |
1. Thyroid hormone raises Basal Metabolic Rate and increases Protein synthesis
2. nearly every cell in the body has a receptor for thyroid hormone |
|
|
What is the name of epithelial cells surrounding the Thyroid follicle and what is their Endocrine function and what is their Exocrine function
|
Follicular epithelial cells
Follicular epithelial cells make thyroglobulin and secrete it into the COLLOID (exocrine function). They are also responsible for, upon activation, secreting T3/T4 back into the adjacent capillary bed (Endocrine function) |
|
|
What is the unique feature of the thyroid gland that distinguishes it from all other endocrine gland? ONly one with this feature
|
Only gland where the endocrine secretions are stored outside the cell (usually stored inside as vesciles).
Hormone is stored in the colloid until needed |
|
|
Which stain is preferentially used to view the colloid and why?
|
PAS staining will make the Colloid look bright red/purple since it contains a lot of glycosylated Thyroglobulin!
|
|
|
The colloid contains little tiny clear spots near the periphery close to the follicular cells. What are these, what is their purpose?
|
Endocytic vesicles containing iodinated Thyroglobulin being packaged with a lysozyme ready for secretion and being uptaken by the surrounding follicular cells
|
|
|
Histological section of the Thyroid follicles.
Be able to notice all the features listed above including clear spots, follicular cells |
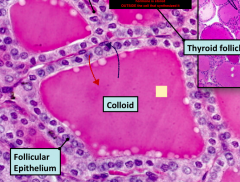
|
|
|
This is a slide of the thyroid follicle stained with PAS
|
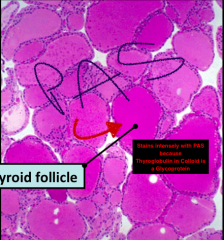
Notice how the colloid is really intensly stained and uniform
Also note that there are capillaries between adjacent follicles (like where the S is ending) |
|
|
List 5 steps of Thyroid hormone synthesis
|
1. Uptake of iodide from BV and concentration of it in the colloid
2. Synthesis and secretion of Thyroglobulin (after going through Golgi for glycosylation) and Thyroid Peroxidase into the colloid 3. Conversion of iodide to iodine by the TPO and subsequent Coupling of iodine residues to tyrosine residues 4. Upon TSH stimulation, uptake of the iodothyrglobulin in endocytic vesicles coupled with lysozymes (seen as clear spots in colloid) 5. Decoupling either T3 or T4 (thyroxine) and release into surrounding capillary bed |
|
|
Super zoomed in pic of the Thyroid Follicle, again notice that the best distinguishing feature is a homogenous colloid with clear spots in periphery.
|
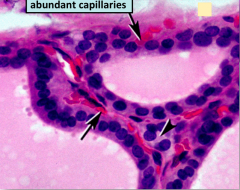
|
|
|
What hormone regulates Thyroid gland?
What process does it cause? What is an associated disease with this hormone system, what is its cause, and what is the diagonstic feature of people with this disease and why? |
1. TSH hormone from the Ant. Pituitary
2. It causes the UPTAKE/Release of T3/T4 3. Graves Disease - Autoimmune where an ACTIVATING ANTIBODY binds to receptor and causes prolonged activation Diagnostic feature: Muscle Wasting |
|
|
What is the function of Calcitonin released by Parfollicular cells and how do they acheive this
|
Calcitonin acts to lower blood calcium levels
Acheives this by binding to osteoclast and reducing their activity |
|
|
What are the two cell types found in the Parathyroid gland and their respective secretions
|
1. Chief cells (Dont confuse with stomach) - Produce Parathyroid hormone secreting
2. Oxyphil cells (we Dont know) |
|
|
Important Histological slide showing the PTH gland.
If the colloid on the side was not shown would be tough to distinguish PTH gland from lymph tissue sine both are really cell dense. The PTH has two key features: EXTREMELY VASCULARIZED and SURROUNDING COLLOID |
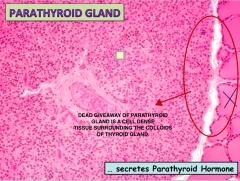
|
|
|
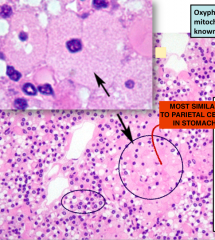
List 2 features to distinguish between oxyphil cells and the principal chief cells (Make PTH) in a histo section of the PTH gland
|
1. Principal chief cells come in clusters and contain large purple dots which are the PTH HORMONE packaged in vesicles
2. The Oxyphil cells resemble Parietal cells of stomach since they are extremely pale with a central nuclei |
|
|
Histological section of the PTH gland showing the two epithelial cell type. Know how to distinguish them.
LOOK for purple dots to indicate chief cells. And clusters of pale, central nuclei for Oxyphil |
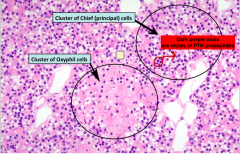
|
|
|
What is the overall function of PTH.
Which (3) organs does it work on to accomplish this and how? |
Overall function: Raise Calcium levels (antagonistic to calcitonin)
Three organs and how? Bone: Increase Osteoclast Kidney: Increase Calcium Reabsorption in the PCT Gut: Increase Vitamin D3 active synthesis so it can lead to calcium absorption |
|
|
Histological close up of the PTH chief cells again. Dont confuse them with lymph cells, since these are in clusters and close to capillaries
|
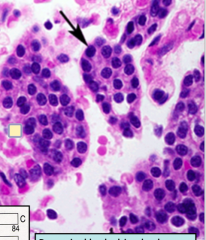
|
|
|
PTH hormone is made from 2 precursors in the Principal Chief cells. What are these precursors
|
Pre-Pro-Parathyroid Hormone
Pro-Parathyroid Hormone (underwent Nterminal cleavage) |
|
|
histological close up of the oxyphil cells. Again look like parietal (pale with central nuclei).
|
|
|
|
Which structure is the pancreas Located underneath of and which structure is it above
|
Underneath the stomach, above the duodenal intestine
|
|
|
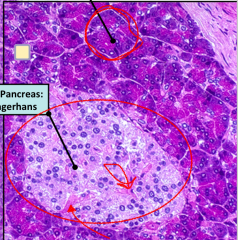
Histological section of the Endocrine pancreas.
Look for a large pale cellular area surrounded by SEROUS ACINI. These cells have no organized arrangement like the acini. They also have plenty of BV running through them |
|
|
|
Discuss the two vascular components of the Pancreas and which structures the supply?
|
Two vascular systems:
1. Insulo-Acinar PORTAL system - It transverses the islet of langerhan (endocrine) and the serous acini (exocrine. 2. Acinar Vascular system - It supplies blood exclusively to the acinar system |
|
|
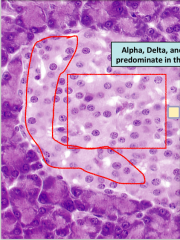
List the three main cell types in the islet, where they are found, what they secrete and function of that secretion
|
1. Beta cells = Located in the Centre of the islet, secrete insulin, lower blood glucose
2. Alpha cells = Located in the periphery of islet, secrete glucagon = raise Blood glucose 3. Delta cells = Located in the periphery of islet, secrete somatostatin = inhibit both insulin and glucagon |
|
|
Histological slide of the Islets.
Again look for a dark surrounding acini suddenly changing to a pale clusters of cell with no real organization. |
|
|
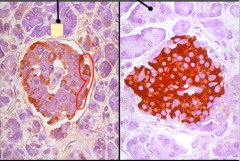
Both these islets contain a antibody against one specific. Which cell for each image and how do ya know
|
First cell contains antibodies towards Alpha cells because it lights up the periphery
Second image contains antibodies towards Beta cells because it lights up the centre and is more abundant (beta cells more abundant overall than alpha) |
|
|
Describe the synthesis and release of insulin in the beta cells.
Describe what feature clinicians use for diagnosis of insulin disorders, and why? |
Synthesized as Preproinsulin (similar to preproparatyhroid hormone)
Turns to proinsulin after Nterminal cleavage in the rER Then sent to Golgi, where it acquires disulfide bridges between the A=B segements (middle C segment still left) Buds off in a exocytic vesicle containing enzymes that cleave the C chain off to turn it into INSULIN and released. Clinicians use the C chain as a diagnostic for disorders since it has a much longer half life and is easily detectable |
|
|
What part of the brain gives rise to both the Pineal gland and the Pituitary gland?
What kind of cells does it generate? |
3rd Ventricle
It generates Neuroendocrine cells (also in the Posterior Pituitary) |
|
|
Describe the 3 step formation of the Pineal gland?
|
1. A dorsal neuroepithelial evagination of the diancephalon forms the "Pineal gland" (Evagination)
2. The neuroerpithelial tissue folds and compacts (compaction) 3. Cells differentiate into glial cells and pinealocytes and interstitial-glial-like cels (Differntiation) |
|
|
Name the distinct feature of Pineal gland histology and what it is made up of?
|
1. Brain Sand
2. Made up of Calcified Matrix proteins |
|
|
What is the name of the numerous indescript cells (no particular uniqe feature) that surround the Brain sand?
|
PINEALOCYTES
|
|
|
Histological slide of Brain sand. Note that the surrounding pinealocytes are indescript. Also there are lots of capillaries indicating endocrine function
|
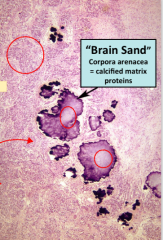
|
|
|
Another histological slide.
Make sure on practical you know what they are pointing to, if they point to the cells near the brain sand know that they are pinealocytes. |
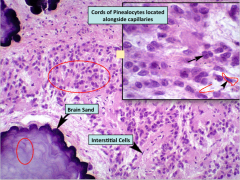
Also note that it is NOT brain sand that secretes the hormone rather the surrounding pinealocytes
|
|
|
List the 5 Steps of Melanin Regulation
|
1. Light detected by Superior Chiasmatic Nuclei
2. Information is sent down the thoracic spinal cord 3. Information reaches the Superior Cervical Ganglia 4. Post ganglionic SYMPATHETIC FIBERS INNERVATE THE PINEALOCYTES 5. Light causes supression, darkness causes stimulation |
|
|
Which 2 structures initially give rise to the pituitary gland?
|
1. Floor of the diancephalon (neuroectodermal tissue - the roof of it gave rise to pineal gland)
2. The roof of the mouth (epithelial tissue) |
|
|
Which structure does the floor of diancephalon give rise to?
Which 3 structures does the roof of the mouth give rise to? List the function of all 3! |
1. Floor of diancephalon = Pars Nervosa/ Pituitary gland
2. Roof of mouth" - Pars Tuberalis = Wraps around Nervosa - Pars Distalis = Anterior pit. Hormone releasing - Pars Intermedia = CT seprating the Nervosa and Distalis |
|
|
Name the 3 nuceli's in the Hypothalamus and where they innervate their axons?
|
1. Hypothalamic Hypophysiotropic Nuclei = Innervates the Hypothalamic hyposphystriophic portal system and this carries trophic hormones to the pars distalis
2. Paraventricular and Supraoptic nuclei innervate directly the capillary bed located in the pars nervosa |
|
|
The hypothalamic hypophysiotrophic portal system contains 2 capillary beds (like all portal system), where are these capillary beds located?
Which artery supplies these capillary beds? |
1. First capillary bed located in the Infidibulum, the second capillary bed located in the pars distalis.
2. The artery that supplies the capillary beds is the Superior Hypophyseal Artery |
|
|
Which artery supplies the capillary bed in the Pars Nervosa?
|
Inferior Hypophyseal artery
|
|
|
List the hormones from the Posterior Pituitary and which cells synthesize them?
Same thing for the Anterior Pituitary? |
Pars Nervosa = ADH, Oxytocin
Synthesized from Neruoendocrine cells Pars Distalis Acidophils: Prolactin and Growth Hormone Basophils: FSH,LH,ACTH,TSH, |
|
|
What are 2 things the Pars Nervosa is made up of?
|
Axons
Glial cells **Not neuron cell bodies, those are found in their respective nuclei (supra or para) |
|
|
Histological slide of the Pituitary gland. Note:
- The Pars distalis is darker since it contains the hormone synthesizing+Secreting cells - The nervosa is light since it contains no cell bodies - The pars intermedia is a remnant of Rathkes pouch which also contributed in development of the Anterior Pituitary |
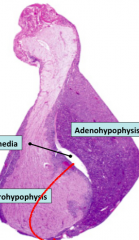
Note the white stuff in the middle is Pars Intermedia, contains CT that seperate the distalis and nervosa
|
|
|
Histo slide again of the 2 lobes, close up.
Note they will always show you them next to each other. The features you need to look for to identify are: - Light area next to a darker staining area. Sepereated by a blank space of CT called intermedia |
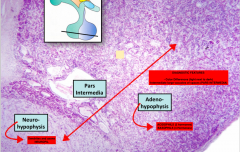
|
|
|
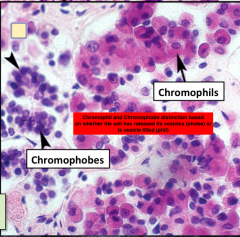
The Adenohypophysis aka Anterior Pit. Contains two distinct cell type categorized on the color of cytoplasm upon staining. What are these 2 cell types, what is the reason for color change, what color are their cytioplasm
|
1. Chromophobes = contain a blank cytoplasm, doesnt stain, and a nuclei only
2. Chromophil = Contain 2 seperate colors depending on subdivision - Acidophil: Pink staining (Prolactin/GH) - Basophil: Blue/Purple staining (TSH/ACTH/LH/FSH) The reason for color change is phobes have either released their secretory vesicles or are regenerating stem cells **Easy way to remember Acidophil hormones are "POG = physiques of greatness and also Prolacting and Growth hormone** |
|
|
Histological section of the Ant.Pit notice the diff between phobes and phils
|
|
|
|
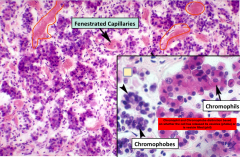
Larger section.
Again notice no acinar structure, no ducts found, tons of capillaries and two distinct cell types |
|
|
|
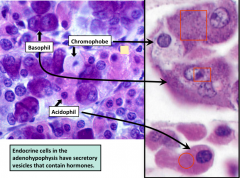
Histological section differentiating acidophil (pinkish) and basophil (blue/purpleish)
Rememer acidophil have only 2 hormones, wehre as the the basophils have 4 |
|
|
|
List the 5 SPECIFIC cell types in the Pars distalis
Under which subcategory they belong to Which hormone they secrete!!! |
1. Acidophils
Somatotrophs: GH Lactotrophs: Prolactin 2. Basophils Thyrotrophs: TSH Corticotrophs: ACTH Gonadtrophs: LH/FSH |
|
|
Once again list which hormone the somatotrophs produce.
List which primary organ they act on Which hormone this organ creates and What affect does it cause?! |
1. Somatotrophs produce Growth Hormone (Somatotrophs are Acidophils)
2. Growth Hormone acts on the liver to produce IGF-1 3. IGF-1 acts on the Bone/Epiphyseal plates to cause bone growth |
|
|
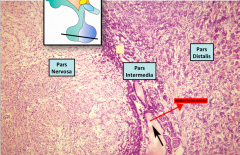
Another histological slide of the Pituitary gland.
Again note, 2 diff staining tissue seperated by a DARK DENSE CT known as PARS INTERMEDIA, REMNANT OF RATHKE You can tell there are 2 diff cell types in the Pars Distalis |
|
|
|
What is the name of the neurons contained in the Pars nervosa? ****
|
THERE ARE NO FKN NEURONS IN THE POSTERIOR PIT. AKA PARS NERVOSA THEY ARE ALL IN THE PARAVENTRICULAR OR SUPRAOPTIC NUCLEI
|
|
|
What are 4 things contained in the Pars Nervosa.
What are they all collectively referred to as? |
4 things contained: Pituicytes, capillary beds, nonmyelinated axons, axon TERMINALS
Collectively termed Neuropil |
|
|
What is the function of Pituicytes, and what specifically are they?
|
Pituicytes are glial cells
More specifically they are astro-glia SUPPORTIVE ROLE |
|
|
What is the distinctive feature of the Pars Nervosa that makes it easy to recognize?
What is the function of these features? Bonus: What is the feature of the Pineal gland, also of neuroectodermal orgigin (roof of diancephalon) |
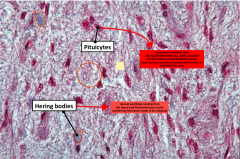
1. Pars Nervosa: herring bodies
Herring bodies are axonal swellings containing hormones (ADH,Oxytocin) ready to be released 2. Pineal gland = PINEALOCYTES (not pitui) and contain BRAIN SAND |
|
|
Histo image of the Posterior Pituitary. Note: Be able to spot Herring Bodies (homogenous mixture) and also the Pituicytes astroglia. Remember astroglia are closely located to a capillary. So that should be visible as well
|
|
|
|
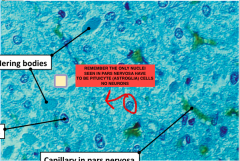
Another Histo slide of the Posterior pitutiary. Note:
There are no neuron cell bodies in the posterior pit. SO they only nuclei you see have to be of those astroglia they are the only cell type there. They are called pituicytes |
|

