![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
74 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
MOA of hypopigmentation in tinea versicolor |
Malassezia may produce Azelaic acid which then blocks melanin synthesis. Woods lamp may shel pale yellow fluorescence. |
|
|
|
Best topical treatment for tinea versicolor |
Imidazole, selenium and zinc shampoos, or oral ketoconazole 400mg weekly x 2 doses (black box warning) |
|
|
|
This substance in modified SDA inhibits growth of Hortaea werneckii |
Cycloheximide |
|
|
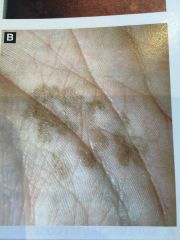
Disease and cause |
Tinea Nigra Hortaea werneckii (golden brown hyphae seen on koh) |
|
|
|
Causes of white and black piedra |
White - trichosporon cutaneum Black - piedraia Hortaea |
Don't confuse with trichophyton |
|
|
Most common cause of tinea corporis (contracted from feet) |
Trichophyton rubrum |
|
|
|
Most common cause of majocchis granuloma |
T rubrum |
|
|
|
Tinea Barbae #1 cause |
T. Mentagrophytes |
|
|
|
Most common cause of tinea faciei, tinea pedis, onychomycosis |
T. Rubrum |
|
|
|
Cause of black dot tinea and not fluorescent on woods lamp |
Endothrix (T. Tonsurans is #1) |
|
|
|
All of the microsporum species are fluorescent ectothrix except which one? |
M. Canis, audouinii, distortum, ferrugineum, gypseum are fluorescent ectothrix (yellow color due to pteridine)
M. Nanum is ectothrix but not fluorescent. |
|
|
|
Fluorescence type of the #1 cause of favus |
T. Schoenleinii (blue white fluorescence) |
|
|
|
T. Interdigitale mentagrophytes causes which infections most often |
Bullous tinea pedis Tinea Barbae White superficial onychomycosis (except in HIV where it is T. Rubrum) |
|
|
|
Number one cause of tinea capitis worldwide |
Microsporum Canis (ectothrix). T Tonsurans is #1 in USA |
|
|
|
Which of the dermatophyte species never involved hair |
Epidermophyton |
|
|
|
Maceration of webspace of fingers differential |
Erosio interdigitalis blastomycetica (candida)
Pseudomonas
Erythrasma |
|
|
|
Cause of lobomycosis |
Lacazia Loboi - Amazon and Mexico. assoc with dolphins. Brass knuckles in chains on histology. Doesn't culture. Tx: excise. |
|
|
|
Treatment of eumycotic mycetoma |
Itraconazole, ketoconazole Debridement |
|
|
|
Treatment of eumycotic mycetoma |
Itraconazole, ketoconazole Debridement |
|
|
|
Name the organisms responsible for white grain in eumycotic mycetoma |
White - acremonium, aspergillus, fusarium |
Don't confuse grains of eumycetoma with those of actinomycetoma. These are true fungi and not bacteria. |
|
|
Treatment of eumycotic mycetoma |
Itraconazole, ketoconazole Debridement |
|
|
|
Name the organisms responsible for white grain in eumycotic mycetoma |
White - acremonium, aspergillus, fusarium |
Don't confuse grains of eumycetoma with those of actinomycetoma. These are true fungi and not bacteria. |
|
|
Yellow grains in eumycetoma (Madura foot) are due to? |
Pseudallescheria boydii |
|
|
|
Treatment of eumycotic mycetoma |
Itraconazole, ketoconazole Debridement |
|
|
|
Name the organisms responsible for white grain in eumycotic mycetoma |
White - acremonium, aspergillus, fusarium |
Don't confuse grains of eumycetoma with those of actinomycetoma. These are true fungi and not bacteria. |
|
|
Yellow grains in eumycetoma (Madura foot) are due to? |
Pseudallescheria boydii |
|
|
|
Black grains in eumycetoma due to? |
Exophiala, curvularia, madurella, leptosphaeria, pyrenochaeta romeroi |
|
|
|
Most common fungal cause of Madura foot in USA (Mexico India and Africa are where this disease is seen more) |
Pseudallescheria boydii |
|
|
|
Name the dematiaceous organisms responsible for medlar bodies on histology |
Disease is chromoblastomycosis or chromomycosis.
fonsecaea pedrosoi (most common). Also rhinocladiella, phialophora, cladosporium spp. |
|
|
|
Name the dematiaceous organisms responsible for medlar bodies on histology |
Disease is chromoblastomycosis or chromomycosis.
fonsecaea pedrosoi (most common). Also rhinocladiella, phialophora, cladosporium spp. |
|
|
|
Treatment of chromoblastomycosis |
Surgery and/or itraconazole |
|
|
|
Name the dematiaceous organisms responsible for medlar bodies on histology |
Disease is chromoblastomycosis or chromomycosis.
fonsecaea pedrosoi (most common). Also rhinocladiella, phialophora, cladosporium spp. |
|
|
|
Treatment of chromoblastomycosis |
Surgery and/or itraconazole |
|
|
|
Cause of sporotrichosis |
Sporothrix schenckii - found in soil, thorns, moss. |
|
|
|
Name the dematiaceous organisms responsible for medlar bodies on histology |
Disease is chromoblastomycosis or chromomycosis.
fonsecaea pedrosoi (most common). Also rhinocladiella, phialophora, cladosporium spp. |
|
|
|
Treatment of chromoblastomycosis |
Surgery and/or itraconazole |
|
|
|
Cause of sporotrichosis |
Sporothrix schenckii - found in soil, thorns, moss. |
|
|
|
Treatment of sporotrichosis |
Itraconazole
or supersaturated potassium iodide for lymphocutaneous form |
|
|
|
Found in dust particles of southwestern USA usually manifesting in lung symptoms and rarely skin |
Coccidioidomycosis (San Joaquin valley fever) |
|
|
|
Histology of cocci? |
Spherules with double refractive thick wall, no capsule, 20-80 microns loaded with endospores |
|
|
|
Histology of cocci? |
Spherules with double refractive thick wall, no capsule, 20-80 microns loaded with endospores |
|
|
|
Cocci treatment? |
Itraconazole or other azole Amp B in pregnancy |
|
|
|
Cause of Ohio river valley disease |
Histoplasmosis - soil or bird/bat droppings. Central to southeast USA |
|
|
|
Cause of Ohio river valley disease |
Histoplasmosis - soil or bird/bat droppings. Central to southeast USA |
|
|
|
Histologic findings of histoplasma capsulatum |
Contains clear pseudocapsule around each of the tiny intracytoplasmic organisms. Looks just like leishmaniasis but lacks kinetoplast and distributed evenly throughout cytoplasm. 2-4 microns. |
|
|
|
80% of those affected by this Great Lakes/Ohio river basin disease have cutaneous findings |
Blastomycosis (North American blasto). Soil and carried by dogs. Primarily pulm infection barely symptomatic in most and then disseminates into skin. Healing centrally leads to cribiform scarring. |
|
|
|
Histology of blasto |
8-15 micron. Round yeast. Broad based budding. Thick double contoured wall. Giant cells. Neutrophilic abscesses. |
|
|
|
Organism causing blastomycosis |
Blastomyces dermatitidis |
|
|
|
Cutaneous infection in Brazil that looks like slow growing painful verrucous nodule around mouth and perioral ulcerations. |
Paracoccidioidomycosis |
|
|
|
Cutaneous infection in Brazil that looks like slow growing painful verrucous nodule around mouth and perioral ulcerations. |
Paracoccidioidomycosis |
|
|
|
Another name for paracoccidioidomycosis and fungus responsible |
South American blasto (inhalation of conidia from environment) - due to paracoccidioides brasilensis |
|
|
|
Cutaneous infection in Brazil that looks like slow growing painful verrucous nodule around mouth and perioral ulcerations. |
Paracoccidioidomycosis |
|
|
|
Another name for paracoccidioidomycosis and fungus responsible |
South American blasto (inhalation of conidia from environment) - due to paracoccidioides brasilensis |
|
|
|
Histology of paracoccidioidomycosis |
Pseudoepitheliomatous hyperplasia with narrow buds radiating outward (Mariner's wheel). |
|
|
|
Opportunistic infection with molluscoid papules when there is a secondary infection (primary skin is rare) |
Cryptococcosis |
|
|
|
Opportunistic infection with molluscoid papules when there is a secondary infection (primary skin is rare) |
Cryptococcosis |
|
|
|
Cryptococcus neoforms is found where |
Pigeon droppings, soil, dust |
|
|
|
Histo findings for cryptococcosis |
2-12micron yeast with budding, capsule stains with mucicarmine and PAS and appears clear with India ink. |
|
|
|
Histo findings for cryptococcosis |
2-12micron yeast with budding, capsule stains with mucicarmine and PAS and appears clear with India ink. |
|
|
|
Treatment of cryptococcosis |
Amp B +\- flucytosine followed by fluconazole for maintenance |
|
|
|
Most common cutaneous pathogen in aspergillosis |
Aspergillus flavus (45 degree branching)
often involves blood vessels, necrosis and hemorrhagic bullae on path |
|
|
|
Histology of zygomycosis (mucormycosis) |
Large ribbon like hyphae that appear clear/tubular with 90 degree branching with lack of neutrophils (immunicompromised usually) |
|
|
|
Major causes of zygomycosis |
Absidia, rhizopus, mucor |
|
|
|
Most common type of candida to cause paronychia |
Candida parapsilosis |
|
|
|
Most common type of candida to cause paronychia |
Candida parapsilosis |
|
|
|
Candida species that is usually fluconazole resistant |
Candida glabrata - so use itraconazole, ketoconazole, or amp B |
|
|
|
Enormous sporangia (500 microns) on histology with thousands of endospores (spherules stain red with mucicarmine) |
Rhinosporidiosis - raspberry polyps. |
|
|
|
Enormous sporangia (500 microns) on histology with thousands of endospores (spherules stain red with mucicarmine) |
Rhinosporidiosis - raspberry polyps. |
|
|
|
Cause of rhinosporidiosis |
Rhinosporidium seeberi found in India, Sri Lanka, Africa. Not a fungus but actually aquatic protozoan. |
|
|
|
Enormous sporangia (500 microns) on histology with thousands of endospores (spherules stain red with mucicarmine) |
Rhinosporidiosis - raspberry polyps. |
|
|
|
Cause of rhinosporidiosis |
Rhinosporidium seeberi found in India, Sri Lanka, Africa. Not a fungus but actually aquatic protozoan. |
|
|
|
Treatment for rhinosporidiosis |
Excision. Can't culture. But can consider Cipro. |
|
|
|
Caused by algae of stagnant water in SE ASIA and can present as olecranon bursitis - name the organism and disease |
Protothecosis - Prototheca wickerhamii |
|
|
|
Histology of Protothecosis |
Daughter cells within a theca resembling soccer ball. 6-10 microns per morula which can be inside or outside macrophage. |
|

