![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
81 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Describe the epidermis?
|
Composed of layers of stratified epithelial cells, forms a protective, waterproof avascular layer of keratin material.
|
|
|
|
Functions of the Mucous Membranes
|
Line body cavities that open to the outside of the body, joining with the skin. Found in GI, the respiratory passages, urinary tract & reproductive tracts.
|
|
|
|
Factors Affecting Skin Integrity
|
Factors influencing resistance include the person's age, the amount of underlying tissues, and illness conditions.
|
|
|
|
How does the state of a person's health have a direct effect on the condition of the skin.
|
Very thin and very obese people tend to be more susceptible to skin irritation and injury.
Fluid loss through fever, vomiting, or diarrhea reduces the fluid volume of the body. |
|
|
|
Intentional Wounds
|
An intentional wound is the result of planned invasive therapy or treatment. These wounds are purposefully created for therapeutic purposes. Examples of intentional wounds include those that result from surgery, intravenous therapy, and lumbar puncture. The wound edges are clean, and bleeding is usually controlled. Because the wound was made under sterile conditions with sterile supplies and skin preparation, the risk for infection is decreased, and healing is facilitated
|
|
|
|
Unintentional Wounds
|
Unintentional wounds are accidenta from unexpected trauma, such as from accidents, injury & burns. Because the wounds occur in an unsterile environment, contamination is likely. Wound edges are usually jagged, multiple trauma is common, and bleeding is uncontrolled. High risk for infection & longer healing time.
|
|
|
|
Closed Wounds
|
A closed wound results from a blow, force, or strain caused by trauma such as a fall, an assault, or a motor vehicle crash. The skin surface is not broken, but soft tissue is damaged, and internal injury and hemorrhage may occur. Examples include ecchymosis and hematomas
|
|
|
|
Open Wounds
|
An open wound occurs from intentional or unintentional trauma. The skin surface is broken, providing a portal of entry for microorganisms. Bleeding, tissue damage, and increased risk for infection and delayed healing may accompany open wounds. Examples include incisions and abrasions
|
|
|
|
Acute Wounds
|
Heals within days to weeks. Wound edges are well approximated & the risk of infection is lessened.
|
|
|
|
Chronic Wounds
|
Do not progress through normal sequence of repair. Wound edges are often not approximated, the risk of infection is increased, and the normal healing time is delayed.
|
|
|
|
Phases of Wound Healing
|
The wound healing process can be divided into four phases that systematically lead to repair of the injury: hemostasis, inflammation, proliferation, and maturation
|
|
|
|
Hemostasis
|
Occurs immediately after the initial injury. Blood vessels constrict & blood clots. After only a brief period of constriction, these same blood vessels dilate and capillary permeability increases & exudate fills space.
|
|
|
|
Inflammatory Phase
|
Lasting about 4 to 6 days. WBC's move to the wound. Localized body response: Pain, HEAT, REDNESS, SWELLING & generalized body response: low grade fever, malaise.
|
|
|
|
Proliferation Phase
|
Lasts for several weeks. Fibroblasts fill the wound space w/ granulation tissue Capillaries grow across the wound forms the foundation for scar tissue.
|
|
|
|
Maturation Phase
|
Begins about 3 weeks after injury, continuing for months or years. Collagen remodeled & deposited compresses the blood vessels forming a scar.
|
|
|
|
Factors Affecting Wound Healing
|
Local factors, those occurring directly in the wound, include pressure, desiccation (dehydration), maceration (over hydration), trauma, edema, infection, and necrosis (death of tissue).
Systemic factors, those occurring throughout the body, include age, circulation to and oxygenation of tissues, nutritional status, wound condition, health status, and medication use |
|
|
|
Pressure
|
Pressure disrupts the blood supply to the wound area. Persistent or excessive pressure interferes with blood flow to the tissue and delays healing
|
|
|
|
Desiccation
|
Desiccation is the process of drying up. Cells dehydrate and die in a dry environment. This cell death causes a crust to form over the wound site and delays healing.
|
|
|
|
Maceration
|
Overhydration related to urinary and fecal incontinence can lead to impaired skin integrity. This damage is related to moisture, changes in the pH of the skin, overgrowth of bacteria and infection of the skin, and erosion of skin from friction on moist skin. Refer to Chapter 37 for further discussion of maceration
|
|
|
|
Trauma
|
Repeated trauma to a wound area results in delayed healing or the inability to heal
|
|
|
|
Edema
|
Edema at a wound site interferes with the blood supply to the area, resulting in an inadequate supply of oxygen and nutrients to the tissue.
|
|
|
|
Infection
|
Bacteria in a wound increase the stress on body, requiring increased energy to deal with the invaders. Infection requires large amounts of energy be spent by the immune system to fight the microorganisms, leaving little or no reserves to attend to the job of repair and healing. In addition, toxins produced by bacteria and released when bacteria die interfere with wound healing and cause cell death
|
|
|
|
Necrosis
|
Dead tissue present in the wound delays healing. Dead tissue appears as slough, moist, yellow stringy tissue, and eschar appears as dry, black, leathery tissue. Healing of the wound will not take place with necrotic tissue in the wound. Removal of the dead tissue must occur for healing to begin
|
|
|
|
Fistula Formation
|
A fistula is an abnormal passage from an internal organ to the outside of the body or from one internal organ to another. Fistulas may be purposefully created; for example, an arteriovenous fistula is created surgically to provide circulatory access for kidney dialysis. However, fistula formation is often the result of infection that has developed into an abscess, which is a collection of infected fluid that has not drained. Accumulated fluid applies pressure to surrounding tissues, leading to the formation of the unnatural passage. The presence of a fistula increases the risk for delayed healing, additional infection, fluid and electrolyte imbalances, and skin breakdown.
|
|
|
|
Psychological Effects of Wounds
|
Because the skin is a sensory organ and plays a major role in communication with others and self-image, wounds require adaptation in the emotional as well as the physical dimension. Although stress and adaptation vary greatly among individuals, actual and potential emotional stressors are common in all patients with wounds. These stressors include pain, anxiety, fear, and changes in body image
|
|
|
|
Factors in Pressure Ulcer Development
|
Pathologic changes at a pressure ulcer site result from blood vessel collapse caused by pressure, usually from body weight. Necrosis eventually occurs, leading to the characteristic ulcer. Two mechanisms contribute to pressure ulcer development: (1) external pressure that compresses blood vessels and (2) friction and shearing forces that tear and injure blood vessels and abrade the top layer of skin.
|
|
|
|
What is the major predisposing factor for a pressure ulcer?
|
Is pressure which results in occluded blood capillaries and poor circulation to tissues. Insufficient circulation leads to necrosis and ulcer formation. A pressure ulcer may form in as little as 1 to 2 hours if the patient has not moved or been repositioned to allow circulation to flow to dependent areas
|
|
|
|
What are the r isks for Pressure Ulcer Development
|
A combination of causes, in addition to pressure, friction, & shearing, immobility, nutrition and hydration, skin moisture, mental status, & age,
Diabetes, Diminished pain awareness Fractures corticosteroid therapy Immunosuppression Poor circulation Previous pressure ulcers Significant obesity or thinness |
|
|
|
The first indication that a pressure ulcer may be developing
|
Blanching of the skin over the area under pressure. Leading to reactive hyperemia while not a pressure ulcer, this area should be watched.
|
|
|
|
Stage I pressure ulcer
|
Skin temperature (warmth or coolness), tissue consistency (firm or boggy feel), and sensation (pain, itching). The ulcer appears as a defined area of persistent redness in lightly pigmented skin, whereas in darker skin tones, the ulcer may appear with persistent red, blue, or purple hues
|
|
|
|
Describe the pressure-relieving measures for Stage I pressure ulcer
|
Frequent turning
Pressure-relieving devices Positioning |
|
|
|
Stage II
Pressure Ulcers |
Partial-thickness skin loss involving epidermis and/or dermis. The ulcer is superficial and presents clinically as an abrasion, blister, or shallow crater.
|
|
|
|
Describe the nursing care for pressure ulcer: Stage II
|
Maintenance of a moist healing environment:
Saline or Occlusive dressing that promotes natural healing but prevents formation of a scar |
|
|
|
Stage III
Pressure Ulcers |
Full-thickness skin loss involving damage or necrosis of subcutaneous tissue that may extend down to, but not through, underlying fascia. The ulcer presents clinically as a deep crater with or without undermining of adjacent tissue.
|
|
|
|
Describe the nursing care for pressure ulcer: Stage III
|
Requires debridement, which can be accomplished by one of the following:
Wet-to-dry dressings Surgical intervention Proteolytic enzymes |
|
|
|
Stage IV
Pressure Ulcers |
Full-thickness skin loss with extensive destruction, tissue necrosis, or damage to muscle, bone, or supporting structures (eg, tendon or joint capsule). Sinus tracts may also be associated with stage IV ulcers.
|
|
|
|
Describe the nursing care for pressure ulcer: Stage IV
|
Wounds are treated in the following manner:
Covered with nonadherent dressing Changed every 8 to 12 hours May require skin grafts |
|
|
|
Pain Assessment
|
Even if pain is never verbalized or expressed, always assume that pain is a definite possibility, and focus on comfort needs. Ask the patient about pain from the wound. If the patient experiences increased or constant pain from the wound, further assessments are necessary. Surgical incisional pain is usually most severe for the first 2 to 3 days and then progressively diminishes.
|
|
|
|
Wound Assessment
|
Wound assessment involves inspection (sight and smell) and palpation for appearance, drainage, odor, and pain. Wound assessment determines the status of the wound, identifies barriers to the healing process, and signs of complications. Accurate assessment provides essential baseline data and information to judge the effectiveness of treatment and wound healing progression. Skin integrity and wound assessment are performed at regular intervals, based on the nature of the wound and facility policy
|
|
|
|
When assessing a wound what should a nurse look for?
|
Location in relation to the nearest anatomic landmark, such as bony prominences. Size-measurements in mm/cm: length, width, & depth, approximation of the wound edges, signs of dehiscence or evisceration, color of the wound & surrounding area. Noting drains, tubes, staples, & sutures.
|
|
|
|
Drainage
|
The inflammatory response results in the formation of exudate, which then drains from the wound. The exudate is composed of fluid and cells that escape from blood vessels and are deposited in or on tissue surfaces. This exudate is called wound drainage and is described as serous, sanguineous, serosanguineous, or, if infected, purulent
|
|
|
|
Serous drainage
|
is composed primarily of the clear, serous portion of the blood and from serous membranes. Serous drainage is clear and watery.
|
|
|
|
Sanguineous drainage
|
consists of large numbers of red blood cells and looks like blood. Bright-red sanguineous drainage is indicative of fresh bleeding, whereas darker drainage indicates older bleeding.
|
|
|
|
Serosanguineous drainage
|
is a mixture of serum and red blood cells. It is light pink to blood tinged
|
|
|
|
Purulent drainage
|
is made up of white blood cells, liquefied dead tissue debris, and both dead and live bacteria. Purulent drainage is thick, often has a musty or foul odor, and varies in color (such as dark yellow or green), depending on the causative organism.
|
|
|
|
Describe the R in RYB wound clasification and what are the nursing interventions needed?
|
(R = Red = Protect)
Red wounds are in the proliferative stage of healing reflect the color of normal granulation tissue. Nursing interventions that include gentle cleansing, use of moist dressings, application of a transparent or hydrocolloid dressing, & dressing changes only when necessary. |
|
|
|
Describe Y of RYB Wound Classification & what are the needed nursing interventions
|
(Y = Yellow = Cleanse)
Yellow color in the wound may indicate the presence of exudate (drainage) or slough and requires wound cleaning. Characterized by oozing from the tissue covering the wound, often accompanied by purulent drainage. Drainage can be whitish yellow, creamy yellow, yellowish green, or beige. nursing interventions include irrigating the wound; using wet-to-moist dressings; using nonadherent, hydrogel, or other absorptive dressings; and consulting with the physician about using a topical antimicrobial medication to decrease the growth of bacteria. |
|
|
|
Describe B of RYB Wound Classification & what are the needed nursing interventions
|
B = Black = Débride)Black in the wound may indicate the presence of an eschar (necrotic tissue), which is usually black but may also be brown, gray, or tan.
The eschar requires débridement (removal) before the wound can heal. These wounds are often cared for by advanced practice nurses who are educated in the care of more complex wounds. The eschar may be removed by sharp débridement (using a scalpel or scissors to cut away the dead tissue), mechanical débridement (scrubbing the wound or applying a wet-to-moist or dry dressing), chemical débridement (using collagenase enzyme agents), or autolytic débridement (using a dressing that contains wound moisture to help the body produce enzymes to break down the eschar). After débridement, the wound is treated as a yellow wound and then, as healing progresses, a red wound. |
|
|
|
Common Types of Drains
Penrose |
Provides sinus tract After incision and drainage of abscess, in abdominal surgery
|
|
|
|
Common Types of Drains
T-tube |
For bile drainage After gallbladder surgery
|
|
|
|
Common Types of Drains
Jackson-Pratt |
Decrease dead space by collecting drainage After breast removal, abdominal surgery
|
|
|
|
Common Types of Drains
Hemovac |
Decrease dead space by collecting drainage After abdominal, orthopedic surgery
|
|
|
|
List the nursing diagnoses related to skin integrity and wound care.
|
Disturbed Body Image
Deficient Knowledge related to wound care Acute Pain Chronic Pain Impaired Skin Integrity Activity Intolerance Self-care Deficit Risk for Impaired Skin Integrity Impaired Tissue Integrity Risk for Trauma Readiness for Enhanced Knowledge: Wound Care may be appropriate for patients who request information about wound care at home |
|
|
|
Outcome Identification and Planning for patients who have or are at risk for impaired skin and tissue integrity
|
Remain free of signs and symptoms of infection
Maintain skin integrity Demonstrate self-care measures to prevent pressure ulcer development Demonstrate self-care measures to promote wound healing Demonstrate evidence of wound healing Demonstrate increase in body weight and muscle size, if appropriate Remain free of infection at the site of the wound or pressure ulcer Experience no new areas of skin breakdown Verbalize that the pain management regimen relieves pain to an acceptable level Be discharged to home within established parameters Demonstrate appropriate wound care measures before discharge Verbalize understanding of signs and symptoms to report and necessary follow-up care |
|
|
|
Infection prevention
|
Signs and symptoms of infection to be immediately reported to the healthcare provider
Need to watch for increased body temperature, red or separated wound edges, increased pain in the wound, and increased drainage that is thick and has a foul odor Wearing of disposable gloves when changing the dressing Hand hygiene before putting on and after removing the gloves Proper methods for disposal of old dressing, such as wrapping old dressing in several layers of newspaper or putting it in a plastic bag before disposal in a trash container |
|
|
|
What factors encourage wound healing?
|
Importance of eating well-balanced meals that are high in protein and vitamins
Need to drink 6 to 8 glasses of fluids each day Rest periods during the day Modifications in activities of daily living and exercise until healing is complete and approval is given by healthcare provider |
|
|
|
Body temperature is regulated
|
Body temperature is regulated by cells in the hypothalamus in response to signals from thermal (heat and cold) receptors located close to the skin's surface. Stimulation of these receptors sends sensory messages to the anterior hypothalamus to initiate mechanisms to dissipate heat (through vasodilation and sweating) or to preserve warmth through vasoconstriction and piloerection (“goose bumps”). Pain receptors, also located near the skin's surface, are also affected by heat and cold as painful stimuli, with excessive heat
|
|
|
|
Effects of Applying Heat
|
The application of local heat dilates peripheral blood vessels, increases tissue metabolism, reduces blood viscosity and increases capillary permeability, reduces muscle tension, and helps relieve pain. Vasodilation increases local blood flow. In turn, the supply of oxygen and nutrients to the area is increased, and venous congestion is decreased. As local blood flow increases, the viscosity of blood is reduced and increased capillary permeability improves the delivery of leukocytes and nutrients while also facilitating the removal of wastes and prolonging clotting time. These actions, combined with increased tissue metabolism, accelerate the inflammatory response to promote healing.
Heat reduces muscle tension to promote relaxation and helps to relieve muscle spasms and joint stiffness. Heat also helps relieve pain by stimulating specific nerve fibers, closing the gate that allows the transmission of pain stimuli to centers in the brain. Because of these local physiologic effects, heat in various forms is used to treat infections, surgical wounds, inflamed tissue, arthritis, joint and muscle pain, dysmenorrhea, and chronic pain. |
|
|
|
Effects of Applying Cold
|
The local application of cold constricts peripheral blood vessels, reduces muscle spasms, and promotes comfort. Cold reduces blood flow to tissues and decreases the local release of pain-producing substances such as histamine, serotonin, and bradykinin. This action in turn reduces the formation of edema and inflammation. Decreased metabolic needs and capillary permeability, combined with increased coagulation of blood at the wound site, facilitate the control of bleeding and reduce edema formation.
Cold also reduces muscle spasm, alters tissue sensitivity (producing numbness), and promotes comfort by slowing the transmission of pain stimuli. Cold, for these effects, is used after direct trauma, for dental pain, for muscle spasms, after sprains, and to treat some chronic pain syndromes. |
|
|
|
Physiologic Considerations Heat and Cold Therapy
|
The rebound phenomenon is important to the therapeutic value of heat and cold and to the safety of patients receiving such therapy. Heat produces maximum vasodilation in 20 to 30 minutes; if heat is continued beyond that time, tissue congestion and vasoconstriction occur (for unknown reasons). With cold, maximum vasoconstriction occurs when the skin reaches 15°C (60°F); then vasodilation begins.
The ability of the body to adapt to heat and cold is an important consideration when applying heat or cold and when teaching patients and caregivers about heat and cold therapy. Initially, heat and cold skin receptors are strongly stimulated by sudden changes in temperature. For the first few seconds after being stimulated, the response decreases rapidly; it then decreases more slowly for the next 30 minutes, as the receptors adapt to the temperature. A hot application, even if the temperature remains constant, does not feel as warm after adaptation has taken place. Be sure to inform patients that increasing the temperature or lengthening the time of application can seriously damage tissues. |
|
|
|
The Nursing Process for Heat and Cold Therapy
|
Before initiating heat or cold therapy, assess the patient's physical and mental status, the condition of the body area to be treated with heat or cold, and the condition of the equipment to be used. Carefully evaluate factors influencing the patient's ability to tolerate heat and cold applications. These factors are the basis for the following considerations with rationale:
|
|
|
|
Explain the difference between primary and secondary skin lesions.
|
Primary lesions are those present at the initial onset of the disease
Secondary lesions are the result of changes over time caused by disease progression, manipulation (scratching, rubbing, picking) or treatments. |
|
|
|
MACULE
|
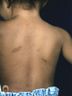
Name the primary lesion
|
A macule is a change in the color of the skin. It is flat, if you were to close your eyes and run your fingers over the surface of a purely macular lesion, you could not detect it.
|
|
|
PAPULE
|
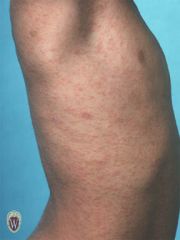
Name this primary lesion
|
A papule is a solid raised lesion that has distinct borders and is less than 1 cm in diameter. Papules may have a variety of shapes in profile (domed, flat-topped, umbilicated) and may be associated with secondary features such as crusts or scales.
|
|
|
NODULE
|
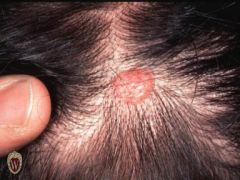
Name this primary lesion
|
A nodule is a raised solid lesion more than 1 cm. and may be in the epidermis, dermis, or subcutaneous tissue.
|
|
|
VESICLE
|
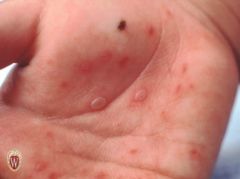
Name the primary lesion
|
Vesicles are raised lesions less than 1 cm. in diameter that are filled with clear fluid.
|
|
|
BULLAE
|
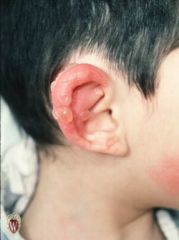
Name the primary lesion
|
Bullae are circumscribed fluid-filled lesions that are greater than 1 cm. in diameter.
|
|
|
PUSTULE
|
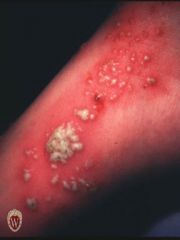
Name the primary lesion
|
Pustules are circumscribed elevated lesions that contain pus. They are most commonly infected (as in folliculitis) but may be sterile (as in pustular psoriasis).
|
|
|
WHEAL
|
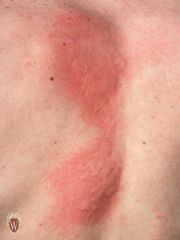
Name the primary lesion
|
A wheal is an area of edema in the upper epidermis.
|
|
|
EXCORIATION
|
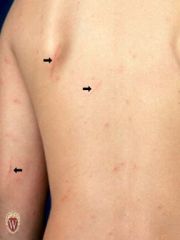
What is the Secondary Lesion
|
Excoriations are traumatized or abraded skin caused by scratching or rubbing
|
|
|
LICHENIFICATION
|
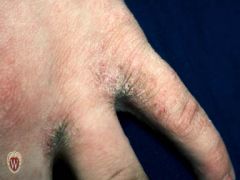
Name this secondary lesion
|
"Lichenification" refers to a thickening of the epidermis seen with exaggeration of normal skin lines. It is usually due to chronic rubbing or scratching of an area.
|
|
|
FISSURE
|
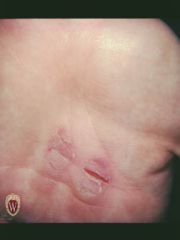
Name the secondary lesion
|
A fissure is linear cleavage of skin which extends into the dermis.
|
|
|
ULCERATION
|
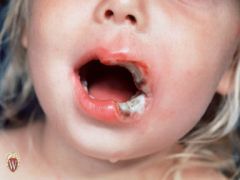
Name the secondary lesions
|
Ulcerations occur when there is necrosis of the epidermis and dermis and sometimes of the underlying subcutaneous tissue.
|
|
|
SCAR
|
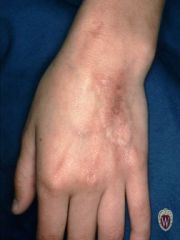
Name the secondary lesions
|
Scars are the permanent fibrotic changes that occur on the skin following damage to the dermis. Scars may have secondary pigment characteristics.
|
|
|
KELOIDS
|
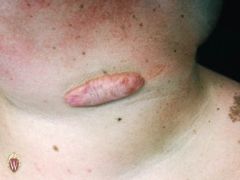
Name the secondary lesion
|
Keloids are an exaggerated connective tissue response of injured skin that extend beyond the edges of the original wound.
|
|
|
What is: PETECHIAE, PURPURA, AND ECCHYMOSES
|
Three terms that refer to bleeding that occurs in the skin are petechiae, purpura, and ecchymoses. Generally, the term "petechiae" refers to smaller lesions. "Purpura" and "ecchymoses" are terms that refer to larger lesions. In certain situations purpura may be palpable. In all situations, petechiae, ecchymoses, and purpura do not blanch when pressed. If there is any question, press on the lesions carefully with a glass slide. Don't break the slide or cut the patient.
|
|
|
|
PETECHIAE
|
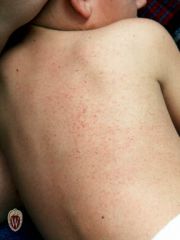
I cause bleeding that occurs in the skin forming small lesions, I am very common among the elderly, what am I?
|
|
|
|
PURPURA
|
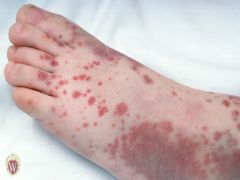
What am I?
|
|
|
|
PLAQUE
|
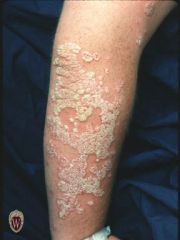
Name the primary lesion
|
A plaque is a solid, raised, flat-topped lesion greater than 1 cm. in diameter. It is analogous to the geological formation, the plateau.
|
|
|
ESCHAR
|
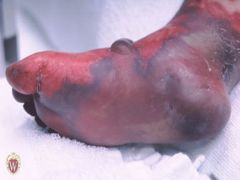
What secondary lesion is this?
|
An eschar is a hard plaque covering an ulcer implying extensive tissue necrosis, infarcts, deep burns, or gangrene.
|
|
|
epidermis, dermis
|
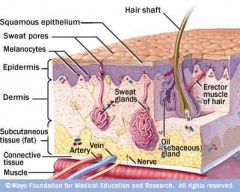
Describe the layers of skin
|
|

