![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
476 Cards in this Set
- Front
- Back
|
Do active phagocytosis as part of the mononuclear phagocyte system; process and present antigens; participate in wound healing |
MACROPHAGES |
|
|
Process antigens and present them to lymphocytes |
DENDRITIC CELLS |
|
|
Produce antibodies against specific antigens |
B LYMPHOCYTES (plasma cells) |
|
|
Kill tumor cells and virus infected cells |
NATURAL KILLER CELLS |
|
|
Precursor cells for macrophages |
MONOCYTES |
|
|
Do phagocytosis early on inflammation; kill bacteria |
NEUTROPHILS |
|
|
Defend against parasites |
EOSINOPHILS |
|
|
The term hematopoiesis refers to the production of (1) and occurs primarily in the (2) after birth. |
1) blood cells 2) bone marrow |
|
|
Each hemoglobin A molecule consists of how many globin chains and how many hemes? |
4 & 4 |
|
|
In order to bind to oxygen, the iron portion of heme must be ...? |
Ferrous Fe2+ |
|
|
What hormone regulates absorption of dietary iron? |
hepcidin |
|
|
After absorption, iron circulates attached to (1) And is stored inside cells attached to (2) |
1) transferrin 2) ferritin |
|
|
After absorption, iron circulates attached to (1) And is stored inside cells attached to (2) |
1) transferrin 2) ferritin |
|
|
What do nitric oxide and prostacyclin do to platelet adhesion and aggregation? |
Inhibit |
|
|
What do thromboxane A2, epinephrine, thrombin, and collagens do to platelet adhesion? |
Trigger |
|
|
What are the primary lymphoid organs? |
Thymus Bone marrow |
|
|
What are the primary lymphoid organs? |
Thymus Bone marrow |
|
|
What are the secondary lymphoid organs? |
Spleen Lymph nodes Peter patchhes (gut associated lymphoid tissue) Tonsils |
|
|
What stabilizes a platelet plug and what is the source of the stabilizing substance? |
Strands of fibrin Fibrin comes from the action of thrombin on fibrinogen, an inactive precuror that circulates in the blood until the clotting system is activated |
|
|
How do platelets expel the serum from the platelet plug this increasing its strength? |
Platelets have actin and myosin filaments in them that enable them to contract. This contraction of aggregated platelets expels the serum from inside the clot |
|
|
What is the difference between PLASMA and SERUM? |
Plasma: liquid portion of blood with its dissolved substances
Serum: is plasma MINUS the clotting favtors |
|
|
What is the difference between a MULTIPOTENT STEM CELL and a HEMATOPOIETIC STEM CELL? |
Multipotent stem cell can differentiate into many different types of cells
Hematopoietic stem cells can only differentiate into various types of BLOOD cells |
|
|
What is the difference between FERRITIN and APOFERRITIN? |
Ferritin: a protein that binds and stores iron
APOFERRITIN: ferritin that does NOT have iron attached |
|
|
What is the different between MITOSIS and ENDOMITOSIS? |
Mitosis: normal cell division that includes DNA replication, anaphase, and cytokinesis
Endomitosis: type of cell division done by megakaryocyte progenitors in which DNA replication occurs but anaphase And cytokinesis are blocked this producing s cell with s large polyploid nucleus and numerous organelles that fragments into platelets |
|
|
The most abundant plasma protein is...? |
ALBUMIN |
|
|
The most abundant plasma protein is...? |
ALBUMIN |
|
|
The most abundant leukocytes are the ...? |
NEUTROPHILS |
|
|
What is another name for platelets? |
Thrombocytes |
|
|
What is another name for platelets? |
Thrombocytes |
|
|
Platelets are cytoplasm is fragments of large cells called (1) that are located in the (2) |
1) megakaryocytes 2) bone marrow |
|
|
Erythropoietin stimulates bone marrow to produce more ...? |
Erythrocytes |
|
|
Thrombopoietin stimulates bone marrow to produce more ...? |
Platelets |
|
|
Tissue factor is also called tissue ...? |
Thromboplastin |
|
|
Tissue factor triggers the ... pathway of clotting |
Extrinsic |
|
|
Plasmid is an enzyme that degrades ... polymers. |
Fibrin |
|
|
Plasmid is an enzyme that degrades ... polymers. |
Fibrin |
|
|
The inactive precursor to plasmin is (1) which is produced by the (2). |
1) plasminogen 2) liver |
|
|
What function is inhibited by plasminogen activators? |
Fibrin stability |
|
|
What function is inhibited by thrombomodulin, protein C, and protein S |
Clotting cascade |
|
|
What function is inhibited by tissue factor pathway inhibitor? |
Clotting cascade |
|
|
What function is inhibited by prostacyclin? |
Platelet activation and aggregation |
|
|
What function is inhibited by prostacyclin? |
Platelet activation and aggregation |
|
|
What function is inhibited by antithrombin III? |
Clotting cascade |
|
|
What function is inhibited by prostacyclin? |
Platelet activation and aggregation |
|
|
What function is inhibited by antithrombin III? |
Clotting cascade |
|
|
What function is inhibited by nitric oxide? |
Platelet activation and aggregation |
|
|
Increased blood level of immature erythrocytes |
Reticulocytosis |
|
|
Increased number or volume of circulating erythrocytes |
Polycythemia |
|
|
Increased number or volume of circulating erythrocytes |
Polycythemia |
|
|
Decreased number or volume of circulating erythrocytes |
Anemia |
|
|
Premature death of damaged erythrocytes |
Eryptosis |
|
|
Having erythrocytes of different shapes |
Poikilocytosis |
|
|
Having erythrocytes of different sizes |
Anisocytosis |
|
|
Decreased number of circulating erythrocytes, leukocytes, and platelets |
Pancytopenia |
|
|
When plasma volume increases to compensate for anemia, blood viscosity (1) which causes blood flow to be (2) |
1) decreases 2) turbulent |
|
|
Defective DNA synthesis in bone marrow precursors usually creates erythrocytes that are ... and normochromic |
Macrocytic |
|
|
Lactose Erin released by neutrophils during bacterial infection (1) iron thus contributing to (2) |
1) binds 2) anemia of chronic disease |
|
|
Hemolysis from a mismatched blood transfusion is an example of (1) hemolytic anemia that occurs (2) |
1) alloimmune 2) intravascularly |
|
|
What is the appearance of the erythrocytes in iron deficiency anemia? |
Microcytic-hypochromic |
|
|
What is the appearance of the erythrocytes in aplastic anemia? |
Normocytic-normochromic |
|
|
What is the appearance of the erythrocytes in aplastic anemia? |
Normocytic-normochromic |
|
|
What is the appearance of the erythrocytes in pernicious anemia? |
Macrocytic-normochromic |
|
|
What is the appearance of the erythrocytes in aplastic anemia? |
Normocytic-normochromic |
|
|
What is the appearance of the erythrocytes in pernicious anemia? |
Macrocytic-normochromic |
|
|
What is the appearance of the erythrocytes in posthemorrhagic anemia? |
Normocytic-normochromic |
|
|
What is the appearance of the erythrocytes in thalassemia? |
Microcytic-hypochromic |
|
|
What is the appearance of the erythrocytes in sickle cell anemia? |
Normocytic-normochromic |
|
|
What is the appearance of the erythrocytes in folate deficiency anemia? |
Macrocytic-normochromic |
|
|
What is the appearance of the erythrocytes in anemia of chronic disease? |
Normocytic-normochromic |
|
|
What is the general cause of hereditary spherocytosis? |
Increased erythrocyte destruction |
|
|
What is the general cause of anemia of chronic disease? |
Impaired erythrocyte production |
|
|
What is the general cause of iron deficiency anemia? |
Impaired erythrocyte production |
|
|
What is the general cause of sickle cell anemia? |
Increased erythrocyte destruction |
|
|
What is the general cause of sickle cell anemia? |
Increased erythrocyte destruction |
|
|
What is the general cause of G6PD deficiency? |
Increased erythrocyte destruction |
|
|
What is the general cause of sickle cell anemia? |
Increased eryhrocyte destruction |
|
|
What is the general cause of G6PD deficiency? |
Increased erythrocyte destruction |
|
|
What is the general cause of pernicious anemia? |
Impaired erythrocyte production |
|
|
What is the general cause of aplastic anemia? |
Impaired erythrocyte production |
|
|
What is the general cause of aplastic anemia? |
Impaired erythrocyte production |
|
|
What is the general cause of folate deficiency anemia? |
Impaired erythrocyte production |
|
|
What is the technical term for the appearance of the tongue that has lost papillae and looks fissured? |
Glossitis |
|
|
What is the technical term for concave brittle fingernails? |
Koilonychia |
|
|
Glossitis And koilonychia are characteristic of what type of anemia? |
Iron deficiency anemia |
|
|
What term describes the color and amount of hemoglobin in the erythrocytes of iron deficiency anemia? |
Hypochromic |
|
|
Hereditary hemochromatosis is an autosomal (1) disorder that causes increased absorption of dietary (2) |
1) recessive 2) iron |
|
|
Sideroblstic anemia’s are characterized by defective synthesis of (1) and may be acquired or hereditary, in which case they usually have recessive (2) transmission. |
1) heme 2) x linked |
|
|
Myelodysplastic syndrome involves defects in all lines of hematopoietic (1) cells; some persons with this condition develop acute (2) |
1) stem 2) leukemia |
|
|
Myelodysplastic syndrome involves defects in all lines of hematopoietic (1) cells; some persons with this condition develop acute (2) |
1) stem 2) leukemia |
|
|
What levels are used to evaluate iron elevens when diagnosing anemia? |
Serum ferritin levels |
|
|
Release of (1) during chronic inflammation contributes to the anemia of chronic disease by decreasing the availability of (2) and inhibiting erythrocytes progenitors |
1) cytokines 2) iron |
|
|
Release of (1) during chronic inflammation contributes to the anemia of chronic disease by decreasing the availability of (2) and inhibiting erythrocytes progenitors |
1) cytokines 2) iron |
|
|
Congenital hemolytic anemia’s are caused by (1) defects in erythrocytes but acquired hemolytic anemia’s usually are caused by the (2) system. |
1) intrinsic 2) immune |
|
|
Hemolysis in most inherited hemolytic anemia’s occurs in the (1) by the action if (2). |
1) spleen 2) macrophages |
|
|
Warm autoimmune hemolytic anemia is caused by (1) binding to erythrocytes with subsequent destruction if those erythrocytes in the (2). |
1) IgG 2) spleen |
|
|
Drug-induced hemolytic anemia from antibiotics usually begins when the antibiotic serves as a ... and binds to erythrocyte proteins. |
Hapten |
|
|
Bone marrow can increase erythrocyte production up to ... times it’s normal rate |
8 |
|
|
When does jaundice occur as a result of hemolysis? |
When heme destruction exceeds the liver’s ability to process and excrete bilirubin |
|
|
What is the location of the erythrocyte defect in thalassemia? |
Hemoglobin synthesis defect |
|
|
What is the location of the erythrocyte defect in thalassemia? |
Hemoglobin synthesis defect |
|
|
What is the location of the erythrocyte defect in hereditary spherocytosis? |
Membrane defect |
|
|
What is the location of the erythrocyte defect in sickle cell anemia? |
Hemoglobin synthesis defect |
|
|
What is the location of the erythrocyte defect in G6PD deficiency anemia? |
Enzyme pathway defect |
|
|
What is the location of the erythrocyte defect in G6PD deficiency anemia? |
Enzyme pathway defect |
|
|
What is the location of the erythrocyte defect in paroxysmal nocturnal hemoglobinuria? |
Membrane defect |
|
|
What is the difference between leukemia and lymphoma? |
Leukemia: cancers of blood-forming cells Lymphoma: cancers of lymphatic tissue |
|
|
What is the difference between a lymphocytic and myelogenous leukemia? |
Lymphocytic: arises from the lymphoid cellnline that normally produces B and T lymphocytes and natural killer cells
Myelogenous: arises from the myeloid cell line that normally produces granulocytes, monocytes, erythrocytes, And platelets |
|
|
What is the difference between splenomegaly and hypersplenism? |
Splenomegaly: enlargement of the spleen Hypersplenism: overactivity of the spleen cause by splenomegaly |
|
|
What is the difference between the composition of arterial thrombi and venous thrombi? |
Arterial: composed primarily of platelet aggregates held together by strands of fibrin Venous: composes primarily of erythrocytes, greater amounts of fibrin and fewer platelets |
|
|
Enlarged lymph nodes |
Lymphadenopathy |
|
|
Lower than normal neutrophil count in the blood |
Neutropenia |
|
|
Lower than normal blood counts of white blood cells red blood cells and olatekets |
Pancytopenia |
|
|
Lower than normal blood counts of white blood cells red blood cells and platelets |
Pancytopenia |
|
|
Higher than normal WBC count |
Leukocytosis |
|
|
Lower than normal WBC count |
Leukopenia |
|
|
Higher than normal blood counts of neutrophils, eosinophils, and basophils |
Granulocytosis |
|
|
Lower than normal blood counts of neutrophils, eosinophils, basophils |
Granulocytopenia |
|
|
Complete absence of neutrophils, eosinophils, and basophils in the blood |
Agranulocytosis |
|
|
Monocytosis occurs during the (1) phase of inflammation whereas neutrophils occurs during the (2) phase of inflammation |
1) late 2) early |
|
|
All types of leukemia are characterized by uncontrolled (1) of WBC in the (2) that thereby (3) the amount and function of erythrocytes and platelets |
1) production 2) bone marrow 3) decreases |
|
|
What does an activated platelet release in a HIT reaction? |
Platelet factor 4 |
|
|
What does an activated platelet release in a HIT reaction? |
Platelet factor 4 |
|
|
When a person forms HIT antibodies they react specifically against what? |
PF4-heparin complex |
|
|
In HIT by what mechanism do more platelets become activated causing more clotting? |
After HIT antibodies bind the PF4-heparin complex, the Fc (nonspecific) end of the antibodies binds to platelet FC receptors, activating the platelets which release substances that promote clotting |
|
|
What causes thrombocytopenia in HIT? |
Platelet number decreases because of micro clots, extension of previous clots, or formation of new clots, all of which use up platelets |
|
|
Autoantibody against plasma membrane components that causes hypercoaguability by binding to platelets and endothelial cells |
Antiphospholipid antibody |
|
|
Autoantibody against plasma membrane components that causes hypercoaguability by binding to platelets and endothelial cells |
Antiphospholipid antibody |
|
|
Abnormal antibody released by malignant plasma cells in multiple myeloma |
M protein |
|
|
Autoantibody against plasma membrane components that causes hypercoaguability by binding to platelets and endothelial cells |
Antiphospholipid antibody |
|
|
Abnormal antibody released by malignant plasma cells in multiple myeloma |
M protein |
|
|
Genetic mutation that causes hypercoagulability by allowing activated clotting factor Va to remain longer in the blood |
Factor V Leiden |
|
|
Mutant tyrosine kinase that derived cell proliferation and survival in some types of leukemia |
BCR-ABL1 variant oncoprotein |
|
|
Genetic translocation between chromosomes 9 and 22 that creates a mutant protein implicated in CML and other types of leukemia |
Philadelphia chromosome |
|
|
Infectious mononucleosis is an acute infection of (1) lymphocytes commonly caused by (2); typical clinical manifestations are pharyngitis, fever, and cervical (3) |
1) B 2) Epstein-Barr virus 3) lymphadenopathy |
|
|
In Africa, (1) lymphoma, a rapidly growing (2) lymphocyte tumor in the (3) And facial bones of children is associated with EBV |
1) Burkitt 2) b 3) jaw |
|
|
AML stands for (1) and CLL stands for (2) |
1) acute myelogenous leukemia 2) chronic lymphocytic leukemia |
|
|
Hypercalcemia And bone lesions are characteristics of (1) because the malignant cells reside in the bone marrow and not in the circulating blood |
Multiple myeloma |
|
|
The term ... disorder indicates that leukemia’s are considered to be the product of a mutated progenitor cell that replicated itself uncontrollably |
Clonal |
|
|
Abnormally precipitated oxidized hemoglobin within an erythrocyte |
Heinz body |
|
|
An endogenous inhibitor of coagulation |
Protein S |
|
|
An endogenous inhibitor of coagulation |
Protein S |
|
|
Presence of immature Buckeyes RBC’s in the blood |
Erythroblastosis |
|
|
Normal enzyme that protects erythrocytes from oxidative damage |
G6PD |
|
|
A child with a G6PD deficiency must not be given (1) because it could trigger a (2) episode |
1) aspirin 2) hemolytic |
|
|
Normally (1) genes control synthesis of the hemoglobin alpha chains and (2) genes control beta chain synthesis, which is crucial to understanding the various forms of (3) |
1) 4 2) 2 3) thalassemia |
|
|
Von Willebrand disease is s genetic (1) condition |
Hemorrhagic |
|
|
What is the difference between the hemoglobin chains of adults and embryonic and fetal hemoglobin? |
Adult: composed of 2 alpha and 2 beta polypeptide chains
Embryonic and feral: 2 alpha and 2 gamma polypeptide chains |
|
|
What is the difference between the frequency of hemolysis in children who have hereditary spherocytosis and G6PD deficiency? |
Children who have hereditary spherocytosis experience persistent hemolysis because their erythrocytes have a membrane defect that makes them fragile Children who have G6PD deficiency do not have hemolysis unless they are exposed to certain drugs or other oxidative stressors that trigger hemolytic crisis |
|
|
What is difference between the chemical structures of hemoglobin A and hemoglobin S? |
A; normal adult hemoglobin with 2 alpha and 3 beta chains
S: associated with sickle cell disease has valine instead of glutamic acid at particular point on the beta chains |
|
|
What is the genetic difference between sickle cell anemia and sickle cell trait? |
Persons with sickle cell anemia have two copies of the mutated gene (homozygous) and produce only hemoglobin S Persons with sickle cell trait have one mutated gene (heterozygous) and produce a mixture of hemoglobin a and s |
|
|
What causes hemoglobin and hematocrit levels to be so different between birth and 3 months? |
Fetal intrauterine environment is hypoxia which stimulates fetal erythropoietin production and drives erythropoiesis |
|
|
Why does cord blood have high reticulocyte levels? |
Reflect very active erythropoiesis of fetal life |
|
|
Why does cord blood have high reticulocyte levels? |
Reflect very active erythropoiesis of fetal life |
|
|
What is the difference between the normal WBC count in an infant and school aged child? And why is this important to know? |
Normal WBC count is much higher in an infant than in a school aged child Important to understand so as not to mistake a normally high WBC count as an indication of infection |
|
|
Before the bone marrow is functional in a fetus production of erythrocytes takes place primarily in the ...? |
Liver |
|
|
A child who has sickle cell anemia and develops a parovirus B19 infection may develop ... crisis? |
Aplastic |
|
|
Acute chest syndrome in sickle cell anemia occurs when sickles erythrocytes cause ... infarction. |
Lung |
|
|
Young children with sickle cell anemia may develop (1) crisis when large amounts of blood oi in the spleen and liver potentially causing death from (2) |
1) sequestration 2) cardiovascular collapse |
|
|
Beta-thalassemia major is also called ... |
Cooley anemia |
|
|
In beta thalassemia the erythrocytes are unstable and prone to hemolysis because they have too many free hemoglobin .... chains. |
Alpha |
|
|
Children with hemophilia experience recurrent episodes of (1) And may develop limited mobility due to damage to (2) from some of these episodes |
1) bleeding 2) joints |
|
|
The most common leukemia in children is ... |
Acute lymphocytic leukemia |
|
|
Fever in acute leukemia is caused by (1) due to decreased neutrophils and by (2) from rapid growth of leukemic cells |
1) infection 2) hypermetabolism |
|
|
Children who have inherited deficiencies of antithrombin III or protein C or S have increased risk for ... |
Thrombosis |
|
|
Hodgkin lymphoma is characterized by (1) enlargement of supraclavicular or cervical lymph nodes and has some association with (2) |
1) painless 2) Epstein Barr virus |
|
|
Childhood non-Hodgkin lymphoma can arise from any (1) tissue and is more similar clinically and histologicslly to acute (2) than it is to adult non-Hodgkin lymphoma |
1) lymphoid 2) lymphocytic leukemia |
|
|
Autosomal recessive factor XI deficiency |
Hemophilia C |
|
|
X-linked recessive factor VIII DEFICIENCY |
Hemophilia A |
|
|
X-linked recessive factor VIII DEFICIENCY |
Hemophilia A |
|
|
X/linked recessive factor IX deficiency |
Hemophilia B |
|
|
What electrical event occurs in the myocardium that generates the P wave on an ECG? |
Atrial depolarization |
|
|
What electrical event occurs in the myocardium that generates the P wave on an ECG? |
Atrial depolarization |
|
|
What do the Syria do in response to depolarization? |
Contract |
|
|
What electrical event occurs in the myocardium that generates the P wave on an ECG? |
Atrial depolarization |
|
|
What do the Syria do in response to depolarization? |
Contract |
|
|
What happens in the ventricles on the ECG from the R to the end of the T wave? |
Ventricular systole |
|
|
What part of the ECG does the mitral valve close? |
Q wave |
|
|
Why is it important for the mitral and tricuspid valves to close at the same time? |
Prevents backward flow of blood into the Atria as the ventricles contract |
|
|
What is the difference between the endocardium and the epicardium? |
Endocardium is the innermost later of the heart
The epicardium is the outermost layer of the heart |
|
|
What is the difference between angiogenesis and arteriogenesis? |
Angiogenesis is the growth of new capillaries
Arteriogenesis is a new artery branching off from a preexisting artery |
|
|
What is the difference between exercise hyperemia and reactive hyperemia? |
Exercise: locally increased blood flow caused by vasodilation in an exercising muscle
Reactive: locally increased blood flow caused by vasodilation after a period of tissue ischemia |
|
|
What is the difference between laminar flow and turbulent flow? |
Laminar flow has concentric layers of molecules that move parallel to the vessel wall
Turbulent flow has eddy currents that move in whorls creating more resistance to flow and a less beneficial effect on the endothelium |
|
|
Provides one way flow of blood from the right atrium into the right venteicle |
Tricuspid valve |
|
|
Anchors the heart valve cusps to the papillary muscles to prevent valve prolapse |
Chordae tendonae |
|
|
The RIGHT atrioventricular valve has (1) cusps And is called the (2) valve |
1) 3 2) tricuspid |
|
|
The RIGHT atrioventricular valve has (1) cusps And is called the (2) valve |
1) 3 2) tricuspid |
|
|
The LEFT atrioventricular valve has (1) cusps and is called the (2) valve... |
1) two 2) mitral |
|
|
Binding of ATP to myosin requires (1) to enable myocardial contraction; excitation-contraction coupling requires (2). |
1) magnesium 2) calcium |
|
|
Which causes a faster heart rate: sympathetic nerve firing or parasympathetic nerve firing? |
Sympathetic |
|
|
Which causes a faster heart rate: stimulation of cardiac B1 receptors or cardiac B2 receptors? |
B1 |
|
|
The aortic and pulmonary valves are the (1) valves and they each have (2) cusps. |
1) semilunar 2) three |
|
|
Another name for the epicardium is the ... pericardium. |
Visceral |
|
|
Two important branches of the left coronary artery are the left (1) and the (2) artery. |
1) anterior descending 2) circumflex |
|
|
Parasympathetic nerves to the heart release the neurotransmitter (1) which binds to (2) receptors. |
1) acetylcholine 2) cholinergic |
|
|
Sympathetic nerves to the heart release the neurotransmitter (1) which binds to (2) receptors. |
1) norepinephrine 2) adrenergic |
|
|
The process of ... enables an organ to regulate its blood flow by altering the resistance in its arterioles. |
Auto regulation |
|
|
The right lymphatic duct and the (1) duct drain lymph into the (2) veins. |
1) thoracic 2) subclavian |
|
|
SPECT uses a radiotracer that is administered ... |
Intravenously |
|
|
Within limits, a greater end-diastolic volume will produce a greater contractile force during systole |
Frank-Starling law of the heart |
|
|
The amount of tension generated in a cardiac chamber or vessel to produce a given internal pressure varies directly with the radius and inversely with the wall thickness |
Laplace’s law |
|
|
The amount of tension generated in a cardiac chamber or vessel to produce a given internal pressure varies directly with the radius and inversely with the wall thickness |
Laplace’s law |
|
|
Blood flow is inversely related to resistance; resistance to blood flow is directly related to vessel length and blood viscosity and inversely related to the vessel radius to the fourth power |
Poiseuille’s law |
|
|
What is the difference between primary and secondary hypertension? |
Primary: has no known cause Secondary: caused by another disease process such as renal disease |
|
|
What is the difference between myocardial hibernation and myocardial stunning? |
Hibernation: involved persistently ischemic myocardium that undergoes metabolic adaptation to survive until perfusion is restored
Stunning: involves temporary loss of contractile ability after perfusion has been restored |
|
|
What is the difference between dilated and restrictive cardiomyopathy? |
Dilated: cardiac chambers are enlarged (have increased diastolic volume), and the myocardium has decreased contractility
Restrictive: cardiac chambers have decreased diastolic volume because the myocardium is rigid and non compliant |
|
|
What is the difference between dilated and restrictive cardiomyopathy? |
Dilated: cardiac chambers are enlarged (have increased diastolic volume), and the myocardium has decreased contractility
Restrictive: cardiac chambers have decreased diastolic volume because the myocardium is rigid and non compliant |
|
|
What is the difference between valvular stenosis and valvular regurgitation? |
Stenosis: narrowing of s valve which impedes the forward flow of blood
Regurgitation: incomplete closure of a valve which allows blood to leak backward through the valve |
|
|
Distended and tortuous superficial veins in which blood has pooled because of damaged valves |
Varicose veins |
|
|
Sustained inadequate venous return due to valvular damage |
Chronic venous insufficiency |
|
|
Sustained inadequate venous return due to valvular damage |
Chronic venous insufficiency |
|
|
Ischemic pain in the lower extremities that occurs while walking but disappears when resting |
Intermittent claudication |
|
|
Sustained inadequate venous return due to valvular damage |
Chronic venous insufficiency |
|
|
Ischemic pain in the lower extremities that occurs while walking but disappears when resting |
Intermittent claudication |
|
|
Inflammatory disease of peripheral arteries that usually is associated with smoking |
Thromboangiitis obliterans |
|
|
Vasospastic disease of peripheral arteries in which episodes of ischemia and pallor are followed by rubies and parathesias |
Raynaud disease |
|
|
Inflammation of the membranous sac that surrounds the heart |
Pericarditis |
|
|
Inflammation of the membranous sac that surrounds the heart |
Pericarditis |
|
|
Compression of the heart by pericardial fluid |
Tamponade |
|
|
The term dissecting aneurysm means that blood enters an artery walk and .... |
Runs between the layers of the wall |
|
|
Risk for myocardial infarction increases with low blood levels of (1) and high blood levels of (2). |
1) HDL 2) LDL |
|
|
Cardiac valve damage in rheumatic fever is caused by what? |
An abnormal immune response |
|
|
Cardiac valve damage in infective endocarditis is caused by what? |
Streptococci or other organisms |
|
|
Constructive pericarditis is a (1) condition that can (2) the heart. |
1) chronic 2) compress |
|
|
Orthopnea, dyspnea, decreases urine output, coughing frothy pink sputum, and crackles on auscultation are signs of what sided heart failure? |
LEFT |
|
|
Orthopnea, dyspnea, decreases urine output, coughing frothy pink sputum, and crackles on auscultation are signs of what sided heart failure? |
LEFT |
|
|
Ankle edema, jugular venous distension, hepatomegaly are signs of what sided heart failure? |
RIGHT |
|
|
Low dietary intake of what electrolytes is a risk factor foR HTN? |
Potassium Magnesium |
|
|
Substance released by the kidneys that contributed to some cases of hyoertension |
Renin |
|
|
Substance released by the kidneys that contributed to some cases of hyoertension |
Renin |
|
|
A clot in a blood vessel that breaks loose and circulated is called ... |
Thromboembolus |
|
|
Sustained hypertension causes left ventricular (1) and coronary atherosclerosis, this increasing the risk for (2). |
1)hypertrophy 2) MI |
|
|
Sustained hypertension causes left ventricular (1) and coronary atherosclerosis, this increasing the risk for (2). |
1)hypertrophy 2) MI |
|
|
Rapidly progressive hypertension with a diastolic pressure above 140 is called (1) hypertension and can damage the (2). |
1) malignant 2) brain |
|
|
Postural hypotension or (1) is a systolic BP decrease of at least (2) and a diastolic BP decrease of st least (3) |
1) orthostatic 2) 20 3) 10 |
|
|
Clot formation at the site of rupture of an atherosclerotic plaque causes tissue (1) which leads to (2) if blood flow is not restored. |
1) ischemia 2) infarction |
|
|
People who are obese have decreased levels of ... an antiatherogenic adipokine |
Adiponectin |
|
|
Acute rheumatic fever is characterized by carditis, acute migratory (1), chorea, And (2) marginatum, which occur 1-5 weeks after streptococci infection of the (3). |
1) polyarthritis 2) erythema 3) pharynx |
|
|
Acute rheumatic fever is characterized by carditis, acute migratory (1), chorea, And (2) marginatum, which occur 1-5 weeks after streptococci infection of the (3). |
1) polyarthritis 2) erythema 3) pharynx |
|
|
Right atrial and right ventricular dilation And hypertrophy |
Tricuspid regurgitation |
|
|
Acute rheumatic fever is characterized by carditis, acute migratory (1), chorea, And (2) marginatum, which occur 1-5 weeks after streptococci infection of the (3). |
1) polyarthritis 2) erythema 3) pharynx |
|
|
Right atrial and right ventricular dilation And hypertrophy |
Tricuspid regurgitation |
|
|
Left atrial hypertrophy and dilation |
Mitral stenosis |
|
|
Acute rheumatic fever is characterized by carditis, acute migratory (1), chorea, And (2) marginatum, which occur 1-5 weeks after streptococci infection of the (3). |
1) polyarthritis 2) erythema 3) pharynx |
|
|
Right atrial and right ventricular dilation And hypertrophy |
Tricuspid regurgitation |
|
|
Left atrial hypertrophy and dilation |
Mitral stenosis |
|
|
Left ventricular hypertrophy and dilation |
Aortic stenosis |
|
|
Acute rheumatic fever is characterized by carditis, acute migratory (1), chorea, And (2) marginatum, which occur 1-5 weeks after streptococci infection of the (3). |
1) polyarthritis 2) erythema 3) pharynx |
|
|
Right atrial and right ventricular dilation And hypertrophy |
Tricuspid regurgitation |
|
|
Left atrial hypertrophy and dilation |
Mitral stenosis |
|
|
Left ventricular hypertrophy and dilation |
Aortic stenosis |
|
|
Left atrial and left ventricular dilation and hypertrophy |
Mitral regurgitation |
|

|
Tetralogy of Fallot Right to left shunt |
|

Front (Term) |
Aortic stenosis No shunt |
|

Front (Term) |
Atrial septal defect Left to right shunt |
|

Front (Term) |
Atrial septal defect Left to right shunt |
|

Front (Term) |
Coarctation of the aorta No shunt |
|

Front (Term) |
Tricuspid atresia Right to left |
|
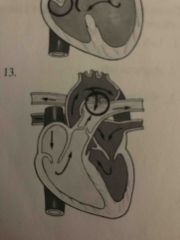
Front (Term) |
Patent ductus arteriosus Left to right shunt |
|

Front (Term) |
Ventricular septal defect Left to right shunt |
|

Front (Term) |
Ventricular septal defect Left to right shunt |
|

Front (Term) |
Pulmonic stenosis No shunt |
|
|
Fetal oxygenation occurs in the ... |
Placenta |
|
|
Fetal oxygenation occurs in the ... |
Placenta |
|
|
Pulmonary overcirculation caused by an uncorrected congenital heart defect causes the smooth muscle layer in the pulmonary arterial tree to (1) and the lumens to (2). |
1) thicken 2) narrow |
|
|
Fetal oxygenation occurs in the ... |
Placenta |
|
|
Pulmonary overcirculation caused by an uncorrected congenital heart defect causes the smooth muscle layer in the pulmonary arterial tree to (1) and the lumens to (2). |
1) thicken 2) narrow |
|
|
Failure of the endocardi cushions to fuse during fetal life causes an (1) canal defect and frequently occurs in children who have (2) syndrome |
1) atrioventricular 2) down |
|
|
Underdevelopment of the left heart is termed ... left heart syndrome |
Hypoplastic |
|
|
Underdevelopment of the left heart is termed ... left heart syndrome |
Hypoplastic |
|
|
With transposition of the great arteries, the aorta arises from the (1) ventricle and the pulmonary artery arises from the (2) ventricle; unless additional defects are present this defect is incompatible with (3) life |
1) right 2) left 3) extrauterine |
|
|
The condition in which the pulmonary artery and the aorta are a single blood vessel is called .... |
Truncus arteriosus |
|
|
The condition in which the pulmonary artery and the aorta are a single blood vessel is called .... |
Truncus arteriosus |
|
|
Young children who develop (1) disease have vasculitis of unknown cause and often develop aneurysms of their (2) arteries that may regress as the condition resolves. |
1) Kawasaki 2) coronary |
|
|
Sustained hypertension in children often is associated with underlying ... disease |
Renal |
|
|
What is the difference between the direction of blood flow through the ductus arteriosus in fetal life and after birth if the ductus arteriosus does not close? Why does this difference occur? |

Back (Definition) |
|
|
What is the difference between the direction of blood flow through the ductus arteriosus in fetal life and after birth if the ductus arteriosus does not close? Why does this difference occur? |

Back (Definition) |
|
|
What is the difference between the clinical manifestations of s congenital heart defect that causes a moderate right to left blood shunt and one that causes a moderate left to right blood shunt? Why does this difference occur? |

Back (Definition) |
|
|
Prevent airway collpse |
Cartilage rings |
|
|
Prevent airway collpse |
Cartilage rings |
|
|
Filter and humidify air |
Nasopharynx |
|
|
Prevent lung collapse at end-exhalation |
Surfactant |
|
|
Prevent lung collapse at end-exhalation |
Surfactant |
|
|
Allow pressure to equalize between adjacent alveoli |
Pores of Kohn |
|
|
The pulmonary circulation has ... pressure and resistance than the systemic circulation |
Lower |
|
|
What is the most effective measurement of of the adequacy of alveolar ventilation? |
PaCO2 |
|
|
Parasympathetic stimulation causes airways to (1); sympathetic stimulation causes airways to (2). |
1) constrict 2) dilate |
|
|
Parasympathetic stimulation causes airways to (1); sympathetic stimulation causes airways to (2). |
1) constrict 2) dilate |
|
|
What intercostal muscles are active during vigorous inspiration? |
External |
|
|
A person at sea level breathing through the nose the gas that reaches the lungs if ... Saturated with water vapor |
Fully |
|
|
The shift in the oxyhemoglobin dissociation curve caused by alterations in pH and PaCO2 is called the ... effect |
Bohr |
|
|
What is the difference between a terminal bronchioles and a respiratory bronchioles? |
Terminal: a conducting airway
Respiratory: a gas-exchange airway |
|
|
What is the difference between type I️ and type IIalveolar cells |
Type I️ provide the structure of alveoli
Type II SECRETE SURFACTANT |
|
|
What is the difference between the visceral pleura and the parietal pleura? |
Visceral: covers the lungs
Parietal: lines the thoracic cavity |
|
|
What is the difference between the visceral pleura and the parietal pleura? |
Visceral: covers the lungs
Parietal: lines the thoracic cavity |
|
|
What is the difference between PaO2 and PAO2? |
PaO2 is the parietal pressure of oxygen in the arterial blood
PAO2 is the partial pressure of oxygen in the alveoli |
|
|
The mononuclear phagocytic cells in the lungs are called alveolar ... |
Macrophages |
|
|
Gas exchange occurs across the ... membrane |
Alveolocapillary |
|
|
Receptors in The conducting airways that initiate the cough reflex in response to inhaled dust are called ... receptors. |
Irritant |
|
|
The V/Q ratio of s normal upright lung is ... |
0.8 |
|
|
The V/Q ratio of s normal upright lung is ... |
0.8 |
|
|
A normal V/Q ratio indicates that ventilation is ... than perfusion |
Less |
|
|
Perfusion is greater than ventilation because pulmonary arterial and venous pressures are greater than alveolar pressure |
Zone III |
|
|
Perfusion is greater than ventilation because pulmonary arterial and venous pressures are greater than alveolar pressure |
Zone III |
|
|
Perfusion happening but is not maximum because pulmonary arterial and venous pressures are opposed by alveolar pressure |
Zone II |
|
|
Perfusion is greater than ventilation because pulmonary arterial and venous pressures are greater than alveolar pressure |
Zone III |
|
|
Perfusion happening but is not maximum because pulmonary arterial and venous pressures are opposed by alveolar pressure |
Zone II |
|
|
No perfusion occurs because alveolar pressure is greater than pulmonary arterial and venous pressures |
Zone I |
|
|
Hemoglobin molecules that have bound oxygen |
Oxyhemoglobin |
|
|
Hemoglobin molecules that have bound oxygen |
Oxyhemoglobin |
|
|
The conducting airways of the lungs |
Bronchi |
|
|
Hemoglobin molecules that have bound oxygen |
Oxyhemoglobin |
|
|
The conducting airways of the lungs |
Bronchi |
|
|
What goblet cells in the bronchi secrete |
Mucus |
|
|
Hemoglobin molecules that have bound oxygen |
Oxyhemoglobin |
|
|
The conducting airways of the lungs |
Bronchi |
|
|
What goblet cells in the bronchi secrete |
Mucus |
|
|
Space between the lungs that contains the heart, great vessels, and esophagus |
Mediastinum |
|
|
Where the trachea divides into the two main bronchi |
Carina |
|
|
Fibers that give lung tissue it’s elasticity |
Elastin |
|
|
Structure that connects the larynx to the bronchi |
Trachea |
|
|
Structure that connects the upper and lower airways |
Larynx |
|
|
Where the bronchi and pulmonary vessels enter the lungs |
Hila |
|
|
The structures that participate in gas exchange |
Acines |
|
|
Presence of pus in the pleural cavity |
Empyema |
|
|
Presence of pus in the pleural cavity |
Empyema |
|
|
Collapse of alveoli |
Atelectasis |
|
|
Presence of pus in the pleural cavity |
Empyema |
|
|
Collapse of alveoli |
Atelectasis |
|
|
Bluish discoloration is the skin caused by desaturation of hemoglobin |
Cyanosis |
|
|
Presence of pus in the pleural cavity |
Empyema |
|
|
Collapse of alveoli |
Atelectasis |
|
|
Bluish discoloration is the skin caused by desaturation of hemoglobin |
Cyanosis |
|
|
PaO2 below normal |
Hypoxemia |
|
|
Presence of pus in the pleural cavity |
Empyema |
|
|
Collapse of alveoli |
Atelectasis |
|
|
Bluish discoloration is the skin caused by desaturation of hemoglobin |
Cyanosis |
|
|
PaO2 below normal |
Hypoxemia |
|
|
Coughing up blood mucus |
Hemoptysis |
|
|
Presence of pus in the pleural cavity |
Empyema |
|
|
Collapse of alveoli |
Atelectasis |
|
|
Bluish discoloration is the skin caused by desaturation of hemoglobin |
Cyanosis |
|
|
PaO2 below normal |
Hypoxemia |
|
|
Coughing up blood mucus |
Hemoptysis |
|
|
Passage of fluid and:or solid particles into the lungs |
Aspiration |
|
|
Processes that increase capillary permeability can cause (1) pleural effusion, but processes that increase capillary hydrostatic pressure can cause (2) pleural effusion |
1) exudative 2) transudative |
|
|
Clinical manifestations of bronchiolitis include tachyons, (1) cough, use of accessory muscles, (2) fever, and hypoxemia. |
1) nonproductive 2) low-grade |
|
|
Clinical manifestations of bronchiolitis include tachyons, (1) cough, use of accessory muscles, (2) fever, and hypoxemia. |
1) nonproductive 2) low-grade |
|
|
What type of ventilation is caused by head injury, anxiety, and response to severe hypoxemia? |
HypERventilation |
|
|
Clinical manifestations of bronchiolitis include tachyons, (1) cough, use of accessory muscles, (2) fever, and hypoxemia. |
1) nonproductive 2) low-grade |
|
|
What type of ventilation is caused by head injury, anxiety, and response to severe hypoxemia? |
HypERventilation |
|
|
What type of ventilation is caused by airway obstruction, reduces firing of neurons to respiratory muscles, respiratory muscle weakness, and reduced compliance of chest wall? |
HypOventilation |
|
|
What is the difference between dyspnea and orthopnea? |
Dyspnea: feeling of breathlessness
Orthopnea: feeling of breathlessness while lying down |
|
|
What is the difference between stridor and wheezing? |
Stridor: high-pitched sounds made during inspiration
Wheezing: whistling sounds on expiration |
|
|
What is the difference between absorption atelectasis and compression atelectasis? |
Absorption: alveolar collapse caused by gases being absorbed from alveoli that are obstructed
Compression: alveolar collapse caused by external pressure on the alveoli |
|
|
What is the difference between communicating and tension pneumothorax? |
Communicating: the pressure of the air in the pleural space is the same as barometric pressure because the air drawn into the pleural space during inspiration is forced back out during expiration
Tension: the pressure of air In The pleural space exceeds barometric pressure because air enters during inspiration but cannot exit during expiration |
|
|
Alternating periods of deep and shallow breathing with apnea episodes |
Cheyne-Stokes |
|
|
Alternating periods of deep and shallow breathing with apnea episodes |
Cheyne-Stokes |
|
|
What breathing pattern exhibits: Increased ventilator rate, small tidal volume |
Restricted |
|
|
Alternating periods of deep and shallow breathing with apnea episodes |
Cheyne-Stokes |
|
|
What breathing pattern exhibits: Increased ventilator rate, small tidal volume |
Restricted |
|
|
What breathing pattern exhibits: rhythmic and effortless with normal tidal volume |
Eupnea |
|
|
Alternating periods of deep and shallow breathing with apnea episodes |
Cheyne-Stokes |
|
|
What breathing pattern exhibits: Increased ventilator rate, small tidal volume |
Restricted |
|
|
What breathing pattern exhibits: rhythmic and effortless with normal tidal volume |
Eupnea |
|
|
What breathing pattern exhibits: irregular quick inspirations with an exploratory pause |
Gasping |
|
|
Alternating periods of deep and shallow breathing with apnea episodes |
Cheyne-Stokes |
|
|
What breathing pattern exhibits: Increased ventilator rate, small tidal volume |
Restricted |
|
|
What breathing pattern exhibits: rhythmic and effortless with normal tidal volume |
Eupnea |
|
|
What breathing pattern exhibits: irregular quick inspirations with an exploratory pause |
Gasping |
|
|
What breathing pattern exhibits: increased ventilator rate, small tidal volume, increased effort, prolonged expiration, and wheezing |
Obstructed |
|
|
What breathing pattern exhibits: increased ventilator rate, very large tidal Volume, and no expiration pause |
Kussmaul |
|
|
Waking up with dyspnea during the night and needing to sit upright or stand to breathe is called ... |
Paroxysmal nocturnal dyspnea |
|
|
Waking up with dyspnea during the night and needing to sit upright or stand to breathe is called ... |
Paroxysmal nocturnal dyspnea |
|
|
A person who has (1) has persistent abnormal filations if the bronchi and a chronic cough that produces large amount of purulent (2). |
1) bronchiectasis 2) sputum |
|
|
Pulmonary fibrosis is an excessive amount of (1) tissue in the lungs and causes (2) lung compliance |
1) fibrotic 2) decreased |
|
|
In asthma, long term airway damage that is irreversible is known as airway ... |
Remodeling |
|
|
Genetic deficiency of (1) causes early-onset emphysema because this enzyme normally inhibits the action of (2) that can destroy lung tissue. |
1) A1 anti-trypsin 2) protolytic enzymes |
|
|
The two disorders known as COPD are emphysema and ... |
Chronic bronchitis |
|
|
The two disorders known as COPD are emphysema and ... |
Chronic bronchitis |
|
|
Chronic bronchitis is characterized by persistent hypersecretion if (1) and chronic (2) cough |
1) mucus 2) productive |
|
|
Clinical manifestations of emphysema include (1) chest and (2) on exertion and eventually at rest. |
1) barrel 2) dyspnea |
|
|
Cot pulmonary is (1) ventricular enlargement caused by chronic pulmonary (2) |
1) RIGHT 2) HTN |
|
|
Cot pulmonary is (1) ventricular enlargement caused by chronic pulmonary (2) |
1) RIGHT 2) HTN |
|
|
Primary lung cancer arising from cells that line the airways is called ... |
Bronchogenic carcinoma |
|
|
Small cell carcinoma in the lung often produces tumor-derived ... |
Hormones |
|
|
Infection and inflammation in the terminal airways and alveoli |
Pneumonia |
|
|
Congenital lack of patency of the nasal cavity within the nasopharynx |
Choanal atresia |
|
|
Congenital lack of patency of the nasal cavity within the nasopharynx |
Choanal atresia |
|
|
Harsh vibratory sound with variable pitch caused by turbulent air flow through a partially obstructed upper airway |
Stridor |
|
|
Localized swelling involving the deep subcutaneous tissue |
Angioedema |
|
|
Compared with older children, a 2-week-old neonate has a blunted ventilatory response to ... |
Hypoxia |
|
|
Acute epiglottitis usually is a (1) infection and tends to occur in children aged (2) years. |
1) bacterial 2) 2-6 |
|
|
Peritonsillar abcess usually is (1) And is a complication of (2). |
1) unilateral 2) tonsillitis |
|
|
Pneumonia in young children is usually a ... infection. |
Viral |
|
|
Pneumonia caused by mycoplasma is known as (1) pneumonia and usually is (2) severe. |
1) atypical 2) not |
|
|
ARDS (1) ALI and is characterized by (2) respiratory distress and severe (3) that is poorly responsive to supplemental oxygen. |
1) follow 2) progressive 3) hypoxemia |
|
|
Acute laryngotracheobronchitis is another name for ... |
Croup |
|
|
Croup is usually caused by a (1) that causes (2) edema. |
1) virus 2) subglottal |
|
|
The most common predisposing factor for childhood OSA is ... hypertrophy. |
Adenotonsillar |
|
|
RDS of the newborn is caused by (1) deficiency; fibrin deposits in the alveoli create the appearance of (2) membranes. |
1) surfactant 2) hyaline |
|
|
Chronic lung disease of prematurity , also called (1), is associated with arrested lung (2). |
1) bronchopulmonary dysplasia 2) development |
|
|
Bronchiolitis is most commonly caused by ... |
Respiratory synctial virus |
|
|
Bronchiolitis is most commonly caused by ... |
Respiratory synctial virus |
|
|
RSV symptoms include (1), cough, and (2) respiratory rate. |
1) rhinorrhea 2) increased |
|
|
Meconium aspiration causes pneumonitis because the ... in meconium causes inflammation |
Bile salts |
|
|
The ... hypothesis attempts to explain the Hugh prevalence of asthma in westernized cultures. |
Hygiene |
|
|
What is the difference between principal cells and the intercalated cells in the collecting duct? |
Principal cells: secrete potassium and reabsorb sodium and water
Intercalated cells: reabsorb potassium and secrete hydrogen ions |
|
|
What is the difference between principal cells and the intercalated cells in the collecting duct? |
Principal cells: secrete potassium and reabsorb sodium and water
Intercalated cells: reabsorb potassium and secrete hydrogen ions |
|
|
What is the difference between tubular secretion and tubular reabsorption? |
Secretion: moves substances from the peritubular capillaries into the renal tubular lumen
Reabsorption: moves them from the renal tubular lumen into the peritubular capillaries |
|
|
The area of the bladder between the openings of the ureters and the urethra |
Trigone |
|
|
The bladder wall muscle |
Detrusor |
|
|
Precipitated material in urine that increase as urine cools |
Crystals |
|
|
Precipitated material in urine that increase as urine cools |
Crystals |
|
|
All the glomeruli are located in the renal ... |
Cortex |
|
|
Precipitated material in urine that increase as urine cools |
Crystals |
|
|
All the glomeruli are located in the renal ... |
Cortex |
|
|
Small openings in the glomerular endothelium called (1) are maintained by vascular endothelial growth factor secreted by the (2). |
1) fenestrae 2) podocytes |
|
|
Natriuretic peptides ... renal excretion of sodium and water |
Increases |
|
|
Natriuretic peptides ... renal excretion of sodium and water |
Increases |
|
|
ADH (1) renal excretion of water which (2) urine specific gravity. |
1) decreases 2) increases |
|
|
Tamm-Horsfall protein, also known as (1), is produced in the (2) nephron segments and protects against (3). |
1) uromedulin 2) distal 3) bacteria |
|
|
The concentration gradient of the renal interstitium (1) from the cortex to the tip of the medulla; the gradient is necessary in order to (2) the urine. |
1) increases 2) concentrate |
|
|
The concentration gradient of the renal interstitium (1) from the cortex to the tip of the medulla; the gradient is necessary in order to (2) the urine. |
1) increases 2) concentrate |
|
|
The countercurrent exchange system is composed of the (1) and its function requires that the fluid within move (2). |
1) vasa recta 2) slowly |
|
|
The kidneys (1) vitamin D, a process that is stimulated by (2). |
1) activate 2) parathyroid hormone |
|
|
Creatinine clearance is used to estimate ... |
GFR |
|
|
Creatinine clearance is used to estimate ... |
GFR |
|
|
Para-aminohiopuric acid clearance is used to estimate ... |
Renal blood flow |
|
|
The glomeruli, most of the proximal tubules, glomerular capillaries, renal corpuscles, interlobular arteries, and affirmed arterioles are located where in the kidney? |
Cortex |
|
|
The collecting ducts, most of the distal tubules, pyramids, and most of the vasa recta are located where in the kidney? |
Medulla |
|
|
What portion of the nephron: reabsorption of large amounts of sodium, water, glucose, amino acids; net reabsorption of bicarbonate; secretion if H+, organic acids, and many medications |
Proximal tubule |
|
|
What part of the nephron is responsible for: Reabsorption of sodium, chloride, and potassium but not much water |
Thick ascending limb of loop of henle |
|
|
What part of the nephron is responsible for: Reabsorption of sodium, chloride, and potassium but not much water |
Thick ascending limb of loop of henle |
|
|
What part of the nephron is responsible for: secretion of potassium, ammonia, and H+; site of action of aldosterone and ADH |
Distal tubule and collecting duct |
|
|
What part of the nephron is responsible for: Reabsorption of sodium, chloride, and potassium but not much water |
Thick ascending limb of loop of henle |
|
|
What part of the nephron is responsible for: secretion of potassium, ammonia, and H+; site of action of aldosterone and ADH |
Distal tubule and collecting duct |
|
|
What part of the nephron is responsible for: ultrafiltration |
Glomerulus |
|
|
What part of the nephron is responsible for: Reabsorption of sodium, chloride, and potassium but not much water |
Thick ascending limb of loop of henle |
|
|
What part of the nephron is responsible for: secretion of potassium, ammonia, and H+; site of action of aldosterone and ADH |
Distal tubule and collecting duct |
|
|
What part of the nephron is responsible for: ultrafiltration |
Glomerulus |
|
|
What part of the nephron is responsible for: reabsorption of water |
Descending limb of loop of henle |
|
|
A process that regulates sodium and water balance by reabsorption of a constant fraction of the sodium load filtered at the glomerulus |
Glomerulotubular balance |
|
|
A process that regulates sodium and water balance by reabsorption of a constant fraction of the sodium load filtered at the glomerulus |
Glomerulotubular balance |
|
|
42- |
Myogenic mechanism |
|
|
A process that regulates sodium and water balance by reabsorption of a constant fraction of the sodium load filtered at the glomerulus |
Glomerulotubular balance |
|

42- |
Myogenic mechanism |
|

43- |
Tubuloglomerular feedback |
|
|
The location where the renal blood vessels, nerves, lymphatics, and ureter enter and exit the kidney is called the ... |
Hilum |
|
|
The epithelial cells of the proximal convoluted tubule are the only renal tubular cells that have ... |
Microvilli |
|
|
The epithelial cells of the proximal convoluted tubule are the only renal tubular cells that have ... |
Microvilli |
|
|
The (1) is the functional unit of the kidney; the (2) ones are highly important for concentrating urine. |
1) nephron 2) juxtamedullary (as in nephrons) |
|
|
Glomerular capillary blood flow is regulated in part by the contractile ... cells and by vasoactive substances secreted by the endothelium. |
Mesangial |
|
|
The filtration fraction is the ratio of the glomerular filtration rate to ... |
Renal plasma flow |
|
|
Renal arterioles are inner ages by (1) nerves; increased firing causes the arterioles to (2). |
1) sympathetic 2) constrict |
|
|
The renal hormone ... degrades catecholamines |
Renalase |
|
|
The term ... refers to how much of a substance can be removed from the blood by the kidneys per a unit of time. |
Clearance |
|
|
Plasma creatinine concentration takes 7-10 days to stabilize and is best for monitoring ... renal disease |
Chronic |
|
|
Plasma creatinine concentration takes 7-10 days to stabilize and is best for monitoring ... renal disease |
Chronic |
|
|
BUN (1) when GFR decreases, but can also vary with dehydration, protein intake, and protein (2), which can make it unreliable for monitoring renal function. |
1) increases 2) catabolism |
|
|
What is the difference between hypospadias and epispadias in males? |
Hypospadias: urethral meatus is located on the central side of the penis
Epispadias: meatus located on the dorsal side of the penis |
|
|
What is the difference between a hypoplastic and dysplastic kidney? |
Hypoplastic: small but otherwise normal
Dysplastic: contains abnormal tissue |
|
|
What is the difference between a hypoplastic and dysplastic kidney? |
Hypoplastic: small but otherwise normal
Dysplastic: contains abnormal tissue |
|
|
What is the difference between primary and secondary incontinence? |
Primary: occurs when a child has not developed bladder control beyond the age at which it is usually achieved
Secondary: occurs in a child who has been dry for at least 6 months and then becomes incontinent again |
|
|
When kidneys fuse in the midline as they ascend during development, the U-shaped kidney is called a ... kidney. |
Horseshoe |
|
|
When kidneys fuse in the midline as they ascend during development, the U-shaped kidney is called a ... kidney. |
Horseshoe |
|
|
Failure of the abdominal muscles and anterior bladder to fuse in the midline with subsequent exposure of the posterior bladder mucosa is called ... of the bladder. |
Extrophy |
|
|
Blockage of the tapered point where the renal pelvis transitions into the ureter is called (1) instruction and causes (2) in neonates. |
1) ureteropelvic junction 2) hydronephrosis |
|
|
Blockage of the tapered point where the renal pelvis transitions into the ureter is called (1) instruction and causes (2) in neonates. |
1) ureteropelvic junction 2) hydronephrosis |
|
|
When a kidney contains both renal and nonrenal tissues the condition is called renal ... |
Dysplasia |
|
|
Blockage of the tapered point where the renal pelvis transitions into the ureter is called (1) instruction and causes (2) in neonates. |
1) ureteropelvic junction 2) hydronephrosis |
|
|
When a kidney contains both renal and nonrenal tissues the condition is called renal ... |
Dysplasia |
|
|
Autosomal dominant polycystic kidney disease arises from mutations of a gene that produces ... |
Polycystins |
|
|
Another name for a Wilms rumor is (1), a rumor if the (2) that usually presents as an enlarging, firm, nontender smooth mass on one side of the (3). |
1) nephroblastoma 2) kidney 3) abdomen |
|
|
Nephrotic syndrome is characterized by proteinuria, (1), hyperlipidemia, And (2), which is often (3) in the morning and more evident in the abdomen and lower extremities in the day. |
1) hypoalbuminemia 2) edema 3) periorbitAl |
|
|
Nephrotic syndrome is characterized by proteinuria, (1), hyperlipidemia, And (2), which is often (3) in the morning and more evident in the abdomen and lower extremities in the day. |
1) hypoalbuminemia 2) edema 3) periorbitAl |
|
|
The most common histopathology pattern of nephrotic syndrome in children is ... |
Minimal change nephropathy |

