![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
42 Cards in this Set
- Front
- Back
|
Labile Cells
|
Continuously Dividing Cells (Hematopoietic cells, surface epithelia)
|
|
|
Stable Tissues (Quiescent)
|
Minimal replicative activity; Parenchyma of most solid organs (liver, kidney, pancreas) also endothelial cells, fibroblasts, smooth muscle cells
|
|
|
Permanent tissues
|
Non-proliferative (Neurons, cardiac muscle cells)
|
|
|
Hypertrophy
|
Increase in SIZE of cells (increased amounts of proteins and organelles by trophic (growth factors) or mechanical triggers to cell.
|
|
|
Physiologic Hypertrophy
|
Increased functional demand or hormonal stimulation ex) skeletal muscle hypertrophy in weight lifting athlete and uterus in pregnancy
|
|
|
Pathologic hypertrophy
|
Cardiac muscle hypertrophy seen in hypertension
|
|
|
Hyperplasia
|
Increase in cell NUMBER; occurs in cells capable of division (labile and stable cells)
|
|
|
Physiologic Hyperplasia examples
|
Hormonal hyperplasia of female breast at puberty and in pregnancy; Compensatory hyperplasia of liver after partial resection
|
|
|
Pathologic hyperplasia examples
|
Excessive stimulation by growth factors or hormones; reversible; ex) Hormonal imbalance stimulates endometrial hyperplasia
|
|
|
Benign Prostatic Hyperplasia
|
Very common in men >50 years old; nodule formation in prostate gland; mech-androgen-induced release of growth factors
|
|
|
Is enlargement of the uterus during pregnancy hyperplasia or hypertrophy?
|
both
|
|
|
Atrophy
|
Decrease in size of a cell due to loss of cell substance; If severe there is a decrease in organ size; physiologic-loss of hormonal stimulation; pathologic-decreased functional demand, loss of innervation, inadequate nutrition
|
|
|
Metaplasia
|
One adult cell type is replace by another cell type (that is better able to handle the stress); cells are reprogrammed; reversible (but may be associated with cancer)
|
|
|
Epithelial metaplasia
|
Ciliated columnar epithelium becomes squamous epithelium (trachea of smokers); Squamous epithelium becomes gastric/intestinal type epithelium (esophagus in acid reflux)
|
|
|
Mesenchymal metaplasia
|
Bone formation in soft tissue (muscle/connective tissue) at sites of injury
|
|
|
Barrett Esophagus
|
Squamous epithelium becomes glandular epithelium which protects against reflux of stomach acid (predisposes to development of glandular carcinoma
|
|
|
Squamous Metaplasia Endocervix
|
Columnar becomes squamous and increases risk of HPV infection
|
|
|
Hypoxia
|
Inadequate oxygenation of blood (lung disease, lack of oxygen in ambient air); Reduced oxygen-carrying capacity of blood (ex. anemia cyanide)
|
|
|
Ischemia
|
Lack of blood supply to site
|
|
|
Necrosis
|
Breakdown of plasma membrane, organelles, and nucleus; leakage of contents (irreversible); adjacent inflammation; invariable pathologic; increased eosinophilia
|
|
|
Apoptosis
|
Cellular fragmentation, apoptotic body; phagocytosis of apoptotic cells and fragments; Shrinkage; plasma membrane intact but altered; no inflammation; often physiologic; may be pathologic; eosinophilic cytoplasm; condensed nucleus
|
|
|
Order of Cell Injury
|
Reversible-->Irreversible-cell death, ultrastructural changes, light microscopic changes, gross morphologic changes
|
|
|
Morphology of reversible cell injury
|
Fatty change-Lipid vacuoles in cytoplasm- occurs with toxic and hypoxic injury, ex) fatty liver secondary to toxins; Cellular swelling-hydropic change or vacuolar degeneration-failure of membrane pumps (membrane blebs); vacuoles appear in cells corresponding to distended endoplasmic reticulum
|
|
|
Why can a liver become fatty?
|
Impairment of microsomal and mitochondrial functions; decreased fatty acid oxidation, decreased apoprotein formation increased mobilization of fatty acids from periphery
|
|
|
Coagulative Necrosis
|
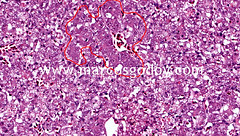
Results from hypoxic or anoxic injury due to ischemia (infarct); persistence of dead cells with intact outlines but has loss of cellular details particulary nuclei; OCCURS IN ALL SOLID ORGANS (except for the brain); denautes both cellular proteins and enzymes
|
|
|
Liquefactive Necrosis
|
Complete digestion of the dead cells; Tissue is semi-liquid as it has been dissolved by hydrolytic enzymes; commonly seen with bacterial and fungal infections; WBC's release digestive enzymes; BRAIN infarcts result in this kind of necrosis
|
|
|
Caseous Necrosis
|
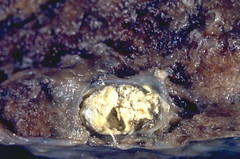
Characteristic of tuberculous infection; resembles cheese; NO cell outlines; usually surrounded by a border of inflammatory cells forming a distinctive pattern (granuloma)
|
|
|
Gangrenous Necrosis
|
Term used for ischemic coagulative necros of lower or upper extremity; wet if bacterial infxn is also present
|
|
|
Fat Necrosis
|
Seen in the pancreas in acute pancreatitis; injury releases lipase which liquefies fat and splits triglycerides; combine with calcium to form chalky white material; can also occur w/ trauma to fatty tissue
|
|
|
Fibrinoid Necrosis
|
Deposition of immune complexes (antigens and antibodies) in vascular wall; Fibrin-like (bright pink appearance); Occurs in vasculitis syndromes
|
|
|
List the specific cellular mechanisms of injury
|
Mitochondria (depletion of ATP and incr. or ROS)
Intracellular entry of calcium (membrane damage, nuclear damage, decre. ATP) Cellular membranes (increase permeability DNA and cellular proteins (damage to DNA, protein misfolding) |
|
|
Does ichemia or hypoxia injure tissues faster?
|
Ischemia because in hypoxia anaerobic glycolysis continues; skeletal muscle dies in 2-3 hours, cardiac 20-30 min
|
|
|
Reperfusion Injury
|
Restoration to ischemic tissue may increase cell injury (mainly in brain and heart); Increased fee radical generation; Increased leukocytes, plasma proteins, and complement (inflammation)
|
|
|
Lipofuscin in heart muscle
|
Indigestible material resulting from lipid peroxidation; "wear and tear" pigment, occurs predominantly with aging; particularly in heart, liver, and brain
|
|
|
Tay-Sachs Disease
|
Abnormal metabolism-increased production of normal substance (gangliosides) because of lack of enzyme to degrade it (lysosomal storage disease)
|
|
|
Anthracosis in lung
|
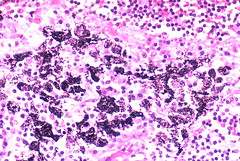
Inhaled in air, phagocytosed by alveolar macrophages, transported to regional lymph nodes
|
|
|
Hypertrophy of Smooth ER in liver
|
adaptive response to barbiturates and alcohol in hepatocytes (to maximize toxin removal)
|
|
|
Cytoskeleton abnormalities
|
accumulations w/ alzheimer's disease; abnormal organization of microtubules; Kartagener syndrome: immotile cilia: sterility and lung infections
|
|
|
Hemosiderin
|
hemoglobin derived pigment containing iron; usually occurs where there has been hemorrhage; found in liver, bone marrow, spleen, lymph nodes
|
|
|
Dystrophic Calcification
|
Non-viable damaged or dying tissues; normal serum calcium; ex) atheromas, aortic valves in elderly
|
|
|
Metastatic Calcification
|
Normal tissues; Hypercalcemia; increased PTH, destruction of bone, Vit D intoxication, Renal failure
|
|
|
Decreased cellular replication
|
Progressive shortening of telomeres or lack of telomers
|

