![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
150 Cards in this Set
- Front
- Back
|
Each receptor cell monitors |
A specific area known as a receptive field |
|
|
Referred pain |
Sensors originating in visceral organs are perceived as pain in other body regions innervated by the same spinal nerves |
|
|
Tactile receptor |
A sensory nerve ending that responds to various stimuli including light and touch |
|
|
What are the 6 tactile receptors |
Free nerve endings A root hair plexus Merkels disks and cells Meissners corpuscle Lamellated corpuscle A Ruffini corpuscle |
|
|
Baroreceptors....their 4 locations and purposes |
Sensors located in blood vessels that sense blood pressure and relay info to the brain so that a proper blood pressure can be maintained. Also are located in the digestive tract to trigger reflex movement of materials along the tract Also located in the bladder wall to provide info on volume and trigger urinary reflex Also located in the lungs to monitor respiratory rate and stretching |
|
|
Chemoreceptors |
A sensory receptor that transducer a chemical signal into an action potential. Detects chemical stimuli in the env. 2 classes: Direct: taste buds Distance: olfactory |
|
|
Olfactory receptor |
A modified neuron with multiple cilia extending from its free surface. Cilia detect smell -> olfactory cell -> olfactory nerve fibers -> olfactory bulb |
|
|
Regenerative basal cell |
Divides to replace worn out olfactory receptor cells |
|
|
Olfactory epithelium |
Contains olfactory receptor cells and olfactory glands |
|
|
Gustatory receptors |
Detects taste. Inside taste buds which form pockets along the sides of epithelial projections called papillae |
|
|
Pupillary muscles |
Two sets of intrinsic smooth muscle within the iris control the diameter of the pupil. Bright light concentric muscles contract to reduce the level of incoming light. Dim light: radial muscles contract to dilate the pupil |
|
|
Aqueous humor |
Secreted by the ciliary body circulates through the posterior and anterior chambers. Lens position maintained by suspensory ligaments |
|
|
The closer the light source |
The longer the focal distance |
|
|
The rounder the lens |
The shorter the focal distance |
|
|
What eye muscle contracts or relaxrs to control distance |
Ciliary muscle Contract = lens rounds = close vision Relax = lens flattens = distant vision |
|
|
What affects focal distance |
Location of light source. Lens shape |
|
|
Image formation |
Light from each portion of an object is focused on a different part of the retina. The resulting image is upside down and backwards |
|
|
Rods and cones |
The shapes of the photoreceptors outer segment. Their membrane discs contain the visual pigments, which are derived from rhodopsin molecules |
|
|
Movement of light in the eye |
Light - bipolar cell - cone/rod in inner segment - discs with visual pigment in outer segment to pigment epithelium |
|
|
Visual association areas |
In the cerebrum integrate the visual information to develop a composite picture of the entire visual field. Eye - optic nerve - brain |
|
|
Otolith in the ear |
In the inner ear vestibular complex. Sensitive to gravity and linear acceleration because their orientation in the head makes it sensitive to change in horizontal movement. When the otolith moves, it distorts hair cell processes and receptor output increases |
|
|
Cochlea |
The sense organ in the inner ear that translates sound to nerve impulses to be sent to the brain. Fluid filled and snail shaped cavern |
|
|
6 steps in sound reception |
1. Waves arrive at tympanic membrane 2. Movement of tympanic membrane moves auditory ossicles 3. Movement of staples at oval window makes pressure waves in vestibular duct 4. Pressure waves distort basilar membrane 5. Causes vibration or hair cells against tectorial membrane. 6. Info relayed to cns over the cochlear branch of cranial nerve |
|
|
Midbrain |
Directs unconscious motor response to sounds |
|
|
Functions of the digestive system |
Ingestion, mechanical processing, digestion, secretion, absorption, excretion, defense |
|
|
Salivary glands |
Secretion of lubricating fluid containing enzymes that break down carbs |
|
|
Pharynx |
Muscular propulsion of materials into the esophagus |
|
|
Oral cavity Stomach |
Oral: mechanical processing. Stomach: chemical breakdown and mechanical processing |
|
|
Small intestine |
Enzymatic digestion and absorption of water, organic substrates, vitamins, and ions. |
|
|
Large intestine |
Dehydration and compaction of undigestible materials in preparation for elimination. |
|
|
Pancreas. |
Exocrine cells secreted buffers and digestive enzymes. Endocrine cells secrete hormones |
|
|
Gallbladder |
Storage and concentration of bile |
|
|
Liver |
Secretion of bile for lipid digestion, storage of nutrients , other vital functions |
|
|
4 layers of digestive tract |
Mucosa: folds, epithelium Submucosa: loose connective tissue and blood and lymph vessels and nerves Muscularis externa: smooth muscle cells...contractions Serosa: outer membrane |
|
|
Mucosa |
Has folds that increase surface area for absorption and permit expansion after a large meal. Has villi in small intestine. Has an epithelium ( moistened by glandular secretions) and loose connective tissue |
|
|
Simple epithelia |
Single layer of cells |
|
|
Stratified epithelium |
Multiple layers of cells. Specialized depending on the location and function |
|
|
Squamous |
Flat. Alveoli and lining of esophagus |
|
|
Columnar |
Column shaped Linings of pharynx, anus, uterus, urethra. |
|
|
Cuboidal |
Cube shaped cells. Epidermis and lining of the mouth |
|
|
Submucosa |
Loose connective tissue. Large blood vessels and lymph vessels. Nerve fibers and sensory neurons. Submucosal plexus |
|
|
Submucosal plexus |
Involved In controlling and coordinating contractions of smooth muscle layers and regulating secretions of digestive glands |
|
|
Muscularis externa |
Band of smooth muscle cells, one in a circular layer and one in a longitudinal layer. Contractions.
2 layers with myenteric plexus in between. |
|
|
Parasympathetic stimulation of Muscularis externa |
Increases muscle tone and activity |
|
|
Sympathetic stimulation of Muscularis externa |
Muscle inhibition and relaxation |
|
|
Myenteric plexus |
Between layers of muscular externa. Nerves. Sensory neurons. Interneurons. Parasympathetic ganglia. Sympathetic postganglionic fibers |
|
|
Serosa |
Membrane that covers the Muscularis externa |
|
|
Mesenteries of the serosa |
Double membrane sheets. Vessels, nerves, lymph. Stabilize position of the intestines and organs. |
|
|
Pacesetter cells |
Trigger waves of contraction that move digestive materials |
|
|
Peristalsis |
Movement of material along the tract. 1. Contraction of circular muscles behind food forces it forward 2. Contraction of longitudinal muscles ahead of food. |
|
|
Segmentation |
Mechanical mixing of materials in small intestine |
|
|
Uvula |
Helps prevent food from entering the pharynx too soon. |
|
|
Oral mucosa |
Stratified squamous epithelium |
|
|
Functions of the oral cavity (4) |
1. Senses and analyses material before swallowing 2. Mechanical processing 3. Lubricates material with mucus and salivary secretions. 4. Begins digestion of carbohydrates and lipids with salivary enzymes |
|
|
Lingual tonsils |
Lymphoid nodules thay help resist infection |
|
|
Salivary glands |
3 pairs that secrete into the oral cavity. Mostly water but also has mucins, ions, buffers, waste products, metabolites, and enzymes |
|
|
Functions of salivary glands (4) |
Lubricates the mouth and dissolve chemicals that stimulate the taste buds
Cleans oral surfaces
Antibodies and lysodomes help control oral bacteria Produce salivary amylase
|
|
|
Salivary amylase |
An enzyme that breaks down starches.
Made by parotid glands (a salivary gland) |
|
|
Enamel |
Contains crystalline form of calcium phosphate, the hardest biological substance. Calcium, phosphates, and vitamin D3 are essential |
|
|
What substance is the bulk of each tooth |
Dentin: a mineralized mix similar to that of bone. Doesn't contain cells |
|
|
Incisors |
Blade shaped teeth at front. Clipping and cutting |
|
|
Cuspids |
Canines. Conical with sharp tip. Tearing and slashing |
|
|
Bicuspids and molara |
Flattened crowns with ridges. Crushing and mashing and grinding |
|
|
Esophagus |
Throat. Have stratified squamous epithelium and contains mucous glands |
|
|
4 steps in swallowing process |
1. Oral phase: reflex response begins. Compression of bolus 2. Pharyngeal: elevation of larynx and folding of epiglottis 3. Esophageal: bolus enters esophagus. Peristalsis waves 4. Bolus enters stomach through the lower esophageal sphincter |
|
|
Purpose of tonuge |
Compacts debris into a bolus |
|
|
Functions of the stomach (4) |
Temporary storage Mechanical breakdown Chemical breakdown of bonds by acids and enzymes Production of intrinsic factor for absorption of vitamin B12 |
|
|
Chyme |
Highly acidic mixture of partially digested food |
|
|
Rugae |
Prominent folds and ridges in the stomach mucosa, when the stomach is empty |
|
|
The stomach is lined by |
Simple columnar epithelium dominated by mucus cells |
|
|
What types of cells are in the gastric wall (4) |
Mucus cells Parietal cells Chief cells Endocrine cells Also have gastric glands |
|
|
Mucus cells |
Secrete alkaline mucus that covers and protects epithelial cells from acids, enzymes, and abrasive materials |
|
|
Gastric glands |
Secrete gastric juice |
|
|
Parietal cells in the gastric wall |
Secrete intrinsic factor and hydrochloric acid |
|
|
Intrinsic factor |
Aids in the absorption of vitamin B12 across the intestinal lining. Needed for erythropoiesis |
|
|
Erythropoiesis |
Making red blood cells |
|
|
Hydrochloric acid produced by Parietal cells |
Lowers the pH of the gastric juices |
|
|
Chief cells |
Secrete a protein pepsinogen, which is converted into pepin, a proteolytic enzyme |
|
|
Proteolytic |
Breakdown of proteins into amino acids or smaller peptides |
|
|
Endocrine cells in gastric wall |
Involved in the regulation of gastric activity |
|
|
3 steps of stomach movement |
1. Cephalic phase: sight..smells...thought of food prepares the stomach to receive the food. Cells in gastric wall are stimulated. So is Submucosal plexus. 2. Gastric phase: food arrives in stomach. Stimulation of stretch receptors and chemoreceptors. Stimulates myenteric plexus to mix and gastrin stimulates stimulates contractions 3. Intestinal phase: chyme enters small intestine. Release of CCK and GIP resulting in reduced gastric activity in the stomach |
|
|
No food is absorbed in the |
Stomach |
|
|
Why is no food absorbed in the stomach (4) |
1. Alkaline mucus covers surface so it's not directly exposed to chyme
2. Epithelial cells lack specialized transport mechanism
3. Gastric lining is impermeable to water 4. Digestion has not completed yet. |
|
|
90% of food is absorbed in the |
Small intestine |
|
|
3 segments of the small intestine |
1. Duodenum: mixing bowl. Receives secretions from the pancreas and liver. 2. Jejunum: Most of digestion and absorption 3. Ileum: longest. Sphincter controls flow of material into large intestine |
|
|
The mucosa of the small intestine is composed of |
A multitude of finger like projections called villi that are covered in Simple columnar epithelium carpeted with microvilli |
|
|
Each villus in the intestinal wall contains |
A network of capillaries that transport respiratory gases and carries absorbed nutrients to the hepatic portal circulation for delivery to the liver. Also contains nerve endings and lymphatic capillary. |
|
|
What are the 4 gastrointestinal hormones |
1. Gastrin: released by stomach upon vagus nerve stimulation and arrival of food, stimulates production of acids and enzymes.
2. Secretin: released by duodenum upon chyme arrival. Targets pancreas, liver, and stomach. Inhibits gastric secretion. Stimulates bile secretion and alkaline buffers
3. CCK: made in duodenum upon arrival of chyme. Targets multiple places. Stimulates pancreatic enzymes, inhibits gastric secretions, relaxation of sphincter at bile duct
4. GIP: released by duodenum and stomach. Stimulates release of insulin by pancreatic islets. Stimulated by large amounts of fats and glucose
|
|
|
Gastrin |
released by stomach upon vagus nerve stimulation and arrival of food, stimulates production of acids and enzymes. |
|
|
Secretin |
released by duodenum upon chyme arrival. Targets pancreas, liver, and stomach. Inhibits gastric secretion. Stimulates bile secretion from liver and alkaline buffers from exocrine pancreas |
|
|
CCK |
made in duodenum upon arrival of chyme. Targets multiple places. Stimulates pancreatic enzymes from exocrine pancreas, inhibits gastric secretions, relaxation of sphincter at bile duct |
|
|
GIP |
released by duodenum and stomach. Stimulates release of insulin by pancreatic islets of the endocrine pancreas. Stimulated by large amounts of fats and glucose |
|
|
Pancreas |
Responsible for most of digestion Endocrine: secrete insulin and glucagon
Exocrine: produces pancreatic juice, a mixture of enzymes and buffers for the small intestine. Stimulated by hormones from the duodenum when chyme arrives: CCK. |
|
|
The pancreas is primarily |
Exocrine |
|
|
Pancreatic amalyse |
Breaks down carbs |
|
|
What accounts for 70% of total pancreatic enzyme production |
Proteases. = trypsin, chymotrypsin, carboxypeptidase Break down complex proteins |
|
|
What are the 3 functions of the liver |
1. Metabolic regulation: regulates composition of circulating blood. All blood leaving the absorptive areas of the digestive tract flows through the liver before reaching the general circulation. 2. Hematological regulation: removal of aged and damaged red blood cells, debris and pathogens by kupffer cells 3. Bile production: help dilute and buffer acids in the chyme as it enters the small intestine |
|
|
Hepatocytes. 2 functions |
The predominant cell type in the liver.
body.
1. Extract absorbed nutrients or toxins from the blood before they reach the rest of the body.2. Monitor and adjust the circulating levels of organic nutrients. Ex. Synthesis and breakdown of glucagon
Can also secrete bile
|
|
|
What is the basic functional unit of the liver |
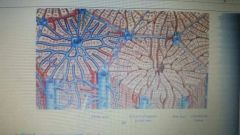
Liver lobes that contain plates of hepatocytes. Sinusoidal are highly permeable capillaries that flow between the plates. Hepatocytes absorb solute from the plasma and secrete proteins back. |
|
|
Gallbladder |
Stores and concentrates bile prior to its excretion to the small intestine. |
|
|
Bile is released into the duodenum |
Under stimulation of CCK |
|
|
Major functon of the liver |
Synthesis and secretion of bile. Storage of glycogen and lipid reserves. Maintenance of normal blood levels of glucose, amino acids, and fatty acids. Inactivation of toxins. Storage of ion reserves. Storage of fat-soluble vitamins. Synthesis of plasma proteins and clotting factors. Phagocytosis of damaged red blood cells by kupffer cells. Phagocytosis of damaged red blood cells by kupffer cells.
|
|
|
3 parts if the large intestine |
1. Cecum: compaction 2. Colon: abundance of mucous cells and lack of villi. Pouches for distension and elongation 3. Rectum: temporary storage of feces |
|
|
Functions of the large intestine |
Absorbing. Preparing fecal material for elimination. Reabsorption of water and bile salts Bacteria residing in colon generate 3 vitamins: K, Biotin, B5 |
|
|
Carbs start being broken down in the |
Stomach |
|
|
Lipids start being broken down in the |
Small intestine. By bile salts and pancreatic lipase |
|
|
Proteins start being broken down in the |
Stomach by pepsin and then trypsin, etc in the small intestine |
|
|
4 types of digestive enzymes |
Carbohydrases: carbs and sugars Lipases (pancreatic): triglycerides Proteases: proteins Nucleases (pancreatic): nucleic acids |
|
|
Hypothalamus |
Production of ADH and other regulatory hormones. ADH: constructs blood vessels and makes u retain water |
|
|
Endocrine cells release |
Hormones into the bloodstream. Travel to target cells: the cell must have receptors that can bind the hormone and initiate a change in cellular activity |
|
|
Two types of hormones (how they affect the cell) |
1. Binds to surface membrane receptors 2. Diffusion |
|
|
How do hormones that bind to plasma membrane cause a reaction |
1. Bind to membrane receptor coupled to a G Protein (link between first and second messenger) 2. Second messenger then activates cell activity |
|
|
How does epinephrine work |
1. Binds to hormone receptor. 2. Triggers G Protein 3. Activates adenylyl cyclase 4. Converts ATP to cAMP 5. Activates kinase enzymes that alter enzyme activity by phosphorylation (adding a phosphate group) |
|
|
Both steroid hormone and thyroid hormone |
Past directly through target cell membranes. Steroid binds to receptors in cytoplasm or nucleus. Thyroid binds to receptors in nucleus or mitochondria. Thyroid hormone increases rate of ATP production |
|
|
The hypothalamus provides |
The highest level of endocrine control. It acts as an important link between the nervous and endocrine systems. Coordinating centers in the hypothalamus regulate the activities of the nervous and endocrine systems |
|
|
What are the three mechanisms of hypothalamic control over endocrine organs |
1. Production of ADH and oxytocin by hypothalamus neurons which travel through axons to pituitary gland then circulation.
2. Secretes 2 classes of regulatory hormones that control endocrine cells in the anterior lobe of the pituitary gland. RH and IH.
3. Contains autonomic nervous system centers that control the endocrine cells of the adrenal medullae in the adrenal gland..causes them to release hormones |
|
|
RH = releasing hormone IH = inhibiting hormone |
RH: stimulates the synthesis and secretion of hormones by the pituitary gland. IH: prevents the synthesis and secretion of pituitary hormones |
|
|
Pituitary gland |
TSH, FDH Oxytocin and ADH Stimulated by the hypothalamus |
|
|
The hormones produces by the pituitary gland |
All use secondary messengers and cAMP |
|
|
Portal vessels of the pituitary gland |
Blood vessels that link two capillary networks, including the vessels between the hypothalamus and the anterior lobe. Also called portal veins because they have the structure of veins |
|
|
What is the portal system of the pituitary gland |
The portal system ensures that all the blood entering the portal vessels reach certain target cells before returning to the general circulation. It consists of the portal vessels that have the structure of veins |
|
|
The regulatory hormones released at the hypothalamus are directly transported to the |
Anterior lobe of the pituitary gland by the hypophyseal portal system |
|
|
The rate of regulatory hormone secretion by the hypothalamus is regulated through |
Negative feedback.
The hypothalamus releases hormones to the pituitary gland which release hormones that affect target organs. These target organs then release hormones that inhibit the pituitary gland and the hypothalamus (prevent more RH from being released) |
|
|
TSH |
Thyroid-stimulating hormone is released by the pituitary gland when stimulated by the hypothalamus through the TRH hormone. It targets the thyroid glands which triggers the release of thyroid hormones. As circulating concentrations of thyroid hormones rise, the rates of TRH and TSH production decline. TRH-> TSH-> thyroid hormones |
|
|
FSH |
Follicle-stimulating hormone is released by the pituitary gland when the hypothalamus releases GnRH. FSH promotes follicle and egg development in females and stimulates the secretion of estrogen. A peptide hormone called inhibin released by the ovaries inhibits the release of FSH and GnRH through negative feedback control mechanisms. |
|
|
ADH |
Antidiuretic hormone is released by the posterior lobe of the pituitary gland and is released when the body is low on water. It affects the kidneys and causes it to decrease the amount of water lost in urine. It also causes vasoconstriction of blood vessels that help increase blood pressure |
|
|
What is the structure of the thyroid gland |
The thyroid gland contains numerous thyroid follicles that are lined by an epithelium. Each follicle contains a viscous colloid, a fluid containing the thyroid hormones. A network of capillaries surrounds each follicle. Under TSH stimulation from the pituitary gland epithelial cells remove the hormones from the follicle and release them into the bloodstream |
|
|
The thyroid gland contains C cells... |
C cells produce Calcitonin (CT) which helps regulate calcium ion concentrations in the body fluids. C cells release calcitonin when the calcium ion concentration of the blood rises above normal. The hormone target the bones and the kidneys. The resulting reduction in blood calcium levels eliminates the stimulus and turns off the C cells |
|
|
Rising blood calcium... |
The thyroid gland produces calcitonin in the C cells |
|
|
Falling calcium levels on the blood |
The parathyroid secrets parathyroid hormone (PTH) |
|
|
Parathyroid hormome |
Secreted by the parathyroid to elevate blood calcium levels. Affects kidneys, bones, and digestive system |
|
|
Chief cells |
Parathyroid cells that produce parathyroid hormone.
Monitor the concentration of circulating calcium ions and secrete parathyroid hormone when calcium concentration falls below normal |
|
|
Thyroid has ___ cells. Parathyroid has ____ cells |
Thyroid has C cells that release calcitonin to reduce blood calcium levels. Parathyroid has chief cells that release parathyroid hormone to increase blood calcium levels |
|
|
The adrenal gland |
Sits on the top of each kidney. Has 2 parts: Adrenal cortex and adrenal medulla |
|
|
The adrenal medulla produces... |
Epinephrine and norepinephrine. These hormones affect most cells by increasing cardiac activity, blood pressure, glycogen breakdown, and release of lipids by adipose tissue |
|
|
The pancreas is primarily an |
Exocrine organ that produces pancreatic juice, a mixture of digestive enzymes and buffers for the small intestine. The Endocrine portion called the pancreatic islets secretes insulin and glucagon |
|
|
The pancreatic islets are a part of the |
Endocrine pancreas and are composed of primarily alpha (glucagon) and beta (insulin) cells |
|
|
What do the alpha cells and beta cells of the endocrine pancreas produce |
The alpha cells produce the hormones glucagon and the beta cells produce insulin. |
|
|
The purpose of glucagon and insulin is to |
Regulate blood glucose concentration |
|
|
When blood glucose levels rise |
Beta cells secrete insulin causing the increased rate of glucose transport into target cells and glucose use. This causes blood glucose levels to decrease |
|
|
When blood glucose levels fall |
Alpha cells secrete glucagon which stimulates the breakdown of glycogen into glucose in the liver and skeletal muscle. Adipose tissue is also stimulated to release fatty acids for use by other tissues and proteins are broken down into their component amino acids for the liver to convert them into glucose. As a result blood glucose levels rise |
|
|
Many organs have secondary endocrine functions |
Examples are the intestines, the kidneys, the heart, the famous, and the gonads |
|
|
What is the endocrine function of the reproductive system |
In males, the interstitial cells of the testes produce the steroid hormones known as androgens, of which testosterone is the most important. In females, estrogen is produced in the ovaries and is a steroid hormone that supports the maturation of the eggs and stimulate the growth of the lining of the uterus |
|
|
In the ovaries, female sex cells develop in specialized structures called |
In the ovaries, female sex cells develop in specialized structures called follicles under stimulation by FSH. Follicle cells surrounding the ova produce estrogen |
|
|
How does the negative feedback of FSH work in the female ovaries |
FSH stimulates follicle maturation in the ovaries. When FSH stimulates the follicles, the follicles also secrete inhibin, which suppresses FSH release by the anterior lobe of the pituitary gland through a negative feedback mechanism |
|
|
What is adaptation syndrome |
Adaptation syndrome is also known as the stress response. It has three phases: the alarm phase, the resistance face, and the exhaustion phase |
|
|
What are the three phases of the adaptation syndrome |
1. Alarm phase = fight or flight. The dominant hormone is epinephrine/ adrenaline. 2. Resistance phase= long term metabolic adjustments. GCs and other hormones act to shift tissue metabolism away from glucose thus increasing its availability to neural tissue. 3. Exhaustion phase = collapse of vital systems. Homeostatic regulation breaks down. Lipid reserves are exhausted. Failure of electrolyte balance |
|
|
When a photon of light hits a retinal in the rhodopin molecule (visual pigment)... |
The retinal changes shape (flattens) then bleaching occurs. Bleaching is when the ATP is used to restore the retinal back to its original bent shape |
|
|
Vestibular complex |
For balance. Otolith moves with gravity, distorting hair cells with sensory nerve endings |
|
|
Organ of corti |
A structure in the cochlea of the inner ear that produces nerve impulses in response to sound vibrations. Vibrations of the structure cause displacement of the cochlear fluid and movement of hair cells against tge tectorial membrane to produce electrochemical signals. The Celia are graded from long to short providing a tuning capability |

