![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
37 Cards in this Set
- Front
- Back
|
Thrombopoeisis is better known as _________________. |
Megakaryopoiesis Megakaryocytopoeisis |
|
|
Are megakaryocytes typically found in peripheral blood? |
No |
|
|
Megakaryocyte mature by the process of _______________. |
Endoreduplication (endomitosis) |
|
|
What happens in endoreduplication? |
Everything reduplicates (nucleus, cytoplasm, granules), but nothing actually divides. |
|
|
Megakaryocytes have a ___________ nucleus. |
Polyploid nucleus |
|
|
What are the stages of megakaryocyte maturation? |
1. Megakaryoblast 2. Promegakaryocyte 3. Megakaryocyte |
|
|
What are the distinguishing features of a megakaryoblast? |
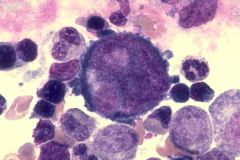
- Very large - Single round nucleus with 1-2 nucleoli - "Hairy" basophilic protrusions - Scant cytoplasm, no granules |
|
|
What are the distinguishing features of a promegakaryocyte? |
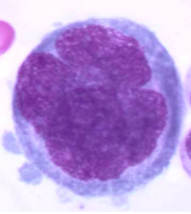
- Increased nuclear and cytoplasmic material - Nucleus becomes lobed - Reddish granules - Membrane demarcation around individual platelets |
|
|
What are the distinguishing features of a megakaryocyte? |
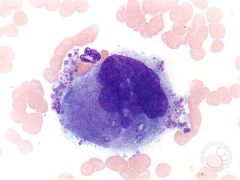
- Gigantic - 8 nuclear lobes with coarse, linear chromatin - Lots of reddish-blue granules - Uniform demarcation system |
|
|
What is the normal number of megakaryocytes in bone marrow? |
1-4 megas per 1000 nucleated cells |
|
|
Platelets are also known as ___________________. |
Thrombocytes |
|
|
What is the major regulating factor of megakaryopoiesis? |
Thrombopoietin (TPO) |
|
|
Where is thrombopoietin (TPO) produced? |
Liver, kidneys, spleen |
|
|
What happens to megakaryocytes in the absence of TPO? |
Apoptosis |
|
|
How do platelet levels affect TPO regulation? |
TPO binds to megas and circulating platelets, so more platelet means less TPO is available to stimulate mega maturation. If platelets are low, more TPO is able to stimulate the production of platelets. |
|
|
How long do platelets last in circulation? |
9-12 days |
|
|
What is the distribution of platelets in the body? |
70% are in peripheral blood 30% are in the spleen |
|
|
What could be considered an abnormally low platelet count? |
< 20,000 |
|
|
What granules are present in platelets? |
1. Alpha granules 2. Dense granules 3. Lysosomes 4. Glycogen |
|
|
What is contained in alpha granules? |
1. Beta thromboglobulin 2. Platelet Factor 4 (PF4) 3. Platelet-derived Growth factor (PDGF) 4. Thrombospondin |
|
|
Which proteins in alpha granules inhibit heparin? |
Beta-thromboglobulin, PF4 |
|
|
What protein in alpha granules promotes interaction between platelets? |
Thrombospondin |
|
|
True/False: Normal platelets will interact with each other and endothelium. |
False |
|
|
What activates the coagulation pathway? |
a) Vascular damage exposing subendothelial collagen (basement membrane) b) Release of tissue factors from damaged epithelial cells |
|
|
What are the 4 functional steps of platelet coagulation? |
1. Adhesion 2. Aggregation 3. Plug formation 4. Clot stabilization |
|
|
What happens during adhesion? |
Platelets bind to collage in subepithelial layers via vonWillebrand Factor (vWF) bridge. Platelets are "activated" by factors that alter their levels of cytosolic Ca, changing their shape into a spiculated sphere. |
|
|
What happens during aggregation? |
GPIIb/IIIa receptors on platelets become active and available for vWF and Fibrinogen binding. Fibrinogen pulls platelets together like glue. |
|
|
What happens during plug formation? |
Platelets degranulate, which recruits more platelets for more aggregation. Clotting cascade creates fibrin to stabilize the mass. Thrombin, plasminogen, tPA, and antiplasmin get trapped in the clot. |
|
|
What happens during clot stabilization? |
Trapped thrombin activates cross-linking of fibrin, everything consolidates and stabilizes at injury site. |
|
|
GPIb binds to _________________. |
vonWillebrand Factor (vWF) |
|
|
GPIIb/IIIa binds to ____________________. |
Fibrinogen |
|
|
Besides coagulation, what other functions do platelets have? |
Maintain vascular integrity by
1) Nurturing endothelial lining by incorporating into wall and releasing PDGF (platelet derived growth factor) 2) Promotes healing of damaged endothelium |
|
|
What is a clinical symptom of low/absent platelets? |
Petechiae or purpura -- RBCs break through vessels and enter lymphatics |
|
|
What is considered a normal "bleeding time" test of platelet function? |
2.5 - 9.5 minutes |
|
|
What are potential causes of platelet clumping in a specimen? |
1. Improper mixing of blood with anticoagulant 2. Improper ratio of blood/anticoagulant 3. (rare) Antibody to EDTA |
|
|
How should platelet count be reported if clumping is seen on the feathered edge of a smear? |
Platelet count is NOT reported |
|
|
What should be done if platelet clumping is seen on the feathered edge of a specimen's smear? |
Redraw a new sample in a sodium citrate (blue top) tube |

