![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
197 Cards in this Set
- Front
- Back
|
What is the systolic blood pressure? What causes it? |
The maximum systemic arterial pressure produced by left ventricular contraction?
|
|
|
What is the magnitude of the systolic blood pressure proportional to? inversely proportional to?
|
proportional to: Stroke volume and velocity of ejection
inversely proportional to: aortic compliance |
|
|
What is systolic hypertension in the elderly characterized by? what causes it?
|
systolic BP is higher than normal in the elderly
Caused by a loss of compliance in large elastic arteries from arteriosclerosis |
|
|
Why does a rigid noncompliant aorta increase BP?
|
B/c it is unable to store the energy of ventricular ejection and nearly all the energy of ejection contributes to the systolic BP
As a result systolic BP is elevated |
|
|
What generates the diastolic BP?
|
Elastic recoil of the aorta
|
|
|
What happens to the mechanical energy generated by systole?
|
Most of it contributes to systolic BP but some of it is stored as mechanical energy when the aorta distends
|
|
|
What is the diastolic BP?
|
The lowest arterial pressure that occurs at the end of left ventricular diastole
|
|
|
What is the magnitude of diastole proportional to? What influences it most?
|
proportional: to HR
Influenced the most by the amount of systemic vascular resistance |
|
|
How do you calculate MAP?
|
[BPsys + (2H BPdias)]3
|
|
|
What is the pulse pressure?
|
BPsys - BPdias
|
|
|
How do you determine BP physiologically?
|
BP = HR x SV x TPR
|
|
|
What variation is seen in BP? when is BP highest? lowest?
|
BP has normal diurnal variation,
BP is highest in the morning and lowest in the evening |
|
|
What effect does exercise have on BP?
|
Isometric exercise (weight lifting) increases BP
Dynamic exercise (swimming) decreases BP |
|
|
What pathology could cause BP to fall during exercise?
|
If systolic BP falls during exercise, systolic myocardial dysfunction secondary to coronary artery disease may be present
|
|
|
When does a wide pulse pressure exist?
|
When BPsys - BPdias is greater than 60mmHg
|
|
|
What is the most common cause for a wide pulse pressure?
|
essential hypertension
|
|
|
What effect would a high cardiac output have on pulse pressure?
|
It would cause a wide pulse pressure
|
|
|
What effect would hyperthyroidism have on pulse pressure?
|
it would cause a wide pulse pressure
|
|
|
What effect would pregnancy have on pulse pressure?
|
It would cause a wide pulse pressure
|
|
|
What effect would anemia have on pulse pressure?
|
It would cause a wide pulse pressure
|
|
|
What effect would fever have on pulse pressure?
|
It would cause a wide pulse pressure
|
|
|
What effect would chronic aortic regurgitation (insufficiency) have on blood pressure? why?
|
it would cause a wide pulse pressure
B/c a portion of the SV into the aorta is returned to the left ventricle during diastole As a result left ventricular EDV and SV are both larger than normal |
|
|
What effect does a large SV have on systolic BP?
|
it increases BP
|
|
|
What effect does chronic aortic regurgitation (insufficiency) have on diastolic BP?
|
Some of the energy stored in the elastic Aorta is released when the regurgitant flow enters the left ventricle
This causes diastolic BP to be higher than normal |
|
|
What is a narrow pulse pressure?
|
When BPsys - BPdias is less than 30mmHg or less than 25% of the BPsys
|
|
|
What effect does aortic stenosis have on pulse pressure? why?
|
May cause a narrow pulse pressure
The smaller opening in the valve decreases SV which reduces the magnitude of the systolic BP |
|
|
What effect would left ventricular systolic dysfunction (CHF) have on pulse pressure?
|
It would cause a narrow pulse pressure
|
|
|
What is normal systolic and diastolic BP?
|
systolic < 120
diastolic < 80 |
|
|
What systolic and diastolic BP would characterize prehypertension?
|
Systolic 120-139
Diastolic 80-89 |
|
|
What systolic and diastolic BP would characterize stage 1 hypertension?
|
Systolic 140-159
Diastolic 90-99 |
|
|
What systolic and diastolic BP would characterize stage 2 hypertension?
|
Systolic >160
Diastolic > 100 |
|
|
How must elevated BP pressure readings be taken?
|
They should be taken twice in the same week
And each visit needs to have two readings taken ~5min apart |
|
|
What is the most common type of hypertension?
|
Essential or "primary" hypertension
|
|
|
When does essential hypertension typically begin? What happens if essential hypertension occurs outside this range?
|
B/e the ages of 35-55
Secondary causes for hypertension (adrenal tumors and vascular occlusion) must be considered |
|
|
What should pts w/ long-standing hypertension be assessed for?
|
Signs of end-organ damage
|
|
|
What end-organ damage pathologies can be caused by long standing essential hypertension? What diseases will these pathologies manifest as?
|
1. Retinopathy (arteriolar sclerosis or neuroretinitis)
2. Heart disease (left ventricular hypertrophy and coronary artery disease) 3. Peripheral vascular resistance (large artery occlusive disease and arterial aneurysms) 4. Cerebral vascular disease (stroke) 5. Kidney disease (proteinuria and renal insufficiency) |
|
|
What systolic and diastolic BPs characterize hypotension?
|
Systolic: < 100
Diastolic: < 60 |
|
|
What pathologies cause hypotension?
|
1. Reduced cardiac function (myocardial infarction or valvular disease)
2. Obstruction to ventricular filling (tamponade or pulmonary emboli) 3. Decreased intravascular volume (blood loss or fluid loss) 4. Excessive vasodilation (microbial sepsis or drugs) |
|
|
What effect does standing have on systolic and diastolic BP? Why doesn't BP change more?
|
systolic: causes pressure to decrease 3.5 mmHg
diastolic: causes pressure to decrease 5 mmHg B/c the drop in BP cause HR, SV and peripheral vascular resistance to increase and compensate |
|
|
What is orthostatic hypotension?
|
A decrease in systolic BP by more than 20 mmHg when a patient stands
|
|
|
How long should you wait to measure a pts BP after standing when you suspect orthostatic hypotension?
|
at least 1 min
|
|
|
If a pt is unable to stand b/c of a drop in pressure, or when the drop in pressure is accompanied by a increase in pulse rate of 30bpm or more what is probably causing the hypo-tension?
|
There is a high likelihood that there has been a large decrease in intravascular volume
i.e. diarrhea, dehydration, bleeding out W |
|
|
If a pt has a drop in BP when standing that is unaccompanied by an inability to stand or a 30 bpm increase in pulse rate what is probably causing the postural hypotension?
|
Failure of the sympathetic nervous system aka "diabetic autonomic neuropathy"
OR it could just be light-headedness that occurs in normal people |
|
|
What effect does inspiration have on systolic/diastolic pressure?
|
Systolic: BP may decrease by 12mmHg
Diastolic: decrease by 6mmHg |
|
|
What causes the drop in BP during inspiration?
|
Pooling of blood in the RA, RV and pulmonary circulation decreasing the amount of blood available in the LV
The storage capacity for blood in the pulmonary spaces increases when the lungs fill w/ air |
|
|
Why do RA and RV filling increase during inspiration?
|
B/c intrathoracic pressure falls and systemic venous return to the heart increases as a result
|
|
|
What is systolic BP proportional to? inversely proportional to?
|
proportional to LV SV and intra-thoracic pressure
|
|
|
What effect does expiration have on systolic BP? what effect does expiration have on LV SV and BP?
|
Increases BPsys b/c of a transfer of blood, LV SV also increases as a result of a shift of blood to the LV
|
|
|
What effect does the change in pressure across the myocardial wall have on BP?
|
During inspiration downward movement of the diaphragm increases thoracic volume and decreases intra-thoracic pressure
The decrease in intra-thoracic pressure also decreases the systolic BP |
|
|
What is a paradoxical pulse?
|
An abnormal finding that exists when there is an inspiratory decrease in systolic BP by more than 12 mmHg
|
|
|
What pathologies are seen in patients w/ a paradoxical pulse?
|
pericardial tamponade and severe bronchospasm (asthma)
|
|
|
Why does pericardial tamponade cause a paradoxical pulse?
|
The LV and RV compete for the same space during ventricular filling b/c the effusion takes up the space
So during inspiration the RA and RV both fill more than usual and LA and LV both decrease So there is a decrease in SV and systolic BP |
|
|
What happens during expiration in pts w/ pericardial tamponade that caused a paradoxical pulse?
|
Blood that was confined to the RA/RV moves to the LA/LV causing SV and BPsys to increase at the expense of RA/RV filling
SO RV SV drops! |
|
|
What characterizes severe asthma? How does this affect BP?
|
Increased resistance to airflow during expiration, so in order to expel air pts must generate a high (positive) intra-thoracic pressure, during inspiration pressure falls to near normal levels
These large swings in intrathoracic pressure affect LV filling and ejection. This causes BPsys to fluctuate dramatically |
|
|
Where should the pts elbow and sphygmomanometer be placed when taking a BP?
|
Elbow positioned at heart level, 4th intercostal space
BP cuff placed over brachial artery one inch above the antecubital fossa NEVER PLACE THE CUFF OVER CLOTHING |
|
|
What error is seen for each 1.3cm above/below the heart the elbow is located?
|
1 mmHg difference in BP for both diastolic and systolic
|
|
|
What error in BP would be seen if the elbow is located 7-8cm below the heart (about the level of the xiphoid)
|
BP will be 6mmHg higher than normal
|
|
|
How big should the sphygomanometer be in relation to the pts arm?
|
20% wider than the diameter of the arm and at least 80% the arm circumference in length
|
|
|
How will a BP cuff that is too small affect diastolic/systolic BP readings? too large?
|
too small: pressures may be 10-15 mmHg higher than normal
too large: results in a pressure so small that it would be of questionable importance |
|
|
When do you palpate the brachial artery while checking BP?
|
During insufflation
|
|
|
What important step must be taken so that the auscultatory gap is not overlooked?
|
Pressure in the cuff must be raised to a level 20-40 mmHg higher than necessary
|
|
|
What rate should pressure be let out of the sphygamanometer? How much pressure should be applied through the stethoscope?
|
10mmHg for every 3 seconds
LIGHT pressure should be applied through the stethoscope |
|
|
What is the phase I Korotkoff sound? What does this designate?
|
Sudden appearance of a clear, sharp, snapping sound
The pressure where this sound occurs is designated systolic blood pressure |
|
|
What is the phase II Korotkoff sound?
|
Sounds soften into a swishing noise
|
|
|
What is the phase III Korotkoff sound?
|
Sounds are crisper and louder
|
|
|
What is the phase IV Korotkoff sound?
|
Sounds are muffled
|
|
|
What is the Phase V Korotkoff sound? what does this signal?
|
The pressure where all sound finally disappears
The pressure where this occurs is the diastolic BP |
|
|
What Korotkoff phase should be used when Korotkoff sounds persist all the way down to 0mmHg? What pathology does this indicate?
|
Phase IV
Indicates aortic insufficiency and extreme bradycardia |
|
|
How long should you wait before repeating BP in one arm?
|
~2minutes
|
|
|
What is the average difference in systolic BP b/e the two arms? which arm has higher BP? what difference is seen in diastolic pressure?
|
Average difference is 10mmHg
Dominant arm has a higher BP No difference is seen in diastolic BP |
|
|
When should BP examination of the lower limbs be performed?
|
In the initial examination for hypertensive patients less than thirty years of age
|
|
|
Where is the sphygomanometer placed when taking BP from the lower limb? where is the stethoscope placed?
|
BP cuff is placed on the thigh w/ the stethoscope placed on the popliteal fossa to auscultate the popliteal artery
|
|
|
How much higher must the cuff pressure be when measuring the BP in the lower limb compared to the upper? why?
|
Cuff is inflated to 40mmHg higher than in the upper extremity
B/c there is increased muscle and soft tissue mass |
|
|
What rate should pressure be released from the BP cuff when measuring lower limb pressures?
|
3mm/sec
|
|
|
What difference is seen in systolic pressure b/e the upper and lower limbs?
|
systolic pressure is higher, BPdias is about the same
|
|
|
What pathology is indicated when the systolic pressure in the arm is higher than the systolic pressure in the leg?
|
A vascular obstruction to blood flow in the lower extremity may be present at any level distal to the subclavian artery
|
|
|
What pathology most commonly causes a systolic BP that is higher in the arm than in the leg?
|
Coarctation of the Aorta
|
|
|
How do you measure the paradoxical pulse using a BP cuff?
|
1. Find phase I Korotkoff sound
2. maintain cuff pressure at the beginning of phase I and observe normal respiratory pattern 3. locate exact pressure where phase I sound is audible on expiration but inaudible on inspiration 4. deflate cuff at 2mm increments until phase I sound is audible during inspiration 5. the amount of pressure difference b/e the two phase I sounds is the paradoxical pulse amount |
|
|
What should you attempt if korotkoff sounds are inaudible?
|
Palpatory blood pressure should be attempted
|
|
|
How do you take a palpatory BP?
|
1. instead of auscultating over brachial artery the examiner palpates the brachial or radial artery
2. The pressure where the pulse first becomes palpable is systolic pressure |
|
|
What is the downside to a palpatory BP?
|
WAY less accurate than an auscultatory BP by about 10mmHg
|
|
|
What is a auscultatory gap? how do you avoid the gap?
|
A temporary disappearance of sound b/e korotkoff phase I and II
Inflating the BPcuff to 20-40mmHg will remove the gap |
|
|
What patients are susceptible to having an auscultatory gap?
|
20% of elderly patients, obese patients and patients who have the BP cuff inflated a second time immediately following a first determination
|
|
|
What effect can overlooking an auscultatory gap have on BP readings?
|
under-estimates systolic BP
over-estimates diastolic BP |
|
|
What effect on BP recording does applying too much pressure w/ the stethoscope have?
|
lowers diastolic BP by 10mmHg or more
|
|
|
What patients can be mistakenly dx'ed w/ hypertension, when really they have pseudohypertension?
|
Pts w/ stiff arteriosclerotic arteries b/c their arteries are harder to compress
|
|
|
What is the only way to get a accurate BP reading in patients w/ pseudohypertension?
|
A intra-arterial catheter
|
|
|
What is a positive osler's sign?
|
Positive when the radial artery, distal to the blood pressure cuff continued to be palpable after the cuff was inflated above systolic pressure
|
|
|
What sign is seen in >44% of elderly patients that are over 85 years old?
|
osler's sign
|
|
|
Where is the pulse rate determined?
|
At the radial artery
|
|
|
How do you determine the pulse rate?
|
counting to 30 than multiplying by 2
Or to 15 and multiplying by 4 |
|
|
When should pulse rate be measured for a full minute?
|
If the pulse is irregular and variable
|
|
|
What affect does inspiration/expiration have on pulse rate?
|
inspiration causes systolic BP to slightly decrease which causes the pulse rate to reflexively increase
expiration causes systolic BP to slightly increase which causes the pulse rate to reflexively decrease |
|
|
What is a normal pulse rate in adults?
|
50-95 bpm
|
|
|
What is bradycardia? tachycardia?
|
Bradycardia: less than 50 bpm
Tachycardia: a pulse rate greater than 100 bpm |
|
|
Why/when is the pulse rate measured at the radial artery inaccurate?
|
When the pulse is irregular and fast b/c the stroke volume of some of the ventricular contractions is too small to generate a palpable peripheral pulse
|
|
|
Where should the examiner measure pulse rate when the pulse rate is irregular and fast?
|
At the cardiac apex (located at the 5th intercostal space in the midclavicular line)
|
|
|
What is the pulse deficit?
|
The difference b/e the measured pulse rate at the cardiac apex and radial artery
|
|
|
What situation does a irregular rhythm describe?
|
a situation where there is variation in the time interval b/e beats, which may be predictable or unpredictable (regularly irregular vs irregularly irregular)
|
|
|
Where is pulse rhythm measured?
|
At the radial pulse
|
|
|
How should amplitude/strength of the pulse be determined?
|
On a beat to beat basis
|
|
|
What is the most important determinant of systolic BP?
|
stroke volume
|
|
|
What is the most important determinant of diastolic BP?
|
Systemic vascular resistance
|
|
|
What causes BPsys to increase and BPdias to decrease during dynamic exercise?
|
Release of local metabolites during dynamic exercise causes vasodilation of vessels, which decreases systemic vascular resistance causes diastolic BP to decrease as well, however SV increases b/c of inc. venous return and other factors so BPsys increases
|
|
|
If a patient has a BP of 100/50 what pathology do they have?
|
wide-pulse pressure
|
|
|
If a patient has a BP of 110/90 what pathology do they have?
|
narrow pulse pressure
|
|
|
What is the definition of HTN?
|
A higher BP in systolic, diastolic or BOTH
|
|
|
What race is at highest risk of HTN?
|
African-americans
|
|
|
What is secondary hypertension? when does it develop?
|
HTN caused secondarily by another dz. Typically if HTN is in a patient under 35 or older than 55 you should think secondary HTN OR if you put a pt on BP lowering drugs and they aren't working you should think secondary HTN
|
|
|
What is the equation to calculate pulse pressure?
|
BPsys - BPdias = PP
|
|
|
What blood pressure changes are seen in essential hypertension?
|
Increased BPsys and Increased BPdias
|
|
|
What factors cause a high cardiac output?
|
1. Anemia
2. Pregnancy 3. Hyperthyroidism 4. Fever |
|
|
What blood pressure changes are seen in chronic aortic regurgitation?
|
Increased BPsys and decreased BPdias
|
|
|
If you are given BPsys and BPdias how could you calculate TPR?
|
Use MAP = 1/3BPsys + 2/3BPdias; then use the value for MAP to calcuate TPR using the formula MAP = HR x SV x TPR
|
|
|
If a patient has a blood pressure of 145/82 what do they have?
|
Stage 1 hypertension
|
|
|
If a patient has a blood pressure of 138/92 what do they have?
|
Stage 1 hypertension
|
|
|
What secondary causes can cause hypertension?
|
Adrenal tumors and vascular occlusion
|
|
|
What is "Shock"?
|
Severe hypotension
|
|
|
What happens to JVP pressure during inspiration? why?
|
It increases b/c the decrease in intrathoracic pressure opens the SVC and IVC allowing more blood to flow through the venae cava into the right heart, increasing JVP
|
|
|
What should you expect if the strength of the pulse changes w/ the phase of respiration?
|
A pulsus paradoxus
|
|
|
What should you expect if the strength of the pulse varies from beat to beat and the variation is not related to respiration?
|
Pulsus alternans
|
|
|
When does pulsus alternans develop?
|
Whehn there is a difference in systolic pressure b/e strong and weak beats by about 15 to 20 mmHg
|
|
|
When is pulsus alternans most noticable?
|
During the several beats following a pause in the cardiac rhythm
|
|
|
What does pulsus alternans indicate? why?
|
Severe left ventricular systolic dysfunction (CHF) probably occurs as a result of alterations in myocardial contractility
|
|
|
What can the examiner make inferences about by evaluating the strength of the pulse?
|
patency of the arterial system
|
|
|
What does a diminished pulse on only one side indicate strongly?
|
Highly suspicious for vascular occlusion
|
|
|
What does the strength of the pulse on palpation correlate directly to?
|
Correlates poorly w/ the level of blood pressure and correlates directly w/ the width of the pulse pressure
|
|
|
What is the normal pulse contour? where is it best assessed?
|
a swift up-stroke followed by a more gradual decline
best assessed at the carotid artery |
|
|
What is pulsus bisferiens? what does it feel like?
|
Occurs in severe aortic regurgitation and in some pts w/ hypertrophic subaortic stenosis (IHSS)
Produces two palpable beats during systole of ea. cardiac cycle |
|
|
What is a hyperkinetic pulse? what does it feel like?
|
Occurs in severe chronic mitral regurgitation or chronic aortic regurgitation where the hyperkinetic pulse is accompanied by an increased pulse pressure that produces the pistol shot pulse, collapsing pulse, or water-hammer pulse
An unusually strong and abrupt character |
|
|
What is a pulse that exhibits a small volume, slow up-stroke and delayed systolic peak? when does it occur/indicate?
|
A plateau pulse, anacrotic pulse or pulsus tardus et parvus
Occurs in valvular aortic stenosis |
|
|
When you feel a pts pulse you feel a small, slow-rising, delayed pulse w/ a notch or shoulder on the ascending limb. What type of arterial pulse abnormality is that? what causes it?
|
An anacrotic pulse caused by aortic stenosis
|
|
|
When you feel a pts pulse you feel a rapid and sudden systolic expansion. What type of arterial pulse abnormality is that? what causes it?
|
A "water-hammer" pulse (aka "pistol shot pulse" aka "collapsing pulse") caused by aortic regurgitation/ mitral regurgitation
|
|
|
When you feel a pts pulse you feel a double-peaked pulse w/ a midsystolic dip. What arterial pulse abnormality is that? what causes it?
|
"Bisferiens" caused by Aortic regurgitation, combined aortic stenosis and aortic regurgitation, and idiopathic hypertrophic subaortic stenosis (IHSS)
|
|
|
When you feel a pts pulse you feel a alternating amplitude of pulse pressure. What abnormality is that? what causes it?
|
A "alternans" caused by congestive heart failure
|
|
|
When you feel a pts pulse you feel a exaggerated drop in systolic blood pressure during inspiration, this was detected by blood pressure assessment. What arterial pulse abnormality is that? what causes it?
|
"Paradoxical (marked) Pulse" caused by Tamponade, Constrictive pericarditis, Chronic obstructive lung disease
|
|
|
What is the "normal" temperature that really has no significance?
|
98.6 deg. F
|
|
|
What variation does temperature show in a person? when is it highest/lowest? How much does it vary?
|
Diurnal variation, highest in the evening and lowest in the morning
May vary by as much 1.5 deg F |
|
|
What can increase temperature in a person?
|
1. OVULATION
2. exercise 3. emotional excitement 4. pregnancy 5. states associated w/ excessive sympathetic discharge and cutaneous vasoconstriction (heart failure) |
|
|
What is the most convenient way to take a temperature?
|
Orally
|
|
|
Where does the temperature in the sublingual artery derive its main arterial supply from?
|
A branch of the external carotid artery
|
|
|
How much does oral temperature vary from true temperature?
|
Underestimates core temperature by .4 deg C (.7 Deg F)
|
|
|
What increases oral temperature?
|
increases .3 deg C after sustained chewing and remains elevated for up to 20 minutes
|
|
|
How much does tachypnea decrease oral temperature?
|
By .5 deg C for ea. 10 minutes per minute increase in respiratory rate
|
|
|
How much does rectal temperature vary from true temperature?
|
Overestimates core temperature by ~.2deg C (.4 degF)
|
|
|
In what patients should you measure temperature rectally?
|
In patients suspected of having factitious fever
|
|
|
Why don't rectal temperatures reflect sudden changes in body temperature?
|
B/c fecal contents can act as a heat sink
|
|
|
By how much does axillary temperature vary from true temperature?
|
Lower than oral temperature by 1 deg. F to 4.2 deg. F so 1.7 deg F to 4.9deg F below true body temperature
Axillary temperature readings are so inaccurate that they should NOT be used |
|
|
What temperature reading method is the closest approximation to true body temperature? Why?
|
Tympanic membrane temperature
B/c a branch of the same artery that perfuses the body's thermostat in the hypothalamus perfuses the tympanic membrane |
|
|
What is the downside to tympanic membrane temperatures?
|
They lack precision
They can vary b/e the left/right sides and certain disease prevent accurate readings |
|
|
What conditions prevent accurate readings of tympanic membrane temperature? what direction do these conditions shift the temperature reading?
|
Tympanic membrane readings may be falsely low if the ear is occluded w/ cerumen
Tympanic membrane readings may be falsely elevated if the pt has inflammation of the tympanic membrane (otitis media) or ear canal (otitis externa) |
|
|
What is "fever" defined as?
|
An oral AM temperature greater than 98.9 deg F (38 degC) or an oral PM temperature greater than 99.9deg. F (38 degC)
|
|
|
What causes a fever physiologically?
|
An elevation in the set point of the body's thermostat including cutaneous vasoconstriction, increased muscle metabolism and shivering to mediate a temperature increase
|
|
|
What fever has the most useful diagnostic pattern of all fever patterns?
|
"relapsing fever" or "saddleback fever"
|
|
|
A patient is describing their fever to you, they describe it as having days of fever alternating w/ days of normal temperature. What fever pattern is that?
|
"Relapsing Fever" aka "Saddleback Fever"
|
|
|
What fever occurs in pts w/ Hodgkin's lymphoma? What is it's pattern"
|
"Pel-Ebstein Fever"; lasts for about a week, remits for a week and then recurs again
|
|
|
What fever pattern is highly suggestive of malarian infection w/ P. Vivax or P. Ovale? what is it's pattern?
|
"Tertian Fever"; Occurs every 3rd day for 48 hours, counting the day of an episode as the first day
|
|
|
What fever pattern is suggestive of malarian infection w/ P. Malariae? What is it's pattern?
|
"Quartan Fever"; occurs every 4th day for 72 hours counting the day of an episode as the first day
|
|
|
A pt is describing their fever to you. They describe it as starting high but falling each day but it never fell all the way to normal (never went below 99.2 deg F). What fever pattern is that?
|
"Remittent Fever"
|
|
|
A pt is describing their fever to you. They describe it as high but it falls back to normal each day. What fever pattern is that?
|
"Intermittent fever"
|
|
|
A pt is describing their fever to you, and they describe it as a huge difference during the day, where the high temperature is 2.5 deg F above the low temperature. What fever pattern is that?
|
"Hectic fever"
|
|
|
A pt is describing their fever to you and they describe it has having fluctuations in temperature by < .5 deg F during a 24 hour period; but the temperature is always elevated. What fever pattern is that?
|
"sustained fever"
|
|
|
How does fever affect pulse rate?
|
Pulse rate increases an avg of 2.5 bpm per minute for ea. degree F of temperature elevation up to 100.8 deg F
Higher temperatures may result in larger pulse increases |
|
|
What infections cause the pulse to NOT increase as much as expected w/ fever?
|
Salmonella typhi and legionella pneumophila
|
|
|
What is the upper limit of fever? what can cause this limit to be surpassed?
|
42 deg C or 107.6 deg F
Core temperature may exceed this value as a result of environmental or drug induced causes of hyperthermia |
|
|
What infection causes fever temperatures exceeding 41.1 deg C (106 deg F)?
|
Gram NEGATIVE bacteria
|
|
|
How do you convert from Fahrenheit to Celsius? Celsius to Fahrenheit?
|
T deg C = 5/9([T deg F] - 32)
T deg F = 9.5 ([T deg C] + 32) |
|
|
What defines hypothermia? what causes hypothermia?
|
A oral temperature less than 95 deg F
Hypothyroidism, hypoadrenalism, overwhelming infection, intoxication and cold exposure Old people and Babies w/ hypothermia have the same drastic effects as hyperthermia do |
|
|
What is the normal respiratory rate? How does this vary?
|
20 breaths/min (range 16-25) has diurnal variation where it is higher in the PM than in the AM
|
|
|
What is Tachypnea? Bradypnea? Apnea? Hyperpnea?
|
Tachypnea = respiratory rate of 25 breaths/min or more
Bradypnea = Respiratory rate < 8 breaths/min Apnea = absence of breathing Hyperpnea = increased depth of breathing |
|
|
A patient has a breathing pattern marked by increased inspiratory and expiratory volumes at a slightly fast but sometimes normal/slowed rate. What respiratory pattern is that? what causes it?
|
Kussmaul's breathing, caused by metabolic acidosis (diabetic ketoacidosis) in order to excrete carbon dioxide and bring the pH back toward normal
|
|
|
A patient has a breathing pattern of alternating periods of apnea and hypepnea. Following the apneic phase, there is a step-wise increase in inspiratory volume followed by a step-wise decrease in volume leading to apnea, at a constant rate. What breathing pattern is that? What causes it?
|
Cheyne-Stokes breathing, caused by alternating over correction and under correction of PCO2
|
|
|
What patients is cheyne-stokes breathing observed in?
|
1. Pts w/ neurologic disease: including bilateral cortical dysfunction, hemorrhage, tumor, infarction and head trauma
2. CHF - 30% of patients 3. Normal people during sleep |
|
|
You are observing a patient's breathing pattern and you notice irregular breathing alternating w/ long periods of apnea. What pattern is that? what causes it?
|
Biot's breathing, observed in pts w/ brainstem dysfunction
|
|
|
What is hyperventilation?
|
Increased alveolar ventilation and CO2 elimination in excess of CO2 production
|
|
|
What do the symptoms of hyperventilation relate to? what do they include?
|
A decreased PCO2 in arterial blood and include lightheadedness, blurred vision, numbness of the fingers, toes and lips; chest pain; shortness of breath; anxiety and fear
|
|
|
What is the most common cause of acute hyperventilation?
|
Uncontrolled anxiety
|
|
|
What is orthopnea?
|
Shortness of breath w/ recumbence that resolves when the pt sits upright
|
|
|
What disorders cause a patient to develop orthopnea?
|
1. Massive ascites
2. Heart failure 3. Chronic lung disease 4. pleural effusion 5. pneumonia |
|
|
What mechanism causes orthopnea?
|
When the vital capacity and lung compliance decrease and venous return increases during supine posture
|
|
|
What is trepopnea?
|
Shortness of breath that is worse in one lateral decubitus postion
|
|
|
What causes trepopnea?
|
1. unilateral lung disease where the pt improves oxygenation by lying w/ their good lung facing down
2. Congestive heart failure from dilated cardiomyopathy where the enlarged heart compresses the left lung and compromises oxygenation when the left lung is down 3. Mediastinal or bronchial tumors where the tumor compresses the airway in one position but not another |
|
|
What is paroxysmal nocturnal dyspnea?
|
PND is shortness of breath that begins several hours after falling asleep in a recumbent position
Patients awaken short of breath and have to get out of bed to catch their breath |
|
|
What causes PND?
|
more SPECIFIC for CHF than orthopnea
|
|
|
What is the patients body mass index?
|
The pts weight in kilograms divided by the height in meters squared (kg/m^2)
|
|
|
What qualifies an overweight person? obese? extreme obesity? underweight?
|
overweight: A BMI that exceeds 25kg/m^2
obese: A BMI exceeding 30kg/m^2 extreme obese: A BMI exceeding 40kg/m^2 underweight: A BMI <18.5 kg/m^2 |
|
|
How can a person w/ a BMI of 27-35 decrease their weight by .5-1 lb/week?
|
By eating 300 to 500 fewer kcal/day
|
|
|
How can a person having a BMI > 35 decrease their weight by .5 to 1 lb/week?
|
By eating 500 to 1000 fewer kcal/day
|
|
|
What is severe malnutrition?
|
Weight loss of 10% of body weight, loss of subcutatneous fat, muscle wasting and edema
|
|
|
How will the BMI change in a malnourished person?
|
It will actually increase w/ the accumulation of edema fluid b/c BMI doesn't directly measure body composition
|
|
|
What is the difference b/e tamponade and asthma in creating a paradoxical pulse?
|
Tamponade is a problem during inspiration
Asthma is a problem during expiration |
|
|
What is an irregularly irregular pulse almost always associated w/? how should you change your exam in response to an irregularly irregular pulse?
|
Atrial fibrillation
You should measure the pulse for a full minute and auscultate the heart sounds as well! |
|
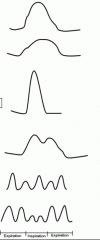
What are these pulse rates?
|
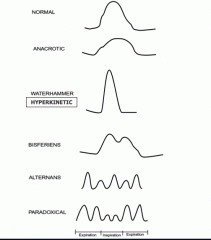
|
|
|
What mechanism causes a bisferiens pulse?
|
HOCM - or abnormal thickening of the myocardium as a result of hypertrophy
|
|
|
What should you ask when a mother calls you saying their child has a fever?
|
Ask "how high is the temperature" AND "how was it measured?"
|
|
|
What disease is associated w/ kussmaul breathing?
|
Diabetic ketoacidosis
|
|
|
What question should ask to assess breathing patterns?
|
"How many pillows do you sleep on at night?"
|

