![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
57 Cards in this Set
- Front
- Back
|
Pathology |
Interested in morphology of disease -Pathology 1) look at specimen grossly and under microscope - determine infection 2) Correlate with clinical presentation |
|
|
White Blood Cells- 2 Categories |
1. Granulocytes 2. M'Mononuclear' cells- nucleus is round and there no granules (but note, all WBCs are really mononuclear) |
|
|
Granulocytes |
Neutrophils (polymorphonuclear), Eosinophils (bilobed nucleus), Basophils |
|
|
'Mononuclear' Cells |
Lymphocytes, monocytes, plasma cells |
|
|
Infection- Definition |
-"Invasion by & multiplication of pathogenic microorganisms in a bodily part or tissue, which may reproduce subsequent tissue injury & progress to overt disease thru a variety of cellular or toxic mechanisms" -Clinically - when microbes cause disease in humans |
|
|
6 Tissue Rxns to Infection |
1) Acute/Suppurative inflammation 2) Mononuclear & granulomatous inflammation 3) Chronic Inflammation & scarring 4) Inflammation w/ eosinophilia 5) Cytopathic/cytoproliferative changes 6) Tissue necrosis *Bold - inflammation |
|
|
Inflammation |
-protective process that brings cells & other molecules of host defense system from blood to injury sites to get rid of infecting organisms & prepare tissue for repair. It is the general response of VASCULARIZED tissue to injury -"-itis" = inflammation due to any cause
|
|
|
Inflammation- Causes |
Many! not just microbial infections |
|
|
Factors that influence type of tissue rxn |
Many! location of microbe, type of microbe, host immune response to microbe, etc |
|
|
Location- one of factors that influence Tissue Rxn Type |
Extracellular organism: -acute inflammation/supparative -immune rxn involves neutrophils & macrophages Intracellular organism: -immune rxn involves mononuclear cell infiltrate: lymphocytes, plasma, cells, and macrophages |
|
|
Purulent/Suppurative Inflammation |
common subtype of acute inflammation- used interchangeably |
|
|
Pyogenic vs purulent |
pyogenic produces pus, purulent contains it |
|
|
Exudate |
fluid discharged or leaked into surrounding tissue due to tissue injury |
|
|
pus |
viable & dying WBC (neutrophils), liquefied necrotic tissue, cellular debris, & protein rich fluid |
|
|
Infectious causes of suppurative inflammation |
neutrophils react against extracellular organisms -most bacteria (most gram+ cocci & gram-- rods) -some fungi |
|
|
Features of Suppurative Inflammation |
-General Features of acute inflammation: rubor, tumor, calor, dolor -purulent exudate -Diagnosis:
|
|
|
Outcomes of Suppurative Inflammation |
-Normal Healing - usual outcome! -Tissue Destruction
-Chronic inflammation & scarring |
|
|
Abscess |
focal lesion where acute inflammatory response resulted in central area of tissue necrosis & neutrophil |
|
|
Summary of acute/supparative inflammation |
-Pt presents w/ acute illness/acute infection due to extracellular bacteria or some fungi will show acute/suppurative inflammation -pus contains: neutrophlils, macrophages, protein rich fluid, cellular debris -Inflammatory response may lead heal (usually), lead to tissue destruction (abscess), progress to chronic infection |
|
|
Mononuclear Inflammation |
-will see infiltrate of mononuclear cells in response to tissue infection *No pus - bc intracellular organisms are handled differently by immune system -most common organisms that elicit response are intracellular organisms & spirochetes |
|
|
Mononuclear inflammation- associated w/ Acute vs associated w/ Chronic Infection |
Acute infection - in response to intracellular organism (e.g. VIRUS) Chronic infection - could be intra or extracellular organism
|
|
|
Granulomatous Inflammation |
-Special subtype of mononuclear inflammation -hallmark: "epitheloid histiocyte" - activated macrophage w/ abundant pink cytoplasm, that also secretes many mediators of inflammatory process -can have infectious or noninfectious etiology
|
|
|
Granuloma |
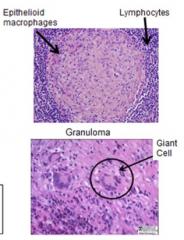
-nodules of activated macrophages, usually surrounded by rim of lymphocytes & plasma cells -Pathogenesis: interaction of certain organisms w/ immune system results in recruitment and activation of macrophages to infection site ---> become activated macrophages aka eptheloid histiocytes --> these group together to form granuloma --within a granuloma, macrophages may fuse to form giant cell that enhances their ability to kill organisms |
|
|
Giant cell |
-within a granuloma, macrophages may fuse to form giant cell that enhances their ability to kill organisms |
|
|
Granulomatous Inflammation- Clinical Presentation |
-Granulamotous inflammations due to microorganisms present as chronic infection -tissues may or may not have central necrosis w/ lymphocytes & plasma cells around periphery
|
|
|
Granuloma Causes |
-can be caused by immune (infectious) or non-immune (noninfectious) mechanisms -When due to infections, granulomas are due to immune-mediated mechanisms against a poorly degradable intracellular microbe
|
|
|
Organisms that Elicit Granulomatous Inflammation |
-Limited # of organisms -Intracellular -Poorly digestible, poorly soluble -resistant to eradication Examples:
|
|
|
Caseous Necrosis |
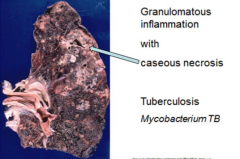
-in central portion of lesion -cheesy-like appearance -characteristic of TB infection |
|
|
Lung Granuloma Histology - Lo Power View |
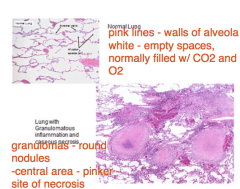
|
|
|
Lung Granuloma Histology - Hi Power View |
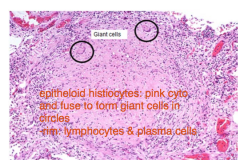
|
|
|
Histology: Abscess vs Granulomatous Inflammation w/ Caseous Necrosis |
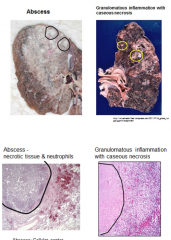
-look similar, w/ necrotic tissue in center -microscopic view tells them apart
|
|
|
Cultures: Abscess vs Granulomatous Inflammation w/ Caseous Necrosis |
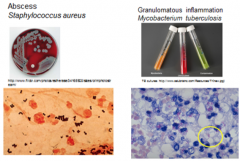
Abscess: -(UR) e.g. Staph on blood agar plate -(BR) gram stain Granulomatous Inflammation: -(UL) M Tb doesn't grow on blood agar, needs special media tubes on upper right -(LL) M Tb doesn't stain w/ gram stains but w/ special stains |
|
|
Summary: Mononculear & Granulomatous Inflammation |
Mononuclear: -Presentation: Acute or chronic infection -Organisms: intracellular, spirochetes, eradicate bacteria -Pathology: ('Mononuclear cells' ) lymphocytes, plasma cells, macrophages Granulomatous: -Presentation: Chronic -Organism: ****TB (other mycobacteria, fungi, parasites) -Pathology: granulomas, epitheloid macrophages, giant cells, w/ or w/o caseous necrosis, rim of lymphocytes & plasma cells |
|
|
Chronic Inflammation & Scarring- Definition |
delayed-onset & protracted duration response of host to tissue injuries & certain foreign injurious agents that may persist for an indefinite period of time |
|
|
Chronic Inflammation- Clinical Presentation |
-can have infectious & noninfectious causes -when due to microorganisms, presentation is a chronic infection |
|
|
Chronic Inflammation & Scarring - Causes |
-Intracelluar -Hard-to-eradicate extracellular -long-standing infection due to any type of organism |
|
|
Chronic Inflammation & Scarring - Tissue Rxn |
-mediated by many chemical mediators -involves any or all of mononuclear cell infiltrate (lymphocytes, plasma cells, & macrophages) & mast cells -When causes significant tissue damage --> scarring *Note: no abscess |
|
|
Chronic Inflammation - Histology |
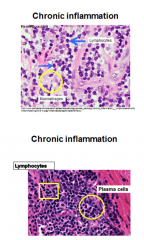
-Lymphocytes: small, scant cytoplasm, & round nuclei -T/B cells: can't be told apart -Cant tell type of organism by just looking at types of cells in tissue run - even though there are diff combinations of mononuclear cells in response to diff types of organisms |
|
|
Scarring aka fibrosis |
-one way to repair damaged tissue, caused by after prolonged or repeated bouts of chronic inflammation involves many cells and release of mediators -fibroblasts move into area where damaged tissue was removed & lay down collagen -permanent change in tissue structure -possible permanent change in tissue function
|
|
|
Hepatitis B |
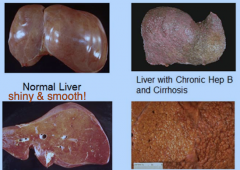
-virus that infects hepatocytes of liver -tissue run is chronic inflammation -may result in cirrhosis - formation bumpy nodules on liver due to fibrosis |
|
|
Hepatitis B- Histology |
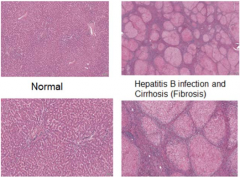
-Normal: homogenous -Abnormal: many pink nodules (of hepatocytes), varying sizes, separated by bands of purple cells (area of fibrosis & chronic inflammation of mononuclear cells)
|
|
|
Cirrhosis Consequences |
Altered liver structure - increased pressure in portal system can cause -Varices: abnormal, enlarged veins in distal esophagus --> risk of severe bleeding -Ascites: fluid in peritoneal cavity --> risk of infection Impaired liver function -Inability to make clotting factors, protein -Jaundice: inability to handle bile |
|
|
Summary: Chronic Inflammation & Scarring |
-Clinical Presentation: Chronic infection -Organisms: Intracellular, hard-to-eradicate extracellular, longstanding infection due to any organism -Tissue Rxn: Mononuclear cell infiltrate & Tissue Damage/Fibrosis w/ long duration
|
|
|
Inflammation with Eosinophila |
-Clinical Presentation- Acute or chronic -Organisms: helminths -Tissue Rxn: abundance of eosinophils, mononuclear cell infiltrate, sometimes granulomas |
|
|
Eosinophils - Histology |
Eosinophils - bright orange-red granules & bilobed nucleus |
|
|
Eosinophils - Function |
Defend against helminthic infections -parasites are too large to be ingested -IgE Antibodies bind to helminths -FcR on eosinophil recognizes Fc -eosinophilic granules: secrete MBP, which is toxic for helminths but also causes extensive host tissue damage
|
|
|
Worm Infections |
Cause eosinophilic response & can also cause granulomatous response -their eggs are seen as a foreign object and granulomas form as a response |
|
|
Cytopathic Changes |
-Definition: Structural changes in cells due to infection by certain viruses -diff changes --> diff viruses Features:
|
|
|
Cytomegalovirus (CMV) |
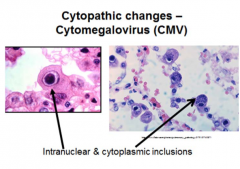
-inclusions made of viral aggregates & altered host cell structures |
|
|
Herpes Simplex Virus |
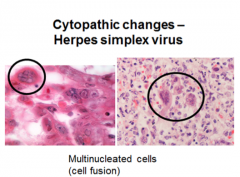
-different than CMV- causes multinucleated cells! |
|
|
HPV |
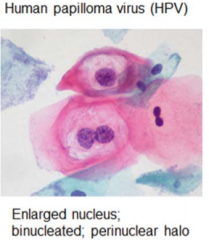
enlarged nucleus, binucleated, perinuclear halo |
|
|
Adenovirus |
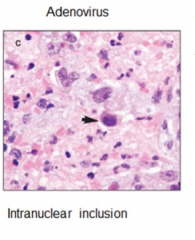
Intranuclear inclusion |
|
|
Cytoproliferative Changes |
-increase in cell # -Organisms: some viruses -Viral infection w/ proliferation: usually associated w/ cytopathic features -Viral infection, proliferation, & transformation to cancer: very uncommon & need viral infection & other factors to cause cellular changes for cancer E.g HPV
|
|
|
HPV |
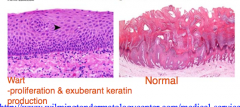
-Some subtypes lead to proliferation and cytopathic changes -infects squamous cells of cervix, inserting viral DNA into host DNA -alone cannot cause development of cancer - needs co-factors! -* |
|
|
Tissue Necrosis - Tissue Rxn |
-sometimes can be widespread necrosis w/ no inflammation -This is most often seen w/ toxin-mediated injury
|
|
|
Gas gangrene |
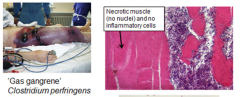
-bacterium secretes toxin that causes rapid death of mscl tissue & also produces gas -Results in in necrotic mscl tissue, masses of bacteria, & no inflammatory infiltrate -Example: Clostridium perfringens |
|
|
Chart: Diff Tissues Cause Diff Types of Tissue Rxns |
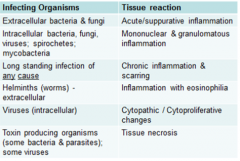
|

