![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
117 Cards in this Set
- Front
- Back
|
diuretics
|
drugs that increase renal excretion of water, sodium and other electrolytes, increasing urine formation
|
|
|
purpose of diuretics
|
manage edema, heart failure, hypertension
|
|
|
goal of diuretics
|
reduce extracellulare fluid volume & reverse abnormal fluid retention in the body.
|
|
|
where do diuretics act
|
on the kidneys
|
|
|
where sodium goes
|
water flows
|
|
|
what are the mose effective diuretics
|
loop diuretics - high ceiling.
lasix |
|
|
lasix
|
furosemide - increase urine output even though there is a decrease in blood flow to the kidneys
|
|
|
where do loop diuretics work
|
on the ascending loop of henle, to prevent sodium and chloride re-absorbtion.
|
|
|
when is the maximum effect of loop diuretics
|
1-2 hours after oral med, 2-10 min after iv med
|
|
|
what are some complications of loop diuretics
|
dehydration, electrolyte imbalance, potassium depletion, can lead to dysrhythmia
|
|
|
when do you use loop diuretics
|
moderate to severe fluid retention
|
|
|
what is the most accurate measurement of fluid retention
|
daily weight
|
|
|
thiazide diuretics
|
benzothiadiazides - block sodium and chloride reabsorbtion in distal tuble.
|
|
|
what is the most common thiazide diuretic?
|
hydrochlorothiazide
|
|
|
what is a thiazide diuretic used for ?
|
long term mngmt of heart failure and hypertension. pt must have adequate urine flow.
|
|
|
when do you use thiazide diuretics cautiously
|
allergy to sulfa drugs
pregnancy pt taking digoxin diabetics |
|
|
what is the goal of Potassium - sparing diuretics
|
to promote diuresis and maintain normal serum _______ levels.
|
|
|
where do K-sparing diuretics work
|
on the distal renal tublule to retain potassium and excrete sodium
|
|
|
hypertension
|
a disease characterized by a systolic bp of >140 or diastolic of > 90
|
|
|
arterial bp
|
the force exerted on artery walls by blood flow
|
|
|
primary hypertension
|
90-95% of all cases of hypertension - the cause is unkown, it is incurable, but controllable. It increases with age
|
|
|
secondary hypertension
|
hypertension with a cause - Caused by : renal, endocrine, or CNS disorders.
drugs that stimulate the CNS drugs that cause Na+ and H2O |
|
|
Per-hypertension
|
120-139systolic or
80-89 diastolic |
|
|
stage 1 hypertension
|
systolic 140-159 or
diastolic 90-99 |
|
|
stage 2 hypertension
|
systolic> 160 or diastolic 100 or >
|
|
|
goal of hypertension mngmt
|
maintain bp 140 /90
if the pt has diabetes, heart failure, or renal disease below 130/80 |
|
|
HTN effects
|
-increased workload of the heart can cause heart failure
-arterial lumen narrows which leads to a decreased blood supply to tissues. -increased risk of thrombosis -organ damage -arteries may rupture @necrotic areas. |
|
|
hypertensive emergencies symptoms
|
severe headache, nausea, vomiting, visual disturbances, neurological disturbances, disoriaentation, decreased level of consciousness
|
|
|
what is the goal when trying to manage bp with meds
|
maintain bp lower than 140/90, 130/80 for diabetics
|
|
|
HTN effects
|
increased workload of the heart
arterial lumen narrows leading to decreased blood supply to tissues increase risk of thrombosis organ damage |
|
|
hypertensive emergencies ss
|
severe headach, nv, visual disturbances, disorientation
|
|
|
beta adrenergic blocking agents - beta blockers
|
occupy beta adrenergic receptor sites to prevent response to sympathetic nerve impulses
|
|
|
beta 1 blockade
|
affects heart,
HR, Cardiac output and renin release is decreased - BP is lowered |
|
|
what are the advantages of beta blockers
|
mminimal hypotension, little effect on sexual function, little to no slowing of cns
|
|
|
when are beta blockers less effective
|
african american pts
|
|
|
when do you avoid use of beta blockers
|
pts with asthma, type 1 diabetes, heart failure, peripheral vascular disease.
|
|
|
example of a beta blocker
|
propanolol - usually end in olol
|
|
|
ace inhibitors
|
block the enzyme that converts angiotension 1 to angiotensin 2
|
|
|
what is the result of a ace inhibitor
|
vasodilation, decrease aldosterone
|
|
|
what do ace inhibitors end with
|
pril
|
|
|
where are ace inhibitors recommended
|
diabetic pts
|
|
|
what may happen at the start of using ace inhibitor
|
hypotension
|
|
|
what is the black box warning of ace inhibitors
|
pregnant women.
|
|
|
angiotensis II receptor blockers
|
blocks the effects of angiotensin II - the potent vasoconstrictor from binding on sites in blood vessels, brain, heart, kidneys, and adrenal glands.
|
|
|
what are ABR's less likely to do then ACE inhibitors
|
cause hyperkalemia
|
|
|
what is the black box warning on ABR's
|
pregnant women
|
|
|
calcium ion antagonists action / result
|
move calcium ions across cell membrane resulting in fewer arrhythmias, slower contraction rate of heart, relaxation of smooth vessels, leading to vasodilation and decreased bp
|
|
|
what does the effect of calcium ion antagonist depend on
|
the severity of the disease.
|
|
|
what is a common direct vasodilator
|
hydralazine (apresoline)
|
|
|
what is the prefered rx of choice for children with htn
|
beta blockers
|
|
|
can you use ace inhibitors on children
|
6years or older - for htn with coexisting conditions - diabetes, renal disease
|
|
|
infiltrations
|
leaking of iv fluids out of vein
|
|
|
what happens during infiltration
|
skin becomes hard(induration) and firm
absencse of blood return skin temp / swelling changed painful, numbness, tingling |
|
|
phlebitis
|
inflammation of only the vein,
preventable through close observation cannula must be removed |
|
|
hematoma and bruising
|
leakage of blood into surrounding tissue
|
|
|
extravasation
|
unintentional infaltration with vesicant medication. causing blisters with subsequent sloughing of tissue due to necrosis.
|
|
|
vesicant meds and fluids
|
TPN - 50% dextrose
Dextroxe 10% or greater then 10% of any IV fluid that is hypertonic Potassium chloride (KCL) Phenytoin (Dilantin) Cytotoxic antineoplastic agents (chemotherapy) |
|
|
special precaution for KCL
|
must always be diluted, never IV push
|
|
|
who is at high risk for extravasation and why
|
infants - size
elderly & CA pts - fragility comatose & anesthetized pt pt using high pressure infusion pumps pts with peripheral or cv disease pts who undergo cpr |
|
|
how do you get speed shock
|
too rapid IV push, IV drip,
ss =irregular pulse, CA, sycope, headach, facial flushing, tighness of chest |
|
|
air embolism
|
traveling embolism of air,
|
|
|
how big does a air embolism need to be to kill someone
|
9-15 cc of air
|
|
|
what is treatment for an air embolism
|
turn to the left side, trangellenberg position this will trap air in right atrium
|
|
|
vasovagal reaction
|
sudden complete colapse of the vein,,
stimulates nerve #10 |
|
|
what to do for infiltration of phlebitis
|
slow large volume infusions to KVO 6-10 ml/hr and STOP piggy back meds until iv team checks site
fill out iv communication form chart carrout out nursing intervention to relieve problem |
|
|
continuous IV
|
one IV line used to infuse fluids
|
|
|
keep open
|
keeps vein open with slow infusion at 6-10 ml per hour- it is a type of primary infusion only the rate is consistently slow
|
|
|
medication
|
use mini bags to deliver medicine in various amounts attached to the primary line
|
|
|
adapted sites
|
converted angiocath used for intermittent delivery of medicines
called - converted angio, adapted angio, medicine/saline/heparin lock |
|
|
what are the 2 basic types of IV fluid replacements
|
colloids and crystaloids
|
|
|
colloids
|
protiens or other large molecules remain in blood because they are too large to cross capillary membrane. Called plasma volume expanders bc they draw h2o from the cells into the plasma and increase plasma osmolality and osmotic pressure
|
|
|
crystalloids
|
IV solution that contains electrolytes that quickly diffuse across membrane leaving plasma and entering IFC and interstitial fluid. used to replace lost fluids.
|
|
|
the infusion of crystaloids can be
|
hypertonic, isotonic, or hypotonic
|
|
|
hypertonic infusion of crystaloids
|
cause h20 to be drawn from cells and tissues and expand plasma volume with osmolality higher then that of plasma
|
|
|
what are the two indirect actions of IFN-gamma?
|
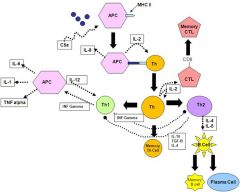
1. stimulates macrophages to produce IL-12
2. stimulates TH1 cells to produce IL-2, IFN-gamma, and TNF-beta pg 240 Parham |
|
|
hypotonic infusion of crystalloids
|
causes h20 to move out of the plasma into the tissues and cells with osmolality lower then that of plasma
|
|
|
isotonic iv solution used for
|
used to restore blood volume bc same concentration as blood plasma
|
|
|
isotonic iv solution examples
|
0.9 % NaCL (NSS)
Lactated ringers 5% d5W d51/4NSS |
|
|
Hypertonic IV solutions used for
|
to draw fluid into the vein and increase blood volume
|
|
|
who don't you administer hypertonic solutions to
|
dehydrated pts or pts that have kidney or heart disease.
|
|
|
examples of hypertonic solutions
|
d5nss
d51/2nss d5lactated ringers d10w (10% dextrose in H20) 3%NS |
|
|
hypotonic iv solutions used for
|
lower concentration than blood plasma
draws fluid from blood into tissues to hydrate cells, reverse dehydration. |
|
|
examples of hypotonic iv solutions
|
0.45%NS
0.33%NSS 2.5%DW |
|
|
contraindications for hypotonic solution
|
it can cause fluid to be drawn into red blood cells causing them to swell and rupture - hemolysis.
do not give for a pt with intercranial pressure |
|
|
iv solutions as a nutrient
|
useful in preventing ketosis and dehydration, but not enough calories to promote wound healing, weight gain, or normal growth
|
|
|
examples of iv solution as a nutrient
|
d5w
d5nss 170 calories/ liter |
|
|
iv solutions as an electrolyte
|
contain varying amounts of sodium, chloride, potassium,
calcium and lactate. |
|
|
examples of iv solutions as electrolyte
|
nss
lactated ringers |
|
|
iv solutions as blood volume expanders
|
draw interstitial fluids into vessels to increase blood volume.
|
|
|
examples of blood volume expanders (colloids)
|
dextran
plasma human serum albumin |
|
|
angiocath veins
|
metacarpal, basilic and cephalic veins
|
|
|
what don't you use with an angiocath
|
do not infuse TPN or chemotherapy
|
|
|
how often do you change and angiocath
|
every 96 hours.
|
|
|
what are central venous access sites used for
|
long term iv therapy, parenteral nutrition, to administer iv meds that are irritating to peripheral veins
|
|
|
Where are central venous access sites inserted
|
subclavian or jugular vein, distal end of the cath in the superior vena cava.
|
|
|
what must guardrails be used with
|
iv postassium, blood products, intralipids, peripheral parenteral nutrition (PPN), TPN
|
|
|
factors affecting infusion rates
|
if the site is inflamed, painful, leaking, slow IV to ko rate, call iv team
-position of arm -admin set -height of infusion bag |
|
|
what is blood coagulation and the clotting process called
|
hemostasis
|
|
|
what are the parts of blood coagulation
|
vasoconstriction
platelet aggregation / clumping instinsic pathway extrinsic pathway. |
|
|
intrinsic pathway
|
inside the body - ends when prothrombin converts to thrombin
|
|
|
extrinsic pathway
|
seen on the outside the body
|
|
|
hageman factor
|
chemical substance that is found in the circulating blood and happens after platelet aggregation.
|
|
|
clot resolution and anticlotting process
|
plasminogen is made in liver and found in plasma
|
|
|
where does the conversion of plasminogen to plasmin begin
|
with the activation of Hageman factor
|
|
|
what does plasmin do to the clot resolution
|
keeps vessels open and funcional by dissolving fibrin threads and resolving the clot
|
|
|
what are the contraindications to anticoagulation therapy
|
active bleeding
history of heparin-induced thrombocytopenia platelet count of <50,000 high risk for bleeding active intacranial lesions |
|
|
anticoagulants
|
given to prevent formation of new clots
does not disolve formed clots |
|
|
injectable heparin
|
acts immediatley after iv injection and within 30 mins
-injected q8-12hr or via continuous infusion |
|
|
what is the anticoagulant of choice for pregnant women
|
injectibale heparin
|
|
|
what are the side affects of heparin
|
hematoma, petechiae, bleeding gums, hematuria, fever, chills,
HIT |
|
|
oral warfarin - coumadin
|
effects occur in 3-5 days.
acts in liver to prevent synthesis of vitamin K |
|
|
cora
|
check vitals and PT
observe for bleeding review protocol for antidote avoid all asprin and asprin compounds |
|
|
what is fresh frozen plasma used for
|
to treat rx bleeding disorders caused by deficiency in clotting factors
|
|
|
what is one unit of FFP equal to
|
200-250ml
|
|
|
what is platelets used for
|
people with platelet deficiency or bleeding disorder.
|
|
|
one unit of platelets equals
|
30-60ml
|
|
|
what is albumin used for
|
to treat hypovolemic shock and low albumin levels
|

