![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
54 Cards in this Set
- Front
- Back
|
Reflux (aka backward flow) |
Flow of a body fluid in the direction opposite it's normal path |
|
|
Epispadias |
A congenital opening of the urethra on the dorsal side (top of penis) of the penis |
|
|
Hypospadias |
An abnormal congenital opening of the male urethra upon the undersurface of the penis |
|
|
Retroperitoneal |
Behind the peritoneal cavity |
|
|
Anatomy of the Kidney |

|
|
|
Cortex of the kidney |
The outer section of the kidney which covers the internal medulla |
|
|
Medulla of the kidney |

|
|
|
Renal cavity of kidney |
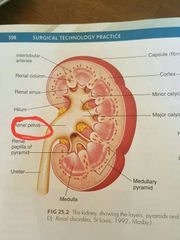
Widest part in the center of the kidney
As it projects from the kidney it becomes the top of the ureter
Is the collecting chamber in the middle of the kidney
Is where the renal tubules empty urine |
|
|
Calyces of kidney (plural for calyx) |
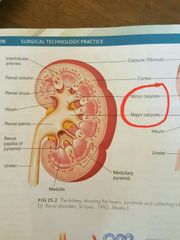
Are the recesses in the internal medulla, which in closes the renal papilla of pyramid
They are used to subdivided sections of the kidney, with distinction between major and minor calyces |
|
|
Renal artery |

Two renal arteries coming from the abdominal aorta |
|
|
Renal vein |

Two veins that extend from each kidney and open into the vena cava |
|
|
Nephron |
The functional unit of the kidney
Responsible for the purification and filtration of the blood
About 1 million in each kidney
Located within the cortex of the kidney |
|
|
Adrenal glands |
Paired organs that lie on the medial side of the upper kidneys
Produce norepinephrine and epinephrine |
|
|
Ureters |
Pair of thin muscular tubes that drain urine from kidneys to the bladder
Urine passes down through them by peristalsis which occurs three times a minute |
|
|
Bladder |
Hallow, muscular organ that functions as a temporary storage for urine
A full bladder holds about one liter of urine
Output is between 700ml and 2000ml each day |
|
|
Urethra |
Extends from the neck of the bladder to the exterior
Males: 7-8 inches in length
Connected to prostate gland
Also used to transport semen
Females: 1-2 inches |
|
|
Anatomy of penis |

|
|
|
Scrotum |

Lies at base of penis
Protects the testicles |
|
|
Testis |

Male gonads responsible for the production of sperm and testosterone
Connected to the abdomen by a spermatic cord and the cremaster muscle |
|
|
Epididymis |

A long-coiled tube that is cupped against the testis
Stores sperm until matured
Connects to the vas deferens |
|
|
Vas deferens (aka ductus deferens or seminal duct) |

Carries sperm from the epididymis to the ejaculatory duct
Enters the abdomen though the spermatic cord
Unites with seminal vesicle and forms the ejaculatory duct |
|
|
Seminal vesicle |

Tube-like glands
Lie behind the bladder
Makes about 70% of the content of semen or seminal fluid |
|
|
Ejaculatory duct |
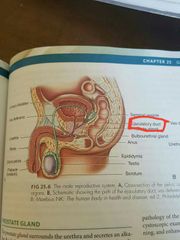
Formed where the seminal vesicle merges with the vas deferens |
|
|
Prostate gland |

Musculglandular structure
Size of a chestnut
Surrounds the bladder neck
Urethra runs through it
Secretes alkaline fluid to nourish and give mobility to sperm
|
|
|
Cowpers gland (aka bulbourethral glands) |
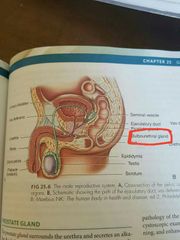
Secretes mucus, part of fluid that makes up semen
|
|
|
Male urethra |
Narrow fibromuscular tube that moves urine and semen externally |
|
|
What are the 4 sections of the male urethra |
Prostatic
Membranous urethra
Bulbar
Penile |
|
|
What does T.U.R.P. stand for and what is its definition? |
Transurethral resection of the prostate
Removal of the prostate gland using a cystourethral approach |
|
|
What is a Foley catheter? |
A urinary tract catheter with a ballon attachment at one end. After the catheter is inserted, the ballon is inflated to prevent the catheter from leaving the bladder |
|
|
What is a retention or indwelling catheter? |
A catheter designed to stay in the bladder for a time period. |
|
|
How does a 2-way Foley work? |
It has a double lumen-one for inflation of the ballon and the other for urinary drainage. |
|
|
How does a 3-way Foley work? |
The 3-way Foley has a larger ballon, either 30 ml or 75 ml. The larger ballon functions as a tamponade-a means of applying pressure at the bladder neck to stop hemorrhage following prostate surgery The third lumen is used to irrigate the bladder following prostate surgery or to instill medication |
|
|
Why do we do a T.U.R.P.? |
To treat benign obstructive enlargement of the prostate gland |
|
|
What is a penile prosthesis? |
An penile implant placed to treat impotence caused by an organic disease |
|
|
How does a penile prosthesis work? |
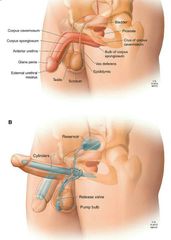
This system has 3 components
1. Inflatable cylinders are placed in the corpora covernosa of the penis
2. A saline reservoir is connected to the cylinders and implanted under the rectus muscle (abdominal cavity)
3. The pump that inflates and deflates the cylinders is placed in the scrotum |
|
|
What is a hydrocele? |
A benign, fluid filled sac that develops in anterior testis. |
|
|
What is a hydrocelectomy? |
The removal of a hydrocele. The hydrocele is drained and removed to prevent rupture and hemorrhage. It can be done open or endoscopically |
|
|
What are kidney stones? |
Stones in the kidney that are formed by the precipitation of specific salts from kidney filtration that have become supersaturated. Stones can become lodged in the kidney itself or can migrate to the ureters |
|
|
What are other terms used to describe kidney stones? |
Renal calculi Nephrolithiasis |
|
|
What does P.S.A. stand for? |
Prostate-specific antigen |
|
|
Why do we perform a P.S.A.? |
To check the levels of a protein that is procured by normal and malignant cells of the prostate gland. Malignant cells produce the protein at greater levels than nor.al cells. If you have a PSA value greater than 10 ng/mL (nanograms/milliliter) suggests that you are at a high risk for prostate cancer. |
|
|
What is mannitol (osmitrol)? |
IV osmotic diuretic; increases the osmolarity of the plasma, causing the osmotic pressure gradient to pull free fluid from the eye into the plasma, thereby reducing the IOP (intraocular pressure)
It is also non-conductive |
|
|
What are the contraindications of mannitol? |
Tobramycin |
|
|
Injectable solution of mannitol? |
5%
10%
15%
20%
25% |
|
|
What is a cystoscope? |
an instrument inserted into the urethra for examining the urinary bladder |
|
|
Resectoscope |
An instrument used to cut and coagulate tissue peice by piece. It is used in conjunction with endoscopic procedures to removes tumors or other tissue, such as the prostate |
|
|
Nonelectrolyte solutions |
Solutions that do not contain electrolytes. These must be used for bladder distention or continuous irrigation whenever electrosurgery is performed |
|
|
What irrigants can be used during a cystoscope procedure? |
Glycine-1.5% Sorbitol-3% Mannitol |
|
|
What is phimosis? |
Stenosis or narrowness of the preputial orifice so that the foreskin cannot be pushed back over the the glans penis |
|
|
What is the definition of undescended testis? |
An undescended testicle (cryptorchidism) is a testicle that hasn't moved into its proper position in the bag of skin hanging below the penis (scrotum) before birth. Usually just one testicle is affected, but about 10 percent of the time both testicles are undescended. |
|
|
How is an ellik used during a T.U.R.P procedure? |
It is used to remove tissue from the bladders lumen. |
|
|
What is a suprapubic prostatectomy? |
The removal of periurethral glandular tissue obstructing the outlet of the urinary tract through a transvesical approach. Usually through a low midline or Pfannenstiel incision |
|
|
What is a simple retropubic prostatectomy? |
It is the enucleation of hypertrophic prostatic tissue through an incision into the anterior prostatic capsule by an extra vesicle approach |
|
|
What is a simple perineal prostatectomy? |
The removal of the prostate gland through a perineal approach. |

