![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
90 Cards in this Set
- Front
- Back
|
What is the average transit time from the basilar layer to the granular layer of the skin?
|
Two weeks
|
|
|
What is the average transit time from the basilar layer to the top of the corneal layer of the skin?
|
Four weeks/one month
|
|
|
What structures make up the roads for the "superhighway of the cell?"
|
Microtubules
|
|
|
Name the keratin protein subtypes for the following cell layers:
a) Basilar b) Spinous c) Granular |
a) K5, K14
b) K1, K10 c) K2a |
|
|
Which of the following has both extra- and intracellular components: Desmogleins, Plakoglobulins, Desmoplakins, Desmocollins
|
Desmogleins and Desmocollins have both extra- and intracellular components
|
|
|
Which is responsible for the brown/black pigmentation of the skin: pheomelanin or eumelanin?
|
Eumelanin is an insoluble, mostly brown/black pigment of the skin. Pheomelanin is a red/yellow pigment found in large quantities in people with "fire red" hair.
|
|
|
What four locations can you find mature melanocytes?
|
1) epidermis and hair bulbs of the skin
2) uveal tract of the eye 3) the cochlea, and vestibular labyrinth of the ear 4) leptomeninges of the brain. |
|
|
What line of melanocytes does NOT come from the neural crest cells?
|
The melanocytes of the retina, which come from the optic cup.
|
|
|
What enzyme is the rate-limiting step in the production of melanin?
|
Tyrosinase, a copper-dependent enzyme at the top of the melanin synthesis pathway.
|
|
|
What is the pathogenesis of Waardenburg Syndrome?
|
Abnormal melanocyte migration, resulting in hypopigmentation and deafness.
|
|
|
How do melanocytes distribute their melanosome organelles to the surrounding Epidermal Melanin Unit?
|
By using their long, slender dendritic arms.
|
|
|
What cell type contains the majority of melanin in the skin?
|
Keratinocytes.
|
|
|
What receptor favors activation of the eumelanin pathway?
|
Binding of MSH (from the POMC precursor) to MCR-1. The AGOUTI gene product antagonizes the eumelanin pathway, promoting pheomelanogenesis.
|
|
|
Describe the pathogenesis of Dermal Melanocytosis (Mongolian Spots)
|
Arrest of melanocyte migration in the dermis.
|
|
|
What causes Piebaldism? What does it look like?
|
Problems with activation of the C-Kit gene leads to a lack of melanocyte proliferation. Many have a white forelock of hair and patches of persistent hypopigmentation.
|
|
|
How do patients with pan-hypopituitaryism present? What is their skin color?
|
Low MSH and ACTH production leads to a chalky-white appearance
|
|
|
How do patients with Addison's present? What is their skin color?
|
Primary adrenal insufficiency leads to high levels POMC expression, resulting in excess MSH and hyper-pigmentation.
|
|
|
What common acquired condition leaves patches of hypo-pigmentation?
|
The auto-immune disease Vitiligo
|
|
|
Name two exogenous skin pigments
|
1) Argyria - from the consumption of colloidal silver
2) Tattoos 3) Minocycline - from the consumption of tetracycline antibiotics. |
|
|
What are the four functions of a basement membrane?
|
Adhesion of the epithelium
Supply Polarity to the tissue Barrier functions Signal Transduction between epithelium and underlying connective tissue |
|
|
Mechanobullous Disorders
|
Epidermolysis Bullosa
|
|
|
What are the three classes of Epidermolysis Bullosa disorders?
|
1) EB Simplex: fragile skin just above the BMZ, within basal keratinocytes
2) Junctional EB: fragile within the BMZ 3) Dystrophic EB: fragile just below the BMZ, at the superficial dermis |
|
|
What two proteins are commonly mutated in EB Simplex?
|
Those produced by basal keratinocytes - Keratins 5 and 14
|
|
|
What cellular structure is most likely to be involved in cases of Junctional EB?
|
The Hemidesmosome. HDs allow basal keratinocytes to adhere to the lamina lucida of the basement membrane.
|
|
|
What three hemidesmosome proteins are modified in cases of JEB?
|
1) Plectin
2) a6b4 Integrin - also associated with plyloric atresia 3) Bullous Pemphigoid Antigen 2 - a.k.a. TXVII Collagen. |
|
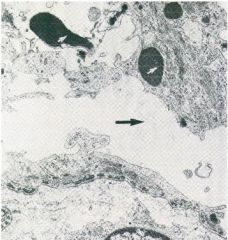
What type of blistering problem is this? What are the light and dark arrows pointing to?
|
Epidermolysis bullosa simplex
Dark Arrow: cleft in lower basal keratinocytes Light Arrow: clumps of abnormal keratin |
|
|
What non-hemidesmosome protein mutation can cause JEB?
|
The most severe types of JEB are caused by mutations in Laminin 5, an anchoring protein found in the lamina lucida.
|
|
|
What gene is always found to be mutated in cases of Dystrophic EB?
|
Type VII Collagen is always mutated in cases of Dystrophic EB.
|
|
|
Which is a transmembrane protein - Integrin or Laminin?
|
Integrin is a transmembrane protein. Mature Laminin proteins are found in the extracellular matrix.
|
|
|
Which Laminin protein subtypes are found within the skin's BMZ?
|
Laminins 1, 5, 6 and 7 are found in the BMZ.
|
|
|
What's the pathophys behind Bullous Pemphigoid?
|
BP patients have autoantibodies to both BPAg1 and BPAg2/TVII Collagen.
|
|
|
What are the disease characteristics of BP?
|
Bullous pemphigoid afflicts mostly older individuals (7th & 8th decade). Bullae are found on the extremities, groin and axilla.
|
|
|
What Immunobullous disorder attacks Laminin 5?
|
Cicatricial Pemphigoid. Typically scars the eyelids and conjunctiva, esophagus and trachea.
|
|
|
Define direct and indirect immunoflourescence.
|
Direct IF is a histologic technique using anti-IgG ABs to stain a patient's tissue specimen.
Indirect IF analyzes a patient's sera for the presence of autoimmune ABs. |
|
|
Explain the phenotype of Dysmorphic EB based on the molecular basis of disease.
|
Unlike non- or lightly-scaring epidermal syndromes, Dysmorphic EB involves fibrous scar formation in the dermis.
|
|
|
What are the three primary sub-types of Pemphigus?
|
1) pemphigus vulgaris - Desmoglein 3
2) pemphigus foliaceus - Desmoglein 1 3) paraneoplastic pemphigus. |
|
|
What is the underlying pathogenesis of Pemphigus Vulgaris?
|
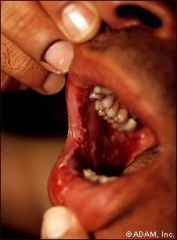
Auto-antibody attack of keratinocyte desmosomes, leading to intra-epidermal blistering.
|
|
|
Why are PV blisters rarely found intact?
|
The disunion of keratinocytes in the epithelium leads to a friable, fragile blister roof. Lesions are usually seen as erosions.
|
|
|
Why are bullous pemphigoid blisters usually found intact?
|
BP attacks BMZ proteins BPAg1 & 2, found in the lamina lucida. Blister roofs are more durable.
|
|
|
What proteins are targeted in the following immunobullous disorders:
1) Pemphigus vulgaris 2) Pemphigus foliaceus |
1) Pemphigus vulgaris- Desmoglein 3
2) Pemphigus foliaceus- Desmoglein 1 |
|
|
What are the three most common collagen types in the skin?
|
Type I - 80%
Type III - 10-15% Type V - 4% |
|
|
Type I Collagen supplies
|
Type I Collagen supplies tissue strength
|
|
|
Type III Collagen supplies
|
Type III Collagen supplies tissue compliance
|
|
|
Type IV Collagen is associated with
|
Type IV Collagen is associated with basement membranes, and is made by epithelial and endothelial cells
|
|
|
What's gone wrong in Ehlers-Danlos syndrome diseases?
|
Ehlers-Danlos Syndrome is a group of collagen synthesis defective diseases.
|
|
|
On average, how long does scalp hair grow in a month?
|
Scalp hair grows at approx. 1cm/month
|
|
|
How fast do fingernails grow?
|
Fingernails grow approx. 3mm/month
|
|
|
In what phase does hair actively grow: anagen, telogen, or catagen?
|
Hair actively grows in the anagenic phase.
|
|
|
What are the four types of hair shafts?
|
1) Terminal - thickest (scalp, eyebrows)
2) Vellus - most hair on the body 3) Intermediate - between terminal and velus 4) Lanugo - hair formed in utero, i.e. first hair |
|
|
What cytokines are associated with a TH-2 response?
|
IL-4, IL-5 and IL-10 are associated with a TH-2 response.
|
|
|
What cytokines are associated with a TH-1 response?
|
IL-2 and IFN-gamma are associated with a TH-1 response.
|
|
|
What are the circulating mediators of the innate immune system?
|
Complement, IL-1, TNF-alpha, INF-gamma and chemoattractants all function in the innate immune response.
|
|
|
Atopic dermatitis is associated with which immune response?
|
Atopic dermatitis, a.k.a. eczema or irritant dermatitis, is a TH-2/humoral response.
|
|
|
With what skin infection is atopic dermatitis commonly associated?
|
Staphylococcus aureus
|
|
|
What immune response is associated with Allergic Contact Dermatitis?
|
ACD follows a cytotoxic T-cell, or TH-1, path. Initially Langerhan's Cells mediate the response.
|
|
|
What causes telangiectasia?
|
Dilation and congestion/hyperemia of the superficial vascular plexus
|
|
|
What are the two causes of scaling of the skin?
|
Hyperorthokeratosis - retention of the granular cell layer and cornified cell layer
Hyperparakeratosis - thinning or absence of the granular layer, cornified layer retain nuclei |
|
|
What cytoskeletal structure is at issue with Epidermolysis bullosa simplex and Bullous congenital ichthyosiform erythroderma/epidermolytic hyperkeratosis?
|
They both involve problems with Keratin/Intermediate Filaments.
|
|
|
What extracellular molecule is associated Bullous pemphigoid?
|
Type XVII Collagen, or BPAg2
|
|
|
Are the Epidermolysis Bullosa disorders typically acquired or congenital?
|
Typically congenital
|
|
|
What are the common Pemphigoid disorders?
|
1) Bullous pemphigoid - geriatric, extremities, BPAg1 & 2
2) Pemphigoid Gestationis - Pregnancy, BPAg2 3) Cicatricial Pemphigoid - Laminin 5 |
|
|
EB Simplex
|
Epidermolysis Bullosa Simplex:
1) Fragile skin at keratinocytes 2) Mutations in K5 & 14 |
|
|
What is characteristic of Junctional EB?
|
1) Fragile WITHIN basement membrane
2) Affected proteins: plectin & BPAg1, A6B4 integrin, Laminin 5 |
|
|
Acanthosis
|
Thickening of the spinous layer. Found in warts, molluscum, and psoriasis
|
|
|
What is one of the molecular etiologies of psoriasis?
|
Abnormal Keratin type switching. Should be to from K1 & 10, in psoriasis mistakenly switched to K6 & 16
|
|
|
Bullous congenital ichthyosiform erythroderma (BCIE)
|
1) Histo: clumping of keratin and keratohyalin in suprabasilar keratinocytes.
2) Caused by genetic defect in keratins K1, K10, K2e (Disase aka epidermolytic kyperkeratosis (EHK)) |
|
|
What disease is caused by a mutation in the keratinocyte enzyme transglutaminase?
|
Nonbullous congenital ichthyosiform erythroderma (NCIE)
1) Thick scale & erythema 2) Defects in cornified cell layer (Disease aka Lamellar ichthyosis) |
|
|
What skin disease is caused by a deficiency in steroid sulfatase?
|
X-Linked recessive ichthyosis
1) Large dark scale, central attachment 2) Enzyme deficiency results in an accumulation of cholesterol sulfate 3) Can't desquamate |
|
|
What three diseases are associated with Type VII Collagen?
|
Dystrophic EB (congenital) - fragile just below the BMZ
Epidermolysis Bullosa Acquisita (acquired) - assoc. with IBD, RA, MM, extensor surface erosions Linear IgA Dermatosis (acquired) - ring-shaped, diag. with immunofluorescence |
|
|
What disorder is associated with Irritable Bowel Syndrome, Rheumatoid Arthritis and Multiple Myeloma?
|
Epidermolysis Bullosa Acquisita
|
|
|
What disease is associated with a mutation in Type IV collagen?
|
Alport's Syndrome. No skin manifestations, but presents with glomerulosclerosis
|
|
|
What elastin deficiency causes "hound dog" faces?
|
Cutis Laxa
|
|
|
Match the types: Lepromatous and Tuberculoid with TH1 and TH2
|
Lepromatous Leprosy <-> TH2: poor outcome
Tuberculoid Leprosy <-> TH1 |
|
|
What skin infection is pathomneumonic with coral-red fluorescence on Wood's lamp exam?
|
The bacterial skin infection Erythrasma glows coral-red under UV light. Cause is Corynebacterium. Looks like a yeast infection.
|
|
|
What clinical sign differentiates Erysipelas from generic Cellulitis?
|
Erysipelas (GAS infection) presents with well demarcated erythematous borders due to its epithelial origins.
Cellulitis, a dermal infection, appears much more diffuse. |
|
|
What are the "Big Three" dermatophytes?
|
Trichophyton, Epidermophyton and Microsporum - the "Tinea Three"
|
|
|
What pigmenting skin infection grows well in humid climates?
|
Tinea versicolor (Malassezia furfur) - Spag and meatballs on KOH. May be hypo- or hyper-pigmented.
|
|
|
What wavelength of UV light causes immediate pigment changes?
|
UVA exposure causes photo-oxidation of preexisting melanin.
|
|
|
What is the cause of delayed tanning?
|
UVB exposure is the cause of the delayed tanning response.
|
|
|
Physiologically, what happens during the delayed tanning response?
|
Melanocyte numbers increase, as well as melanosome synthesis and transfer.
|
|
|
Spongiosis is
|
an exudative collection edema fluid between keratinocytes that stretches the intracellular bridges
|
|
|
What two broad-functioning cytokines trigger the innate immune response?
|
Interleukin-1 (IL-1) and Tumor Necrosis Factor alpha (TNFa)
|
|
|
What are the two primary cytokines responsible for a TH1 response?
|
Interleukin-2 (IL-2) and Interferon-gamma (INF-g) stimulate a cytotoxic TH1 T-Cell response.
|
|
|
What are the three primary cytokines of a TH2 response?
|
Think flyfishing "10 and 2": TH2 response is generated by IL-10, as well as IL-4 and IL-5
|
|
|
What effect does IL-12 have on undifferentiated T-Cells?
|
IL-12 stimulates the production of TH1 cells, and inhibits the production of TH2 cells.
|
|
|
What endothelial ligand binds T-Cell Cutaneous Lymphocyte Antigen (CLA)?
|
E-selectin, expressed on dermal capillary endothelial cells, is a "homing signal" for T-Cells headed for the skin.
|
|
|
What are the three stages of cancer in the Multistage Model for Photocarcinogenesis?
|
Initiation: mutation of a target gene
Promotion: external forces lead to clonal expansion Progression: further genetic damage leads to cancer |
|
|
What two tumor suppressor genes are most important in non-melanomatous skin cancer?
|
p53 and PTCH (patched)
|
|
|
What gene is associated with Familial Melanoma?
|
CDKN2A, aka p16
|
|
|
A defect in what gene is responsible for Basal Cell Nevus Syndrome?
|
PTCH (patched).
|

