![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
81 Cards in this Set
- Front
- Back
|
Oxygen Tank Storage |
Storage area must be: clutter-free, cool and dry, away from heat/open flame; Tanks must be upright and secured (chained to wall, in stands, or on carts); Caps/lids must be over valves for all tanks not in use; If a tank were to fall over the cap/lid would protect the valve from being broken off |
|
|
Oxygen Tank Dangers |
If the tank falls or is dropped and the valve is broken, the tank becomes a TORPEDO; High velocity can go through cement walls; Can seriously injure veterinary medical staff and patients; Store appropriately and handle with caution |
|
|
Oxygen Tank Tags |
All tanks come with tags that indicate whether the tank is full, in use or empty; VT tears off the bottom of the tag to indicate the tanks status; When the tank is empty "In Use" portion of the tag is removed |
|
|
Oxygen Tank Gauges |
Oxygen tank pressure is 2200 psi when full; If the gauge reads less than 500 psi, do not use; Line pressure is the pressure in the line trough which oxygen flows to get to surgery, radiology room (etc.) which should be 40-60 psi
|
|
|
Oxygen Tank Gauge for V115 |
There is a panel outside surgery that alerts staff if the line pressure is too high or too low |
|
|
Pressure Reduction Valve |
Reduces the pressure to a safe operating pressure of 40-50 psi |
|
|
Oxygen Flow Rate |
1-3 L/min - >10kg; 3-5L/min- < 10kg; Metabolized by the lungs- be aware of gas escaping from the sides of the mask |
|
|
Chamber/Tank Induction |
Often used for wildlife and fractious feline patients; Oxygen flow rate is 5 L/min |
|
|
Inhalant Anesthesia |
Depresses the CNS to cause unconsciousness; Different inhalants have varying degrees of muscle relaxation, different analgesic effects, and different effects on organ system functions |
|
|
Daily Anesthetic Equipment Maintenance |
wash with warm water and germicidal soap (NOT chlorhexidine); Scrub inside of ETTS with a brush (pipecleaners for small ones); Rinse thoroughly and air dry; When cleaning and drying leave cuff inflated |
|
|
Weekly Anesthetic Equipment Maintenance |
Use washing machine with water and germicidal cleaner and agitate slightly on gentle cycle; Place ETT's, reservoir bags and breathing circuit into a mesh bag and let soak; After soaking run the machine through the entire gentle cycle; Let items dry overnight- hang up breathing circuits |
|
|
Anesthetic Equipment Used on Contagious Animals |
Either: Throw it all away, use a disposable circuit, or; Disinfect completely by going through the weekly cleaning process, or; Gas sterilization (sporocidal and bacteriocidal) |
|
|
Anesthetic Machine Weekly Cleaning |
Soak the following part for 20-30 minutes with chlohexidine solution: Empty soda lime canister, inspiratory and respiratory valves and domes; Rinse well and air dry overnight; Clean parts of machine that cannot be soaked with cloth containing chlorhexidine solution and rinse; Clean out castors- wheels to roll it around |
|
|
Maintaining Normothermia- Hypothermia |
Decrease in core body temperature; Animals require less anesthetic due to potential over-dose- rate of metabolism by the liver enzymes is decreased - longer lasting drugs; Increased wound healing time; In recovery- can shiver now- requiring more oxygen (200-600%); Can cause problems in patients with cardio pulmonary disease |
|
|
Causes of Hypothermia |
Vasodilation (drugs); Patients under anesthetic- cold and dry oxygen cause animals to cool down; During surgery- open and will lose lots of heat; Reduced circulation, HR & BP; Opioids mess with thermoregulatory center of the brain; Surgical suite is cold; Shaved areas and swab; Surgery table is metal=cold; Cannot shiver to warm themselves; IV fluids are colder than the animals body temp- drops to 0.25 degrees celcius/hr |
|
|
Pre-Therm Method to Maintain Normothermia |
Mattress that provides even warming across the whole blanket |
|
|
Circulating Hot Water Blanket Method to Maintain Normothermia |
Reservoir and blanket must be on the same level- equal height; Must put a blanket on top of the blanket |
|
|
Bair Hugger Method to Maintain Normothermia |
Reverse vacuum blowing warm air onto the patient (tiny holes on one side blowing the air at the patient) |
|
|
Hot Dog Method to Maintain Normothermia |
Electrically conductive fabric that provides even heating across the entire blanket; Has bungee cords to wrap the blanket over on intself |
|
|
Majic Bag Method to Maintain Normothermia |
Caution when using- can have burn injuries from them; Must mix oats before placing with patients and wrap in a blanket |
|
|
Hot Water Bottles Method to Maintain Normothermia |
Put something between the animal and the bottle; Best between hind legs; Dry the bottle before placing on patient to avoid steam burns |
|
|
Other Methods to Maintain Normothermia |
Socks, body heat, garbage bag- put patient inside to avoid getting wet during dental procedures, IV fluid tube passed through a bowl of warm water, hot water in a sink, and put IV bag in a sink and wrap in a towel |
|
|
Anesthetic Drug Protocols |
A good combination of drugs used to sedate difficult cats for procedures such as x-rays; Kitty Majic: 0.1mL dexmedetomidine, 0.1mL ketamine, 0.1mL butorphanol
|
|
|
Anesthetic Procedure |
History/physical exam of patient/ diagnostic tests; Anticipated problems- hypotension, hpoventilation, hypothermia, decreased tear production; Premedication/Patient Preparation- Venous access, patients pain-free (stop pain before it starts); Induction- rapid loss of consciousness, no excitation, rapid airway control (intubate quickly); Maintenance- typically by inhalant anesthesia (few contraindications) |
|
|
Anestetic Procedure of Patient Monitoring |
Patient support- aiway protection, fluid administration, heat supplementation, respiratory support - fresh O2 and giving IPPV when they aren't breathing on their own, artificial tears- lost blink reflex and prevent corneal ulcers |
|
|
Pop-Off Valve |
AKA pressure relief valve and exhaust valve; 2 types: typical, and a press down to close |
|
|
IPPV |
Intermiten Positive Pressure Ventilation; Maximum pressure= cats+small dogs- 8-10 cm of H2O, medium dogs= 12-15 cm of H2O, large dogs= 15-20 cm of H2O; Atelectasis - animals are taking shallower breaths (alveoli collapsing slightly); Done every 5 minutes |
|
|
Methods of Sterilization |
Autoclave, cold sterilization, and gas sterilization |
|
|
Autoclave |
Recall the 3 basic principals: heat, pressure, and time; In order to be effective, surgical packs must be exposed to the proper temperature for a sufficient length of time |
|
|
Autoclave Tuttnauer Times |
Sterilization- 45 minutes from cold, and 35 minutes from warm; Dry time- 20-30 minutes |
|
|
Autoclave Temperature |
273 degress Farhenheit |
|
|
Autoclave Structure |
Central sterilizing chamber; Trays inside chamber hold surgical packs; Seal created by rubber gasket when the door closed; Temperature/pressure gauges, dial for setting time, button to set sterilized and dry cycles; Water reservoir and pressure release valve |
|
|
Autoclave Overview of Operation |
Water is allowed to flow into the chamber; Surgical packs loaded; Door closed tightly; Temperature and pressure build up; Steam condenses on objects; Pressure in chamber released when sterilization cycle complete; Door opened- packs go through drying cycle |
|
|
Autoclave Items Sterilized Using Steam Sterilization |
Glassware; Stainless steel instruments; Some plastics; Some types of rubber; Surgical gowns; Surgical drapes |
|
|
Autoclave Important Points to Remember |
High pressure in autoclave chamber- do not attempt to open door until pressure released; Items in autoclave are hot- use caution when removing; For adequate sterilization steam must be able to circulate- item should be packed loosely in the autoclave |
|
|
Monitoring Steam Sterilization Commercial Test Vials |
When assessing auto; Glass vial- inoculated with spores, autoclave should kill them- send vial to lab and they will culture it- if the bacteria grows autoclave is not working; Usually done at least once a year |
|
|
Material Needed for Autoclaving: Recap |
Distilled water; Oven mitts; Sterilization indicators/autoclave tape |
|
|
Cold Sterilization |
Often referred to as "cold sterile"; Liquid chemical disinfection; Involves immersion of instruments in chemical solution; Effective primarily against vegetative bacterial forms- therefore, more accurate to call it "cold disinfection"; Instruments must be immersed for sufficient time |
|
|
Cold Sterilization Equipment |
Nail clippers for declaws, individual instruments such as hemostatic forceps, dental instruments |
|
|
Gas Sterilization |
Uses ethylene oxide- is colourless, flammable and explosive; Kills all microorganisms (highly sporacidal); Highly toxic- irritating to skin and mucous membranes; Prevents replication of microorganisms by inactivating DNA; Requires special chamber, to contain gas, and proper ventilation; Items must air out for period of 24 hours |
|
|
Items for Gas Sterilization |
Endotracheal tubes; Rubber catheters; Syringes; Intravenous catheters; Needles |
|
|
Scissors |
Man different types; Used for such tasks as removing sutures, dissecting tissue during surgery, or cutting bandage material |
|
|
Stage 1 of Anesthesia |
Immediately after inhalation or injectable agent administered; Decreased sensitivity to pain; All reflexes present; Patient may struggle, urinate, defecate or show other signs of fear or anxiety |
|
|
Stage 2 of Anesthesia |
Begins with loss of consciousness; All reflexes present- may appear exaggerated; Animal can chew and swallow- may yawn; Brain starts to lose control of voluntary bod functions- animal may exhibit involuntary excitement: rapid limb movement, vocalization, struggling; Breathing may be irregular or animal may appear to hold its breath; Potentially unpleasant for patient and hazardous for staff; Epinephrine release, cardiac arrhythmias and arrest; Important to ensure smooth passage to Stage 3 |
|
|
Stage 3 of Anesthesia |
Subdivided into 4 planes- each indicates increasing anesthetic depth |
|
|
Stage 3 Plane 1 |
Light plane or anesthesia; Respiratory pattern becomes regular; Limb movement cease; Eyeballs begin to rotate ventrally; Gag and swallow reflexes depressed; Pedal palpebral reflexes present but weaker |
|
|
Stage 3 Plane 2 |
Medium plane of anesthesia- suitable for most surgical procedures; Eyeballs rotate ventromedially; Respiration regular but shallow; RR, HR, and BP decreased; Pedal and swallowing reflexes lost; Laryngeal and palpebral reflexes are weakened or lost |
|
|
Stage 3 Plane 3 |
Deep plane of anesthesia; HR, BP, and RR decrease- increases CRT; Eyeball position is central |
|
|
Stage 4 of Anesthesia |
Plane 4; Early anesthetic overdose; Marked drop in HR and BP; CRT is prolonged- pale MM; Abdominal breathing - inadequate ventilation; Pupils dilate- pupillary light reflex is lost (PLR); Too deep an anesthetic plane- animal in risk of cardiopulmonary arrest (CPA) |
|
|
Stage 4 Result |
Respiration ceases; Cardiac Arrest; Death; Resuscitation of patient required |
|
|
Reflexes |
Healthy animals respond to different stimuli; Reflexes lost with anesthesia- monitored to help determine depth of anesthesia |
|
|
Palpebral Reflex |
Blink reflex; Lightly tap medial or lateral canthus of eye; Loss of this reflex dependent upon drugs used |
|
|
Swallow Reflex |
Lost at medium depth of anesthesia; Regained just before patient regains consciousness; Once returns, safe to remove ET tube |
|
|
Pedal (toe pinch) Reflex |
Patient withdraws limb in response to pinching of a digit or pad; Helpful for mask inductions (when assessing other reflexes difficult) |
|
|
Pupillary Light Reflex |
Constriction (miosis) of pupils in response to light |
|
|
Corneal Reflex |
Touch cornea with sterile object and note whether blinks; Not commonly used in dogs and cats (used primarily for large animals) |
|
|
Laryngeal Reflex |
Stimulated when larynx touched by object; This reflex protects animal from aspiration into lungs; Present during intubation if animal not sufficiently anesthetized |
|
|
Muscle Tone Reflex |
Deeper anesthesia increases muscle relaxation; One example is jaw tone- is lost when animal anesthetized |
|
|
Monitoring Equipment |
Assists with monitoring patients during general anesthesia; Does not replace the senses of the veterinary technician |
|
|
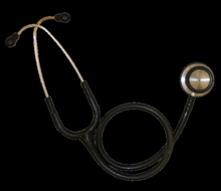
Regular stethoscope; Sound vibrate plastic disk and send sound waves to ear pieces; Maintain asepsis- ensure sterile surgical field not contaminated when auscultating heart and lungs |
|
|
Why might heart rate be difficult to hear when patient is under anesthesia? |
Strength of heart contractions diminished due to anesthetic drugs; Position of heart (gravity)- patient in dorsal recumbency or in lateral recumbency |
|
|
Information that can be acquired using a regular stethoscope |
Heart rate; Heart abnormalities; Respiration rate; Quality of respiration; Abdominal Sounds |
|

|
Esophageal Stethoscope; Placed in esophagus of patient; Amplifies sounds of heartbeat |
|
|
Esophageal Stethoscope |
Has a variety of catheter sizes; Measure the catheter from the nose to the 5th rib; Lubricate catheter- water or lubricant; Can be attached to an audio monitor; Used to acquire heart rate and heart rhythm; If using a stethoscope tube, can clip ear pieces to the surgery table (for storage during surgery) |
|
|
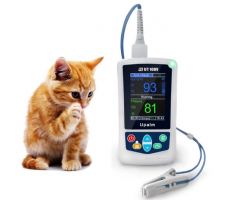
Pulse Oximeter; Probe is clipped to pink/non-pigmented tissue- tongue, lip, inside of pinna, between toes, vulva/prepuce, skin of abdomen (shaved); Also a rectal probe |
|
|
Information Acquired from a Pulse Oximeter |
Pulse -NOT heart rate; Saturation of oxygen in the hemoglobin of the RBC's |
|

|
Doppler Blood Pressure Monitor; To use, shave the area between the metacarpal and the carpal pads (front, back or tail); Appropriate size of cuff on patient just below the elbow; Attach the cuff to the sphygmomanometer; Palpate for pulse; Place ultrasound get on probe- concave side; Place probe on shaved area; Inflate cuff to 20mm above when last heard pulse; Deflate the cuff slowly- systolic pressure read at point that round returns |
|
|
Doppler Blood Pressure Monitor |
Amplifies sound of pulse- "whoosh whoosh"; Acquires systolic blood pressure (mm Hg), and pulse; Do not use cleaning solution or alcohol to clean the probe (water only) |
|

|
ApAlert; Detects apnea- cessation of breathing; Beeps each time a patient exhales; Adapter connects to ETT and breathing circuit; Sensor detects temperature changes between the warm exhaled air and cool inhaled air; Will alarm if animal does no breathe in set period of time |
|
|
ApAlert Attachment |
Can increase mechanical dead space |
|
|
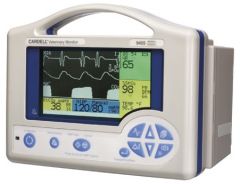
Capnograph; AKA End-Tidal CO2 monitor; Different brands; One of the functions of the Cardell |
|
|
Information Acquired From using the Capnograph |
Monitors breathing by measuring exhaled (end tidal) CO2 and inhaled CO2; End tidal CO2=EtCO2; Inhaled CO2=inspCO2 |
|

|
ECG; AKA electrocardiogram; Another function of the Cardell monitor; Acquires the rhythm of the heart- helps diagnose arrhythmias and a variety of heart problems |
|
|
Oscillimetric Blood Pressure Monitor |
Blood pressure measuring device that automatically inflates and deflates the blood pressure cuff; Can be set to measure pressure every 1, 2, 3, 5, 10, 45, and 60 minutes; Another function of the Cardell |
|
|
Information acquired by the Oscillometric Blood Pressure Monitor |
Systolic BP; Diastolic BP; Mean Arterial Pressure (MAP); Pulse; NOT RELIABLE IN PATIENTS UNDER 5KG |
|
|
Heart Rate Under Anesthesia |
Dogs: 70-120 Cats: 130-170 At Rest= Dogs: 70-160 Cats: 150-210 |
|
|
Respiratory Rate Under Anesthesia |
Dogs: 8-15 Cats:12-18 At Rest= Dogs: 8-20 Cats: 8-30 |
|
|
Rectal Temperature Under Anesthesia |
Dogs: 38 Cats: 38 At Rest= Dogs: 37.5-39 Cats:38-39 |
|
|
Systolic Blood Pressure Under Anesthesia |
Dogs: 120 (Intervene is <90, >170) Cats: 120 "" At Rest= Dogs: 100-160 Cats: 100-160 |
|
|
MAP (mm Hg) Under Anesthesia
|
Dogs:100 (Intervene is <90, >170)
Cats:100 "" At Rest= Dogs:80-120 Cats:80-120 |
|
|
Saturation of Hemoglobin with Oxygen on Room Air Under Anesthesia |
Dogs:98% Cats:98% At Rest= Dogs:99-100% Cats:99-100% |

