![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
40 Cards in this Set
- Front
- Back
|
There are four general components of repair by fibrosis, what are they?
|
-Formation of new blood vessels (angiogenesis)
-Migration and proliferation of fibroblasts -Deposition of ECM -Maturation and reorganization of fibrous tissue |
|
|
Repair begins within _____ hours?
|
24 hours
|
|
|
Repair by Fibrosis causes emigration of fibroblasts and endothelial cell proliferation. By 2-5 days, what tissue is present?
|
At 3-5 days, granulation tissue is apparent,
|
|
|
Appearance of granulation tissue is characterized by:
|
-Proliferation of fibroblasts
-macrophages -myofibroblasts with contractile actin |
|
|
Histologically compare Granulation tissue to a healed (scarred) myocardial infarction.
|
Granulation tissue has myofibroblasts with pinkish type 3 collagen.
A healed scare will be avascular, with dense CT (dense fibrosis) |
|
|
Blood vessels are assembed by what two processes?
|
1.) Vasculogenesis: assembed from angioblasts during embryonic development
2.) angiogenesis: -preexisting vessels send out sprouts to make new vessels |
|
|
The four general steps in new capillary vessel development are :
1.) proteolytic degradation of parent vessell BM 2.) Endothelial cell migration toward an angiogenic stimulus. What are the last two steps? |
3.) Proliferation of endothelial cells behind leading edge
4.) Maturation of endothelial cells; including recruitment of pericytes and smooth muscle cells for support. |
|
|
New vessels are leaky due to incomplete interendothelial junctions. The most important factors that induce angiogenesis are:
|
1.) basic fibroblast growth factor (bFGF)
2.) Vascular endothelial growth factor (VEGF) |
|
|
What do angiogenic factors like bFGF and VEGF cause?
|
-proliferation
-endothelial cells to secrete proteinases to degrade BM -endothelial cell migration -direct vascular tube formation |
|
|
Regarding angiogenesis, structural ECM proteins regulate ______________ while nonstructural ECM proteins ______________.
|
structural ECM proteins regulate vessel sprouting via integrins
Nonstructural ECM proteins: -destabilize cell-ECM interactions and also facilitate cell migration via thrombospondin and tenascin C |
|
|
Angiogenesis starts with little capillary buds with no lumen. Describe the growth of a BV.
|
Capillary "bud-cells" begin migrating outwards and proximal cells b/g dividing. Eventually, migrating cells form arcades with other migrating cells in the middle and the bud acquires a lumen. Finally, smooth muscle comes along and adheres to the outside.
|
|
|
Fibrosis (scar formation) builds on what type of tissue?
|
builds on granulation tissue framework of new vessels and loose ECM.
|
|
|
What are the two steps of fibrosis?
|
1.) emigration and proliferation of fibroblasts into site of injury.
2.) deposition of ECM by these cells |
|
|
Recruitment and stimulation of fibroblasts are driven by what three Growth factors?
|
1.) Platelet derived growth factor (PDGF)
2.) bFGF 3.) TGF-B |
|
|
During scar formation these cells are important because they elaborate growth factors and other medaiators that induce fibroblast proliferation.
|
Mononuclear cells (specifically Macrophages)
No neutrophils because the wound is clean by now. |
|
|
Collagen synthesis is critical to development of strength in would healing. What makes collagen and when?
|
Fibroblasts begin making collagen early (3-5 days) and continues for weeks.
|
|
|
Collagen synthesis is induced by what 3 molecules?
|
1.) Growth factors (PDGF, bFGF, and TGF-B)
2.) cytokines (IL-1) 3.) tumor necrosis factor (TNF) |
|
|
Granulations tissue is used as a scaffold to make a scar which is composed of what materials?
|
Inactive fibroblasts and collagen
|
|
|
Bacterial produces or other immune complexes activate macrophages to secrete _______ and ________. These initiate fever, endothelial cell effects, fibroblasts proliferation and other cytokine secretion.
|
IL-1/TNF
|
|
|
Degradation of collagens and other ECM components occurs by metalloproteinases. There are three important classes:
|
1.)interstitial collagenases
cleave fibrillar col I, II, III 2.) gelatinases (type IV) collagenases) that degrade amorphous col and fibronectin. 3.) stromelysins: -variety of ECM such as proteoglycans, laminin, fibronectin or amorphous collagen. |
|
|
Degradation of scar or "scar remodeling" is mainly controlled by what enzyme class?
|
Metalloproteinases
|
|
|
Activated collagenases (metalloproteinases) can be rapidly inhibited by:
|
Tissue inhibitors of metalloproteinases (TIMPs)
These prevent the collagenases from overchewing collagen |
|
|
Metalloproteinases are made by fibroblasts, macrophages and neutrophils and are regulated by:
|
-growth factors
-cytokines -phagocytosis Inhibited by TGF-B inhibited by steroids |
|
|
Since metalloproteinases are inactive, they must first be activated by:
|
-chemicals (HOCl. radical)
-Proteases(plasmin) |
|
|
Healing by first intention or primary union is healing of clean uninfected incision that causes only focal disruption of BM. What type of generation is occuring?
|
Epithelial regerneration predominates over fibrosis.
|
|
|
Within 24 hours of first intention healing, what is happening?
|
-neutrophils at incision margin migrating toward the fibrin clot.
-Basal cells at incision margin exhibit an increase in mitotic activity. |
|
|
Within 48 hours of first intention healing, what is happening?
|
Epithelial cells proliferate and deposit basement membrane components and cells meet in midline beneath the scab in a thin but continuous epithelial layer.
|
|
|
Day 3 of first intention healing, what is happening?
|
-Macrophages replaced neutrophils
-Granulation tissue invades incision space -collagen fibers are evident at incision margins -Fibers are vertically oriented and do not bridge incision -epithelia thickens and epidermal covering layer. |
|
|
Day 5 of first intention healing, what is happening?
|
-Neovascularization stops
-collagen increases and bridges incision -epidermis recovers its normal thickness -surface keratinization |
|
|
During the second week of healing by first intention, collagen continues to accumulate and you have increase fibroblasts. What three things are diminished?
|
WBC's, edema and vascularity
|
|
|
What is blanching?
|
Increasing collagen deposition and regression of blood vessels; Mature scar.
|
|
|
At what time during the healing by first intention is a scar
1.)devoid of WBCs and covered by epidermis 2.)dermal appendages destroyed by incision are lost* 3.) Tensile strength of the wound increases with time |
End of the first month
|
|
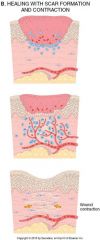
Not a questions!!
|
Not a question
|
|
|
This is a type of wound healing caused by cell or tissue loss, infarction, inflammatory ulceration, abscess or large wounds.
|
Second Intention
|
|
|
healing by second intention is more complex because parenchymal cells alone cannot heal; how is healing done?
|
Healing is by regeneration and fibrosis;
There is more granulation tissue but bulk of wound is fibrosis |
|
|
Second intention healing differs from First intention healing in several ways:
1.)Non-opposed wound margins 2.) Large tissue defects have a more necrotic debris, exudate and fibrin what is 3 and 4? |
3.) More granulation tissue
4.)Myofibroblasts-->wound contraction within 6 weeks |
|
|
What is the single most important cause of delay in healing?
|
Infection
Glucocorticoids can also delay wound healing b/c of anti-inflammatory effects |
|
|
What are the facts that interfere with repair:
1.) Infection 2.)Nutrition 3.) Glucocorticoids (steroids) what other 3 things? |
4.) Mechanical
5.)Poor perfusion 6.) Foreign bodies |
|
|
What are keloids?
|
-accumulation of collagen
-hereditary in blacks and asians |
|
|
Exuberant granulation (proud flesh) is:
|
Excessive granulation tissue
-abnormal cell growth and ECM production -hinders re-epithelialization -Cautery or surgical resection is necessary for restoration of epithelial continuity. |

