![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
109 Cards in this Set
- Front
- Back
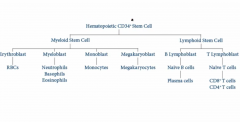
|
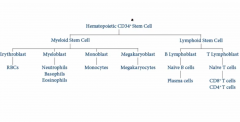
|
|
|
Normal WBC
|
5-10K
|
|
|
Leukopenia
|
Low WBC
|
|
|
Leukocytosis
|
High WBC
|
|
|
Neutropenia
|
Low # of neutrophils
Can be caused by: - Drug toxicity - Severe infection |
|
|
What do you treat neutropenia with?
|
GM-CSF or G-CSF - boosts granulocyte production
|
|
|
Lymphopenia
|
Low # of lymphocytes
Caused by: - Immunodeficiency (pt w/ DiGeorge) - High cortisol state (pt w/ Cushings) - Autoimmune destruction (pt w/ Lupus) - Whole body radiation |
|
|
Most sensitive cell to radiation
|
Lymphocyte
|
|
|
Neutrophilic Leukocytosis
|
High # of neutrophils
Caused by: - Bacterial Infection - Tissue necrosis - High cortisol state (disrupts the adhesion of marginated pool of neutrophils, increasing their number in the blood) |
|
|
CD16
|
Marker for Fc reeceptor
|
|
|
Immature neutrophils
|
Decreased CD16, Decreased ability to bind to Fc receptor. Increase in neutrophils --> increase in immature neutrophils --> can't bind to immunoglobuilin
|
|
|
Monocytosis
|
Caused by chronic inflammatory states, malignancy
|
|
|
Eosinophilia
|
Caused by:
Allergic reactions Parasites Hodgkin Lymphoma (due to increase in IL-5) |
|
|
Basophilia
|
CML
|
|
|
Lymphocytic Leukocytosis
|
Caused by:
Viral infections Bordetella pertussis (produces lymphocytic leukocytosis promoting factor --> prevents lymphocytes from entering lymph node) |
|
|
Infectious Mononucleosis
|
- EBV infection --> lymphocytic leukocytosis composed of reactive CD8+ T cells
- CMV is the less common cause - Virus transmitted by saliva; classically infects teens |
|
|
EBV primarily infects
|
- Oropharynx
- Liver - B cells |
|
|
CD8+ T cell response to Infectious Mononucleosis
|
- Generalized LAD (lymphadenopathy - enlarged lymph nodes --> hyperplasia of paracortex)
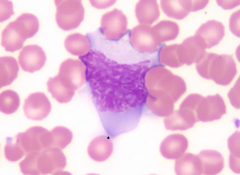
- Splenomegaly (periarterial lymphatic sheath) - High WBC with atypical lymphocytes (CD8+ T cells --> nucleus is large, abundant cytoplasm, very large cell - almost looks like a monocyte) |
|
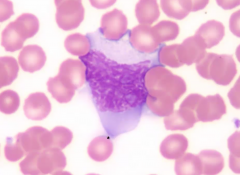
Infectious Mononucleosis
|
|
|
|
Monospot Test
|
- Used for screening infectious mononucleosis
- Detects IgM heterophile Abs - Usually turns pos w/i 1 week after infection - Neg test suggests CMV cause - definitive diagnosis is done by testing for EBV viral capsid antigen |
|
|
Complications of Infectious Mononucleosis
|
- Increased risk for splenic rupture (get splenomegaly; ask pt w/ mononucleosis to avoid contact sports for at least 1 year)
- Rash if exposed to PCN - Dormancy of virus in B cells (increased risk for recurrence, increased risk for lymphoma) |
|
|
Acute Leukemia
|
Disruption in ability of blasts to mature (neoplastic proliferation of blasts)
Accumulation of > 20% blasts in bone marrow |
|
|
Effects of increased blasts
|
They crowd out normal hematopoiesis
Results in acute presentation w/ anemia, thrombocytopenia, or neutropenia Blasts usually enter in blood resulting in a high WBC |
|
|
Blasts
|
Large, immature cells, often with punched out nucleoli on a blood smear
|
|
|
AML
|
Accumulation of myeloid blasts
Marker: MPO (myeloperoxidase) --> can crystalize into Auer rod |
|
|
ALL
|
Accumulation of lymphoid blast
TdT + (DNA Pol) --> marker |
|
|
ALL
|
Neoplastic accumulation of lymphoblast
Pos. nuclear staining for TdT (DNA Pol) TdT is absent in myeloid blasts and mature lymphocytes Most commonly arises in kids Associated with Down syndrome (after 5 y/p) |
|
|
B-ALL
|
- Most common type of ALL
- Lymphoblasts classically express CD10, CD19, CD20 - Excellent response to chemo (requires prophylaxis to scrotum & CSF) - Prognosis based on cytogenic abn t(12;21) -- good prognosis - usually in kids t(9;22) -- poor prognosis- usually in adults (Ph+ ALL) |
|
|
T-ALL
|
Lymphoblasts express markers CD2 thru CD8
Do not express CD10 Presents as a mediastinal thymic mass in a teen Acute lymphoblastic lymphoma (malignant cells forming a mass) |
|
|
AML
|
Neoplastic accumulation of myeloblasts
Stain for MPO (can be seen as Auer rods) Usually in older adults (50-60 y/o) Subclassification: - cytogenic abn - lineage of myeloblasts - surface markers |
|
|
Acute Promyelocytic Leukemia |
t(15;17) RAR (retinoic acid receptor) disrupted; promyelocytes accumulate Promyelocytes --> Auer rods --> DIC Treatment: ATRA (all-trans retinoic acid) causes blasts to mature |
|
|
Acute Monocytic Leukemia
|
Proliferation of monoblasts; Lack MPO
Blasts characteristic infiltrate gums |
|
|
Acute Megakaryoblastic Leukemia
|
Proliferation of Megakaryoblasts
Lack MPO Associated with Down Syndroms (before age 5) |
|
|
Down Syndrome and Leukemia
|
Increased risk
Before 5: Acute Megakaryoblastic Leukemia After 5 : ALL |
|
|
AML can also arise from?
|
Pre-existing dysplasia
- Prior exposure to alkylating agents or radiotherapy |
|
|
Myelodysplastic Syndromes
|
Cytopenias w/ hypercellular bm
Abn maturation w/ increase blast Most pt die from infection or bleeding May progress to acute leukemia (> 20 % blasts) |
|
|
Chronic Leukemia
|
Neoplastic proliferation of mature circulating lymphocytes
High WBC Usually insidious in onset and seen in older adults |
|
|
CLL
|
Neoplastic proliferation of naive B cells
Cells coexpress CD5 and CD20 Increased lymphocytes and smudge cells on blood smear Involvement of lymph nodes Generalized lymphadenopathy (LAD) cause small lymphocytic lymphoma |
|
|
Complications of CLL
|
Hypogammaglobulinemia (don't produce Ig) --> most common cause of death in these pt is infection
Autoimmune hemolytic anemia Transformation to diffuse large B cell lymphoma (pt w/ enlarging lymph node or enlarging spleen) |
|
|
Hairy Cell Leukemia
|
Neoplastic proliferation of mature B cells
Hairy cytoplasmic processes Positive for TRAP |
|
|
Clinical features of Hairy Cell Leukemia
|
Splenomegaly (red pulp)
Dry tap with bone marrow aspiration Lymphadenopathy is usually absent |
|
|
How do you treat Hairy Cell Leukemia
|
Excellent response to 2-CDA
Adenosine deaminase inhibitor (part of the purine degradation pathway) Adenosine accumulates in toxic levels in neoplastic B cells |
|
|
ATLL
|
Neoplastic proliferation of mature CD4+ T cells
Associated with HTLV-1 (Japan and Caribbean) |
|
|
Classical Features of ATLL
|
Rash
Generalized LAD w/ HSM (hepatosplenomegaly) Lytic bone lesions with hypercalcemia |
|
|
Mycosis Fungoides
|
Neoplastic proliferation of mature CD4+ T cells
Cells infiltrate skin producing a rash, plaques, or nodules Aggregates of neoplastic T cells in epidermis = Pautrier microabscesses |
|
|
When mycosis fungoides cell spread into blood
|
Known as Sezary Syndrome.
Characteristic lymphocytes with cerebriform nuclei as seen on blood smear. |
|
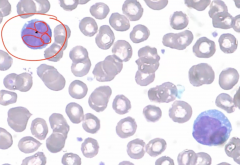
Cerebriform nuclei
|
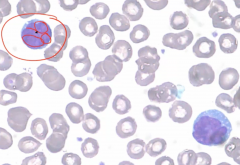
|
|
|
Myeloproliferative Disorder
|
Neoplastic accumulation of mature myeloid cells --> myeloproliferative disorder.
Disease of late adulthood Results in high WBC w/ hypercellular BM Cells of all myeloid lineages are increased Classified based upon dominant myeloid cell |
|
|
Complications of Myeloproliferative Disorders
|
Increased risk for hyperuricemia and gout (RBCs lose their nucleus and it is degraded via the purine degradation pathway--> increase in uric acid--> gout)
Progression to marrow fibrosis Transformation to acute leukemia |
|
|
Chronic Myeloid Leukemia
|
Neoplastic proliferation of mature myeloid cells, especially granulocytes.
Basophils are characterisiticaly increased t(9;22) bcr-abl with increased tyrosine kinase activity |
|
|
First Line of Treatment for Chronic Myeloid Leukemia
|
Imantinib
Blocks tyrosine kinase activity |
|
|
Characteristics of CML
|
Splenomegaly common
Enlarging spleen suggests accelerated phase of disease Transformation to acute leukemia usually follows shortly thereafter Transformation into acute leukemia --> AML (2/3) ALL(1/3) Mutation is in a pluripotent stem cell |
|
|
CML must be distinguished from
|
Leukemoid Reaction
CML granules are LAP negative (leukocyte alkaline phosphatase which is associated with inflammation) CML has increased basophils CML granulocytes exhibit t(9;22) |
|
|
Polycythemia Vera
|
Neoplastic proliferation of mature myeloid cells, especially RBCs.
Granulocytes and platelets are increased Associated with JAK2 kinase mutation |
|
|
Clinical Symptoms of Polycythemia Vera
|
Blurry vision and headache
Increased risk of venous thrombosis (high risk for Bud-Chiari) Flushed face due to congestion Itching after bathing (due to increased mast cells. Bathing leads to mast cells releasing histamine resulting in itchiness) |
|
|
Treatment of Polycythemia Vera
|
Phlebotomy
Second line of treatment is hydroxyurea w/o treatment, death usually occurs w/i 1 year |
|
|
Polycythemia vera must be distinguished from?
|
Reactive polycythemia
In PV, SaO2 is normal and EPO is increased In reactive polycythemia due to lung disease, SaO2 is low and EPO is increased In reactive polycythemia due to ectopic EPO, EPO is high and SaO2 is normal |
|
|
Essential Thrombocythemia
|
Neoplastic proliferation of mature myeloid cells, especially platelets. RBCs and granulocytes are also increased.
Associated with JAK2 kinase mutation |
|
|
Symptoms of Essential Thrombocythemia
|
Increased risk of bleeding and/or thrombosis
Rarely progress to marrow fibrosis or acute leukemia No significant risk for hyperuricemia or gout |
|
|
Myelofibrosis
|
Neoplastic proliferation of mature myeloid cells especially megakaryocytes
Associated with JAK2 kinase mutation Megakaryocytes produce excess PDGF --> results in marrow fibrosis |
|
|
Clinical Features of Myelofibrosis
|
Splenomegaly due to extramedullary hematopoiesis
Leukoerythoblastic smear (in bone marrow there are reticulin gates that prevent precursors from entering the blood. In spleen, reticulin gates don't exist --> leukoerythroblastic smear --> results in tear drop cells --> squeezed though gates/fibrosis) - Increased risk of infection, thrombosis, bleeding |
|
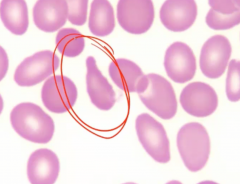
|
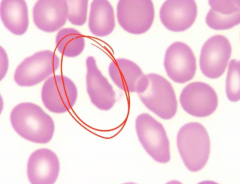
Teardrop cell due to myelofibrosis
|
|
|
Lymphadenopathy
|
Enlarged lymph nodes
|
|
|
Painful LAD
|
Associated with acute infection
|
|
|
Painless LAD
|
Chronic Inflammation, metastatic carcinoma, or lymphoma
|
|
|
Enlargement of follicles
|
Due to RA, AIDS
|
|
|
Enlargement of Paracortex
|
Due to viral infection (e.x: infectious mononucleosis)
|
|
|
Enlargement of sinus histiocytes
|
LN draining tissue with cancer
|
|
|
Lymphoma
|
Neoplastic proliferation of lymphoid cells resulting in a mass
Can are is LN or extranodal tissue |
|
|
Follicular Lymphoma
|
t(14;18)
Neoplastic small B cells (CD20+) that make follicle-like nodules Clinically presents in late adulthood with painless LAD bcl2 on chromosome 18 (bcl2 stabilizes mitochondrial membrane; prevents cytochrome C from inducing apoptosis) --> don't want this to happen in follicle --> cells can't die IgH on chromosome 14 Pushes bcl2 into IgH position --> highly active gene and bcl2 is overexpressed |
|
|
Treatment of follicular lymphoma
|
Asymptomatic usually
Symptomatic treatment with low-dose CTX or rituximab |
|
|
Complications associated with follicular lymphoma
|
Can progress to diffuse large B cell lymphoma
Presents as an enlarging lymph node |
|
|
How do you distinguish follicular lymphoma from follicular hyperplasia?
|
Disruption of normal LN architecture
Lack of tingible body macrophages in germinal center (macrophages eating debris of apoptotic cells) Expression of bcl2 in follicles Monoclonality |
|
|
Mantle Cell Lymphoma
|
t(11;14)
Neoplastic small B cells (CD20+) that expand mantle zone Clinically presents in late adulthood with painless LAD Cyclin D1 on chromosome 11 Overexpression of cyclin D1 --> promotes G1/S transition into cell cycle |
|
|
Marginal Zone Lymphome
|
Neoplastic small B cells (CD20+) that expand into marginal zone.
(in center is follicle, then mantle, then marginal zone) |
|
|
What is Marginal Zone Lymphoma Associated with?
|
Hashimoto's Thyroiditis, Sjogren Syndrome, H. pylori
Marginal zone is formed by post germinal center B cells |
|
|
MALToma
|
Marginal zone lymphoma in mucosal sites (e.g stomach)
Gastric MALToma may regress w/ treatment of H. pylori |
|
|
Burkitt Lymphoma
|
t(8;14)
Neoplastic intermediate sized B cells CD20+ EBV Extranodal mass on child on YA African form- mass on jaw Sporadic form - mass on abdomen c-myc on chromosome 8. cmyc promotes cell growth; high mitotic rate and starry skin appearance |
|
|
Diffuse B Cell Lymphoma
|
Neoplastic large B cells (CD20+) that grow diffusely in sheets.
Most common form of NHL Clinically aggressive Arises sporadically or from transformation from follicular lymphoma Presents in late adult hood as an enlarging LN or extranodal mass |
|
|
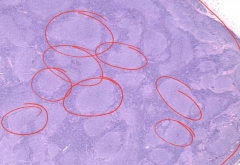
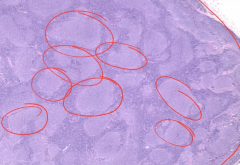
Follicular Lymphoma
|
|
|
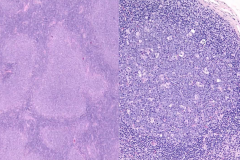
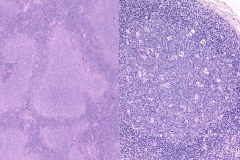
(L) Follicular Lymphoma
(R) Follicular Hyperplasia |
|
|
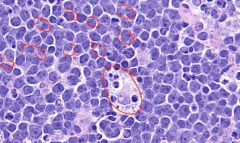
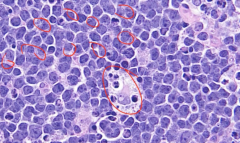
Starry Sky of Burkitt's Lymphoma
|
|
|
Hodgkins Lymphoma
|
Rare neoplastic cells - Reed Sternberg cells (CD15, CD30) --> secrete cytokines and draws in reactive cells --> mass
Occasionally results in 'B' symptoms (fever, chills, and night sweats) Attracts lymphocytes, plasma cells, macrophages, and eosinophils May lead to fibrosis Reactive inflammatory cells are the bulk of tumor and basis for classification |
|
|
Subtypes of Hodgkins Lymphoma
|
Nodular Sclerosis (70% of cases)
Lymphocyte rich Mixed Cellularity Lymphocyte depleted |
|
|
Nodular Sclerosis
|
Most common
Classical presentation: enlarging LN or mediastinal LN in a YA usually female |
|
|
Biopsy of Nodular Sclerosis
|
LN divided by large bands of fibrosis
Reed-Sternberg cells are present in lake-like spaces (lacunar cells) |
|

|
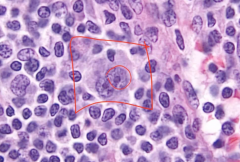
Reed Sternberg Cell
|
|
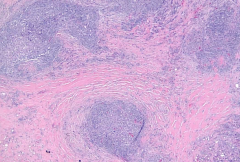
|
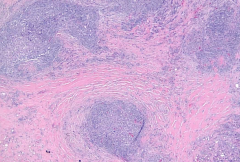
Bands of fibrosis associated with Hodgkin's Lymphoma
|
|
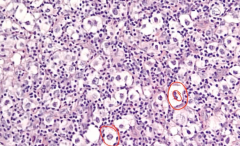
|
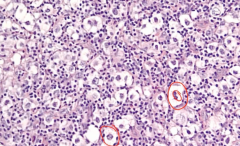
Lacunar Cells
|
|
|
Lymphocyte rich Hodgkin's Lymphoma
|
Best Prognosis
|
|
|
Mixed Cellularity Hodgkin's Lymphoma
|
Associated with abundant eosinophils (IL-5)
|
|
|
Lymphocyte depleted Hodgkin's Lymphoma
|
Worse prognosis - seen in elderly and HIV patients
|
|
|
Multiple Myeloma
|
Malignant Proliferation of plasma cells in bone marrow
Most common primary malignancy of bone High serum IL-6 sometimes present |
|
|
Characteristic of Multiple Myeloma
|
Bone pain with hypercalcemia
Neoplastic plasma activate RANK receptor on osteoclasts (plasma cells produce osteoclast activating factor) Lytic punched out lesions seen on x-ray, especially in vertebrae and skull Increases risk of fracture Elevated serum protein - neoplastic plasma cell produce Ig - M spike present on SPEP, most commonly due to IgG or IgA (indicates monoclonal Ig) Increased risk for infection |
|
|
Why is there an increased risk for infection with multiple myeloma
|
Monoclonal Ab lacks Ag diversity
Infection most common cause of death |
|
|
Blood smear with Multiple Myeloma
|
Rouleaux formation of blood
Increase in serum proteins decreases charge between RBCs so they stack like poker chips |
|
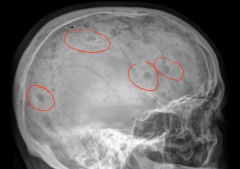
|
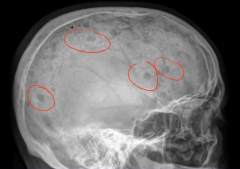
Multiple Myeloma
|
|

|
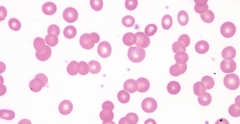
Rouleaux Blood Formation
|
|
|
Primary AL Amyloidosis
|
Caused by Multiple Myeloma
Free light chain circulates in serum and deposits in tissue |
|
|
Proteinuria
|
Associated with Multiple Myeloma
Free light chain is excreted in urine as Bence-Jones proteins Deposition in kidney tubules leads to risk for renal failure (myeloma kidney) |
|
|
MGUS (Monoclonal Gammopathy of Underdetermined Significance)
|
Increased serum protein with M spike on SPEP
Other features of multiple myeloma are absent (no lytic lesions, hypercalcemia, AL amyloid, or Bence Jones proteinuria) Common in elderly (seen in 5% of 70 y.os) 1% develop multiple myeloma |
|
|
Waldenstrom Macroglobinemia
|
B cell lymphoma w/ monoclonal IgM production
|
|
|
Clinical Features of Waldenstrom Macroglobinemia
|
- Generalized LAD; lytic bone lesions absent
- Increased serum protein with M-spike (comprised of IgM) --> increases viscosity of blood - Visual and neurological deficits (retinal hemorrhage or stroke) - Bleeding (due to hyperviscosity --> prevents platelet aggregation) |
|
|
Treatment for acute complications of Waldenstrom Macroglobinemia
|
Plasmapheresis - which removes IgM from serum
|
|
|
Langerhan Cells
|
Specialized dendritic cells found predominantly in skin
Derived from bone marrow monocytes Present antigen to naive T cells |
|
|
Langerhan Cell Histiocytosis
|
Neoplastic proliferation of Langerhan Cells
Characteristic Birbeck (tennis racket) granules seen on EM Cells are CD1A+ and S100+ by immunhistochemistry |
|
|
Letterer-Siwe Disease
|
Malignant proliferation of Langerhans cells
Classic presentation is skin rash and cystic skeletal defects in an infant <2 Multiple organs involved Rapidly fatal |
|
|
Eosinophilic Granuloma
|
Benign Proliferation of Langerhan cells in bone
Classic presentation is pathologic fracture in adolescent; skin is not involved. Biopsy shows Langerhan cells with mixed inflammatory cells including eosinophils |
|
|
Hand-Schuller-Christian Disease
|
Malignant proliferation of Langerhan cells
Classic presentation = scalp rash, lytic skull defects, diabetes insipidus, and exopthalmos in a child |

