![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
66 Cards in this Set
- Front
- Back
|
What gonadotropins act at the ovary?
|
FSH/LH
|
|
|
What is the second messenger through which the gonadotropins act at the ovary?
|
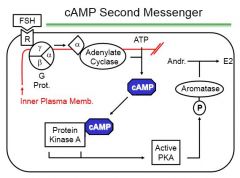
cAMP
|
|
|
What modification do the gonadotropins cause in cells at the ovary?
|
Phosphorylation of enzymes that regulate gonad cell function
|
|
|
What are the actions of the gonadobtropins at the gonads?
|
Gametogenesis
Steroidogenesis |
|
|
What is the source of the precursors for steroidogenesis at the gonads?
|
Cholesterol via LDLs from the bloodstream
|
|
|
What's the mechanism of steroid action?
|
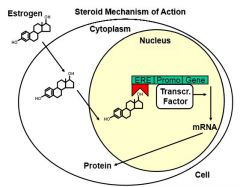
Lipid soluble; go through the nuclear and plasma membranes
Bind to receptors in nucleus Promote gene transcription |
|
|
What are some of the steroid-receptors found within the nucleus?
|
Estrogen response elements
Progesterone response elements Androgen response elements |
|
|
What are the feedback actions of estrogen in the body?
|
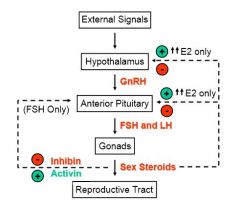
Negative feedback on:
Hypothalamus GnRH release Pituitary LH release At HIGH levels estrogen can have a positive feedback loop on: GnRH LH |
|
|
What are the activities of inhibin and activin? What do they act on?
|
Inhibit and stimulate FSH secretion, from the pituitary, respectively.
|
|
|
What is the 2 cell/2 gonadotropin theory?
|
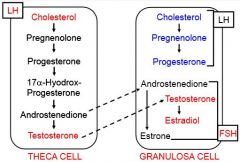
You have theca cells and granulosa cells:
LH acts at theca cells LH (during cycling only) and FSH act at granulosa cells |
|
|
What cells does LH act on?
|
Theca cells
|
|
|
What cells does FSH act on?
|
Granulosa cells
|
|
|
What is the effect of LH action at theca cells?
|
Androgen production
|
|
|
What is the effect of FSH at granulosa cells?
|
Estrogen production
|
|
|
What are the functions of the ovary?
|
Oogenesis
Folliculogenesis Corpeus luteum formation |
|
|
What are the components of folliculogenesis?
|
Support of oogenesis
Support of steroidogenesis |
|
|
What's the main hormone produced by the corpus leutum? What is the function/
|
Progesterone
Maintain pregnancy/support luteal phase of the cycle |
|
|
What is the pathway of migration of eggs in the fetus?
|
1. Yolk sac ectderm
2. Gonadal ridge 3. Formation of fetal ovary |
|
|
When does oocyte mitosis stop in humans?
|
20 weeks!
|
|
|
What stage of meiosis do oocytes areest at? What are they called?
|
Prophase 1
Primary oocytes |
|
|
When are oocytes recruited to complete meiosis?
|
Puberty
|
|
|
What is the definition of an oogonia?
|
Human germ cell that:
-Undergoes mitotic divisions -exists during first 3 months of fetal development -stops mitosis and startws meiosis |
|
|
What is the definition of a primary oocyte?
|
Oocyte that has started meiosis and arrests in prophase of meiosis 1
|
|
|
How many primary oocytes do humans have?
|
2-4 million
|
|
|
What is the definition of a secondary oocyte/
|
Adault oocyte
Just prior to ovulation; finished with meiosis 1 |
|
|
What is the definition of an ovum?
|
Ovulated oocyte that has been penetrated by a sperm and finished meiosis 2
Haploid before it joins with sperm. |
|
|
What happens in the process of oogenesis?
|
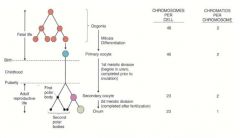
|
|
|
How many follicles grow during each wave of folliculogenesis?
|
10-25!
Not all of them grow, t hough. |
|
|
What happens if conditions are correct during folliculogenesis? Not correct?
|
Correct: ONE follicle becomes dominant
Incorrect: all of them die. The one "chosen" follicle then ovulates. |
|
|
What is the definition of a primordial follicle?
|
Single layer of squamous granulosa cells
Oocyte non-growing |
|
|
What is the definition of a primary follicle?
|
Single cuboidal layer of granulosa cells
-Primary oocyte grows (transcription) -Zona pellucida forms |
|
|
What marks the transition of a primordial follicle to a primary follicle?
|
Presence of the zona pellucida
|
|
|
What is the definition of a secondary follicle?
|
Primary oocyte
Granulosa cells Theca cells Preantrum LH/thea/androgens FSH/granulosa/estrogens |
|
|
What is the definition of a a mature follicle?
|
Contains an antrum
Produces lots o estrogen Increases in size (antrum growth) Oocyte stops growing |
|
|
What is another name for a mature follicle?
|
Graafian follicle
|
|
|
What is an antrum of a follicle?
|
Fluid-filled space
|
|
|
What is the effect of estrogen from a mature follicle?
|
Induces LH receptors in granulosa cells
Mucus secretion from the cervix endometrium growth Increases cilica movement in the oviduct At HIGH levels, positive feecback on LH-->surge-->ovulation |
|
|
What are the stages of follicle development?
|
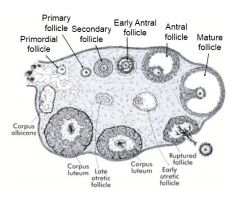
|
|
|
During what phase of meiosis is an oocyte released?
|
Metaphase II
|
|
|
What are the oocytes that are able to resume meiosis?
|
Only the oocytes within the preantral follicle
|
|
|
What's the stimulus for the preantral follicle to resume meiosis?
|
LH surge
|
|
|
What's the mechanism by which an oocyte stays in meiotic arrest?
|
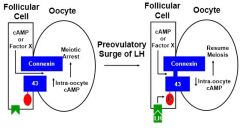
Normally, oocytes have gap junctions to granulosa cells.
Messages (cAMP) pass between the follicular cell and the oocyte, keeping the oocyte in arrest When LH binds to the granulosa cells, you have phosphorylation of connexin 43, which stops the transport of cAMP As a result, the oocyte is able to undergo meiosis |
|
|
What are the mechanisms underlying ovulation?
|
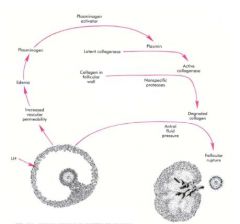
1. Enzymatic activity: LH activates cascade, causing increased activity that breaks down the follicle wall
2. Hydrostatic forces: fluid within the antrum builds up pressure |
|
|
After ovulation, what do the granulosa cells become?
|
Luteal cells
|
|
|
What do luteal cells produce?
|
Progesterone (primary)
Estrogen (bits) |
|
|
How long does the corpus luteum last?
|
10 days
|
|
|
Broadly, what are the two phases of the menstrual cycle?
|
1-14: follicular phase
15-28; luteal phase |
|
|
How much time passes between dominant follicle selection and ovulation?
|
1 week
|
|
|
What is stimulus for the retention of the corpus luteum?
|
Beta HCG
|
|
|
What is the effect of high progesterone (on the presence of estrogen) on LH and FSH?
|
Decreases in plasma levels
|
|
|
What are the steps that take place in the menstrual cycle?
|
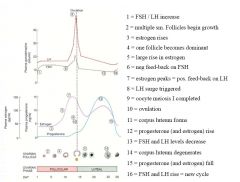
|
|
|
What's on the outside of the ovulated oocyte? What's the effect of this?
|
Cumulus cells
They're sticky, which allow the fimbriae to "grab" the oocyte and bring it down the fallopian tube |
|
|
What is the impact of cervical mucus on sperm transit?
|
Make s it easier
|
|
|
What is the site of fertilization?
|
Oviduct
|
|
|
What's the mechanism of the sperm/zona pellucida interaction?
|
1. Binds to ZP3
2. Acrosome reaction 3. Binds to ZP2 4. Penetrates the egg 5. Binds to the oolemma: ZP3-->ZP3f; hardening 6. Block to polyspermy |
|
|
What is the cell that actually implants in the uterine wall?
|
Blastocyst
|
|
|
What are the properties of a blastomere?
|
Totipotent: each can form an embryo/fetus
|
|
|
When does embryonic genomic control start?
|
Morula
You start to have polarity of the embryo. |
|
|
How many cells are in the morula?
|
16 cells.
|
|
|
What does a morula give rise to? What happens at this stage?
|
Blastocyst
You have water being pumped into the blastocoele |
|
|
What are the two cell populations within the blastocyst?
|
Inner cell mass
Cells on outside --> trophectoderm |
|
|
What is the stage at which the embryo implants?
|
Blastocyst stage
|
|
|
What does the blastocyst secrete?
|
human chorionic gonadotropin
Acts like LH; keeps the progesterone going. |
|
|
What's the action o fhuman chorionic gonadotropin on the body?
|
Keeps progesterone secretion going
|
|
|
When is HCG detectable in the urine?
|
One month after the last perioe, or about 14 days after fertilization
|
|
|
What are the components of the placenta?
|
Chorion
Amnion |

