![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
16 Cards in this Set
- Front
- Back
|
Define COPD
*** primary cause? |
preventable and treatable disease state characterized by air-flow limitation that is not fully reversible.
The air-flow limitation is usually progressive and is associated with an abnormal inflammatory response of the lungs to noxious particles or gases, primarily caused by cigarette smoking. |
|
|
what is the difference of emphysema vs chronic bronchitis?
|
emphysema: condition of the lung characterized by abnormal permanent enlargement of the air spaces distal to the terminal bronchioles accompanied by destruction of their walls and without obvious fibrosis. COLLAPSED BRONCHIOLE
bronchitis: the presence of chronic productive cough for three months in each of two successive years in a patient in whom other causes of chronic cough have been excluded. Caused by excess mucus |
|
|
please describe the mechanism of COPD
|
Tissue destruction with loss of elastic recoil (in alveoli), destruction of terminal bronchioles and associated blood supply with resultant gas exchange abnormalities
ciliary dysfunction with poor clearance of secretions occurs due to Mucous gland hypertrophy/Goblet cell hyperplasia |
|
|
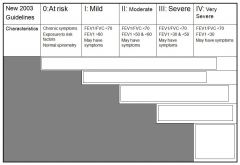
what does the diagnosis of COPD require?
*** |
spirometry
forced expiratory volume in one second (FEV1)/forced vital capacity (FVC) less than 70% confirms the presence of air-flow limitation that is not fully reversible. |
|
|
FEV1/FVC ratio of what constitutes COPD?
* |
less than 70%
confirms the presence of air-flow limitation that is not fully reversible. |
|
|
why are bullae bad in COPD?
|
they can be a collection site for infection
and they press down on good lung areas |
|
|
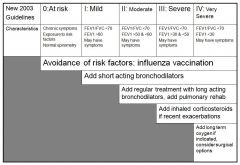
what is the major treatment of COPD?
|
get them off tobacco!!
|
|
|
|
|
|
what is LVRS
|
lung volume reduction surgery
treatment of COPD |
|
|
what criteria must you meet to be eligible for a lung transplant
|
Not smoking for greater than 6 months
|
|
|
what is the appropriate treatment for exacerbation of COPD
|
Steroids (or Nebulizers)
|
|
|
for a standard pt, what is required to qualify for O2? (2)
|
Oxygen saturation of 88% or less
PaO2 of 55 mm Hg or less |
|
|
severe deficiency of ____ poses a strong risk factor for early-onset emphysema
|
Alpha 1 Antitrypsin
|
|
|
people with normal levels of Alpha 1 Antitrypsin have what phenotype?
|
MM
|
|
|
Young patient, no history of smoking, BASILAR PREDOMINATE EMPHYSEMA
this is a classic case of... |
Alpha 1 antitrypsin deficiency
|
|
|
Orange team > ?
|
PURPLE TEAM
|

