![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
57 Cards in this Set
- Front
- Back
|
'reduced oxygen carrying capacity of blood' -
|
anemia
|
|
|
What is the average Hb (hemoglobin) and HCT (Hematocrit) of Males?
|
Hb: 13.6-17.2 gm/dL
HCT: 39-49 |
|
|
What is the average Hb (hemoglobin) and HCT (Hematocrit) of Females
|
Hb: 12-15 gm/dL
HCT: 33-43 |
|
|
What is the MCV (Mean Cell Volume)?
|
82-96 = average volume of RBC
|
|
|
Mean cell hemoglobin (MCH):
|
average content of Hb per RBC
|
|
|
Mean cell hemoglobin conc. (MCHC)
|
average conc. of Hb in a volume of RBC
|
|
|
RBC Distribution Width (RDW)
|
the coefficient of variation of red blood cell volume
|
|
|
Which of the following are symptoms of Anemia?
mucous membranes weakness Pale skin malaise easy fatiguability dyspnea |
weakness
malaise easy fatiguability dyspnea |
|
|
iron deficiency
thalassemia lead poisoning are all associated with ? |
microcytic RBC morphology
(<80 MCV) |
|
|
What are the 3 main mechanism of anemia?
|
Blood loss
Increased destruction (hemolytic) Impaired production |
|
|
Chronic Blood loss anemia occurs when:
|
blood loss exceeds that of iron reserves
|
|
|
Disruption of intracellular membranes, enzymes or the presence of hemoglobin disorders within the cell are examples of?
|
Intrinsic Hemolytic Anemia
|
|
|
*Shorted RBC life span
*Increased erythropoiesis *increased products pf RBC destruction are results of ? |
Hemolytic Anemia
|
|
|
Where do most Hemolytic anemias occur?
|
Spleen
|
|
|
Hemolytic anemias RARELY occur ________ but will may be due to the following?
mechanical injury toxins infection complement fixation |
intravascular
|
|
|
Which type of Hemolytic anemia has:
-NO hemoglobinemia -NO hemoglobinuria |
extrinsic hemolytic anema
|
|
|
When do the following occur?
increased erythroid precursors in marrow Reticulocytosis in peripheral blood Inceased bilirubin: pigment gallstones Chronic: hemosiderosis |
BOTH extrinsic/intrinsic hemolytic anemias
|
|
|
An intrinsic hemolytic anemia associated with a mutation in
ankyrin |
Hereditary Spherocytosis
|
|
|
Due to inflexible RBC, Spherocytosis shortens the lifespan of RBCs from ____ to _______
|
120 days ---> 10-20 days
|
|
|
What intrinsic enzyme disorder protects against Malaria (plasmodium falciparum)?
|
G6PD deficiency
Glucose-6-Phosphate |
|
|
What is the tx for (HS) Hereditary Spherocytosis?
|
Splenectomy
|
|
|
What is an intermittent hemolytic anemia that clinically presents as
-hemolysis after oxidative stress -Neonatal jaundice -chronic low grade hemolytic anemia |
G6PD Deficiency
|
|
|
In what conditions might Heinz bodies and 'bite' cells within a blood smear
|
G6PD Deficiency
|
|
|
A point gene mutation involving the substitution of Valine with Glutamate results in ______ and abnormal hemoglobin in the disease called _________?
|
HbS
Sickle Cell Anemia |
|
|
What are the main differences in Hb composition between adults and children?
|
Difference in HbF/HbA concentration:
Adult: -HbA = 96% -HbA(2) = 3 % -HbF = 1% Children -HbF = 75% |
|
|
At what age do children adapt an adult levels of HbA in the blood?
|
6 months
|
|
|
HbS molecules aggregate upon deoxygenation resulting eventually in irreversible cell damage:
|
Sickle Cell Anemia
|
|
|
exhibits sequestration in areas (bone marrow / spleen) where blood flow is sluggish.
|
Sickle Cell Disease
|
|
|
Chronic anemia may lead to _________ and _________?
|
Bone marrow expansion
Hyperplasia |
|
|
Which disease can develop aplastic crisis by B19 virus?
|
Sickle Cell Disease
|
|
|
What are 2 treatments in Sickle Cell Disease?
|
1) Hyroxurea: increase of HbF combats HbS
2) Exchange transfusion (crisis) |
|
|
decreased synthesis of normal alpha or beta hemoglobin chain
|
Thalassemias
|
|
|
What condition exhibits an excess of alpha globin chains?
|
Beta Thalassemia
|
|
|
Microcytic anemia
affects Mediterraneans HbF > HbA |
Beta Thalassemia
|
|
|
Which form of Thalassemia is most severe and why?
|
Beta Thalassemia b/c of the excess of free alpha globin chains which are most toxic
|
|
|
-Rare
-Homozygotic -severe, life-threatening, (childhood death, retardation) transfusion-dependent |
beta Thal Major
|
|
|
-resistance to malaria
-mild anemia -Asymptomatic |
beta Thal Minor
|
|
|
Why are α chains more toxic to RBC?
|
Under-hemoglobinized RBCs
-poor oxygen carrying of Hb Decreased survival: -insoluble inclusion --> membrane damage -early apoptosis |
|
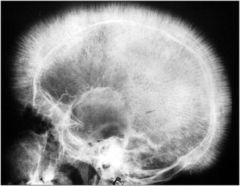
What is associated with 'crew cut' appearance on radiograph?
|
Beta Thalassemia
|
|
|
Defined as a MCV greater than 100 fL
|
Megaloblastic Anemia
|
|
|
Serum findings of:
Low iron Low TIBC Decreased transferrin saturation High ferritin |
Anemia of Chronic Disease:
impaired Iron utilization due to secondary disease (RA, infection) |
|
|
Serum findings of:
Low ferritin Decreased saturation of transferrin Increased TIBC |
Iron Deficiency Anemia
|
|
|
Hypochromic Microcytic Anemia
|
Iron Deficiency Anemia
|
|
|
What assists iron absorption in GI tract?
|
Transferrin
|
|
|
What is Hb converted to before being excreted with bilirubin in bile?
|
Biliverdin
|
|
|
Iron deficiency
Anemia of chronic disease Megaloblastic anemia are examples of? |
Hyperproliferative Anemias
|
|
|
- RBCs susceptible to lysis by complement
- decrease in all GPI linked proteins *CD55, 59 |
PNH (Paroxysmal Nocturnal Hemoglobinuria)
|
|
|
_____ and ______ have high affinity for oxygen which means poor transporters of oxygen to tissues due to inability to release oxygen
|
HbH
Hb Bart |
|
|
Sign of anemia (fatigability, dyspnea etc)
Microcytic hypochromic anemia High oxygen affinity Oxidative damage leads to splenic sequestration |
HbH Disease
|
|
|
Fetal distress
δ-globin tetramers Extremely high oxygen affinity Fetal demise |
Hemoglobin Barts Disease
|
|
|
Deficiency of B12 and Folic Acid result in
|
Megaloblastic Anemia
|
|
|
What disease may come about from malabsorption of B12 vitamin?
|
Crohn's disease
|
|
|
What disease may come about from malabsorption of Folic Acid?
|
Celiac's Disease (Sprue)
|
|
|
-Moderate to severe anemia
-Thrombocytopenia -Leukopenia with hypersegmented neutrophils -Neurological changes secondary to dorsal column demyelination are all associated with ? |
B12 Megaloblastic anemia
|
|
|
-Moderate to severe anemia
-Thrombocytopenia -Leukopenia with hypersegmented neutrophils |
Folic Acid Deficiency (sans neurological problems)
|
|
|
Non-clonal increase in the concentration of red blood cells unlike myeloproliferative disorders
|
Polycythemia
|
|
|
Caused by:
Increased erythropoietin (tumor or hypoxemia) Dehydration Treat by: phlebotomy or hydration |
Polycythemia
|

