![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
591 Cards in this Set
- Front
- Back
|
بسم الله |
الرحمن الرحيم |
|
|
ربي اشرح لي صدري |
و يسر لي أمري |
|
|
و احلل عقدة من لساني |
يفقهوا قولي |
|
|
8, low grade fever with persistent cough, subcutaneous emphysema, next ? |
Chest X-ray |
|
|
8, low grade fever with persistent cough, subcutaneous emphysema, next ? |
Chest X-ray |
|
|
Pulmonary auscultation page 7 |
7 |
|
|
Pleural effusion auscultation? |
Decreased ( breath sound and tactile fremitus ) , Dullness |
|
|
Child, cystic fibrosis, recurrent severe pulmonary symptoms , given cefepime and oseltamivir , which empiric antibiotic ??? |
IV vancomycin ( staph infection ) |
|
|
52, wakes repeatedly at night with choking sensation, fall asleep when reading or watching tv, BMI 34, hypertension ??? |
Obstructive sleep apnea ( transient obstruction due to laxity of pharyngeal tissue) |
|
|
FEV1/FVC ratio ? FEV1 normal? |
75% FEV1= 80-120% |
|
|
60, SOB, mucoid cough for 5 months, oxygen saturation 92%, FEV1= 75%, FEV1/FVC< 70% , which measure decrease mortality in this patient? |
Smoking cessation ( not oxygen because the saturation is normal to mild ) |
|
|
60, severe SOB, severe weight loss, X-ray: pleural effusion, next ? |
Thoracentesis except patients with clear CHF symptoms those the first step is diuretics |
|
|
28, bronchial asthma, the episodes on average twice a week, he takes albuterol inhaler which doing well, next? |
Continue current regimen |
|
|
Pleural effusion auscultation? |
Decreased ( breath sound and tactile fremitus ) , Dullness |
|
|
Postoperative, mild hypoxemia ( 90%), decreased breath sounds at bases, pO2 is decreased and pCO2 is decreased?? |
Impaired cough and shallow breathing due to atelectasis Rx: early mobilization, incentive spirometry.... Ps: pO2 and pCO2 refer to gas on the arterial side. |
|
|
7, difficulty in breathing, asthma symptoms ( عرصات عم يخدعوك), hypotension, history of allergy to food, initial treatment?? |
IM epinephrine ( anaphylaxis) |
|
|
Accident, systolic pressure is 60 , pulse 130, after putting on mechanical ventilator he developed cardiac arrest why ? |
Decreased right ventricular preload due to hypovolemic shock and positive pressure made by ventilator |
|
|
Child, cystic fibrosis, recurrent severe pulmonary symptoms , given cefepime and oseltamivir , which empiric antibiotic ??? |
IV vancomycin ( staph infection ) |
|
|
52, wakes repeatedly at night with choking sensation, fall asleep when reading or watching tv, BMI 34, hypertension ??? |
Obstructive sleep apnea ( transient obstruction due to laxity of pharyngeal tissue) |
|
|
FEV1/FVC ratio ? FEV1 normal? |
75% FEV1= 80-120% |
|

Accident, vital signs are normal, mild respiratory distress, bruises on anterior chest and abdomen, breath sounds decreased at left lung base ?? |
Diaphragm injury |
|
|
60, severe SOB, severe weight loss, X-ray: pleural effusion, next ? |
Thoracentesis except patients with clear CHF symptoms those the first step is diuretics |
|
|
28, bronchial asthma, the episodes on average twice a week, he takes albuterol inhaler which doing well, next? |
Continue current regimen |
|
|
Accident, vital signs are normal, mild respiratory distress, bruises on anterior chest and abdomen, breath sounds decreased at left lung base ?? |
Diaphragm injury |
|
|
65, COPD exacerbation, central venous catheter in right subclavian vein and placed on mechanical ventilation, even all treatment the pulse oximetry is 83%, BP 80/50, tracheal deviated to left, breath sound is absent on right, next ????? |
Needle thoracostomy (at the second intercostal space in the midclavicular line ) followed by emergent tube thoracostomy This patient has tension pneumothorax |
|
|
Place of needle thoracostomy?? |
2nd intercostal space in midclaviclular line , if failed use fifth intercostal space in midaxillary line |
|
|
Pleural effusion auscultation? |
Decreased ( breath sound and tactile fremitus ) , Dullness |
|
|
Postoperative, mild hypoxemia ( 90%), decreased breath sounds at bases, pO2 is decreased and pCO2 is decreased?? |
Impaired cough and shallow breathing due to atelectasis Rx: early mobilization, incentive spirometry.... Ps: pO2 and pCO2 refer to gas on the arterial side. |
|
|
7, difficulty in breathing, asthma symptoms ( عرصات عم يخدعوك), hypotension, history of allergy to food, initial treatment?? |
IM epinephrine ( anaphylaxis) |
|
|
Accident, systolic pressure is 60 , pulse 130, after putting on mechanical ventilator he developed cardiac arrest why ? |
Decreased right ventricular preload due to hypovolemic shock and positive pressure made by ventilator |
|
|
اللهم فهمني و علمني |
و ارزقني تذكر المعلومات و الاجابة الصحيحة في الامتحان يا رحيم يا الله |
|
|
Child, cystic fibrosis, recurrent severe pulmonary symptoms , given cefepime and oseltamivir , which empiric antibiotic ??? |
IV vancomycin ( staph infection ) |
|
|
52, wakes repeatedly at night with choking sensation, fall asleep when reading or watching tv, BMI 34, hypertension ??? |
Obstructive sleep apnea ( transient obstruction due to laxity of pharyngeal tissue) |
|
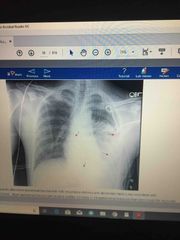
Accident, vital signs are normal, mild respiratory distress, bruises on anterior chest and abdomen, breath sounds decreased at left lung base ?? |
Diaphragm injury |
|
|
60, SOB, mucoid cough for 5 months, oxygen saturation 92%, FEV1= 75%, FEV1/FVC< 70% , which measure decrease mortality in this patient? |
Smoking cessation ( not oxygen because the saturation is normal to mild ) |
|
|
60, severe SOB, severe weight loss, X-ray: pleural effusion, next ? |
Thoracentesis except patients with clear CHF symptoms those the first step is diuretics |
|
|
28, bronchial asthma, the episodes on average twice a week, he takes albuterol inhaler which doing well, next? |
Continue current regimen |
|
|
Accident, vital signs are normal, mild respiratory distress, bruises on anterior chest and abdomen, breath sounds decreased at left lung base ?? |
Diaphragm injury |
|
|
65, COPD exacerbation, central venous catheter in right subclavian vein and placed on mechanical ventilation, even all treatment the pulse oximetry is 83%, BP 80/50, tracheal deviated to left, breath sound is absent on right, next ????? |
Needle thoracostomy (at the second intercostal space in the midclavicular line ) followed by emergent tube thoracostomy This patient has tension pneumothorax |
|
|
Place of needle thoracostomy?? |
2nd intercostal space in midclaviclular line , if failed use fifth intercostal space in midaxillary line |
|
|
Pleural effusion auscultation? |
Decreased ( breath sound and tactile fremitus ) , Dullness |
|
|
Postoperative, mild hypoxemia ( 90%), decreased breath sounds at bases, pO2 is decreased and pCO2 is decreased?? |
Impaired cough and shallow breathing due to atelectasis Rx: early mobilization, incentive spirometry.... Ps: pO2 and pCO2 refer to gas on the arterial side. |
|
|
7, difficulty in breathing, asthma symptoms ( عرصات عم يخدعوك), hypotension, history of allergy to food, initial treatment?? |
IM epinephrine ( anaphylaxis) |
|
|
Accident, systolic pressure is 60 , pulse 130, after putting on mechanical ventilator he developed cardiac arrest why ? |
Decreased right ventricular preload due to hypovolemic shock and positive pressure made by ventilator |
|
|
اللهم فهمني و علمني |
و ارزقني تذكر المعلومات و الاجابة الصحيحة في الامتحان يا رحيم يا الله |
|
|
Child, cystic fibrosis, recurrent severe pulmonary symptoms , given cefepime and oseltamivir , which empiric antibiotic ??? |
IV vancomycin ( staph infection ) |
|
|
52, wakes repeatedly at night with choking sensation, fall asleep when reading or watching tv, BMI 34, hypertension ??? |
Obstructive sleep apnea ( transient obstruction due to laxity of pharyngeal tissue) |
|
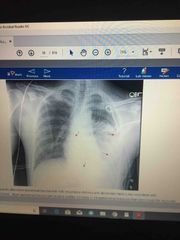
Accident, vital signs are normal, mild respiratory distress, bruises on anterior chest and abdomen, breath sounds decreased at left lung base ?? |
Diaphragm injury |
|
|
60, SOB, mucoid cough for 5 months, oxygen saturation 92%, FEV1= 75%, FEV1/FVC< 70% , which measure decrease mortality in this patient? |
Smoking cessation ( not oxygen because the saturation is normal to mild ) |
|
|
60, severe SOB, severe weight loss, X-ray: pleural effusion, next ? |
Thoracentesis except patients with clear CHF symptoms those the first step is diuretics |
|
|
28, bronchial asthma, the episodes on average twice a week, he takes albuterol inhaler which doing well, next? |
Continue current regimen |
|
|
Accident, vital signs are normal, mild respiratory distress, bruises on anterior chest and abdomen, breath sounds decreased at left lung base ?? |
Diaphragm injury |
|
|
65, COPD exacerbation, central venous catheter in right subclavian vein and placed on mechanical ventilation, even all treatment the pulse oximetry is 83%, BP 80/50, tracheal deviated to left, breath sound is absent on right, next ????? |
Needle thoracostomy (at the second intercostal space in the midclavicular line ) followed by emergent tube thoracostomy This patient has tension pneumothorax |
|
|
Place of needle thoracostomy?? |
2nd intercostal space in midclaviclular line , if failed use fifth intercostal space in midaxillary line |
|
|
56, sudden SOB, left sided pain worsen with cough, DM, hypertension, smoking, fever, leukocytosis, hypoxemia, ECG ( irregular PR intervals, no P wave , narrow QRS ) ??? |
Pulmonary embolism caused by atrial fibrillation |
|
|
Dyspnea on exertion, choking at night , BMI 48 , which additional findings related to electrolytes?? |
Obstructive sleep apnea with obesity hypoventilation syndrome . Decreased chloride due to Bicarbonate retention ( compensatory kidney for the respiratory acidosis) |
|
|
Adult, SOB with cough and blood in sputum, no weight loss or fever, bilateral rales, creatine 2.6, dysmorphic red cells in urinalysis ?? |
Goodpasture’s diseases Dx: renal biopsy : basement membrane IgG antibodies |
|
|
56, sudden SOB, left sided pain worsen with cough, DM, hypertension, smoking, fever, leukocytosis, hypoxemia, ECG ( irregular PR intervals, no P wave , narrow QRS ) ??? |
Pulmonary embolism caused by atrial fibrillation |
|
|
Dyspnea on exertion, choking at night , BMI 48 , which additional findings related to electrolytes?? |
Obstructive sleep apnea with obesity hypoventilation syndrome . Decreased chloride due to Bicarbonate retention ( compensatory kidney for the respiratory acidosis) |
|
|
Adult, SOB with cough and blood in sputum, no weight loss or fever, bilateral rales, creatine 2.6, dysmorphic red cells in urinalysis ?? |
Goodpasture’s diseases Dx: renal biopsy : basement membrane IgG antibodies |
|
|
رب اشرح لي صدري |
و يسر لي أمري |
|
|
Nonproductive cough, night sweats, weight loss, right upper lobe cavity with infiltrate , what is the epidemiology? |
Emigration from endemic area because it’s a TB |
|

Left sided Pulmonary symptoms without night sweet or fever or weight loss, history of Hodgkin lymphoma treated with chemo and radiation??? |
Secondary malignancy |
|
|
45 with HIV, SOB, left sided chest pain with green phlegm, fever, the pain is worse with deep inspiration??? |
Empyema |
|
|
Pleural effusion features from CHF ?? |
Transudative effusion, the pH of it is 7.4-7.55 Ps: normal pH of pleura is 7.60 |
|
|
Elderly( 68) , confusion, high fever, productive cough, leukocytosis, right lower lobe infiltrate, BUN 24 ?? |
Community acquired pneumonia Rx: hospitalization ( inpatient due to high CURB-65 criteria), administration of abx( fluoroquinolone: moxifoxacin, or ceftriaxone plus azithromycin) |
|
|
58, smoking history, persistent cough for 3 months, weight loss, hemoptysis, no night sweat or fever, the mucus membranes are moist, no edema, hyponatremia, Rx? |
Fluid restriction because the hyponatremia is due to SIADH ( the membranes are moist) Mostly the patient has small cell lung cancer Ps: didn’t give hypertonic saline because the symptoms aren’t severe. |
|
|
Small cell lung cancer complication related to fluids ?? |
Hyponatremia due to SIADH Rx: fluids restriction |
|
|
Front (Term) |
Pulmonary compliance |
|
|
Patient with asthma exacerbation, oximetry 84%, given albuterol, ipratropium, methylprednisolone, after one hour the lab results ( pH: 7.32, PaCO2: 50, PaO2: 65), next ? |
Endotracheal intubation ( elevated PaCO2 or even normal) |
|
|
34, dyspnea, severe left chest pain increases with inspiration, hemoptysis, using OCP ?? |
Pulmonary embolism due pulmonary infarction |
|
|
Exudative is defined by one of Light criteria |
Fluid patient Protein / serum > 0.5 Fluid LDH/ serum > 0.6 Fluid LDH > 2/3 of the upper limit for LDH of serum |
|

45 with HIV, SOB, left sided chest pain with green phlegm, fever, the pain is worse with deep inspiration??? |
Empyema |
|
|
Low glucose levels in exudate due to ?? |
High Metabolic activity of leukocytes and bacteria in pleural fluid |
|
|
Nasal breathing, stuffy nose, occasional dry cough for a year , no allergies, not relieved by loratadine , boggy erythematous nasal mucosa?? |
Nonallergic rhinitis (vasomotor) Rx: intranasal corticosteroids , intranasal antihistamines |
|
|
Burning building, 15% Burn, oropharynx erythema, carboxyhemoglobin is 20%, best management? |
Endotracheal intubation to prevent upper airway obstruction by edema |
|
|
Dry cough for 8 weeks, history of chronic rhinorrhea , skin rash, improved after chlorpheniramine , why ?? |
Decreased nasal secretions because this patient has upper airway cough syndrome ( postnasal drip) Rx: H1 histamine antagonist |
|
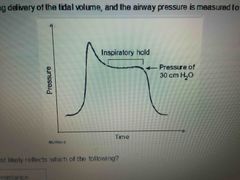
Front (Term) |
Pulmonary compliance |
|
|
Hemoptysis, cough, weight loss, X-ray: irregular nodule in the peripheral right upper field, no lymph node enlargement??? |
Adenocarcinoma of the lung Associated with clubbing, hypertrophic osteoarthropathy |
|
|
Palpitations, headache, vomiting, had COPD treated with theophylline..etc, a week ago treated for a wound with ciprofloxacin, ECG shows atrial tachycardia, next ??? |
Serum theophylline levels ( toxicity caused by inhibition of cytochrome oxidase by cipro) |
|
|
70, fever and cough, fever, leukocytosis, no cervical lymphadenopathy, X-ray: right lower lobe infiltration ??? |
Community acquired pneumonia caused by strep pneumoniae |
|
|
On ventilator, respiratory rate 18, tidal volume 450, FiO2 40%, PEEP 5 cm H2O, his pH : 7.51, PCo2: 22, best next ? |
Decrease respiratory rate ( to reduce the respiratory alkalosis) |
|
|
9, difficulty breathing from nose for 6 months, recurrent sinus infection and pneumonias, vit D deficiency, nasal polyps, digital clubbing, thin girl ???? |
Cystic fibrosis Ps: primary ciliary dyskinesia is similar to CF in respiratory symptoms but it has reversed visceral organs , normal growth. |
|
|
Bacterial pneumonia causing pleural effusion (parapneumonic empyema ) characterized by ? |
Exudate { Low glucose ( <60), low pH( <7.2), high protein }. Rx: drainage ( chest tube), abx |
|
|
Clubbing and sudden onset of joint arthropathy in chronic smoker suggest ?? |
Hypertrophic osteoarthropathy Do chest X-ray to role out malignancy |
|
|
Chest pain and progressive dyspnea, after intubation at the site the breath sounds on the left are decreased,why ? |
Because the endotracheal tube is placed into the right main bronchus Rx: reposition of the tube |
|
|
Asthma exacerbation treated with the medications, positive airway pressure is started in the second day, after 2 hours the patient becomes agitated, respiratory acidosis, next ? |
Endotracheal intubation |
|
|
Collision, no distress, developed tachypnea, tachycardia after 2 hours, hypoxemia, right patchy irregular alveolar infiltrate on X-ray??? |
Pulmonary contusion |
|
|
55, pulmonary symptoms, FEV1= 67%, FEV1/FVC=65%, after bronchodilator the FEV1= 82% ??? |
Asthma ( because the patient is improved) Not COPD: because the patient doesn’t improve after bronchodilator in COPD. |
|
|
The indicator of asthma in PFTs is |
FEV1 |
|
|
Child, High fever, noisy breathing, stridor, drooling, had runny nose, oximetry 86% ??? |
Epiglottis ( H influenza type b ) Dx: lateral neck X-ray ( thumbprint sign) Rx: endotracheal intubation, abx |
|
|
ARDS features |
Hypoxemia, bilateral alveolar infiltrate leading to impaired gas exchange, decreased lung compliance and pulmonary hypertension |
|
|
Postoperative, syncope, decreased lung sounds, hypotension, right bundle branch block, he died why ?? |
Massive pulmonary thromboembolism Dx:CT pulmonary angiography |
|
|
CREST syndrome |
Calcinosis cutis, Raynaud phenomenon, esophageal dysmotility with reflux, sclerodactyly , telangiectasia |
|
|
Exertional SOB, lightheaded, no pulmonary symptoms, had Raynaud phenomenon, heartburn, which other fundings ??? |
CREST syndrome associated with limited cutaneous systemic sclerosis ( right ventricular enlargement, right sided heart failure) |
|
|
Nonproductive cough, night sweats, weight loss, right upper lobe cavity with infiltrate , what is the epidemiology? |
Emigration from endemic area because it’s a TB |
|

Left sided Pulmonary symptoms without night sweet or fever or weight loss, history of Hodgkin lymphoma treated with chemo and radiation??? |
Secondary malignancy |
|
|
45 with HIV, SOB, left sided chest pain with green phlegm, fever, the pain is worse with deep inspiration??? |
Empyema |
|
|
Pleural effusion features from CHF ?? |
Transudative effusion, the pH of it is 7.4-7.55 Ps: normal pH of pleura is 7.60 |
|
|
Elderly( 68) , confundion, high fever, productive cough, leukocytosis, right lower lobe infiltrate, BUN 24 ?? |
Community acquired pneumonia Rx: hospitalization ( inpatient due to high CURB-65 criteria), administration of abx( fluoroquinolone: moxifoxacin, or ceftriaxone plus azithromycin) |
|
|
58, smoking history, persistent cough for 3 months, weight loss, hemoptysis, no night sweat or fever, the mucus membranes are moist, no edema, hyponatremia, Rx? |
Fluid restriction because the hyponatremia is due to SIADH ( the membranes are moist) Mostly the patient has small cell lung cancer Ps: didn’t give hypertonic saline because the symptoms aren’t severe. |
|
|
Small cell lung cancer complication related to fluids ?? |
Hyponatremia due to SIADH Rx: fluids restriction |
|
|
Front (Term) |
Pulmonary compliance |
|
|
Patient with asthma exacerbation, oximetry 84%, given albuterol, ipratropium, methylprednisolone, after one hour the lab results ( pH: 7.32, PaCO2: 50, PaO2: 65), next ? |
Endotracheal intubation ( elevated PaCO2 or even normal) |
|
|
34, dyspnea, severe left chest pain increases with inspiration, hemoptysis, using OCP ?? |
Pulmonary embolism due pulmonary infarction |
|
|
Exudative is defined by one of Light criteria |
Fluid patient/ serum > 0.5 Fluid LDH/ serum > 0.6 Fluid LDH > 2/3 of the upper limit for LDH of serum |
|

45 with HIV, SOB, left sided chest pain with green phlegm, fever, the pain is worse with deep inspiration??? |
Empyema |
|
|
Low glucose levels in exudate due to ?? |
High Metabolic activity of leukocytes and bacteria in pleural fluid |
|
|
Nasal breathing, stuffy nose, occasional dry cough for a year , no allergies, not relieved by loratadine , boggy erythematous nasal mucosa?? |
Nonallergic rhinitis (vasomotor) Rx: intranasal corticosteroids , intranasal antihistamines |
|
|
Burning building, 15% Burn, oropharynx erythema, carboxyhemoglobin is 20%, best management? |
Endotracheal intubation to prevent upper airway obstruction by edema |
|
|
Dry cough for 8 weeks, history of chronic rhinorrhea , skin rash, improved after chlorpheniramine , why ?? |
Decreased nasal secretions because this patient has upper airway cough syndrome ( postnasal drip) Rx: H1 histamine antagonist |
|
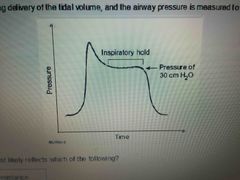
Front (Term) |
Pulmonary compliance |
|
|
Hemoptysis, cough, weight loss, X-ray: irregular nodule in the peripheral right upper field, no lymph node enlargement??? |
Adenocarcinoma of the lung Associated with clubbing, hypertrophic osteoarthropathy |
|
|
Palpitations, headache, vomiting, had COPD treated with theophylline..etc, a week ago treated for a wound with ciprofloxacin, ECG shows atrial tachycardia, next ??? |
Serum theophylline levels ( toxicity caused by inhibition of cytochrome oxidase by cipro) |
|
|
70, fever and cough, fever, leukocytosis, no cervical lymphadenopathy, X-ray: right lower lobe infiltration ??? |
Community acquired pneumonia caused by strep pneumoniae |
|
|
On ventilator, respiratory rate 18, tidal volume 450, FiO2 40%, PEEP 5 cm H2O, his pH : 7.51, PCo2: 22, best next ? |
Decrease respiratory rate ( to reduce the respiratory alkalosis) |
|
|
9, difficulty breathing from nose for 6 months, recurrent sinus infection and pneumonias, vit D deficiency, nasal polyps, digital clubbing, thin girl ???? |
Cystic fibrosis Ps: primary ciliary dyskinesia is similar to CF in respiratory symptoms but it has reversed visceral organs , normal growth. |
|
|
Bacterial pneumonia causing pleural effusion (parapneumonic empyema ) characterized by ? |
Exudate { Low glucose ( <60), low pH( <7.2), high protein }. Rx: drainage ( chest tube), abx |
|
|
Clubbing and sudden onset of joint arthropathy in chronic smoker suggest ?? |
Hypertrophic osteoarthropathy Do chest X-ray to role out malignancy |
|
|
Chest pain and progressive dyspnea, after intubation at the site the breath sounds on the left are decreased,why ? |
Because the endotracheal tube is placed into the right main bronchus Rx: reposition of the tube |
|
|
Asthma exacerbation treated with the medications, positive airway pressure is started in the second day, after 2 hours the patient becomes agitated, respiratory acidosis, next ? |
Endotracheal intubation |
|
|
Collision, no distress, developed tachypnea, tachycardia after 2 hours, hypoxemia, right patchy irregular alveolar infiltrate on X-ray??? |
Pulmonary contusion |
|
|
أستغفر الله و أتوب إليه |
ربي اغفر لي يا غفور |
|
|
55, pulmonary symptoms, FEV1= 67%, FEV1/FVC=65%, after bronchodilator the FEV1= 82% ??? |
Asthma ( because the patient is improved) Not COPD: because the patient doesn’t improve after bronchodilator in COPD. |
|
|
The indicator of asthma in PFTs is |
FEV1 |
|
|
Child, High fever, noisy breathing, stridor, drooling, had runny nose, oximetry 86% ??? |
Epiglottis ( H influenza type b ) Dx: lateral neck X-ray ( thumbprint sign) Rx: endotracheal intubation, abx |
|
|
ARDS features |
Hypoxemia, bilateral alveolar infiltrate leading to impaired gas exchange, decreased lung compliance and pulmonary hypertension |
|
|
Postoperative, syncope, decreased lung sounds, hypotension, right bundle branch block, he died why ?? |
Massive pulmonary thromboembolism Dx:CT pulmonary angiography |
|
|
CREST syndrome |
Calcinosis cutis, Raynaud phenomenon, esophageal dysmotility with reflux, sclerodactyly , telangiectasia |
|
|
Exertional SOB, lightheaded, no pulmonary symptoms, had Raynaud phenomenon, heartburn, which other fundings ??? |
CREST syndrome associated with limited cutaneous systemic sclerosis ( right ventricular enlargement, right sided heart failure) |
|
|
Nonproductive cough, night sweats, weight loss, right upper lobe cavity with infiltrate , what is the epidemiology? |
Emigration from endemic area because it’s a TB |
|
|
In systemic sclerosis the mechanism of pulmonary arterial hypertension is ??? |
Hyperplasia of the intimal smooth muscle layer The FEV1/FVC is normal |
|
|
45 with HIV, SOB, left sided chest pain with green phlegm, fever, the pain is worse with deep inspiration??? |
Empyema |
|
|
Pleural effusion features from CHF ?? |
Transudative effusion, the pH of it is 7.4-7.55 Ps: normal pH of pleura is 7.60 |
|
|
Elderly( 68) , confundion, high fever, productive cough, leukocytosis, right lower lobe infiltrate, BUN 24 ?? |
Community acquired pneumonia Rx: hospitalization ( inpatient due to high CURB-65 criteria), administration of abx( fluoroquinolone: moxifoxacin, or ceftriaxone plus azithromycin) |
|
|
58, smoking history, persistent cough for 3 months, weight loss, hemoptysis, no night sweat or fever, the mucus membranes are moist, no edema, hyponatremia, Rx? |
Fluid restriction because the hyponatremia is due to SIADH ( the membranes are moist) Mostly the patient has small cell lung cancer Ps: didn’t give hypertonic saline because the symptoms aren’t severe. |
|
|
Small cell lung cancer complication related to fluids ?? |
Hyponatremia due to SIADH Rx: fluids restriction |
|
|
Front (Term) |
Pulmonary compliance |
|
|
Patient with asthma exacerbation, oximetry 84%, given albuterol, ipratropium, methylprednisolone, after one hour the lab results ( pH: 7.32, PaCO2: 50, PaO2: 65), next ? |
Endotracheal intubation ( elevated PaCO2 or even normal) |
|
|
34, dyspnea, severe left chest pain increases with inspiration, hemoptysis, using OCP ?? |
Pulmonary embolism due pulmonary infarction |
|
|
Exudative is defined by one of Light criteria |
Fluid patient/ serum > 0.5 Fluid LDH/ serum > 0.6 Fluid LDH > 2/3 of the upper limit for LDH of serum |
|
|
Left sided Pulmonary symptoms without night sweet or fever or weight loss, history of Hodgkin lymphoma treated with chemo and radiation??? |
Secondary malignancy |
|
|
Low glucose levels in exudate due to ?? |
High Metabolic activity of leukocytes and bacteria in pleural fluid |
|
|
Nasal breathing, stuffy nose, occasional dry cough for a year , no allergies, not relieved by loratadine , boggy erythematous nasal mucosa?? |
Nonallergic rhinitis (vasomotor) Rx: intranasal corticosteroids , intranasal antihistamines |
|
|
Burning building, 15% Burn, oropharynx erythema, carboxyhemoglobin is 20%, best management? |
Endotracheal intubation to prevent upper airway obstruction by edema |
|
|
Dry cough for 8 weeks, history of chronic rhinorrhea , skin rash, improved after chlorpheniramine , why ?? |
Decreased nasal secretions because this patient has upper airway cough syndrome ( postnasal drip) Rx: H1 histamine antagonist |
|
|
The 3 common causes of chronic cough > 8 weeks??? |
Upper airway cough syndrome Asthma GERD |
|
|
Hemoptysis, cough, weight loss, X-ray: irregular nodule in the peripheral right upper field, no lymph node enlargement??? |
Adenocarcinoma of the lung Associated with clubbing, hypertrophic osteoarthropathy |
|
|
Palpitations, headache, vomiting, had COPD treated with theophylline..etc, a week ago treated for a wound with ciprofloxacin, ECG shows atrial tachycardia, next ??? |
Serum theophylline levels ( toxicity caused by inhibition of cytochrome oxidase by cipro) |
|
|
70, fever and cough, fever, leukocytosis, no cervical lymphadenopathy, X-ray: right lower lobe infiltration ??? |
Community acquired pneumonia caused by strep pneumoniae |
|
|
On ventilator, respiratory rate 18, tidal volume 450, FiO2 40%, PEEP 5 cm H2O, his pH : 7.51, PCo2: 22, best next ? |
Decrease respiratory rate ( to reduce the respiratory alkalosis) |
|
|
9, difficulty breathing from nose for 6 months, recurrent sinus infection and pneumonias, vit D deficiency, nasal polyps, digital clubbing, thin girl ???? |
Cystic fibrosis Ps: primary ciliary dyskinesia is similar to CF in respiratory symptoms but it has reversed visceral organs , normal growth. |
|
|
Bacterial pneumonia causing pleural effusion (parapneumonic empyema ) characterized by ? |
Exudate { Low glucose ( <60), low pH( <7.2), high protein }. Rx: drainage ( chest tube), abx |
|
|
Clubbing and sudden onset of joint arthropathy in chronic smoker suggest ?? |
Hypertrophic osteoarthropathy Do chest X-ray to role out malignancy |
|
|
Chest pain and progressive dyspnea, after intubation at the site the breath sounds on the left are decreased,why ? |
Because the endotracheal tube is placed into the right main bronchus Rx: reposition of the tube |
|
|
Asthma exacerbation treated with the medications, positive airway pressure is started in the second day, after 2 hours the patient becomes agitated, respiratory acidosis, next ? |
Endotracheal intubation |
|
|
Collision, no distress, developed tachypnea, tachycardia after 2 hours, hypoxemia, right patchy irregular alveolar infiltrate on X-ray??? |
Pulmonary contusion |
|
|
أستغفر الله و أتوب إليه |
ربي اغفر لي يا غفور |
|
|
55, pulmonary symptoms, FEV1= 67%, FEV1/FVC=65%, after bronchodilator the FEV1= 82% ??? |
Asthma ( because the patient is improved) Not COPD: because the patient doesn’t improve after bronchodilator in COPD. |
|
|
The indicator of asthma in PFTs is |
FEV1 |
|
|
Child, High fever, noisy breathing, stridor, drooling, had runny nose, oximetry 86% ??? |
Epiglottis ( H influenza type b ) Dx: lateral neck X-ray ( thumbprint sign) Rx: endotracheal intubation, abx |
|
|
ARDS features |
Hypoxemia, bilateral alveolar infiltrate leading to impaired gas exchange, decreased lung compliance and pulmonary hypertension |
|
|
Postoperative, syncope, decreased lung sounds, hypotension, right bundle branch block, he died why ?? |
Massive pulmonary thromboembolism Dx:CT pulmonary angiography |
|
|
CREST syndrome |
Calcinosis cutis, Raynaud phenomenon, esophageal dysmotility with reflux, sclerodactyly , telangiectasia |
|
|
Exertional SOB, lightheaded, no pulmonary symptoms, had Raynaud phenomenon, heartburn, which other fundings ??? |
CREST syndrome associated with limited cutaneous systemic sclerosis ( right ventricular enlargement, right sided heart failure) |
|
|
62, exertional dyspnea and dry cough for year, carpenter for navy ships, FEV1 decreased, FEV1/FVC normal, diffusion capacity lung for carbon monoxide is decreased??? |
Interstitial lung disease caused by occupational exposure pulmonary fibrosis ( asbestos) |
|
|
Beclomethasone inhaler complication in asthma patient |
Thrush ( oral candidiasis) |
|
|
Using ACEi , after a week has cough, next step ? |
Discontinue ACEi |
|

ARDS management |
Mechanical ventilation ( low tidal volume, high PEEP, high FiO2) |
|
|
Bronchiectasis( bronchial wall thickened and bronchial dilation) pathophysiology ? |
Prolonged Infectious insult with impaired clearance |
|
|
Patient with bronchiectasis should be evaluated for ? |
Immunity and CF |
|
|
Symptoms of CAP, next ? |
Chest X-ray , if confirmed give empiric abx |
|
|
62, history of surgery 2 weeks ago, now: suddenly dyspnea, no productive cough, tachycardia, mild hypoxia, low grade fever, next ?? |
CT angiogram of the chest ( PE) |
|
|
Diseases classified according FEV1/FVC and diffusion capacity of lung for carbon monoxide ( DLCO) ?? |
Low FEV1/FVC(obstructive lung disease) , if decreased DLCO >> COPD , if DLCO doesn’t decrease >>asthma. Normal FEV1/FVC (restrictive disease), if DLCO decreased >> interstitial lung disease, if DLCO doesn’t decrease>> chest wall weakness. |
|
|
Postoperative pneumonia prevention by ?? |
Incentive spirometry |
|
|
ARDS management |
Mechanical ventilation ( low tidal volume, high PEEP, high FiO2) |
|
|
87, fever, foul smelling, productive cough, history of recurrent pneumonia, dementia symptoms, decreased breath sounds in right upper lobe ??? |
Aspiration pneumonia due to impaired swallowing and cough reflex in advanced dementia patients. |
|

2 years of episodic cough productive yellow sputum, her condition improves with abx but she continues to have persistent cough, coarse crackles bilaterally, diffuse rhonchi , X-ray reveals atelectasis , confirmation??? |
High resolution CT scan ( bronchiectasis ) |
|
|
MS, sudden SOB with left sided chest pain worsen in 2 days, no fever, reduced breath sounds and dullness at left base lung ?? |
Pulmonary embolism |
|
|
71, seizures tonic clonic, his Blood gases demonstrate Respiratory acidosis, why ? |
Hypoventilation |
|
|
Dullness to percussion , increased breath sounds especially during expiration, increased tactile fremitus ??? |
Consolidation of the lung ( lobar pneumonia) |
|
|
Male, Pulmonary symptoms, weight loss, large anterior mediastinal mass, elevated B-hCG, a- fetoprotein ?? |
Nonseminomatous germ cell tumors Ps: AFP elevation distinguished between this tumor and seminoma (only rise B-hCG ) |
|
|
62, exertional dyspnea and dry cough for year, carpenter for navy ships, FEV1 decreased, FEV1/FVC normal, diffusion capacity lung for carbon monoxide is decreased??? |
Interstitial lung disease caused by occupational exposure pulmonary fibrosis ( asbestos) |
|
|
Beclomethasone inhaler complication in asthma patient |
Thrush ( oral candidiasis) |
|
|
Using ACEi , after a week has cough, next step ? |
Discontinue ACEi |
|

ARDS management |
Mechanical ventilation ( low tidal volume, high PEEP, high FiO2) |
|
|
Bronchiectasis( bronchial wall thickened and bronchial dilation) pathophysiology ? |
Prolonged Infectious insult with impaired clearance |
|
|
Patient with bronchiectasis should be evaluated for ? |
Immunity and CF |
|
|
Symptoms of CAP, next ? |
Chest X-ray , if confirmed give empiric abx |
|
|
62, history of surgery 2 weeks ago, now: suddenly dyspnea, no productive cough, tachycardia, mild hypoxia, low grade fever, next ?? |
CT angiogram of the chest ( PE) |
|
|
اللهم ذكرني ما أقرأ |
و دلني على الاجابة الصحية في الامتحان يا مقتدر |
|
|
Diseases classified according FEV1/FVC and diffusion capacity of lung for carbon monoxide ( DLCO) ?? |
Low FEV1/FVC(obstructive lung disease) , if decreased DLCO >> COPD , if DLCO doesn’t decrease >>asthma. Normal FEV1/FVC (restrictive disease), if DLCO decreased >> interstitial lung disease, if DLCO doesn’t decrease>> chest wall weakness. |
|
|
Postoperative pneumonia prevention by ?? |
Incentive spirometry |
|
|
ARDS management |
Mechanical ventilation ( low tidal volume, high PEEP, high FiO2) |
|
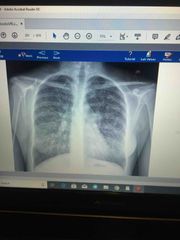
2 years of episodic cough productive yellow sputum, her condition improves with abx but she continues to have persistent cough, coarse crackles bilaterally, diffuse rhonchi , X-ray reveals atelectasis , confirmation??? |
High resolution CT scan ( bronchiectasis ) |
|
|
Child, pneumonia symptoms with minimal fluid on lateral decubitus film , next ? |
Abx because it’s pneumonia with parapneumonic pleural effusion Ps: large effusion require drain |
|
|
MS, sudden SOB with left sided chest pain worsen in 2 days, no fever, reduced breath sounds and dullness at left base lung ?? |
Pulmonary embolism |
|
|
71, seizures tonic clonic, his Blood gases demonstrate Respiratory acidosis, why ? |
Hypoventilation |
|
|
Dullness to percussion , increased breath sounds especially during expiration, increased tactile fremitus ??? |
Consolidation of the lung ( lobar pneumonia) |
|
|
Male, Pulmonary symptoms, weight loss, large anterior mediastinal mass, elevated B-hCG, a- fetoprotein ?? |
Nonseminomatous germ cell tumors Ps: AFP elevation distinguished between this tumor and seminoma (only rise B-hCG ) |
|
|
62, exertional dyspnea and dry cough for year, carpenter for navy ships, FEV1 decreased, FEV1/FVC normal, diffusion capacity lung for carbon monoxide is decreased??? |
Interstitial lung disease caused by occupational exposure pulmonary fibrosis ( asbestos) |
|
|
Beclomethasone inhaler complication in asthma patient |
Thrush ( oral candidiasis) |
|
|
Using ACEi , after a week has cough, next step ? |
Discontinue ACEi |
|
|
2 years of episodic cough productive yellow sputum, her condition improves with abx but she continues to have persistent cough, coarse crackles bilaterally, diffuse rhonchi , X-ray reveals atelectasis , confirmation??? |
High resolution CT scan ( bronchiectasis ) |
|
|
Bronchiectasis( bronchial wall thickened and bronchial dilation) pathophysiology ? |
Prolonged Infectious insult with impaired clearance |
|
|
Patient with bronchiectasis should be evaluated for ? |
Immunity and CF |
|
|
Symptoms of CAP, next ? |
Chest X-ray , if confirmed give empiric abx |
|
|
62, history of surgery 2 weeks ago, now: suddenly dyspnea, no productive cough, tachycardia, mild hypoxia, low grade fever, next ?? |
CT angiogram of the chest ( PE) |
|
|
اللهم ذكرني ما أقرأ |
و دلني على الاجابة الصحية في الامتحان يا مقتدر |
|
|
Diseases classified according FEV1/FVC and diffusion capacity of lung for carbon monoxide ( DLCO) ?? |
Low FEV1/FVC(obstructive lung disease) , if decreased DLCO >> COPD , if DLCO doesn’t decrease >>asthma. Normal FEV1/FVC (restrictive disease), if DLCO decreased >> interstitial lung disease, if DLCO doesn’t decrease>> chest wall weakness. |
|
|
Postoperative pneumonia prevention by ?? |
Incentive spirometry |
|
|
ARDS management |
Mechanical ventilation ( low tidal volume, high PEEP, high FiO2) |
|
|
87, fever, foul smelling, productive cough, history of recurrent pneumonia, dementia symptoms, decreased breath sounds in right upper lobe ??? |
Aspiration pneumonia due to impaired swallowing and cough reflex in advanced dementia patients. |
|
|
Child, pneumonia symptoms with minimal fluid on lateral decubitus film , next ? |
Abx because it’s pneumonia with parapneumonic pleural effusion Ps: large effusion require drain |
|
|
MS, sudden SOB with left sided chest pain worsen in 2 days, no fever, reduced breath sounds and dullness at left base lung ?? |
Pulmonary embolism |
|
|
71, seizures tonic clonic, his Blood gases demonstrate Respiratory acidosis, why ? |
Hypoventilation |
|
|
Dullness to percussion , increased breath sounds especially during expiration, increased tactile fremitus ??? |
Consolidation of the lung ( lobar pneumonia) |
|
|
Male, Pulmonary symptoms, weight loss, large anterior mediastinal mass, elevated B-hCG, a- fetoprotein ?? |
Nonseminomatous germ cell tumors Ps: AFP elevation distinguished between this tumor and seminoma (only rise B-hCG ) |
|
|
Immigrant, Persistent cough, dyspnea for 3 months, E: crackles, enlarged cardiac silhouette with vascular congestion, left main bronchus is elevated, irregular rhythm on ECG ?? |
Mitral stenosis caused by rheumatic heart disease |
|
|
8, chronic smoker, have progressive SOB and wheezing for 2 days, E: using accessory muscle in breathing, normal vital, auscultation: decreased??? |
Chronic obstructive pulmonary disease exacerbation. |
|
|
Accident, Respiratory distress, bilateral coarse breath sounds, X-ray: multiple ribs fractures ? |
Flail chest |
|
|
Sleep apnea treatment |
Weight reduction, avoid sleep in supine . |
|
|
Recurrent sinusitis and otitis despite antibiotics, joint and back pain, urinary symptoms??? |
Granulomatosis with polyangiitis Dx: ANCA( quantitive serum autoantibodies |
|
|
Compensation of respiratory acidosis ??? |
Renal bicarbonate retention ( metabolic alkalosis) |
|
|
Newborn, preterm, delivered at 28 weeks, has central cyanosis, bilateral breath sounds are diminished , grunting,flaring, retraction, X-ray: diffuse reticular granular opacities bilaterally ?? |
Respiratory distress syndrome Rx: early continuous positive air pressure |
|
|
6 months of dry cough and worsening dyspnea, late expiratory crackles, digital clubbing, no accompanying etiology , what is the abnormality??? |
Increased alveolar-arterial gradient ( interstitial lung disease) due to idiopathic fibrosis |
|
|
Front (Term) |
Laryngeal edema ( fixed upper airway obstruction) due to food allergies Rx: epinephrine, corticosteroids, antihistamines |
|
|
Front (Term) |
Back (Definition) |
|
|
Child, difficulty breathing development, rhinorrhea, congestion dry cough ( barking dog ), stridor at rest, Rx ??? |
Racemic epinephrine ( croup) Ps: if no stridor ( humidified air ) |
|
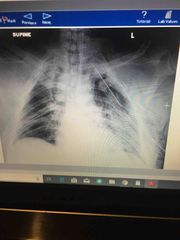
Accident, Respiratory distress, bilateral coarse breath sounds, X-ray: multiple ribs fractures ? |
Flail chest |
|
|
Management of ARDS treated with mechanical ventilation complications |
Low tidal volume ventilation which leads to decreased overdistending alveoli ( improves mortality) |
|
|
63, cough , wheezing, yellow sputum, lost weight, smoking history, prominent fingers clubbing that wasn’t 6 months ago, why the digital clubbing ?? |
Occult malignancy |
|
|
1 hour baby, respiratory distress symptoms, however he has intercostal retraction and clear breath sounds, X-ray: fluid in the interlobar fissures |
Transient tachypnea of newborn ( delayed resorption and clearance of alveolar fluid) Rx: supportive |
|
|
COPD decreased vital capacity cause ? |
Progressive expiratory airflow limitation( air trapping) |
|

6 months of dry cough and worsening dyspnea, late expiratory crackles, digital clubbing, no accompanying etiology , what is the abnormality??? |
Increased alveolar-arterial gradient ( interstitial lung disease) due to idiopathic fibrosis |
|

Front (Term) |
Laryngeal edema ( fixed upper airway obstruction) due to food allergies Rx: epinephrine, corticosteroids, antihistamines |
|
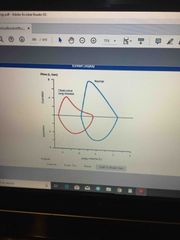
Front (Term) |

Back (Definition) |
|
|
60, pulmonary symptoms, decreased FEV1/FVC, DLCO is normal???? |
COPD ( chronic bronchitis) لا تنخدع بمهنة المريض، خلي تركيزك عالفحص الصدري Ps: if DLCO decreased ( emphysema) |
|
|
Left sided chest discomfort, history of accident 2 months ago , X-ray : mediastinal deviation , next ?? |
CT of chest and abdomen ( to role out diaphragm rupture) |
|
|
38, progressive SOB, cough with mucoid for 6 months, no wheezing, no other symptoms, X-ray: bilateral basilar lucency, next ?? |
Serum alpha-1 antitrypsin deficiency. |
|
|
Silicosis symptoms ( stone worker) with TB symptoms With kidney symptoms, upper airway involved ( trachea) ??? |
Granulomatosis with polyangiitis Dx: ANCA , biopsy Rx: corticosteroids, methotrexate, cyclophosphamide |
|
|
Immigrant, hemoptysis, with cough and foamy sputum, IV fluids and oxygen is portable X-ray: dense opacity in upper right lobe , next ?? |
Respiratory isolation ( TB high suspicion) , if continue bleeding put him on lateral position and do bronchoscopy to Dx and Rx. |
|
|
Fresh frozen plasma indicated if the INR is |
> 1.5 |
|
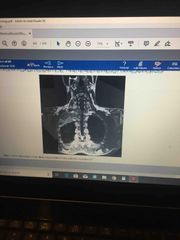
Pulmonary symptoms, with right arm pain |
Superior pulmonary sulcus tumor ( pancoast tumors) |
|
|
Asthma exacerbation treated with albuterol and IV methylprednisolone, the next day she developed high leukocytosis with bands form ?? |
Medication effect ( steroids) |
|
|
Mediastinum tumors according to location |
Anterior: thymoma Posterior: neurogenic tumors, esophageal leiomyoma Middle: bronchogenic cysts, trachea, lymphoma, |
|

Left sided chest discomfort, history of accident 2 months ago , X-ray : mediastinal deviation , next ?? |
CT of chest and abdomen ( to role out diaphragm rupture) |
|
|
HIV, noncompliant with treatment, pulmonary symptoms( PCP), given abx and 5 L normal saline, after 2 days he developed hyponatremia with confusion??? |
SIADH which happens in euvolemia state |
|
|
Pneumonia symptoms on the left side , the oxygen saturation is normal when lying on right side, but it decreased when lying of the left side ( affected side ) , why ?? |
Intrapulmonary shunting ( right to left) of blood due to gravity |
|
|
6th rib fracture, base atelectasis , best essential Rx?? |
Pain control to maintain adequate ventilation |
|
|
Immigrant, Persistent cough, dyspnea for 3 months, E: crackles, enlarged cardiac silhouette with vascular congestion, left main bronchus is elevated, irregular rhythm on ECG ?? |
Mitral stenosis caused by rheumatic heart disease |
|
|
8, chronic smoker, have progressive SOB and wheezing for 2 days, E: using accessory muscle in breathing, normal vital, auscultation: decreased??? |
Chronic obstructive pulmonary disease exacerbation. |
|
|
Accident, Respiratory distress, bilateral coarse breath sounds, X-ray: multiple ribs fractures ? |
Flail chest |
|
|
Sleep apnea treatment |
Weight reduction, avoid sleep in supine . |
|
|
Recurrent sinusitis and otitis despite antibiotics, joint and back pain, urinary symptoms??? |
Granulomatosis with polyangiitis Dx: ANCA( quantitive serum autoantibodies |
|
|
Compensation of respiratory acidosis ??? |
Renal bicarbonate retention ( metabolic alkalosis) |
|
|
Newborn, preterm, delivered at 28 weeks, has central cyanosis, bilateral breath sounds are diminished , grunting,flaring, retraction, X-ray: diffuse reticular granular opacities bilaterally ?? |
Respiratory distress syndrome Rx: early continuous positive air pressure |
|
|
6 months of dry cough and worsening dyspnea, late expiratory crackles, digital clubbing, no accompanying etiology , what is the abnormality??? |
Increased alveolar-arterial gradient ( interstitial lung disease) due to idiopathic fibrosis |
|
|
Front (Term) |
Laryngeal edema ( fixed upper airway obstruction) due to food allergies Rx: epinephrine, corticosteroids, antihistamines |
|
|
Front (Term) |
Back (Definition) |
|
|
Child, difficulty breathing development, rhinorrhea, congestion dry cough ( barking dog ), stridor at rest, Rx ??? |
Racemic epinephrine ( croup) Ps: if no stridor ( humidified air ) |
|

Accident, Respiratory distress, bilateral coarse breath sounds, X-ray: multiple ribs fractures ? |
Flail chest |
|
|
Management of ARDS treated with mechanical ventilation complications |
Low tidal volume ventilation which leads to decreased overdistending alveoli ( improves mortality) |
|
|
63, cough , wheezing, yellow sputum, lost weight, smoking history, prominent fingers clubbing that wasn’t 6 months ago, why the digital clubbing ?? |
Occult malignancy |
|
|
1 hour baby, respiratory distress symptoms, however he has intercostal retraction and clear breath sounds, X-ray: fluid in the interlobar fissures |
Transient tachypnea of newborn ( delayed resorption and clearance of alveolar fluid) Rx: supportive |
|
|
COPD decreased vital capacity cause ? |
Progressive expiratory airflow limitation( air trapping) |
|

6 months of dry cough and worsening dyspnea, late expiratory crackles, digital clubbing, no accompanying etiology , what is the abnormality??? |
Increased alveolar-arterial gradient ( interstitial lung disease) due to idiopathic fibrosis |
|
Front (Term) |
Laryngeal edema ( fixed upper airway obstruction) due to food allergies Rx: epinephrine, corticosteroids, antihistamines |
|
Front (Term) |
Back (Definition) |
|
|
60, pulmonary symptoms, decreased FEV1/FVC, DLCO is normal???? |
COPD ( chronic bronchitis) لا تنخدع بمهنة المريض، خلي تركيزك عالفحص الصدري Ps: if DLCO decreased ( emphysema) |
|
|
Left sided chest discomfort, history of accident 2 months ago , X-ray : mediastinal deviation , next ?? |
CT of chest and abdomen ( to role out diaphragm rupture) |
|
|
38, progressive SOB, cough with mucoid for 6 months, no wheezing, no other symptoms, X-ray: bilateral basilar lucency, next ?? |
Serum alpha-1 antitrypsin deficiency. |
|
|
Silicosis symptoms ( stone worker) with TB symptoms With kidney symptoms, upper airway involved ( trachea) ??? |
Granulomatosis with polyangiitis Dx: ANCA , biopsy Rx: corticosteroids, methotrexate, cyclophosphamide |
|
|
Immigrant, hemoptysis, with cough and foamy sputum, IV fluids and oxygen is portable X-ray: dense opacity in upper right lobe , next ?? |
Respiratory isolation ( TB high suspicion) , if continue bleeding put him on lateral position and do bronchoscopy to Dx and Rx. |
|
|
Fresh frozen plasma indicated if the INR is |
> 1.5 |
|

Pulmonary symptoms, with right arm pain |
Superior pulmonary sulcus tumor ( pancoast tumors) |
|
|
50, fatigue, sleep during day,, doesn’t sleep well at night, morning headache , smoking history, BMI 36 , next?? |
Nocturnal polysomnography ( the gold standard for OSA) |
|
|
Asthma exacerbation treated with albuterol and IV methylprednisolone, the next day she developed high leukocytosis with bands form ?? |
Medication effect ( steroids) |
|
Left sided chest discomfort, history of accident 2 months ago , X-ray : mediastinal deviation , next ?? |
CT of chest and abdomen ( to role out diaphragm rupture) |
|
|
19, has asthma-like symptoms after Twice a week workout sessions??? |
Exercise induced bronchoconstriction Rx: inhaled albuterol 10 minutes before exercise Ps: if she exercise daily then she should use inhaled corticosteroids. |
|
|
HIV, noncompliant with treatment, pulmonary symptoms( PCP), given abx and 5 L normal saline, after 2 days he developed hyponatremia with confusion??? |
SIADH which happens in euvolemia state |
|
|
Pneumonia symptoms on the left side , the oxygen saturation is normal when lying on right side, but it decreased when lying of the left side ( affected side ) , why ?? |
Intrapulmonary shunting ( right to left) of blood due to gravity |
|
|
6th rib fracture, base atelectasis , best essential Rx?? |
Pain control to maintain adequate ventilation |
|
|
Immigrant, Persistent cough, dyspnea for 3 months, E: crackles, enlarged cardiac silhouette with vascular congestion, left main bronchus is elevated, irregular rhythm on ECG ?? |
Mitral stenosis caused by rheumatic heart disease |
|
|
8, chronic smoker, have progressive SOB and wheezing for 2 days, E: using accessory muscle in breathing, normal vital, auscultation: decreased??? |
Chronic obstructive pulmonary disease exacerbation. |
|
|
Accident, Respiratory distress, bilateral coarse breath sounds, X-ray: multiple ribs fractures ? |
Flail chest |
|
|
Sleep apnea treatment |
Weight reduction, avoid sleep in supine . |
|
|
Recurrent sinusitis and otitis despite antibiotics, joint and back pain, urinary symptoms??? |
Granulomatosis with polyangiitis Dx: ANCA( quantitive serum autoantibodies |
|
|
Compensation of respiratory acidosis ??? |
Renal bicarbonate retention ( metabolic alkalosis) |
|
|
Newborn, preterm, delivered at 28 weeks, has central cyanosis, bilateral breath sounds are diminished , grunting,flaring, retraction, X-ray: diffuse reticular granular opacities bilaterally ?? |
Respiratory distress syndrome Rx: early continuous positive air pressure |
|
|
6 months of dry cough and worsening dyspnea, late expiratory crackles, digital clubbing, no accompanying etiology , what is the abnormality??? |
Increased alveolar-arterial gradient ( interstitial lung disease) due to idiopathic fibrosis |
|
|
Front (Term) |
Laryngeal edema ( fixed upper airway obstruction) due to food allergies Rx: epinephrine, corticosteroids, antihistamines |
|
|
Front (Term) |
Back (Definition) |
|
|
Child, difficulty breathing development, rhinorrhea, congestion dry cough ( barking dog ), stridor at rest, Rx ??? |
Racemic epinephrine ( croup) Ps: if no stridor ( humidified air ) |
|
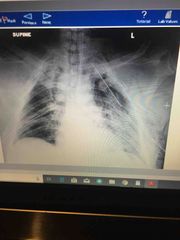
Accident, Respiratory distress, bilateral coarse breath sounds, X-ray: multiple ribs fractures ? |
Flail chest |
|
|
Management of ARDS treated with mechanical ventilation complications |
Low tidal volume ventilation which leads to decreased overdistending alveoli ( improves mortality) |
|
|
63, cough , wheezing, yellow sputum, lost weight, smoking history, prominent fingers clubbing that wasn’t 6 months ago, why the digital clubbing ?? |
Occult malignancy |
|
|
1 hour baby, respiratory distress symptoms, however he has intercostal retraction and clear breath sounds, X-ray: fluid in the interlobar fissures |
Transient tachypnea of newborn ( delayed resorption and clearance of alveolar fluid) Rx: supportive |
|
|
COPD decreased vital capacity cause ? |
Progressive expiratory airflow limitation( air trapping) |
|

6 months of dry cough and worsening dyspnea, late expiratory crackles, digital clubbing, no accompanying etiology , what is the abnormality??? |
Increased alveolar-arterial gradient ( interstitial lung disease) due to idiopathic fibrosis |
|
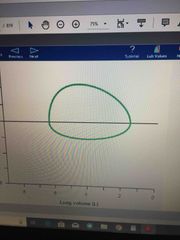
Front (Term) |
Laryngeal edema ( fixed upper airway obstruction) due to food allergies Rx: epinephrine, corticosteroids, antihistamines |
|
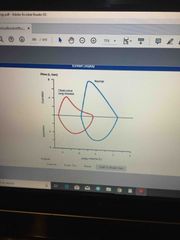
Front (Term) |

Back (Definition) |
|
|
60, pulmonary symptoms, decreased FEV1/FVC, DLCO is normal???? |
COPD ( chronic bronchitis) لا تنخدع بمهنة المريض، خلي تركيزك عالفحص الصدري Ps: if DLCO decreased ( emphysema) |
|
|
Left sided chest discomfort, history of accident 2 months ago , X-ray : mediastinal deviation , next ?? |
CT of chest and abdomen ( to role out diaphragm rupture) |
|
|
38, progressive SOB, cough with mucoid for 6 months, no wheezing, no other symptoms, X-ray: bilateral basilar lucency, next ?? |
Serum alpha-1 antitrypsin deficiency. |
|
|
Silicosis symptoms ( stone worker) with TB symptoms With kidney symptoms, upper airway involved ( trachea) ??? |
Granulomatosis with polyangiitis Dx: ANCA , biopsy Rx: corticosteroids, methotrexate, cyclophosphamide |
|
|
Immigrant, hemoptysis, with cough and foamy sputum, IV fluids and oxygen is portable X-ray: dense opacity in upper right lobe , next ?? |
Respiratory isolation ( TB high suspicion) , if continue bleeding put him on lateral position and do bronchoscopy to Dx and Rx. |
|
|
Fresh frozen plasma indicated if the INR is |
> 1.5 |
|
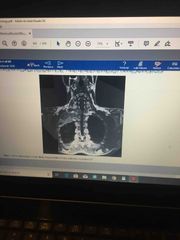
Pulmonary symptoms, with right arm pain |
Superior pulmonary sulcus tumor ( pancoast tumors) |
|
|
50, fatigue, sleep during day,, doesn’t sleep well at night, morning headache , smoking history, BMI 36 , next?? |
Nocturnal polysomnography ( the gold standard for OSA) |
|
|
Asthma exacerbation treated with albuterol and IV methylprednisolone, the next day she developed high leukocytosis with bands form ?? |
Medication effect ( steroids) |
|

Left sided chest discomfort, history of accident 2 months ago , X-ray : mediastinal deviation , next ?? |
CT of chest and abdomen ( to role out diaphragm rupture) |
|
|
19, has asthma-like symptoms after Twice a week workout sessions??? |
Exercise induced bronchoconstriction Rx: inhaled albuterol 10 minutes before exercise Ps: if she exercise daily then she should use inhaled corticosteroids. |
|
|
HIV, noncompliant with treatment, pulmonary symptoms( PCP), given abx and 5 L normal saline, after 2 days he developed hyponatremia with confusion??? |
SIADH which happens in euvolemia state |
|
|
Pneumonia symptoms on the left side , the oxygen saturation is normal when lying on right side, but it decreased when lying of the left side ( affected side ) , why ?? |
Intrapulmonary shunting ( right to left) of blood due to gravity |
|
|
6th rib fracture, base atelectasis , best essential Rx?? |
Pain control to maintain adequate ventilation |
|
|
3- weeks of hacking, nonproductive cough , sensation of dripping into back of his neck, no other symptoms, next ? |
Oral antihistamine first generation ( upper airway cough syndrome) |
|
|
Flattering diaphragm in COPD leads to ?? |
Increase work of breathing |
|
|
Elasticity and compliance in COPD |
Decreased elasticity Increased compliance |
|
|
Infant, doesn’t gain weight, loose oily bowel movement, has pulmonary symptoms, had pneumonia month ago, small boy, what other findings??? |
Absence of bilateral vas deferens ( male infertility ) by cystic fibrosis Dx: elevation sweat chloride Rx: airway clearance, broad spectrum abx ( staph, pseudo) |
|
|
Pulmonary right sided symptoms, Pleural effusion: glucose < 60, pH< 7.2 , LDH 620 ?? |
Pneumonia with complicated( exudate) parapneumonic effusion Rx: abx and drainage |
|

34, hemoptysis, sudden right- sided chest pain with dyspnea, pain increase with deep breathing, history of HIV, heroin, cellulitis, CD4 is 350, tachycardia??? |
Pulmonary thromboembolism |
|
|
35, fell on stairs, having pain in shoulder, X-ray: reveals normal shoulder and 1.5 cm lesion in the right lung , next ? |
Ask for previous X-ray for comparison ( absence of growth over 2-3 years rules out malignancy) if previous X-ray not available do CT |
|
|
Pulmonary function test in chronic lung disease |

Back (Definition) |
|
|
56, progressive exertional dyspnea,no Pulmonary symptoms, insulation and plumbing worker, digital clubbing, bibasilar crackles, the PFTs finding ?? |
Decreased diffusion lung capacity( asbestosis) Dx: pleural plaques on imaging |
|
|
60, undergoing surgery, he vomited during intubation, after 4 hours postoperative he becomes tachypnea and hypoxia, bilateral crackles?? |
Inflammatory reaction to aspirated gastric acid (pneumonitis ) Rx: supportive Ps: aspiration pneumonia: infection after days, fever, Rx ( antibiotics) |
|

Flattering diaphragm in COPD leads to ?? |
Increase work of breathing |
|
|
24, evaluation of PFTs due to dyspnea, low back pain improves with activity, FEV1/FVC 95%, Vital capacity is decreased??? |
Chest wall motion restriction due to ankylosing spondylitis |
|
|
Ct scan of solitary nodule management |
Benign: serial CT scans Intermediate suspicious of malignancy: biopsy or PET scan High suspicious for malignancy: surgical excision |
|
|
Fat embolism characteristics |
Respiratory distress, neurological abnormalities, petechial rash |
|
|
Accident, symptoms...etc, Po2 was 81, after giving fluids the PO2 becomes 75, bilateral diffuse rales in both lungs?? |
Pulmonary contusion |
|
|
65, lung nodule irregular without calcification , smoking history, 2-cm, in the right lower lobe , Best next step ?? |
Surgical excision ( high suspicious malignancy) |
|
|
Solitary pulmonary nodule on routine chest X-ray chart page 534 |

Back (Definition) |
|
|
Causes of hypoxemia page 571 |
571 |
|
|
Complications of positive pressure ventilation for ARDS |
Alveolar damage, pneumothorax, hypotension |
|
|
ARDS Patient, after giving positive pressure ventilation developed SOB , hypotension, tachycardia, tracheal deviation, unilateral breath sound absence?? |
Pneumothorax |
|
|
Postpartum cesarean sudden onset of severe dyspnea and right sided chest pain , moderate respiratory distress, ECG sinus tachy , next ?? |
IV heparin ( not CT angiogram because the patient is moderate distress and there is not contraindications for anticoagulant) after heparin do the CT .. |
|
|
COPD acute exacerbation management ( severe and moderate) ?? |
Oxygen, inhaled bronchodilator, systemic corticosteroids, Abx( if > 2 symptoms), oseltamivir( if influenza), NPPV( if ventilatory failure, tracheal intubation NPPV: noninvasive positive pressure ventilation |
|
|
COPD, sudden severe dyspnea and right sided chest pain, E: no tracheal deviation, tactile fremitus and breath sounds are decreased in right side , wheezing in left, why ?? |
Rupture of an apical alveolar bleb( secondary spontaneous pneumothorax ) |
|
|
34, hemoptysis, sudden right- sided chest pain with dyspnea, pain increase with deep breathing, history of HIV, heroin, cellulitis, CD4 is 350, tachycardia??? |
Pulmonary thromboembolism |
|
|
Accident, Hypotension, tachycardia, tachypnea, trachea shifted to right, on left absent breath sound and dullness??? |
Hemothorax |
|
|
Pulmonary function test in chronic lung disease |
Back (Definition) |
|
|
68, Navy worker, progressive dyspnea dry cough for a year, fine crackles ? |
Idiopathic Pulmonary fibrosis due to restrictive profile ( decreased DLCO and TLC, normal FEV1/FVC ) |
|
|
40, exertional dyspnea for 6 months, decreased breath sounds, mild LFTs elevated, his father died from cirrhosis ??? |
Alpha-1 antitrypsin deficiency |
|
|
3- weeks of hacking, nonproductive cough , sensation of dripping into back of his neck, no other symptoms, next ? |
Oral antihistamine first generation ( upper airway cough syndrome) |
|
|
Flattering diaphragm in COPD leads to ?? |
Increase work of breathing |
|
|
Elasticity and compliance in COPD |
Decreased elasticity Increased compliance |
|
|
Infant, doesn’t gain weight, loose oily bowel movement, has pulmonary symptoms, had pneumonia month ago, small boy, what other findings??? |
Absence of bilateral vas deferens ( male infertility ) by cystic fibrosis Dx: elevation sweat chloride Rx: airway clearance, broad spectrum abx ( staph, pseudo) |
|
|
Pulmonary right sided symptoms, Pleural effusion: glucose < 60, pH< 7.2 , LDH 620 ?? |
Pneumonia with complicated( exudate) parapneumonic effusion Rx: abx and drainage |
|
34, hemoptysis, sudden right- sided chest pain with dyspnea, pain increase with deep breathing, history of HIV, heroin, cellulitis, CD4 is 350, tachycardia??? |
Pulmonary thromboembolism |
|
|
35, fell on stairs, having pain in shoulder, X-ray: reveals normal shoulder and 1.5 cm lesion in the right lung , next ? |
Ask for previous X-ray for comparison ( absence of growth over 2-3 years rules out malignancy) if previous X-ray not available do CT |
|
|
Pulmonary function test in chronic lung disease |

Back (Definition) |
|
|
56, progressive exertional dyspnea,no Pulmonary symptoms, insulation and plumbing worker, digital clubbing, bibasilar crackles, the PFTs finding ?? |
Decreased diffusion lung capacity( asbestosis) Dx: pleural plaques on imaging |
|
|
60, undergoing surgery, he vomited during intubation, after 4 hours postoperative he becomes tachypnea and hypoxia, bilateral crackles?? |
Inflammatory reaction to aspirated gastric acid (pneumonitis ) Rx: supportive Ps: aspiration pneumonia: infection after days, fever, Rx ( antibiotics) |
|
|
Flattering diaphragm in COPD leads to ?? |
Increase work of breathing |
|
|
24, evaluation of PFTs due to dyspnea, low back pain improves with activity, FEV1/FVC 95%, Vital capacity is decreased??? |
Chest wall motion restriction due to ankylosing spondylitis |
|
|
Ct scan of solitary nodule management |
Benign: serial CT scans Intermediate suspicious of malignancy: biopsy or PET scan High suspicious for malignancy: surgical excision |
|
|
Fat embolism characteristics |
Respiratory distress, neurological abnormalities, petechial rash |
|
|
Accident, symptoms...etc, Po2 was 81, after giving fluids the PO2 becomes 75, bilateral diffuse rales in both lungs?? |
Pulmonary contusion |
|
|
65, lung nodule irregular without calcification , smoking history, 2-cm, in the right lower lobe , Best next step ?? |
Surgical excision ( high suspicious malignancy) |
|
|
Solitary pulmonary nodule on routine chest X-ray chart page 534 |

Back (Definition) |
|
|
Causes of hypoxemia page 571 |
571 |
|
|
Complications of positive pressure ventilation for ARDS |
Alveolar damage, pneumothorax, hypotension |
|
|
ARDS Patient, after giving positive pressure ventilation developed SOB , hypotension, tachycardia, tracheal deviation, unilateral breath sound absence?? |
Pneumothorax |
|
|
اللهم نجحني |
اللهم اجعلني من المتفوقين يا الله |
|
|
Postpartum cesarean sudden onset of severe dyspnea and right sided chest pain , moderate respiratory distress, ECG sinus tachy , next ?? |
IV heparin ( not CT angiogram because the patient is moderate distress and there is not contraindications for anticoagulant) after heparin do the CT .. |
|
|
COPD acute exacerbation management ( severe and moderate) ?? |
Oxygen, inhaled bronchodilator, systemic corticosteroids, Abx( if > 2 symptoms), oseltamivir( if influenza), NPPV( if ventilatory failure, tracheal intubation NPPV: noninvasive positive pressure ventilation |
|
|
COPD, sudden severe dyspnea and right sided chest pain, E: no tracheal deviation, tactile fremitus and breath sounds are decreased in right side , wheezing in left, why ?? |
Rupture of an apical alveolar bleb( secondary spontaneous pneumothorax ) |
|
|
34, hemoptysis, sudden right- sided chest pain with dyspnea, pain increase with deep breathing, history of HIV, heroin, cellulitis, CD4 is 350, tachycardia??? |
Pulmonary thromboembolism |
|
|
Accident, Hypotension, tachycardia, tachypnea, trachea shifted to right, on left absent breath sound and dullness??? |
Hemothorax |
|
|
Pulmonary function test in chronic lung disease |
Back (Definition) |
|
|
68, Navy worker, progressive dyspnea dry cough for a year, fine crackles ? |
Idiopathic Pulmonary fibrosis due to restrictive profile ( decreased DLCO and TLC, normal FEV1/FVC ) |
|
|
40, exertional dyspnea for 6 months, decreased breath sounds, mild LFTs elevated, his father died from cirrhosis ??? |
Alpha-1 antitrypsin deficiency |
|
|
3- weeks of hacking, nonproductive cough , sensation of dripping into back of his neck, no other symptoms, next ? |
Oral antihistamine first generation ( upper airway cough syndrome) |
|
|
Flattering diaphragm in COPD leads to ?? |
Increase work of breathing |
|
|
Elasticity and compliance in COPD |
Decreased elasticity Increased compliance |
|
|
Infant, doesn’t gain weight, loose oily bowel movement, has pulmonary symptoms, had pneumonia month ago, small boy, what other findings??? |
Absence of bilateral vas deferens ( male infertility ) by cystic fibrosis Dx: elevation sweat chloride Rx: airway clearance, broad spectrum abx ( staph, pseudo) |
|
|
Pulmonary right sided symptoms, Pleural effusion: glucose < 60, pH< 7.2 , LDH 620 ?? |
Pneumonia with complicated( exudate) parapneumonic effusion Rx: abx and drainage |
|
|
22, 188cm, BMI 19, sudden dyspnea while watching tv, the dyspnea gradual improves but still the sharp pain with deep inspiration, X-ray: small right apical pneumothorax , Rx? |
Supplement oxygen ( primary spontaneous pneumothorax) Dx: visceral pleural line on X-ray Ps:: If Large and stable patient: ( needle thoracostomy) If unstable: tube thoracostomy |
|
|
35, fell on stairs, having pain in shoulder, X-ray: reveals normal shoulder and 1.5 cm lesion in the right lung , next ? |
Ask for previous X-ray for comparison ( absence of growth over 2-3 years rules out malignancy) if previous X-ray not available do CT |
|
|
Solitary pulmonary nodule on routine chest X-ray chart page 534 |
Back (Definition) |
|
|
56, progressive exertional dyspnea,no Pulmonary symptoms, insulation and plumbing worker, digital clubbing, bibasilar crackles, the PFTs finding ?? |
Decreased diffusion lung capacity( asbestosis) Dx: pleural plaques on imaging |
|
|
60, undergoing surgery, he vomited during intubation, after 4 hours postoperative he becomes tachypnea and hypoxia, bilateral crackles?? |
Inflammatory reaction to aspirated gastric acid (pneumonitis ) Rx: supportive Ps: aspiration pneumonia: infection after days, fever, Rx ( antibiotics) |
|
|
Solitary nodule round with sharp borders 1cm, previous 3 years X-ray was normal, next? |
CT of the chest |
|
|
24, evaluation of PFTs due to dyspnea, low back pain improves with activity, FEV1/FVC 95%, Vital capacity is decreased??? |
Chest wall motion restriction due to ankylosing spondylitis |
|
|
Ct scan of solitary nodule management |
Benign: serial CT scans Intermediate suspicious of malignancy: biopsy or PET scan High suspicious for malignancy: surgical excision |
|
|
Fat embolism characteristics |
Respiratory distress, neurological abnormalities, petechial rash |
|
|
Accident, symptoms...etc, Po2 was 81, after giving fluids the PO2 becomes 75, bilateral diffuse rales in both lungs?? |
Pulmonary contusion |
|
|
65, lung nodule irregular without calcification , smoking history, 2-cm, in the right lower lobe , Best next step ?? |
Surgical excision ( high suspicious malignancy) |
|
|
53, several days of SOB, productive cough, uses heroin IV, fever, oxygen saturation is 89%, extensive white plaques on oral mucosa, bilateral crackles, mechanism of hypoxemia ?? |
Ventilation/ perfusion mismatch ( right to left intrapulmonary shunt) due to pneumonia ( mostly PCP) |
|
|
Causes of hypoxemia page 571 |
571 |
|
|
Complications of positive pressure ventilation for ARDS |
Alveolar damage, pneumothorax, hypotension |
|
|
ARDS Patient, after giving positive pressure ventilation developed SOB , hypotension, tachycardia, tracheal deviation, unilateral breath sound absence?? |
Pneumothorax |
|
|
اللهم نجحني |
اللهم اجعلني من المتفوقين يا الله |
|
|
Postpartum cesarean sudden onset of severe dyspnea and right sided chest pain , moderate respiratory distress, ECG sinus tachy , next ?? |
IV heparin ( not CT angiogram because the patient is moderate distress and there is not contraindications for anticoagulant) after heparin do the CT .. |
|
|
COPD acute exacerbation management ( severe and moderate) ?? |
Oxygen, inhaled bronchodilator, systemic corticosteroids, Abx( if > 2 symptoms), oseltamivir( if influenza), NPPV( if ventilatory failure, tracheal intubation NPPV: noninvasive positive pressure ventilation |
|
|
COPD, sudden severe dyspnea and right sided chest pain, E: no tracheal deviation, tactile fremitus and breath sounds are decreased in right side , wheezing in left, why ?? |
Rupture of an apical alveolar bleb( secondary spontaneous pneumothorax ) |
|
|
34, hemoptysis, sudden right- sided chest pain with dyspnea, pain increase with deep breathing, history of HIV, heroin, cellulitis, CD4 is 350, tachycardia??? |
Pulmonary thromboembolism |
|
|
Accident, Hypotension, tachycardia, tachypnea, trachea shifted to right, on left absent breath sound and dullness??? |
Hemothorax |
|
|
Pulmonary function test in chronic lung disease |
Back (Definition) |
|
|
68, Navy worker, progressive dyspnea dry cough for a year, fine crackles ? |
Idiopathic Pulmonary fibrosis due to restrictive profile ( decreased DLCO and TLC, normal FEV1/FVC ) |
|
|
40, exertional dyspnea for 6 months, decreased breath sounds, mild LFTs elevated, his father died from cirrhosis ??? |
Alpha-1 antitrypsin deficiency |
|
|
54, chronic cough and blood sputum, weight loss, fatigue, X-ray: hilar mass in left lung, hypercalcemia ???? |
Squamous cell carcinoma |
|
|
Paraneoplastic syndromes in small cell carcinoma of lung ?? |
ACTH, SIADH |
|
|
Child, same cystic fibrosis symptoms ( recurrent infections), point of maximal impulse is on right chest ??? |
Kartagener syndrome ( primary ciliary dyskinesia) Dx: low nasal nitric acid |
|
|
Asthma exacerbation, given inhaled albuterol and systemic steroids intubated, after 6 hours the attack is gone and she can’t rise her arms above head , tremor, next?? |
Serum electrolytes ( albuterol causes hypokalemia) |
|
|
13 day, clear runny nose, cough , E: bilateral wheezing and crackles, complication?? |
Apnea ( bronchiolitis caused by respiratory syncytial virus) Rx: supportive Prevention: palivizumab |
|
|
Child, Situs inversus, recurrent sinusitis, bronchiectasis ?? |
Kartagener syndrome |
|
|
Postoperative day, oxygen saturation 89%, respiratory acidosis??? |
Alveolar hypoventilation |
|
|
Normal A-a gradient ( PAO2-PaO2) |
< 15 If > 30 it’s considered elevated |
|
|
33, repeated episodes of generalized symptoms with pulmonary symptoms for 6 months, comes suddenly and last several days, she breeds budgerigars, serology: antibodies to the bird antigen, Rx? |
Avoid exposure to birds ( hypersensitivity pneumonitis ) |
|
|
36, dyspnea on exertion, lungs are clear, X-ray: prominent pulmonary arteries, enlarged right heart?? |
Primary Pulmonary hypertension |
|

COPD exacerbation, treated with oxygen, IV antibiotics, ...etc, but she still dyspneic and use accessory muscles, she still alert , next ?? |
Start noninvasive positive pressure ventilation ( decreased mortality), if failed do mechanical ventilation |
|
|
55, recurrent pneumonia in last 4 months, and now also , smoking, leukocytosis, fever previous and current X-ray reveal consolidation in right lower lung( same place ) next? |
CT scan to role out malignancy ( localized airway obstruction) |
|
|
COPD exacerbation, treated with oxygen, IV antibiotics, ...etc, but she still dyspneic and use accessory muscles, she still alert , next ?? |
Start noninvasive positive pressure ventilation ( decreased mortality), if failed do mechanical ventilation |
|
|
Asthma patient taking albuterol, he has 3-4 night symptoms in month, next step ? |
Add corticosteroids |
|
|
Child, same cystic fibrosis symptoms ( recurrent infections), point of maximal impulse is on right chest ??? |
Kartagener syndrome ( primary ciliary dyskinesia) Dx: low nasal nitric acid |
|
|
Asthma exacerbation, given inhaled albuterol and systemic steroids intubated, after 6 hours the attack is gone and she can’t rise her arms above head , tremor, next?? |
Serum electrolytes ( albuterol causes hypokalemia) |
|
|
13 day, clear runny nose, cough , E: bilateral wheezing and crackles, complication?? |
Apnea ( bronchiolitis caused by respiratory syncytial virus) Rx: supportive Prevention: palivizumab |
|
|
يا رحمن يا رحيم ، يا غفور يا كريم |
اكتبني من الناجحين المتفوقين في الامتحان يا الله |
|
|
Child, Situs inversus, recurrent sinusitis, bronchiectasis ?? |
Kartagener syndrome |
|
|
Postoperative day, oxygen saturation 89%, respiratory acidosis??? |
Alveolar hypoventilation |
|
|
Normal A-a gradient ( PAO2-PaO2) |
< 15 If > 30 it’s considered elevated |
|
|
33, repeated episodes of generalized symptoms with pulmonary symptoms for 6 months, comes suddenly and last several days, she breeds budgerigars, serology: antibodies to the bird antigen, Rx? |
Avoid exposure to birds ( hypersensitivity pneumonitis ) |
|
COPD exacerbation, treated with oxygen, IV antibiotics, ...etc, but she still dyspneic and use accessory muscles, she still alert , next ?? |
Start noninvasive positive pressure ventilation ( decreased mortality), if failed do mechanical ventilation |
|
|
Asthma exacerbation, pH: 7.43, PaO2: 65, PaCO2: 40, which indicator of patient getting worse ?? |
Normal PaCO2 ( because in asthma exacerbation usually respiratory alkalosis developed, which means the PaCO2 must be low ) Ps: if PaCO2 is normal or elevated in asthma exacerbation it’s mean respiratory failure |
|
|
55, recurrent pneumonia in last 4 months, and now also , smoking, leukocytosis, fever previous and current X-ray reveal consolidation in right lower lung( same place ) next? |
CT scan to role out malignancy ( localized airway obstruction) |
|
|
COPD exacerbation, treated with oxygen, IV antibiotics, ...etc, but she still dyspneic and use accessory muscles, she still alert , next ?? |
Start noninvasive positive pressure ventilation ( decreased mortality), if failed do mechanical ventilation |
|
|
Asthma patient taking albuterol, he has 3-4 night symptoms in month, next step ? |
Add corticosteroids |
|
|
Child, same cystic fibrosis symptoms ( recurrent infections), point of maximal impulse is on right chest ??? |
Kartagener syndrome ( primary ciliary dyskinesia) Dx: low nasal nitric acid |
|
|
Asthma exacerbation, given inhaled albuterol and systemic steroids intubated, after 6 hours the attack is gone and she can’t rise her arms above head , tremor, next?? |
Serum electrolytes ( albuterol causes hypokalemia) |
|
|
13 day, clear runny nose, cough , E: bilateral wheezing and crackles, complication?? |
Apnea ( bronchiolitis caused by respiratory syncytial virus) Rx: supportive Prevention: palivizumab |
|
|
يا رحمن يا رحيم ، يا غفور يا كريم |
اكتبني من الناجحين المتفوقين في الامتحان يا الله |
|
|
Child, Situs inversus, recurrent sinusitis, bronchiectasis ?? |
Kartagener syndrome |
|
|
Postoperative day, oxygen saturation 89%, respiratory acidosis??? |
Alveolar hypoventilation |
|
|
Normal A-a gradient ( PAO2-PaO2) |
< 15 If > 30 it’s considered elevated |
|
|
33, repeated episodes of generalized symptoms with pulmonary symptoms for 6 months, comes suddenly and last several days, she breeds budgerigars, serology: antibodies to the bird antigen, Rx? |
Avoid exposure to birds ( hypersensitivity pneumonitis ) |
|

COPD exacerbation, treated with oxygen, IV antibiotics, ...etc, but she still dyspneic and use accessory muscles, she still alert , next ?? |
Start noninvasive positive pressure ventilation ( decreased mortality), if failed do mechanical ventilation |
|
|
Asthma exacerbation, pH: 7.43, PaO2: 65, PaCO2: 40, which indicator of patient getting worse ?? |
Normal PaCO2 ( because in asthma exacerbation usually respiratory alkalosis developed, which means the PaCO2 must be low ) Ps: if PaCO2 is normal or elevated in asthma exacerbation it’s mean respiratory failure |
|
|
55, recurrent pneumonia in last 4 months, and now also , smoking, leukocytosis, fever previous and current X-ray reveal consolidation in right lower lung( same place ) next? |
CT scan to role out malignancy ( localized airway obstruction) |
|
|
COPD exacerbation, treated with oxygen, IV antibiotics, ...etc, but she still dyspneic and use accessory muscles, she still alert , next ?? |
Start noninvasive positive pressure ventilation ( decreased mortality), if failed do mechanical ventilation |
|
|
Asthma patient taking albuterol, he has 3-4 night symptoms in month, next step ? |
Add corticosteroids |
|
|
Respiratory distress syndrome in infant risk factor?? |
Prematurity, maternal DM |
|
|
24, worsening productive cough with tenacious sputum, fever, SOB for a week, hemoptysis, had these symptoms before improving with abx but never gone , E: Upper lung fields crackles, digital clubbing, cause ?? |
Defective chloride channel ( Bronchiectasis caused by CF) Dx: High resolution CT |
|
|
31, SOB, anxiety, no others symptoms, the symptoms resolved after one hour, next ? |
D-dimer ( if normal: reassurance, if elevated follow up) |
|
|
38, dry cough , malaise, bilateral hilar adenopathy ?? |
Sarcoidosis ( noncaseating granulomatous inflammation) |
|
|
Mechanical ventilation, FiO2 is 70%, PaO2: 54, PaCO2: 30, next ? |
Increase PEEP to maintain the oxygenation( ps: u can also increase the FiO2 but when it’s < 60) |
|
|
69, SOB, cough, Edema, faint heart sound, JVD: 11, decreased breath sounds, hepatomegaly and ascites, X-ray: enlargement of central pulmonary arteries???? |
Cor pulmonale ( isolated right heart failure due to pulmonary hypertension) |
|
|
The indication for initiation long term home oxygen therapy? |
Oxygen saturation < 88 |
|
|
Indications for long term oxygen therapy |
1. PaO2< 55 or SaO2 < 88 2. (PaO2 < 59 or SaO2< 89) with hematocrit > 55 |
|
|
53, 2 episodes of hemoptysis, history of 2 years morning cough producing white sputum, smoker, construction? |
Chronic bronchitis |
|
|
55, fever, SOB, productive cough, foul smelling sputum, history of acute pancreatitis, Bar fight, E: missing teeth, dense lower lobe infiltrate?? |
Aspiration pneumonia due to alcoholism |
|
|
12, bee sting, developed full body hives, difficulty breathing, vomiting, history of moderate persistent asthma, after giving im epinephrine she got better, after 10 minutes the symptoms returned, next ? |
Im epinephrine ( as needed) for anaphylaxis Prevention: venom immunotherapy |
|
|
Newborn in respiratory distress syndrome, BP 70/40, nasal flaring, grunting, absent breath sound on the left, scaphoid abdomen, next ?? |
Endotracheal intubation ( congenital diaphragmatic hernia), then gastric tube to decompress the bowel |
|
|
Postoperative cough and some sputum, E: decreased breath sounds at right lung base without wheezing or prolonged expiration, arterial blood gases will be ??? |
Decreased PCO2 and PO2, increased pH ( respiratory alkalosis due to atelectasis) Rx and preoperative prevention: breathing exercise |
|
|
42, difficulty breathing and wheezing, history of persistent nasal blockage, had angina 6 months ago which taking medications ( aspirin,atovarsatin ..etc) , why the respiratory symptoms??? |
Pseudoallergic drug reaction ( aspirin respiratory disease) Rx: stop NSAIDs, use leukotriene receptor antagonists( montelukast) |
|
|
Postoperative, so many symptoms ( hypotension, leukocytosis, Fever...etc) , next step? |
IV normal saline 0.9%( for hypertension caused by septic shock) , then vasopressors( dopamine) |
|
|
Shoulder pain, hand pain with chronic pulmonary symptoms , horner syndrome, next ?? |
chest X-ray ( Superior pulmonary sulcus tumors of lung) |
|
|
COPD increased survival interventions?? |
Long-term supplemental oxygen ( for significant hypoxemia ) Ps: significant hypoxemia( 1. PaO2< 55 or SaO2< 88, 2. If none there and hematocrit > 55 |
|
|
Right upper lobe perfusion defect with good ventilation, the GFR is 20 ( < 30 ), Rx? |
Unfractionated heparin ( due to renal insufficiency) |
|
|
Patient on mechanical ventilation, FiO2 is 80%, PaO2 is 105, PaCo2 is 37 , next ?? |
Decrease fraction of inspiration oxygen below 60% (FiO2 < 60%) to prevent oxygen toxicity |
|
|
Asthma patient, progressive asthma symptoms, no dyspnea , her throat is sore and hoarseness that resolves during the day , next ? |
Add omeprazole ( comorbid GERD causing asthma exacerbation) |
|
|
Respiratory distress syndrome in infant risk factor?? |
Prematurity, maternal DM |
|
|
24, worsening productive cough with tenacious sputum, fever, SOB for a week, hemoptysis, had these symptoms before improving with abx but never gone , E: Upper lung fields crackles, digital clubbing, cause ?? |
Defective chloride channel ( Bronchiectasis caused by CF) Dx: High resolution CT |
|
|
31, SOB, anxiety, no others symptoms, the symptoms resolved after one hour, next ? |
D-dimer ( if normal: reassurance, if elevated follow up) |
|
|
38, dry cough , malaise, bilateral hilar adenopathy ?? |
Sarcoidosis ( noncaseating granulomatous inflammation) |
|
|
Mechanical ventilation, FiO2 is 70%, PaO2: 54, PaCO2: 30, next ? |
Increase PEEP to maintain the oxygenation( ps: u can also increase the FiO2 but when it’s < 60) |
|
|
69, SOB, cough, Edema, faint heart sound, JVD: 11, decreased breath sounds, hepatomegaly and ascites, X-ray: enlargement of central pulmonary arteries???? |
Cor pulmonale ( isolated right heart failure due to pulmonary hypertension) |
|
|
The indication for initiation long term home oxygen therapy? |
Oxygen saturation < 88 |
|
|
Indications for long term oxygen therapy |
1. PaO2< 55 or SaO2 < 88 2. (PaO2 < 59 or SaO2< 89) with hematocrit > 55 |
|
|
53, 2 episodes of hemoptysis, history of 2 years morning cough producing white sputum, smoker, construction? |
Chronic bronchitis |
|
|
55, fever, SOB, productive cough, foul smelling sputum, history of acute pancreatitis, Bar fight, E: missing teeth, dense lower lobe infiltrate?? |
Aspiration pneumonia due to alcoholism |
|
|
12, bee sting, developed full body hives, difficulty breathing, vomiting, history of moderate persistent asthma, after giving im epinephrine she got better, after 10 minutes the symptoms returned, next ? |
Im epinephrine ( as needed) for anaphylaxis Prevention: venom immunotherapy |
|
|
Newborn in respiratory distress syndrome, BP 70/40, nasal flaring, grunting, absent breath sound on the left, scaphoid abdomen, next ?? |
Endotracheal intubation ( congenital diaphragmatic hernia), then gastric tube to decompress the bowel |
|
|
Collision, pulse oximetry 88, no tracheal deviation, several chest wall bruises, right chest moves inward during inspiration, decreased breath sounds?? |
Rib fractures( > 3 ) leading to flail chest Rx: pain control, oxygen |
|
|
Asthma patient, difficulty in breathing one hour ago, had antibiotic earlier this morning for upper respiratory infection, hypotension, E: urticarial rash over the body, next ?? |
Im epinephrine ( anaphylaxis due to allergy to antibiotics) |
|
|
COPD exacerbation management |
Bronchodilators( B-agonist and anticholinergic) and Systemic glucocorticoids ( methylprednisolone) , oxygen... |
|
|
53, plumber, smoking history, 4 months of progressive dyspnea, weight loss, E: bilateral pleural plaques, 6 cm cavity mass in right lower lung ?? |
Bronchogenic carcinoma ( asbestos exposure) |
|
|
Collision, unresponsive, BP is 70/30, no tracheal deviation, extremities are cold, tachycardia, what also ?? |
Small left ventricle with ejection fraction of 75% |
|
|
Cough with blood tinged sputum, history of malaise congestion sore throat 10 days ago, no other findings, X-ray normal, scattered bilateral wheezing and crackles clear with cough , next ?? |
Symptomatic treatment only ( acute bronchitis caused by upper respiratory viral infection ), don’t use abx |
|
|
ACEi using, chronic nonproductive cough ?? |
Side effect by increasing levels of kinins, substance P, prostaglandins, thromboxane |
|
|
History of cancer, unconscious, severe hypotension, elevated pulmonary artery and right atrial pressure, normal PCWP ???? |
Pulmonary embolism If PCWP is elevated the cause will be left ventricle dysfunction |
|
|
Elevated PCWP means? |
Left ventricle dysfunction |
|
|
66, exertional dyspnea for 2 years, recurrent cough productive of whitish sputum, E: scattered expiratory wheezing, Rx?? |
Muscarinic antagonist ( COPD) |
|
|
Postoperative cough and some sputum, E: decreased breath sounds at right lung base without wheezing or prolonged expiration, arterial blood gases will be ??? |
Decreased PCO2 and PO2, increased pH ( respiratory alkalosis due to atelectasis) Rx and preoperative prevention: breathing exercise |
|
|
37, transplant, cough with bright blood, fever, pleuritic pain, E: right upper lobe dense infiltrate grown in size, CT: several nodular lesions with surrounding ground-glass( halo sign) opacities ?? |
Invasive aspergillosis Rx: voriconazole and caspofungin |
|
|
54, fatigue, cough with blood for few months , weight loss , immigrant treated for TB 10 years ago ?? |
Chronic pulmonary aspergillosis Dx: IgG aspergillus serology |
|
|
COPD exacerbation, oxygen saturation 91%, given medications with high facial mask oxygen,he developed seizure why ?? |
Carbon dioxide retention ( due to supplemental oxygen causing V/Q mismatch) |
|
|
PE Patient with obesity on further evaluation what the arterial blood gas gradient?? |
High alveolar-arterial gradient |
|
|
COPD exacerbation acid-base status?? |
Respiratory acidosis , widespread wheezing |
|
|
66, SOB, history of hypertension, stenting , E: decreased breath sounds at bases, bilateral crackles, occasional wheezes, respiratory alkalosis, ??? |
CHF |
|
|
Transudate vs exudate effusion |
Transudate: decreased oncotic pressures, elevated hydrostatic Exudate: increased permeability, disruption to lymphatic outflow |
|
|
Exudate criteria |
Protein ( pleural/ serum) > 5 or LDH( pleural/serum) > 0.6 or Pleural LDH > two thirds upper limit of normal serum LDH |
|

54, fatigue, cough with blood for few months , weight loss , immigrant treated for TB 10 years ago ?? |
Chronic pulmonary aspergillosis Dx: IgG aspergillus serology |
|
|
42, difficulty breathing and wheezing, history of persistent nasal blockage, had angina 6 months ago which taking medications ( aspirin,atovarsatin ..etc) , why the respiratory symptoms??? |
Pseudoallergic drug reaction ( aspirin respiratory disease) Rx: stop NSAIDs, use leukotriene receptor antagonists( montelukast) |
|
|
Postoperative, so many symptoms ( hypotension, leukocytosis, Fever...etc) , next step? |
IV normal saline 0.9%( for hypertension caused by septic shock) , then vasopressors( dopamine) |
|
|
Shoulder pain, hand pain with chronic pulmonary symptoms , horner syndrome, next ?? |
chest X-ray ( Superior pulmonary sulcus tumors of lung) |
|
|
COPD increased survival interventions?? |
Long-term supplemental oxygen ( for significant hypoxemia ) Ps: significant hypoxemia( 1. PaO2< 55 or SaO2< 88, 2. If none there and hematocrit > 55 |
|
|
Right upper lobe perfusion defect with good ventilation, the GFR is 20 ( < 30 ), Rx? |
Unfractionated heparin ( due to renal insufficiency) |
|
|
Patient on mechanical ventilation, FiO2 is 80%, PaO2 is 105, PaCo2 is 37 , next ?? |
Decrease fraction of inspiration oxygen below 60% (FiO2 < 60%) to prevent oxygen toxicity |
|
|
Asthma patient, progressive asthma symptoms, no dyspnea , her throat is sore and hoarseness that resolves during the day , next ? |
Add omeprazole ( comorbid GERD causing asthma exacerbation) |
|
|
Respiratory distress syndrome in infant risk factor?? |
Prematurity, maternal DM |
|
|
24, worsening productive cough with tenacious sputum, fever, SOB for a week, hemoptysis, had these symptoms before improving with abx but never gone , E: Upper lung fields crackles, digital clubbing, cause ?? |
Defective chloride channel ( Bronchiectasis caused by CF) Dx: High resolution CT |
|
|
31, SOB, anxiety, no others symptoms, the symptoms resolved after one hour, next ? |
D-dimer ( if normal: reassurance, if elevated follow up) |
|
|
38, dry cough , malaise, bilateral hilar adenopathy ?? |
Sarcoidosis ( noncaseating granulomatous inflammation) |
|
|
Mechanical ventilation, FiO2 is 70%, PaO2: 54, PaCO2: 30, next ? |
Increase PEEP to maintain the oxygenation( ps: u can also increase the FiO2 but when it’s < 60) |
|
|
69, SOB, cough, Edema, faint heart sound, JVD: 11, decreased breath sounds, hepatomegaly and ascites, X-ray: enlargement of central pulmonary arteries???? |
Cor pulmonale ( isolated right heart failure due to pulmonary hypertension) |
|
|
The indication for initiation long term home oxygen therapy? |
Oxygen saturation < 88 |
|
|
Indications for long term oxygen therapy |
1. PaO2< 55 or SaO2 < 88 2. (PaO2 < 59 or SaO2< 89) with hematocrit > 55 |
|
|
53, 2 episodes of hemoptysis, history of 2 years morning cough producing white sputum, smoker, construction? |
Chronic bronchitis |
|
|
55, fever, SOB, productive cough, foul smelling sputum, history of acute pancreatitis, Bar fight, E: missing teeth, dense lower lobe infiltrate?? |
Aspiration pneumonia due to alcoholism |
|
|
12, bee sting, developed full body hives, difficulty breathing, vomiting, history of moderate persistent asthma, after giving im epinephrine she got better, after 10 minutes the symptoms returned, next ? |
Im epinephrine ( as needed) for anaphylaxis Prevention: venom immunotherapy |
|
|
Newborn in respiratory distress syndrome, BP 70/40, nasal flaring, grunting, absent breath sound on the left, scaphoid abdomen, next ?? |
Endotracheal intubation ( congenital diaphragmatic hernia), then gastric tube to decompress the bowel |
|
|
Collision, pulse oximetry 88, no tracheal deviation, several chest wall bruises, right chest moves inward during inspiration, decreased breath sounds?? |
Rib fractures( > 3 ) leading to flail chest Rx: pain control, oxygen |
|
|
Asthma patient, difficulty in breathing one hour ago, had antibiotic earlier this morning for upper respiratory infection, hypotension, E: urticarial rash over the body, next ?? |
Im epinephrine ( anaphylaxis due to allergy to antibiotics) |
|
|
COPD exacerbation management |
Bronchodilators( B-agonist and anticholinergic) and Systemic glucocorticoids ( methylprednisolone) , oxygen... |
|
|
53, plumber, smoking history, 4 months of progressive dyspnea, weight loss, E: bilateral pleural plaques, 6 cm cavity mass in right lower lung ?? |
Bronchogenic carcinoma ( asbestos exposure) |
|
|
Collision, unresponsive, BP is 70/30, no tracheal deviation, extremities are cold, tachycardia, what also ?? |
Small left ventricle with ejection fraction of 75% |
|
|
Cough with blood tinged sputum, history of malaise congestion sore throat 10 days ago, no other findings, X-ray normal, scattered bilateral wheezing and crackles clear with cough , next ?? |
Symptomatic treatment only ( acute bronchitis caused by upper respiratory viral infection ), don’t use abx |
|
|
ACEi using, chronic nonproductive cough ?? |
Side effect by increasing levels of kinins, substance P, prostaglandins, thromboxane |
|
|
History of cancer, unconscious, severe hypotension, elevated pulmonary artery and right atrial pressure, normal PCWP ???? |
Pulmonary embolism If PCWP is elevated the cause will be left ventricle dysfunction |
|
|
Elevated PCWP means? |
Left ventricle dysfunction |
|
|
66, exertional dyspnea for 2 years, recurrent cough productive of whitish sputum, E: scattered expiratory wheezing, Rx?? |
Muscarinic antagonist ( COPD) |
|
|
Postoperative cough and some sputum, E: decreased breath sounds at right lung base without wheezing or prolonged expiration, arterial blood gases will be ??? |
Decreased PCO2 and PO2, increased pH ( respiratory alkalosis due to atelectasis) Rx and preoperative prevention: breathing exercise |
|
|
37, transplant, cough with bright blood, fever, pleuritic pain, E: right upper lobe dense infiltrate grown in size, CT: several nodular lesions with surrounding ground-glass( halo sign) opacities ?? |
Invasive aspergillosis Rx: voriconazole and caspofungin |
|
|
54, fatigue, cough with blood for few months , weight loss , immigrant treated for TB 10 years ago ?? |
Chronic pulmonary aspergillosis Dx: IgG aspergillus serology |
|
|
COPD exacerbation, oxygen saturation 91%, given medications with high facial mask oxygen,he developed seizure why ?? |
Carbon dioxide retention ( due to supplemental oxygen causing V/Q mismatch) |
|
|
PE Patient with obesity on further evaluation what the arterial blood gas gradient?? |
High alveolar-arterial gradient |
|
|
COPD exacerbation acid-base status?? |
Respiratory acidosis , widespread wheezing |
|
|
66, SOB, history of hypertension, stenting , E: decreased breath sounds at bases, bilateral crackles, occasional wheezes, respiratory alkalosis, ??? |
CHF |
|
|
Transudate vs exudate effusion |
Transudate: decreased oncotic pressures, elevated hydrostatic Exudate: increased permeability, disruption to lymphatic outflow |
|
|
Exudate criteria |
Protein ( pleural/ serum) > 5 or LDH( pleural/serum) > 0.6 or Pleural LDH > two thirds upper limit of normal serum LDH |
|
54, fatigue, cough with blood for few months , weight loss , immigrant treated for TB 10 years ago ?? |
Chronic pulmonary aspergillosis Dx: IgG aspergillus serology |
|
|
اللهم اني توكلت عليك يا قدير |
فلا تردني خائباً يا الله و نجحني في الامتحان |
|
|
42, difficulty breathing and wheezing, history of persistent nasal blockage, had angina 6 months ago which taking medications ( aspirin,atovarsatin ..etc) , why the respiratory symptoms??? |
Pseudoallergic drug reaction ( aspirin respiratory disease) Rx: stop NSAIDs, use leukotriene receptor antagonists( montelukast) |
|
|
Postoperative, so many symptoms ( hypotension, leukocytosis, Fever...etc) , next step? |
IV normal saline 0.9%( for hypertension caused by septic shock) , then vasopressors( dopamine) |
|
|
Shoulder pain, hand pain with chronic pulmonary symptoms , horner syndrome, next ?? |
chest X-ray ( Superior pulmonary sulcus tumors of lung) |
|
|
COPD increased survival interventions?? |
Long-term supplemental oxygen ( for significant hypoxemia ) Ps: significant hypoxemia( 1. PaO2< 55 or SaO2< 88, 2. If none there and hematocrit > 55 |
|
|
Right upper lobe perfusion defect with good ventilation, the GFR is 20 ( < 30 ), Rx? |
Unfractionated heparin ( due to renal insufficiency) |
|
|
Patient on mechanical ventilation, FiO2 is 80%, PaO2 is 105, PaCo2 is 37 , next ?? |
Decrease fraction of inspiration oxygen below 60% (FiO2 < 60%) to prevent oxygen toxicity |
|
|
Asthma patient, progressive asthma symptoms, no dyspnea , her throat is sore and hoarseness that resolves during the day , next ? |
Add omeprazole ( comorbid GERD causing asthma exacerbation) |
|
|
Respiratory distress syndrome in infant risk factor?? |
Prematurity, maternal DM |
|
|
24, worsening productive cough with tenacious sputum, fever, SOB for a week, hemoptysis, had these symptoms before improving with abx but never gone , E: Upper lung fields crackles, digital clubbing, cause ?? |
Defective chloride channel ( Bronchiectasis caused by CF) Dx: High resolution CT |
|
|
31, SOB, anxiety, no others symptoms, the symptoms resolved after one hour, next ? |
D-dimer ( if normal: reassurance, if elevated follow up) |
|
|
38, dry cough , malaise, bilateral hilar adenopathy ?? |
Sarcoidosis ( noncaseating granulomatous inflammation) |
|
|
Mechanical ventilation, FiO2 is 70%, PaO2: 54, PaCO2: 30, next ? |
Increase PEEP to maintain the oxygenation( ps: u can also increase the FiO2 but when it’s < 60) |
|
|
69, SOB, cough, Edema, faint heart sound, JVD: 11, decreased breath sounds, hepatomegaly and ascites, X-ray: enlargement of central pulmonary arteries???? |
Cor pulmonale ( isolated right heart failure due to pulmonary hypertension) |
|
|
The indication for initiation long term home oxygen therapy? |
Oxygen saturation < 88 |
|
|
Indications for long term oxygen therapy |
1. PaO2< 55 or SaO2 < 88 2. (PaO2 < 59 or SaO2< 89) with hematocrit > 55 |
|
|
53, 2 episodes of hemoptysis, history of 2 years morning cough producing white sputum, smoker, construction? |
Chronic bronchitis |
|
|
55, fever, SOB, productive cough, foul smelling sputum, history of acute pancreatitis, Bar fight, E: missing teeth, dense lower lobe infiltrate?? |
Aspiration pneumonia due to alcoholism |
|
|
12, bee sting, developed full body hives, difficulty breathing, vomiting, history of moderate persistent asthma, after giving im epinephrine she got better, after 10 minutes the symptoms returned, next ? |
Im epinephrine ( as needed) for anaphylaxis Prevention: venom immunotherapy |
|
|
Newborn in respiratory distress syndrome, BP 70/40, nasal flaring, grunting, absent breath sound on the left, scaphoid abdomen, next ?? |
Endotracheal intubation ( congenital diaphragmatic hernia), then gastric tube to decompress the bowel |
|
|
Collision, pulse oximetry 88, no tracheal deviation, several chest wall bruises, right chest moves inward during inspiration, decreased breath sounds?? |
Rib fractures( > 3 ) leading to flail chest Rx: pain control, oxygen |
|
|
Asthma patient, difficulty in breathing one hour ago, had antibiotic earlier this morning for upper respiratory infection, hypotension, E: urticarial rash over the body, next ?? |
Im epinephrine ( anaphylaxis due to allergy to antibiotics) |
|
|
COPD exacerbation management |
Bronchodilators( B-agonist and anticholinergic) and Systemic glucocorticoids ( methylprednisolone) , oxygen... |
|
|
53, plumber, smoking history, 4 months of progressive dyspnea, weight loss, E: bilateral pleural plaques, 6 cm cavity mass in right lower lung ?? |
Bronchogenic carcinoma ( asbestos exposure) |
|
|
Collision, unresponsive, BP is 70/30, no tracheal deviation, extremities are cold, tachycardia, what also ?? |
Small left ventricle with ejection fraction of 75% |
|
|
Cough with blood tinged sputum, history of malaise congestion sore throat 10 days ago, no other findings, X-ray normal, scattered bilateral wheezing and crackles clear with cough , next ?? |
Symptomatic treatment only ( acute bronchitis caused by upper respiratory viral infection ), don’t use abx |
|
|
ACEi using, chronic nonproductive cough ?? |
Side effect by increasing levels of kinins, substance P, prostaglandins, thromboxane |
|
|
History of cancer, unconscious, severe hypotension, elevated pulmonary artery and right atrial pressure, normal PCWP ???? |
Pulmonary embolism If PCWP is elevated the cause will be left ventricle dysfunction |
|
|
Elevated PCWP means? |
Left ventricle dysfunction |
|
|
66, exertional dyspnea for 2 years, recurrent cough productive of whitish sputum, E: scattered expiratory wheezing, Rx?? |
Muscarinic antagonist ( COPD) |
|
|
Postoperative cough and some sputum, E: decreased breath sounds at right lung base without wheezing or prolonged expiration, arterial blood gases will be ??? |
Decreased PCO2 and PO2, increased pH ( respiratory alkalosis due to atelectasis) Rx and preoperative prevention: breathing exercise |
|
|
37, transplant, cough with bright blood, fever, pleuritic pain, E: right upper lobe dense infiltrate grown in size, CT: several nodular lesions with surrounding ground-glass( halo sign) opacities ?? |
Invasive aspergillosis Rx: voriconazole and caspofungin |
|
|
54, fatigue, cough with blood for few months , weight loss , immigrant treated for TB 10 years ago ?? |
Chronic pulmonary aspergillosis Dx: IgG aspergillus serology |
|
|
COPD exacerbation, oxygen saturation 91%, given medications with high facial mask oxygen,he developed seizure why ?? |
Carbon dioxide retention ( due to supplemental oxygen causing V/Q mismatch) |
|
|
PE Patient with obesity on further evaluation what the arterial blood gas gradient?? |
High alveolar-arterial gradient |
|
|
COPD exacerbation acid-base status?? |
Respiratory acidosis , widespread wheezing |
|
|
66, SOB, history of hypertension, stenting , E: decreased breath sounds at bases, bilateral crackles, occasional wheezes, respiratory alkalosis, ??? |
CHF |
|
|
Transudate vs exudate effusion |
Transudate: decreased oncotic pressures, elevated hydrostatic Exudate: increased permeability, disruption to lymphatic outflow |
|
|
Exudate criteria |
Protein ( pleural/ serum) > 5 or LDH( pleural/serum) > 0.6 or Pleural LDH > two thirds upper limit of normal serum LDH |
|

54, fatigue, cough with blood for few months , weight loss , immigrant treated for TB 10 years ago ?? |
Chronic pulmonary aspergillosis Dx: IgG aspergillus serology |
|
|
اللهم اني توكلت عليك يا قدير |
فلا تردني خائباً يا الله و نجحني في الامتحان |
|
|
42, difficulty breathing and wheezing, history of persistent nasal blockage, had angina 6 months ago which taking medications ( aspirin,atovarsatin ..etc) , why the respiratory symptoms??? |
Pseudoallergic drug reaction ( aspirin respiratory disease) Rx: stop NSAIDs, use leukotriene receptor antagonists( montelukast) |
|
|
Postoperative, so many symptoms ( hypotension, leukocytosis, Fever...etc) , next step? |
IV normal saline 0.9%( for hypertension caused by septic shock) , then vasopressors( dopamine) |
|
|
Shoulder pain, hand pain with chronic pulmonary symptoms , horner syndrome, next ?? |
chest X-ray ( Superior pulmonary sulcus tumors of lung) |
|
|
COPD increased survival interventions?? |
Long-term supplemental oxygen ( for significant hypoxemia ) Ps: significant hypoxemia( 1. PaO2< 55 or SaO2< 88, 2. If none there and hematocrit > 55 |
|
|
Right upper lobe perfusion defect with good ventilation, the GFR is 20 ( < 30 ), Rx? |
Unfractionated heparin ( due to renal insufficiency) |
|
|
Patient on mechanical ventilation, FiO2 is 80%, PaO2 is 105, PaCo2 is 37 , next ?? |
Decrease fraction of inspiration oxygen below 60% (FiO2 < 60%) to prevent oxygen toxicity |
|
|
Asthma patient, progressive asthma symptoms, no dyspnea , her throat is sore and hoarseness that resolves during the day , next ? |
Add omeprazole ( comorbid GERD causing asthma exacerbation) |
|
|
36, 4 months of cough, white sputum, worsen at night, history of GERD, normal breath sound, split second heart sound with inspiration, next ? |
PFTs to check bronchodilator response ( asthma) |
|
|
The most effective way to differentiate asthma from COPD |
Spirometry before and after administration of bronchodilator |
|
|
Asthma vs COPD Rx |
Asthma: albuterol and inhaled corticosteroids COPD: albuterol and long- acting anticholinergic inhaler |
|
|
53, suddenly collapsed and lost consciousness for 3 minutes, left sided chest pain, no seizure, E: hypotension, tachycardia, oximetry 80%, tachypnea, jugular venous pressure 13, which other finding ?? |
Right heart dysfunction due to massive PE |
|
|
36, 4 months of cough, white sputum, worsen at night, history of GERD, normal breath sound, split second heart sound with inspiration, next ? |
PFTs to check bronchodilator response ( asthma) |
|
|
The most effective way to differentiate asthma from COPD |
Spirometry before and after administration of bronchodilator |
|
|
Asthma vs COPD Rx |
Asthma: albuterol and inhaled corticosteroids COPD: albuterol and long- acting anticholinergic inhaler |
|
|
53, suddenly collapsed and lost consciousness for 3 minutes, left sided chest pain, no seizure, E: hypotension, tachycardia, oximetry 80%, tachypnea, jugular venous pressure 13, which other finding ?? |
Right heart dysfunction due to massive PE |
|
|
72, passing while getting out of bed, no seizure, no chest pain, no SOB, history of watery diarrhea 2-3 days, BP is 120/70 while supine and 98/50 while standing, which laboratory value indicator of this condition |
Decreased urine sodium due to activating of aldosterone ( due to hypovolemia ) |
|
|
الحمد لله على الختام اللهم ذكرني ما قرأت في الامتحان |
و أرشدني إلى الاجابة الصحيحة يا رب اللهم إني توكلت عليك |

