![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
110 Cards in this Set
- Front
- Back
|
What is Criminal Commitment? |
a procedure in which a person may be confined in a mental institution for determination of fitness to stand trial or after a verdict of NCRMD |
|
|
What is Civil Commitment? |
a procedure in which a mentally ill and dangerous person, who may not have committed a crime, may be involuntarily incarcerated in a psychiatric hospital |
|
|
True or False: In Canada civil commitment is under federal legislation while criminal commitment is under provincial legislation |
False: civil commitment is provincial and criminal commitment is federal |
|
|
What is the defence "Not Criminally Responsible on account of Mental Disorder" (NCR)? |
a situation where an individual has committed an illegal offence, but due to the effects of a mental disorder are not held criminally responsible for their actions |
|
|
What are the two components any crime? |
1) mens rea (the guilty mind) 2) actus reus (the guilty action) |
|
|
What two criteria must be met for a person to be deemed NCR? |
1) have a mental disorder (aka "disease of the mind") 2) the mental disorder must be severe enough to prevent the person from knowing right from wrong at the time of the offence |
|
|
What is Neurolaw? |
a new field of inquiry which stems from the use of neuroscience data in a legal context |
|
|
What does "Fitness to Stand Trial" refer to? |
the mental state of the accused person at the time of the trial (i.e. whether they are capable of standing trial) |
|
|
What are the requirements for Fitness to Stand Trial? |
1) Do they understand the legal proceedings occurring? 2) Do they understand the likely consequences of the legal proceedings? 3) Are they capable of communicating with their lawyer? |
|
|
What assessment measure is used to supplement clinical judgment for Fitness to Stand Trial? |
the FIT-R |
|
|
What is the procedure when someone is determined to be unfit to stand trial? |
step 1) the person is criminally committed to a psychiatric hospital for treatment step 2) assessed every 4 months by a provincial review board for fitness to stand trial step 3) then put on trial when they are fit |
|
|
What are the criteria for a person to be civilly committed? |
1) have mental disorder 2) pose an immediate danger to self or others |
|
|
What are he two major categories of civil commitment procedures? |
1) Formal commitment - commitment ordered by a judge 2) Informal commitment - emergency commitment accomplished without initially involving the courts |
|
|
How is a formal civil commitment procedure undertaken? |
step 1: initiated by request from any responsible citizen (i.e. psychologist, family, etc.) step 2: if judge believes reason to purse, person held for 72 hrs for mental health assessment step 3: if person meets commitment criteria they may be committed for treatment |
|
|
What is Community Commitment? |
a form of commitment in which person is committed for involuntary treatment while still living in the community |
|
|
What are Community Treatment Orders (CTOs)? |
a legal tool that specifies the treatment that must be adhered to for the person to be released into the community |
|
|
What is the consequence of non-adherence to a CTO? |
person apprehended and examined involuntarily to determine if involuntary commitment is warranted or person is apprehended and involuntarily committed without reexamination |
|
|
True or False: It is easy to predict whether a person is dangerous |
False: It can be very difficult |
|
|
What is the Actuarial approach? |
an approach to the prediction of a person's dangerousness using statistical formulae composed of weighted known predictor variables |
|
|
What is the HCR-20 ? |
a structured form used to help with clinical judgment of dangerousness that assesses historical, clinical, and risk variables |
|
|
What are the 4 principles of the Canadian Code of Ethics for Psychologists? |
1) Respect for the dignity of persons 2) Responsible caring 3) Integrity of relationships 4) Responsibility to society |
|
|
What is required in most Canadian provinces when a person's right to refuse treatment is circumvented? |
a substitute decision-maker is asked to provide consent (i.e. family member) |
|
|
What institutional body is responsible for reviewing the safety and general ethical properties of behavioural research proposals? |
Institutional Review Boards (IRBs) |
|
|
What is informed Consent? |
an agreement of a person to serve as a research participant or to enter therapy, after being told the possible benefits and risks |
|
|
Why is Informed Consent obtained? |
to allow research participants and patients the ability to judge whether they want to accept any inherent risks |
|
|
Define Confidentiality |
an agreement between two persons that nothing will be revealed to third parties, except those intimately involved in treatment |
|
|
Define Privileged Communication |
the communication between two person which is held confidential |
|
|
What are the three exceptions to confidentiality? |
1) Imminent risk of harm to self or others 2) incidence of child abuse 3) incidence of elder abuse |
|
|
What are the three groups of older adults? |
1) young-old = age 65-74 2) old-old = age 75-84 3) oldest-old = age 85+ |
|
|
True or False: older adults are more different from one another than individuals at any other age group |
True |
|
|
Define Age Effects |
the consequences of being a given chronological age |
|
|
Define Cohort Effects |
the consequences of being born in a given year and having grown up during a particular time period |
|
|
Define Time-of-Measurement Effects |
confounds that arise because events at an exact point in time have a specific effect on a variable being studied over time |
|
|
Define Selective Mortality |
a possible confound for longitudinal studies in which less healthy individuals are more likely to drop out of the study over time |
|
|
What are the goals of developing assessments for elderly persons? |
1) develop short, but reliable and valid measures for the elderly 2) develop measures with items tailored directly to concerns and symptoms of elderly people |
|
|
Define Dementia |
an umbrella term for gradual deterioration of intellectual/cognitive abilities to the point that social and occupational functions are impaired |
|
|
What are the potential symptoms of dementia? |
1) difficulty remembering 2) leaving tasks unfinished 3) poor hygiene 4) getting lost 5) difficulty making plans/decisions 6) poor impulse control 7) deterioration of abstract ideas 8) Disturbances in emotion |
|
|
What are the three major classifications of Dementias? |
1) Alzheimer's Disease 2) Frontal-Temporal Dementias 3) Frontal-Subcortical Dementias |
|
|
What are the DSM-5 Diagnostic Criteria for Neurocognitive Disorders? (including the two specifiers) |
1) Evidence of cognitive decline 2) Cognitive deficits interfere with independence 3) Cognitive deficits not due to delirium specifiers: 1) cause of the decline 2) major or mild neurocognitive disorder |
|
|
What percentage of dementias in older people does Alzheimer's Disease account for? |
about 50% of cases |
|
|
What is the clinical presentation and course of Alzheimer's Disease? |
Insidious/gradual onset with slow progression over years Starts with inability to learn or encode new info Then problems with naming and spatial skills as well as poor insight, but retain social graces late stage see broad severe functional decline and behavioural problems death typically occurs 10-12 years after onset |
|
|
What are the Neurological Correlates of Alzheimer's Disease? |
1) Gross atrophy of cerebral cortex; first in the hippocampus and entorhinal cortex, then in the temporal and parietal lobes, and finally in the frontal lobes 2) plaques scattered throughout the cortex Plaques - small, round areas composing remnants of lost neurons and B-amyloid 3) Neurofibrillary tangles - tangled, abnormal protein filaments that accumulate within cell bodies of neurons |
|
|
What neurotransmitter is implicated in Alzheimer's Disease? |
reduced levels of Acetylcholine |
|
|
What is the role of genetics in Alzheimer's Disease? |
strong evidence for genetic component, especially in early onset Alzheimer's Disease APOE-E4 polymorphisms are risk factors genetic markers = APP, PSEN1 or PSEN 2 |
|
|
What is the role of environment in Alzheimer's Disease? |
cognitive activity preserves crystallized intelligence more than fluid intelligence cognitive reserve hypothesis - notion high education levels delay clinical expression of dementia because brain develops reserve neural structures as a form of neuroplasticity |
|
|
What are Frontal-Temporal Dementias? |
dementias that may be marked by extreme behavioural and personality changes or language declines |
|
|
What percentage of dementias in elderly people do Frontal-Temporal dementias account for? |
about 10-15% |
|
|
What is the typical age of onset for Frontal-Temporal Dementias? |
late 50s |
|
|
What is Pick's Disease? |
a degenerative disorder in which pick bodies (spherical inclusions) appear in the bodies neurons |
|
|
Explain the Behavioural Variant of Frontal-Temporal Dementias |
personality changes due to loss of serotonergic neurons in the frontal lobes |
|
|
Explain the Language Variant of Frontal-Temporal Dementias |
language declines due to loss of serotonergic neurons in the language system of the frontal and temporal lobes |
|
|
What is the clinical presentation of Frontal-Subcortical Dementias? |
1) poor attention and slow thinking 2) Motor problems 3) executive deficits (i.e. problem-solving, abstraction, etc.) 4) memory problems due to poor organization and retrieval problems |
|
|
What is Huntington's Chorea? |
a frontal-subcortical dementia caused by a single dominant gene located on chromosome 4 major behavioural feature = writhing movements |
|
|
What is Parkinson's Disease? |
a frontal-subcortical dementia caused by degeneration of the substantia nigra which results in low dopamine to the striatum and cortex marked by muscle tremors, muscle rigidity, and akanesia (inability to initiate movement) |
|
|
What is Vascular Dementia? |
a frontal-subcortical dementia diagnosed when patient with dementia has evidence of cerebrovascular disease presumed to cause the dementia |
|
|
What are the Alpha-Synucleinopathies? |
related disorders to dementia, all caused by abnormal alpha-synuclein deposition include Parkinson's Disease Dementia (PDD) and Lewy Body Dementia (LBD) |
|
|
What is Parkinson's Disease Dementia (PDD)? |
an alpha-synucleinopathy that presents as a frontal-temporal dementia with motor symptoms preceding gross cognitive decline and possibly visual hallucinations |
|
|
What is Lewy Body Dementia (LBD)? |
an alpha-synucleinopathy characterized by significant cognitive declines early on, such as major fluctuations in attention, visuo-spatial impairment, executive dysfunction, and visual hallucinations |
|
|
What are Biological Treatments for Alzheimer's Disease? |
1) Acetylcholinesterase inhibitors (i.e. donepezil/Aricept) 2) NMDA Agonists - block excessive glutamate which in Alzheimer's disease can be toxic (i.e. Memantine) 3) Antioxidants 4) experimental treatment to block amyloid 5) excluding reversible causes of dementia |
|
|
What is Delirium? |
a clouded state of consciousness characterized by trouble concentrating, inability to maintain coherent thoughts, perceptual disturbances, memory impairment, and paranoid delusions |
|
|
What is the difference between Delirium and other conditions? |
people with delirium have lucid intervals and are due to an underlying cause |
|
|
What is the treatment for delirium? |
treat the underlying cause if possible |
|
|
What are the two classifications of childhood disorders? |
1) externalizing disorders - outward-directed behaviours (aka undercontrolling disorders) 2) internalizing disorders - inward-focused experiences (aka overcontrolling disorders) |
|
|
What are the Neurodevelopmental Disorders in DSM-5? |
1) ADHD 2) Learning Disorders 3) Communication Disorders 4) Motor Disorders 5) Intellectual Disability 6) Autism Spectrum Disorder |
|
|
What are Learning Disorders (LDs)? |
disorders involving inadequate development in a specific area of academics (i.e. reading, writing, or math) *not due to intellectual disability, ASD, a physical disorder, or deficient educational opportunities |
|
|
What is Reading Disorder (dyslexia)? |
difficulty with word recognition and reading comprehension |
|
|
What is Mathematics Disorder (dyscalulia)? |
difficulty rapidly and accurately recalling math facts and counting objects |
|
|
What is Disorder of Written Expression? |
difficulty in production of the written word |
|
|
What is the Etiology of Learning Disorders? |
chromosome 13 implicated in dyslexia Generalist gene hypothesis - proposes the genes that affect one ability are the same genes that affect a different ability, even though there are also some genes that effect each specific ability left hemisphere abnormalities in dyslexia and disorder of written expression right hemisphere abnormalities in dyscalculia |
|
|
What is the Treatment for Learning Disorders? |
special education plans or programs in schools |
|
|
Identify and Define the four Communication Disorders |
1) Language disorder - difficulty with expressing one's self in speech 2) Phonological disorder - difficulty with certain speech sounds 3) Fluency disorder - disturbances in verbal fluency, including repeated sounds, long pauses between words, substituting easy words for difficult ones, and repeating whole words 4) Social (Pragmatic) Communication disorder - persistent difficulty in social use of verbal or nonverbal communication |
|
|
Identify and Define the two two Motor Disorders discussed in lecture? |
1) Developmental Coordination Disorder - marked impairment in the development of motor coordination 2) Tic Disorder - involves involuntary, repetitive movements and vocalizations |
|
|
What is the DSM-5 Criteria for Intellectual Disability? |
1) Intelligence-Test Score (IQ = 70 or below) 2) Adaptive Functioning (deficits in social, communication, and practical skills) 3) Age of Onset = before age 18 |
|
|
What are the severity levels of Intellectual Disability? |
1) mild (most common) 2) moderate 3) severe 4) profound |
|
|
What are the etiology of Intellectual Disability? |
1) No identifiable cause in majority of cases 2) Hereditary disorders (PKU) 3) Early Alterations in Embryonic Development (Down's Syndrome and Fetal Alcohol Syndrome) 4) Later pregnancy and perinatal problems (Fetal malnutrition and prematurity) 5) Childhood infection, trauma, and poisoning |
|
|
What is Phenylketonuria (PKU)? |
a genetic disorder that, through a deficiency in a liver enzyme, phenylaline hydroxylase, causes severe intellectual disability |
|
|
What is Down's Syndrome? |
a form of moderate to severe intellectual disability, caused by an extra chromosome, in which the individual has several distinctive physical traits |
|
|
What are the Treatments for Intellectual Disability? |
Systematic behavioural interventions based on operant conditioning at home and in school Self-Instructional Training - a CBT approach that tries to help improve overt behaviour by changing how a patient silently talks to themselves |
|
|
What is the phenotype presentation of Asperger's Syndrome? |
high IQ, normal language skills, but poor social skills |
|
|
What is the core deficit in Autism Spectrum Disorder (ASD)? |
social skills (theory of mind) deficits |
|
|
What are the Characteristics of Autism Spectrum Disorder (ASD), other than the core deficit? |
1) extreme autistic aloneness 2) Communication deficits (i.e. Echolalia, Pronoun Reversal, and Neologisms) 3) Obsessive-compulsive acts (i.e. upset easily by changes, and strong attachment to specific objects) 4) Ritualistic Acts (i.e. repetitive, rigid behaviour, and unusual motor movements) |
|
|
What is the Etiology of Autism Spectrum Disorder (ASD)? |
1) ASD perhaps the most heritable psychiatric disorders 2) epileptic seizures 3) Abnormal brain wave patterns 4) brain regions implicated: - cerebellum - amygdala and corpus callosum - Medial frontal cortex and media temporal cortex |
|
|
What are the Treatments for Autism Spectrum Disorder (ASD)? |
1) Early Intensive Behavioural Intervention (EIBI): involves delivery of early (before age 5) and intensive (20 hrs per week for 2 years) modelling and operant conditioning treatment 2) Antipsychotics to reduce aggressive and self-mutilation behaviour 3) Antidepressants to reduce stereotypic and repetitive behaviours 4) Stimulants to reduce inattentiveness and hyperactivity |
|
|
What are the Characteristic Symptoms of ADHD? |
1) Attention Deficits: - difficulty concentrating - difficulty sustaining attention - Trouble following through with instructions - Forgetful in daily activities 2) Hyperactivity-Impulsivity Symptoms: - constantly in motion - can't sit still - Unable to stop moving or talking - activities and movements seem haphazard 3) Difficulty with peer-relations |
|
|
What are the specifier types for ADHD? |
1) inattentive type 2) hyperactive-impulsive type 3) combination type |
|
|
In how many settings must symptoms be for an ADHD diagnosis? |
At least 3 settings |
|
|
What is the Etiology of ADHD? |
1) Inhibitory control deficits may be inherited predisposition 2) Frontal-Striatal circuitry dysfunction 3) decreased cerebellum and cerebrum volumes 4) delays in cortical maturation 5) dysfunction of dominergic and noradrenergic systems |
|
|
What type of drugs are given for ADHD? |
Stimulants (i.e. Ritalin/Methyphenidate) |
|
|
What are the psychological treatments for ADHD? |
1) Parent training 2) Classroom management (i.e. take advantage of operant-conditioning principles) |
|
|
What are the three themes of the DSM-5 Oppositional Defiant Disorder (ODD) diagnosis? |
1) Disobedient, hostile, and deviant behaviour 2) Angry, irritable mood 3) Vindictiveness |
|
|
What is the main difference between ODD and CD? |
children with ODD defy adult requests, but DO NOT violate the basic rights of others |
|
|
What is the clinical presentation of Conduct Disorder (CD)? |
Repetitive patterns of behaviour that include: 1) Aggressiveness to other people and animals (i.e. bullying, cruelty) 2) Destruction of property 3) Deceitfulness or theft 4) Serious violations of the rights of others |
|
|
What other disorder is conduct disorder a DSM-5 criteria for? |
Antisocial Personality Disorder (ASPD) |
|
|
What are the two specifiers for Conduct Disorder diagnosis? |
1) age of onset - childhood-onset type - adolescent-onset type 2) callous-unemotional subtype |
|
|
What two features of a Conduct Disorder diagnosis are associated with later development and ASPD, and more severe problems? |
1) childhood-onset type 2) callous-unemotional subtype |
|
|
What Biological Factors contribute to CD? |
1) aggressive behaviour may be inherited, but not delinquent behaviour 2) Neuropsychological deficits = poor verbal skills, difficulty with executive functioning, and memory problems 3) Neurological correlates: - amygdala and anterior cingulate cortex underactivity to negative stimuli - reduced HPA-Axis response (i.e. low cortisol) - amygdala-prefrontal cortex dysfunction associated with poor fear conditioning |
|
|
What Psychological Factors contribute to CD? |
1) hostile-ineffective parenting 2) Inconsistent parental discipline and parental adjustment difficulties 3) Cognitive bias to perceive neutral peer behaviour as hostile/aggressive 4) Chaotic social environment |
|
|
Explain the Biopsychosocial Model of Conduct Disorder |
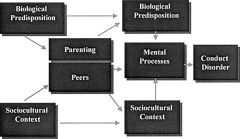
|
|
|
What is the Course of Conduct Disorder? |
Treatment is often ineffective, except when delivered in young children |
|
|
What are the treatments for Conduct Disorder? |
Parental Management Training - teaching parents to modify their responses to their children so prosocial, rather than antisocial, behaviour is consistently rewarded Multi-Systematic treatment (MST) - intensive and comprehensive therapy in the community by targeting all areas of the child's life Anger Management Training - teaching clients self-control strategies during anger-provoking situations |
|
|
What is Disruptive Mood Dysregulation Disorder (DMDD)? |
a mood disorder characterized by persistent irritability and episodes of temper outbursts, three or more times per week |
|
|
What is Substance Dependence? |
the abuse of a drug, sometimes accompanied by physiological dependence, and made evident by tolerance and withdrawal symptoms |
|
|
What is tolerance? |
a physiological process in which larger and larger doses of the drug are need to achieve the same desired effect |
|
|
What are Withdrawal symptoms? |
negative physiological and/or psychological effects when a person stops taking an addictive drug |
|
|
What is Substance abuse? |
the recurrent use of drug to such an extent that they experience one or more of the following: 1) failure to fulfill major obligations 2) exposure to physical danger 3) legal problems 4) persistent social or interpersonal problems |
|
|
What is polydrug use? |
use or abuse of multiple drugs at the same time |
|
|
What is Alcohol Dependence? |
a disorder characterized by abuse or dependence on alcohol, accompanied by tolerance and withdrawal symptoms, and delirium tremens (DTs) |
|
|
What is Delirium Tremens (DTs)? |
an acute form of delirium caused by withdrawal from an addictive substance (i.e. Alcohol), which involves high autonomic activity (i.e. shaking, sweating, high HR, fever, etc.) |
|
|
True or False: Women have higher rates of high risk drinking |
False: men have higher rates of high risk drinking |
|
|
What are the Short-term Effects of Alcohol? |
1) Biphasic Effects: - initially acts as stimulant - later acts as depressant 2) Effects on neurotransmitters - stimulates GABA system - increases dopamine and serotonin - inhibits glutamate receptors |

