![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
63 Cards in this Set
- Front
- Back
|
differ stress from strain
|
stress; ratio of applied force to cross sectional area
strain: change in length of a material when stress is applied |
|
|
what are two major regions of a stress-strain curve
|
elastic region - initial straight portion of the curve (the material hasnt changed shape yet)
plastic region - non linear portion of the cirve (deformation of the material occurs) |
|
|
what are 3 major points on a stress-strain curbe
|
yield point; point where linear portion ends and non linear portion begins (deformation begins)
ultimate tensile strength: max stress that material can withstand on a curve failure strength: point where fracture occurs (aka fracture strength) |
|
|
what is the modulus of elasticity of a material
|
-the stiffness of a material
|
|
|
what is fatigue failure
|
delayed failure from fluctuating or cyclic stresses
|
|
|
what type of sensitivity is observed with metal implants
|
Type 4
-delayed response, cell mediated -osteolysis and dermatitis |
|
|
what is the most common metal allergy and in what alloy can it be found
|
-nickel is most common
- SS contains 15% nickel |
|
|
what is stress shielding
|
-phenomenon by which bone mass is decreased over period of time bc a rigid device takes the load and not the bone
|
|
|
how can stress shielding be reduced in fracture fixation
|
-use less rigid or flexible fixation devices
-use metal plates that are thinner -use metals that have a modulus of elasticity (stiffness) closer to that of bone |
|
|
what is osteointegration
|
process by which bone attaches to a material or device
|
|
|
which type of bone are staples meant for
|
cancellous; cortical is too hard to get staples through?
|
|
|
for an oblique fracture, should the screw fixation be perpendicular to bone or fracture line
|
-to the bone to rpevent sliding of the fragments on each other during axial load
|
|
|
what is a herbert bone screw
|
no head
pitch is different on either end of the screw |
|
|
the primary advantage of cortical bone is stability; what is the advantage of cancellous
|
facilitates osteogenesis
|
|
|
list an xenograft
|
coralline hydroxyapatite
|
|
|
how long after skin grafitng will the area "pink up" and what is this process called
|
- 48 hours later
-inosculation: graft is getting its new blood supply |
|
|
what is the best suturing technique for areas of high tension
|
mattress
|
|
|
how do you relieve tension from the bases of a flap after performing an advancement flap
|
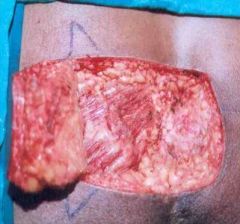
cut Burow's triangles in tissue adjacent to the pivot point
|
|
|
Bone morphogenic proteins (BMP) are growth factors needed for bone growth; who discovered them
|
Urist in 1965
|
|
|
what is lyophilization
|
-process by which freeze dried bone reduces its antigenicity (used in allograft)
|
|
|
name the non toxic dye used to asess the viability of skin flaps
|
fluorescein
|
|
|
what is the MC failure of skin flaps
|
vascular embarrassment
|
|
|
increase in length for a 60 degree Z plasty
|
75%
|
|
|
what is the minimum angle of a Z plasty
|
35 degrees, any less then 45 though will impair blood flow to the flap
|
|
|
what is a Gillies stitch
|
-suture utilized at teh apical portions of incisions that does not penetrate the epidermis of teh apex, thus dec vascular damage
|
|
|
what is the process by which skin grafts must heal when placed over an avascular area
|
bridging; must get vascular supply from surrounding tissue
|
|
|
how are the RSTL oriented on the plantar foot
|
transversely
|
|
|
give the thickness of thin, intermediate and thick STSG
|
thin 0.008-0.012 inch
intermediate 0.012-0.016 thick 0.016-0.020 |
|
|
how many cortices for syndesmotic screw
|
3
|
|
|
fixation for SH 4 fracture of distal tibia
|
smooth k wire
|
|
|
which method of fixation works best in Open wedge osteotomies
|
staples because they maintain the size of osteotomy when graft is being resorbed
|
|
|
cutting cone
|
-is an osteon (composed of osteoclasts being chased by osteoblasts across the fx line)
-also resorption canal invaded by vascular buds |
|
|
what is the first step in proper lag technique
|
reduce the fracture with a bone clamp
|
|
|
T or F: two crossed K wires provides compression
|
False
K wires provide splintage not compression |
|
|
how many threads of a screw should extend beyond the far cortex
|
2
|
|
|
when can a screw be used alone for internal fixation of a fracture
|
when the fx is at least twice as long as the diam of the bone
|
|
|
best type of fixation for pseudoarthrosis following debridement and graft placement
|
neutralization plate
|
|
|
how long for NWB of base osteo of 1st met
|
6-8 weeks
|
|
|
what is the cx of not overdrilling the proximal fragment
|
distraction rather then compression
|
|
|
when fixating a fracture, is the "load screw" perpendicular to the bone or fracture
|
bone
|
|
|
describe load screw technique (offset drilling)
|
use the holes closet to teh fracture sight first, the first two screws are considered the "load screws"
|
|
|
what are the 4 basic techniques of internal fixation
|
-splinting
-neutralization -buttressing -interfrag compression |
|
|
what is a transfixation screw
|
-syndesmotic screw
|
|
|
if pt has a nickel allergy, how would you fixate their CBWO
|
bio absorbable screw
|
|
|
5 weeks out; sclerosis it noted at an osteotomy site
|
-beginning of non union
|
|
|
which type of screw allows for percutaneous placement across the fracture sight
|
cannulated
|
|
|
what is Pauwels principle
|
long bone eccentrically loaded is subjected to tension forces on teh convex side and compression on the concave side
|
|
|
which effect is produced when using two different types of metals in close proximity to each other in the body
|
galvanic corrosion
|
|
|
what is the purpose of the posterior 1/3 semi tube plate in a distal oblique fib fracture
|
anti glide plate that prevents proximal migration of distal fracture fragment
|
|
|
T or F; threads of a lag screw should cross the fx line
|
False
|
|
|
K wire sizes
|
0.035 inch
0.045 0.054 0.062 |
|
|
steinman pin sizes
|
5/64-12/64 except 11/64
|
|
|
T or F; do lag screws provide dynamic interfrag compression
|
no they provide static interfrag compression
|
|
|
how is dynamic interfrac compression achieved; given an example in the foot
|
-acheived with tension band fixation
-styloid fractures can be fixated with tension band -tension band harnesses forces generated at the level of the fracture when the bone comes under load |
|
|
review screw sets and over under drill sizes
|
.
|
|
|
what is the primary function of a neutralization plate
|
to protect interfrag compression lag screws deom bending, shearing, and torsional forces
|
|
|
what is the primary purpose of a buttress plate
|
to prevent axial deformity fron bending, shearing and torsion forces
|
|
|
when appying bone screws should the depth gauge be used prior to tapping or after
|
after. once the threads are tapped, teh depth gauge could disrupt the threads
|
|
|
increased oxygen tension favors bone healing. what does a decreased oxygen tension promote
|
cartilage formation instead of bone formation
|
|
|
large (>6 cm) osseous defects are best treated by what special type of bone graft
|
vascularized bone transfer
|
|
|
how much of their inital strength will cortical grafts lose to osteoclastic activity
|
30-40%
|
|
|
what is the rate that cutting cones advance during bone healing
|
50-80 micrometers/day
|
|
|
how long does revascularization of a cortical and cancellous bone graft take, respectively
|
cancellous - with in hours
cortical - after 6th day |

