![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
22 Cards in this Set
- Front
- Back
|
What are the specific advantages of intravenous drug administration?
|
> Entire dose reaches systemic circulation immediately
> Permits accurate titration |
|
|
What are the specific disadvantages of intravenous drug administration?
|
> Risk of infection
> Increased risk of adverse effects > Site: requires IV access - overweight patients problematic > Injections hurt, can cause bruises and frighten children and needle phobics |
|
|
What is the general advantage of parenteral drug administration over oral administration?
|
Parenteral bypasses first-pass metabolism of the hepatic circulation
|
|
|
What are the general disadvantages of parenteral administration over oral administration?
|
> Risk of infection
> Injections can cause bruises and pain > Frightens children and needle phobics |
|
|
What are the specific advantages of intramuscular drug administration?
|
> Good absorption and rapid onset (compared to enteral)
> Straightforward administration |
|
|
What are the specific disadvantages of intramuscular drug administration?
|
> Delayed absorption in shock (blood diverted to organs)
> Site: only certain muscles (deltoid or gluteal) |
|
|
What are the specific advantages of subcutaneous drug administration?
|
> Constant & slow absorption → prolonged effect
> Onset more rapid compared to oral |
|
|
What are the specific disadvantages of subcutaneous drug administration?
|
> Delayed absorption in shock (blood diverted to organs)
> Absorption dependant on blood flow |
|
|
What are the advantages of enteral drug administration?
|
> Safe - reduced risk of adverse effects and infection
> Easy administration - preferred by patients > Cheapest > Prolonged action |
|
|
What are the disadvantages of enteral drug administration?
|
> Cannot bypass first-pass metabolism
> Unpredictable absorption due to degradation by stomach acid and enzymes or contents of stomach > Uncooperative patients may not take them |
|
|
Define bioavailability (F) and the factors that affect it.
|
Fraction of the administered dose of drug that reaches the systemic circulation (F=1 for IV drugs)
Affected by: First-pass metabolism Absorption - GI tract disease/abnormality may affect this |
|
|
Define volume of distribution. |
Apparent volume into which a known amount of drug must be dispersed to give the measured plasma concentration If you give a dose of a known amount and subsequently measure the drug serum conc., how much the drug has been diluted (how much of the drug is in the blood vs extravascular compartment)? |
|
|
Define clearance. |
Theoretical volume of plasma "cleared" of drug per unit time (e.g. mlmin⁻¹) |
|
|
Define half-life. |
The time required for the serum concentration to reduce by half
|
|
|
Define steady state and how long it takes to reach. |
Drug conc. is in dynamic equilibrium: the amount of drug administered is equal to the amount of drug eliminated within one dosing interval (when giving repeated doses)
|
|
|
What is maintenance dosing?
|
The maintenance rate of drug administration equal to the rate of elimination in the steady state
|
|
|
Define pharmacokinetics. |
The science of the rate of movement of drugs within biological systems, as affected by the metabolism, absorption, distribution and elimination of medications
“What your body does to the drug" |
|
|
Define pharmacodynamics. |
Study of the biochemical and physiologic processes underlying drug action > Mechanism of drug action > Efficacy > Drug-receptor interaction > Safety profile
“What the drug does to your body" |
|
|
How can you reach steady state quicker than 4-5 half-lives? |
Give a (large) loading dose - if therapeutic effect is needed more quickly than it takes to reach steady state i.e. for drugs with long half-lifes |
|
|
Describe the difference between the loading dose and maintenance dose in terms of what they are dependent on. |
Loading dose depends only on the desired drug conc. and the volume of distribution Maintenance dose depends on drug clearance |
|
|
Define linear pharmacokinetics. |
Concentration that results from a dose is proportional to the dose
Double the dose, double the concentration
Rate of elimination is proportional to the concentration 50% of a drug will be cleared in one half-life
90% of drugs have linear pharmacokinetics |
|
|
Define non-linear pharmacokinetics. |
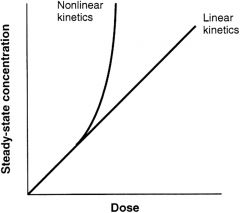
Concentration that results is not proportional to dose
Rate of elimination is constant regardless of amount of drug present Clinical relevance: side effects are dependent on drug conc. → have to give much smaller doses and monitor for drugs that exhibit NLPKs |

