![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
66 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
What is the eye?
|
An eye is an organ that detects light. Different kinds of light-sensitive organs are found in a variety of creatures. The simplest eyes do nothing but detect whether the surroundings are light or dark. More complex eyes are used to provide the sense of vision.
|
|
|
|
How does the eye work?
|
The eye works by allowing light to enter it and project onto a light-sensitive panel of cells known as the retina at the rear of the eye, where the light is detected and converted into electrical signals, which are then transmitted to the brain via the optic nerve. Such eyes are typically roughly spherical, filled with a transparent gel-like substance called the vitreous humour, with a focusing lens and often an iris which regulates the intensity of the light that enters the eye.
|
|
|
|
Describe the stimulus for the visual system as in the energy that gets captured?
|
The Stimulus is Electromagnetic radiation
NOTES: Light can be though of either as composed of electromagnetic waves or as a collection particles (photons), and it behaves as either depending on the circumstances, but really is a bit of both. In this case, the wave nature of light is the most important. The small wavelength energy is high energy like gamma rays that comes from out of space and they will pass right through your body and you would not even know it but slightly lower energy like x rays also pass through your body but not through the ossified bone as well. Ultraviolet rays, you cannot see this but you get sun burn because of it. Visible light is the range of electromagnetic energy that we see with the eye and we experience this as a series of light. There is nothing about the eye that has pigment packages to it, like green or blue, so electromagnetic energy does not have color to it, it is perception of the brain, that brings it out. If your eye can see lower energy it will be glowing with radial stations through the rim. At the beach, you cannot see the infrared rays but you feel it = feels warm. The lower wavelengths are the broadcast waves. |
|
|
|
1. Between what wavelength is visible light?
2. Why are we only sensitive to visible light and not radial stations blasting through? |
1. visible wavelength: 400 - 700 nanometer
2.We are sensitive only to visible light instead of radio stations because the eye has receptors that are only specifically turned only to capture this energy and see only visible light in a specific bandwidth |
|
|
|
How do the different types of vision develop?
|
At some point, color vision develops when receptor cells develop multiple pigments. As a chemical instead of mechanical adaptation, this may happen at any of the points described above, or not at all, and the capability may disappear and reappear, as organisms become predator or prey. Similarly, night and day vision emerge when receptors differentiate into rods and cones, respectively.
|
|
|
|
Describe the eye?
|
The eye is like a camera. The eyes of cephalopods, fish, amphibians, and snakes usually have fixed lens shapes, and focusing vision is achieved by telescoping the lens (similar to how a camera focuses).
|
|
|
|
What are the 9 structures found in the eye?
|
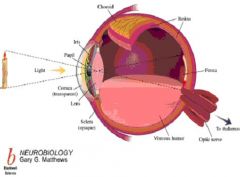
1. Cornea
2. Lens 3. Iris 4. Vitreus humor 5. Retina 6. Choroid 7. Sclera 8. Conjunctiva 9. Optic nerve head |
CLIVe ReCS COp
|
|
|
Describe the Cornea?
|
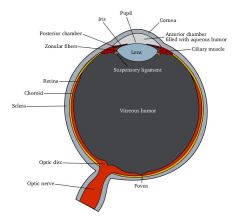
(1)70-80% of refraction
(2)Clincal involvement: ammetropia, astigmatism NOTE: The cornea is the transparent front part of the eye that covers the iris, pupil, and anterior chamber and provides most of an eye's optical power [1]. Together with the lens, the cornea refracts light and consequently helps the eye to focus. The cornea gives a larger contribution to the total refraction than the lens, but whereas the curvature of the lens can be adjusted to "tune" the focus, the curvature of the cornea is fixed. |
|
|
|
What is ammetropia and astigmatism?
|
When the light entering the eye is not correctly focused on the retina, the eye is said to have an ammetropia. When ammetropia exists the image on the retina is not sharp, and the person will perceive blur.
There are four common ammetropias: 1. Nearsightedness (Myopia): This is the most common ammetropia. When someone is nearsighted, the image of distant objects is formed in front of the retina. People who are nearsighted have difficulty seeing objects in the distance without correction (glasses or contact lenses). They can usually see objects that are close without the need of correction. The more myopia a person has, the thicker the lenses they need to see distant things in focus. Higher amounts of myopia also require more lasering of the cornea in laser refractive surgery. 2. Farsightedness (Hyperopia): The focal length of the eye is too long. While hyperopic people generally have more difficulty seeing objects up close, hyperopia may produce a varied range of symptoms. This is because the focusing system of the eye (accomodation) can compensate for hyperopia, flexing the crystalline lens, and bring the image back into focus. For this reason, farsighted people have very good vision in youth and will usually not wear corrective lenses. With age we gradually lose the ability to flex the lens (accommodate), so farsighted people generally experience blur and eyestrain later in life than nearsighted people do. The age at which farsighted people have symptoms will depend on how much hyperopia they have. 3. Astigmatism: Typically, astigmatism simply means that the eye is slightly out-of-round. The result is that the eye has no distinct focal point, but rather a focal range through different parts of the eye. The symptoms of astigmatism can vary greatly, and it can co-exist with the other ammetropias. 4. Presbyopia: This is the gradual loss of accommodation, or the ability of the eye to adjust to different focal lengths and amount of light. It occurs when the crystalline lens starts to stiffen, a process that begins in our early twenties. Because we have plenty of excess lens elasticity, we usually don’t experience symptoms until we reach our forties. The stiffening of the lens is what causes farsighted (hyperopic) people to experience blur and eyestrain, usually before their forties. |
|
|
|
Describe the lens?
|
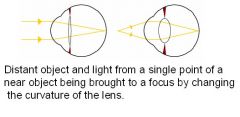
(1) Variable focus (accommodation) by smooth muscle (ciliary body, sphincter action on lens by zonule fibers to change lens radius of curvature)
(2) Parasympathetic innervation (Edinger-Westfal nucleus, ciliary ganglion) (3) Clinical involvement: cataracts, presbyopia NOTES: The lens or crystalline lens is a transparent, biconvex structure in the eye that, along with the cornea, helps to refract light to focus on the retina. The lens is flexible and its curvature is controlled by ciliary muscles. By changing the curvature of the lens, one can focus the eye on objects at different distances from it. This process is called accommodation. -Accommodation is the process by which the eye increases optical power to maintain a clear image (focus). |
|
|
|
What is Edinger-Westphal nucleus?
|
The Edinger-Westphal nucleus is the accessory parasympathetic nucleus of the oculomotor nerve (cranial nerve III), supplying the constricting muscles of the iris. Anatomically, the paired nuclei are posterior to the main motor nucleus and anterolateral to the cerebral aqueduct in the rostral midbrain at the level of the superior colliculus. It is the most rostral of the parasympathetic nuclei in the brain stem.
Functionally, it supplies preganglionic parasympathetic fibers to the eye, constricting the pupil, and accommodating the lens. |
|
|
|
Describe the ciliary ganglion?
|
The ciliary ganglion is small parasympathetic ganglion lying in the orbit between the optic nerve and the lateral rectus muscle that is associated with the nasociliary nerve (a branch of the ophthalmic division of the trigeminal nerve). The ciliary ganglion is a part of the nervous pathway responsible for the constriction and dilation of the pupil as well as sensation from the cornea.
It receives presynaptic fibers from the Edinger-Westphal nucleus by way of the oculomotor nerve (CN III) and in turn gives rise to postsynaptic fibers that innervate the ciliary muscle and the iris sphincter muscle. It reveives three roots: (1) sensory fibres that come directly from the nasociliary nerve, and do not synapse in the ganglion; (2) sympathetic fibres that come from the the plexus associated with the internal carotid artery and the ophthalmic artery and do not synapse in the ganglion; (3) presynaptic parasympathetic fibres from the inferior division of the oculomotor nerve (CNIII, Edinger-Westphal nucleus). The parasympathetic fibres synapse within the ganglion. The postganglionic fibres travel via the short ciliary nerve. These include: (1) general sensory to the eye; (2) sympathetic fibres to the dilator pupillae; (3) parasympathetic fibres to the sphincter pupillae and ciliary muscles of the eye. |
|
|
|
What are cataracts?
|

A cataract is any opacity which develops in the crystalline lens of the eye or in its envelope.
NOTES: Cataracts form for a variety of reasons, including long term ultraviolet exposure, secondary effects of diseases such as diabetes, or simply due to advanced age; they are usually a result of denaturation of lens proteins. Genetic factors are often a cause of congenital cataracts and may also play a role in predisposing someone to cataracts. Some cataract formation is to be expected in any person over the age of 70. Fully half of all people between the ages of 65 and 74 and about 70% of those over 75 have some cataract formation. Cataracts may also be produced by eye injury or physical trauma. A study among Icelandair pilots showed commercial airline pilots as three times as likely to develop cataracts as people with non-flying jobs. This is thought to be caused by radiation coming from outer space. Cataracts may be partial or complete, stationary or progressive, hard or soft. |
|
|
|
Describe the iris?
|
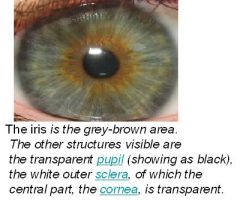
(1)Eye color
(2)Camera diaphragm; Pupil = aperture (f-stop) (3)Smooth muscle (radial & circumference) by sympathetic (superior cervical ganglion) and parasympathetic innervation (EW nucleus-ciliary ganglion ) (4)Clinical involvement: pupillary light reflex tests midbrain path through pretectum (brain swelling compromises midbrain early due to entrapment by bone) NOTES: In anatomy, the iris (plural irises or irides) is the most visible part of the eye of vertebrates, including humans. The iris is an annulus (or flattened ring) consisting of pigmented fibrovascular tissue known as a stroma. The stroma connects a sphincter muscle, which contracts the pupil, and a set of dialator muscles which open it. The back surface is covered by a two-cell thick epithelial layer, the iris pigment epithelium, but the front surface has no epithelium. The outer edge of the iris, known as the root, is attached to the sclera and the anterior ciliary body. The iris and ciliary body together are known as the anterior uvea. Just in front of the root of the iris is the region through which the aqueous humour constantly drains out of the eye, with the result that diseases of the iris often have important effects on intraocular pressure, and indirectly on vision. |
|
|
|
Describe the pupil?
|
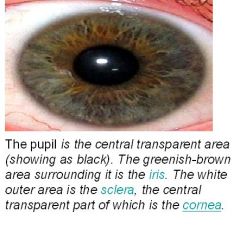
In the eye, the pupil is the opening in the middle of the iris. It appears black because most of the light entering it is absorbed by the tissues inside the eye. In humans and many animals (but few fish), the size of the pupil is controlled by involuntary contraction and dilation of the iris, in order to regulate the intensity of light entering the eye. This is known as the pupillary reflex. In bright light, the human pupil has a diameter of about 1.5 millimeter, in dim light the diameter is enlarged to about 8 millimeter. In strong light, the pupil constricts and is small, but still allows light to be cast over a large part of the retina. When an eye is photographed with a flash, the iris cannot close the pupil fast enough and the blood-rich retina is illuminated, resulting in the red-eye effect.
|
|
|
|
Why does dilation of pupils occur?
|
Dilation occurs when signals from sympathetic fibers (these fibres travel from the sympathetic trunk up to the face) cause the iris dilator muscles to contract. Damage to the sympathetic tract to the face (cranial nerve VII) results in Horner's syndrome, a symptom of which is excessive pupillary constriction (miosis) in one eye. This disparity in pupil size is termed anisocoria.
The human pupil dilates if the person sees something (or someone) of interest or is aroused. Studies have shown that humans (especially females) are judged as more attractive if their pupils are wide open and more dilated than normal. The name Belladonna (beautiful lady) comes from the fabled use of the juices of the Nightshade plant by Italian women who would use eyedrops made from an extract of the plant in their eyes in order to enlarge their pupils and make their eyes appear more beautiful. In some cases gradual blindness has occurred through the overuse and abuse of belladonna to enhance the beauty of the eyes. Atropine, a chemical found in belladonna, is used by modern eye doctors to dilate the pupils so that they can examine the retina. Excessive dilation is called mydriasis. Hallucinogenic drugs, such as LSD and psilocybin, and some stimulants such as cocaine also cause dilation of the pupils. |
|
|
|
Why does constriction of pupils occur especially related to pupillary light reflex?
|
When bright light is shone on the eye, it will automatically constrict. This is the pupillary reflex, which protects the retina from bright light, and is an important test of brainstem function. Also, the pupil will constrict if a person sees a thing or person which arouses anger or loathing.
The oculomotor nerve, specifically the parasympathetic part coming from the Edinger-Westphal nucleus, terminates on the circular iris sphincter muscle. When this muscle contracts, it reduces the size of the pupil. Certain drugs cause constriction of the pupils, such as heroin. Another term for the constriction of the pupil is miosis. Substances that cause miosis are called miotic. |
|
|
|
Describe the role of the Vitreous humour?
|
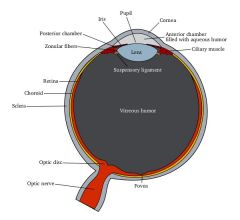
(1) viscous gel; intra-ocular pressure pushes against the sclera to keep eye spherical
(2) Clinical involvement: “floaters” NOTES: Vitreous humour is the clear aqueous solution that fills the space between the lens and the retina of the vertebrate eyeball. The solution is 99% water, but has a gelatinous viscosity two to four times that of water. The primary purpose of the vitreous humour is to provide a cushioned support for the rest of the eye, as well as a clear unobstructed path for light to travel to the retina. The collagen fibres of the vitreous are held apart by electrical charges. With aging, these charges tend to reduce, and the fibres may clump together. Similarly, the gel may liquify, a condition known as syneresis, leading to cells and other organic clusters to float freely within the vitreous. These commonly lead to floaters, or muscae volitantes (flying flies), which are perceived in the visual field as spots or fiberous strands. Floaters are generally harmless, but the sudden onset of reoccuring floaters may signify a posterior vitreous detachment (PVD) or other diseases of the eye. |
|
|
|
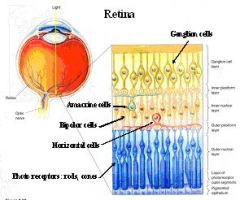
Describe the retina?
|
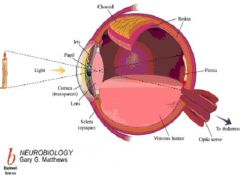
(1) Receptor sheet (photoreceptors)
(2) Fovea (a) High acuity central vision (~5 deg visual angle) (b) All cone photoreceptors and “pealed back” retinal layers (3) Pigmented epithelium (a) black, prevents internal reflections (4) Clinical involvement: retinal detachment, diabetic retinopathy, retinitis pigmentosa NOTES: The retina is a thin layer of cells at the back of the eyeball that converts light into nervous signals. The retina contains photoreceptor cells (rods and cones) which receive the light; the resulting neural signals then undergo complex processing by other neurons of the retina, and are transformed into action potentials in retinal ganglion cells whose axons form the optic nerve. The retina not only detects light, it also plays a significant part in visual perception. In embryonal development, the retina and the optic nerve originate as outgrowths of the brain. The unique structure of the blood vessels in the retina have been used for biometric identification. |
|
|
|
What are the 10 layers of the retina?
|
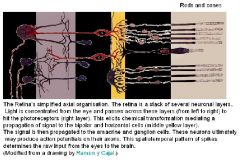
1. Retinal pigment epithelium (RPE)
2. Photoreceptor layer 3. External limiting membrane - Layer that separates the inner segment portions of the photoreceptors from their cell nuclei. 4. Outer nuclear layer 5. Outer plexiform layer - In the macular region, this is known as the Fiber layer of Henle. 6. Inner nuclear layer 7. Inner plexiform layer 8. Ganglion cell layer - Layer that contains nuclei of ganglion cells and gives rise to optic nerve fibers. 9. Nerve fiber layer 10. Inner limiting membrane |
|
|
|
What is fovea?
|
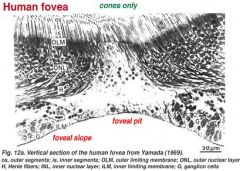
The fovea, a part of the eye, is a spot located in the center of the macula. The fovea is responsible for sharp central vision, which is necessary in humans for reading, watching television or movies, driving, and any activity where visual detail is of primary importance.
At the center of the fovea there is a pit with a diameter of about 0.2 mm. It has a high concentration of cone cells and virtually no rods. Compared to the rest of the retina, the cones in the foveal pit are smaller and more densely packed (in a hexagonal pattern), and they are not obscured by a layer of nerve cells or blood vessels; all of this together accounts for the sharp vision associated with them. The fovea is largely responsible for the color vision in humans which is superior to most other mammals. The foveal pit is not located exactly on the optical axis; it is displaced about 4 to 8 degrees temporal to the optical axis. Surrounding the foveal pit is the foveal rim, where the neurons displaced from the pit are located. This is the thickest part of the retina. Since the fovea does not have rods, it is not sensitive to dim lights. Astronomers know this: in order to observe a dim star, they use peripheral vision, looking out of "the side of their eyes". The fovea is covered in a yellow pigment called xanthophyll. This absorbs blue light and is probably an evolutionary adaption to the problem of chromatic aberration. |
|
|
|
What is the role of Retina Pigment Epithelium (RPE)?
|
The pigmented layer under the retina which performs many functions required for the retina to work properly. The following are some known functions:
* Supplies blood for the outer two thirds of the retina. * Resynthesizes photosensitive pigments. * Trims the outer segments of the rods and cones. * Keeps the retina attached via a sucking force. |
|
|
|
Describe retinal detachment?
|
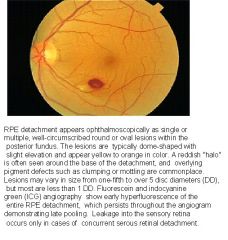
Retinal detachment is a disorder of the eye in which the retina peels away from its underlying layer of support tissue. Without rapid treatment, it can lead to vision loss and blindness.
The retina is a thin disc-shaped layer of light-sensitive tissue on the back wall of the eye. Its job is to translate what we see into neural impulses and send them to the brain via the optic nerve. Occasionally, injury or trauma to the eye or head may cause a small tear in the retina, which allows fluid to seep through, and peel it away like a bubble in wallpaper. |
|
|
|
Describe Retinitis pigmentosa, or RP?
|

Retinitis pigmentosa, or RP, is a genetic eye condition. Generally, night blindness precedes tunnel vision by years or even decades. Many people with RP do not become legally blind until their 40s or 50s and retain some sight all their life. Others go completely blind from RP, in some cases as early as childhood. Progression of RP is different in each case.
RP is a group of inherited disorders in which abnormalities of the photoreceptors (rods and cones) or the retinal pigment epithelium (RPE) of the retina lead to progressive visual loss. Affected individuals first experience defective dark adaptation or nyctalopia (night blindness), followed by constriction of the peripheral visual field and, eventually, loss of central vision late in the course of the disease. |
|
|
|
Describe diabetic retinopathy?
|

Diabetic retinopathy is retinopathy (damage to the retina) caused by complications of diabetes mellitus, which could eventually lead to blindness. It is an ocular manifestation of systemic disease which affects up to 80% of all diabetics who have had diabetes for 15 years or more.
|
|
|
|
Describe the choroid layer of the eye?
|
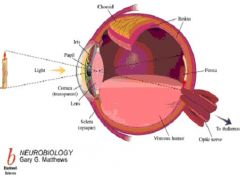
(1) Vascular layer
(2) Elaborates fluid and nutrients into posterior segment NOTES: The choroid, also known as the choroidea or choroid coat, is the vascular layer of the eye lying between the retina and the sclera. The choroid provides oxygen and nourishment to the outer layers of the retina [1]. Along with the ciliary body and iris, the choroid forms the uveal tract. In humans and other primates, darkly colored melanin pigment in the choroid helps limit reflections within the eye that would potentially result in the perception of confusing images. Poor vision frequently results from lack of this pigmentation in human albinos. By contrast, the choroid of many other animals contains reflective materials that help to collect light in dim situations; this is one type of tapetum lucidum. The red eye effort on photos are caused by the reflection of light from choroid. It appears red because of the choroid's blood vessels. |
|
|
|
Describe the sclera of the eye?
|
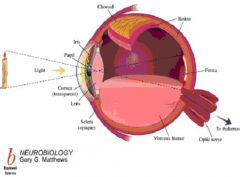
(1) Tough outer covering
(2) White, reflects all external light NOTES: The sclera is the white outer coating of the eye made of tough fibrin connective tissue which gives the eye its shape and helps to protect the delicate inner parts. In children, it is thinner and shows some of the inlying blueness. There are some diseases like scleritis that cause some blindness. It appears that these diseases produce a dark vertical line through the eye sight which avoids the 100% of visibility. |
|
|
|
Describe conjunctiva of the eye?
|
(1) Skin-like membrane from the limbus of cornea to the orbit
(2) Isolates retro-orbital space (3) Clinical involvement: Conjunctivitis NOTES: The conjunctiva is a membrane that covers the sclera (white part of the eye) and lines the inside of the eyelids. It helps lubricate the eye by producing mucus and tears, although not as much tears as the lacrimal gland. |
|
|
|
What is conjunctivitis?
|
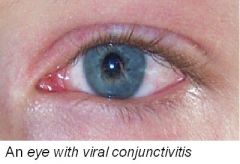
Conjunctivitis (commonly called "pinkeye") is an inflammation of the conjunctiva (the outermost layer of the eye and the inner surface of the eyelids), often due to infection. There are three common varieties of conjunctivitis, viral, allergic, and bacterial. Other causes of conjunctivitis include thermal and ultraviolet burns, chemicals, toxins, overuse of contact lenses, foreign bodies, vitamin deficiency, dry eye, dryness due to inadequate lid closure, exposure to chickens infected with Newcastle disease, epithelial dysplasia (pre-cancerous changes), and some conditions of unknown cause such as sarcoidosis.
|
|
|
|
Describe the optic nerve head?
|
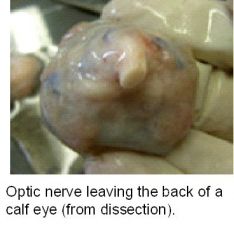
(1) axons and vasculature exits eye
(2) no photoreceptors; blind spot (3) Clinical involvement: glaucoma NOTES: The optic nerve is the second of twelve paired cranial nerves but is considered to be part of the central nervous system as it is derived from an outpouching of the diencephalon during embryonic development. This is an important issue, as fiber tracks of the mammalian central nervous system (as opposed to the peripheral nervous system) are incapable of regeneration and hence optic nerve damage produces irreversible blindness. The fibers from the retina run along the optic nerve to nine primary visual nuclei in the brain, from whence a major relay inputs into the primary visual cortex. The optic nerve is composed of retinal ganglion cell axons and support cells. It leaves the orbit (eye) via the optic canal, running postero-medially towards the optic chiasm where there is a partial decussation (crossing) of fibers from the temporal visual fields of both eyes. Most of the axons of the optic nerve terminate in the lateral geniculate nucleus from where information is relayed to the visual cortex. |
|
|
|
What are the 6 components of the photoreceptors in the retina?
|
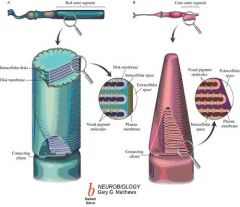
1. Outer segment
2. Cilium 3. Inner segment 4. Synaptic terminal 5. Cones 6. Rods |
pOCIS Can Run
|
|
|
Compare:
1. Outer segment of photoreceptors of the retina 2. Inner segment of photoreceptors of the retina |
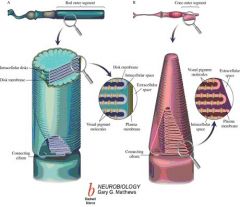
1. Outer segment of photoreceptors : Light absorption by densely packed photopigments in densely stacked disks
2. Inner segment of photoreceptors: Cell nucleus and metabolic machinery |
|
|
|
Describe the cilium of photorecepto cells of the retina?
|
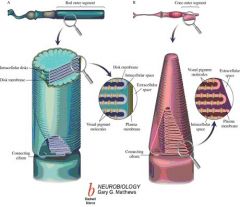
The outer segment of the rod photoreceptor cell in the human eye is connected to its cell body with a specialized non-motile cilium.
|
|
|
|
Describe the cone photoreceptors?
|
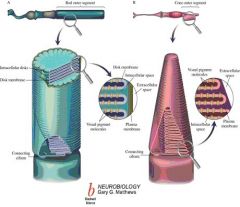
Cones
i. Bright light ii. Central retina iii. Three photopigments (trichromatic) in 3 different cone types (1) Short wavelength (blue) cones (2) Middle wavelength (green) cones (3) Long wavelength (red) cones (4) Clinical involvement: dichromatic (red/green color defective), monochromatic (color blind, rare) NOTES: Cone cells, or cones, are cells in the retina of the eye which only function in relatively bright light. There are about 6 million in the human eye, concentrated at the fovea. They gradually become more sparse towards the outside of the retina. Cones are less sensitive to light than the rod cells in the retina (which support vision at low light levels), but allow the perception of color. They are also able to perceive finer detail and more rapid changes in images, because their response times to stimuli are faster than those of rods (Kandel et al., 2000). Because humans (normally) have three kinds of cones, with different photopsins, which have different response curves (that is, they respond to variation in color in different ways), we have trichromatic vision. The central retina is cone-dominated and the peripheral retina is rod-dominated. In total there are about six million cones and a hundred and twenty-five million rods. The cones respond to bright light and mediate high-resolution vison and colour vision. Humans and old world monkeys have three different types of cones (trichromatic vision) while other mammals lack cones with red sensitive pigment and therefore have poorer (dichromatic) colour vision. |
|
|
|
Describe trichromatic color vision ?
|
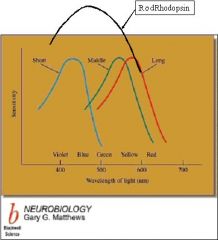
Three photopigments (trichromatic) in 3 different cone types
(1) Short wavelength (blue) cones (2) Middle wavelength (green) cones (3) Long wavelength (red) cones (4) Clinical involvement: dichromatic (red/green color defective), monochromatic (color blind, rare) NOTES: Trichromatic color vision is the ability of humans and some other animals to see different colors, mediated by interactions among three types of color-sensing cone cells. Each of the three types of cone in the retina of the eye contains a different type of photosensitive pigment called retinal, which is composed of a transmembrane protein called opsin and a light-sensitive protein called 11-cis retinal. Each different pigment is especially sensitive to a certain wavelength of light (that is, the pigment is most likely to produce a cellular response when it is hit by a photon with the specific wavelength to which that pigment is most sensitive). The three types of cones are L, M, and S, which have pigments that respond best to light of long (especially 560 nm), medium (530 nm), and short (420 nm) wavelengths respectively (Kandel et al., 2000). Since the likelihood of response of a given cone varies not only with the wavelength of the light that hits it but also with its intensity, the brain would not be able to discriminate different colors if it had input from only one type of cone. Thus, interactions between at least two types of cone is necessary to produce the ability to perceive color. With at least two types of cones, the brain can compare the signals from each type and determine both the intensity and color of the light. For example, moderate stimulation of a medium-wavelength cone cell could mean that it is being stimulated by very bright red (long-wavelength) light, or by not very intense yellowish-green light. But very bright red light would produce a stronger response from L cones than from M cells, while not very intense yellowish light would produce a stronger response from M cells than from other cells (counterintuitively, a "strong response" here refers to a large hyperpolarization, since rods and cones communicate that they are being stimulated by not firing). Thus trichromatic color vision is accomplished by using combinations of cell responses. |
|
|
|
Describe color blindness?
|

Color blindness, or color vision deficiency, in humans is the inability to perceive differences between some or all colors that other people can distinguish. It is most often of genetic nature, but may also occur because of eye, nerve, or brain damage, or due to exposure to certain chemicals. Color blindness is usually classed as a disability; however, in select situations color blind people have advantages over people with normal color vision. Color blind hunters are better at picking out prey against a confusing background, and the military have found that color blind soldiers can sometimes see through camouflage that fools everyone else. Monochromats may have a minor advantage in dark vision, but only in the first five minutes of dark adaptation.
|
|
|
|
Describe Rod cells?
|
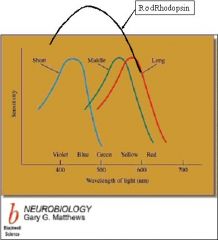
i. Dim light (night vision)
ii. Peripheral retina iii. Rhodopsin (a) Broad band (no color vision) NOTES: Rod cells, or rods, are photoreceptor cells in the retina of the eye that can function in less intense light than can the other type of photoreceptor, cone cells. Since they are more light-sensitive, rods are responsible for night vision. Named for their cylindrical shape, rods are concentrated at the outer edges of the retina (see peripheral vision). There are about 100 million rod cells in the human retina. A rod cell is sensitive enough to respond to a single photon of light. Since rods require less light to function than cones, they are therefore the primary source of visual information at night. Cone cells, on the other hand, require tens to hundreds of photons to become activated. Additionally, multiple rod cells converge on a single interneuron, collecting and amplifying the signals. This convergence comes at a cost to visual acuity, however, since the pooled information from multiple cells is less distinct than if the visual system received information from each rod cell individually. The convergence of rod cells also tends to make peripheral vision very sensitive to movement. Rod cells also respond more slowly to light than do cones, so stimuli they receive are added over about a hundred milliseconds. While this makes rods more sensitive to smaller amounts of light, it also means that their ability to sense temporal changes (such as quickly changing images) is less accurate than that of cones (Kandel et al., 2000). Because they have only one type of light sensitive pigment (rather than the three types that human cone cells have), rods have little, if any, role in color vision. |
|
|
|
Describe synaptic terminals of photoreceptors?
|
Like cones, rod cells have a synaptic terminal, an inner segment, and an outer segment. The synaptic terminal forms a synapse with another neuron, for example a bipolar cell. The inner and outer segments are connected by a cilium (Kandel et al., 2000). The inner segment contains organelles and the cell's nucleus, while the outer segment, which is pointed toward the front of the eye, contains the light-absorbing materials (Kandel et al., 2000).
|
|
|
|
Compare Rods and Cones?
|

Here is a chart
|
|
|
|
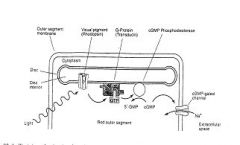
Describe the 5 major steps in phototransduction of photoreceptors?
|
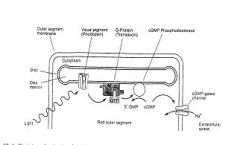
1. “Dark current”, photoreceptors depolarized in darkness
2. cGMP-gated cation channel 3. Photoreceptors hyperpolarize to light 4. Light activates multi-stage, amplifying, 2nd messenger cascade within outer segments 5. No voltage-dependent Na channels NOTES: Activation of a photoreceptor cell is actually a hyperpolarization; when they are not being stimulated, rods and cones depolarize and release a neurotransmitter spontaneously, and activation of photopigments by light sends a signal by preventing this. Depolarization occurs due to the fact that in the dark, cells have a relatively high concentration of cyclic guanosine 3'-5' monophosphate (cGMP), which opens ion channels (largely sodium channels, though Calcium can enter through these channels as well). The positive charges of the ions that enter the cell down its electrochemical gradient change the cell's membrane potential, cause depolarization, and lead to the release of the neurotransmitter glutamate. Glutamate can depolarize some neurons and hyperpolarize others, allowing photoreceptors to interact in an antagonistic manner. When light hits photoreceptive pigments within the photoreceptor cell, the pigment changes shape. This causes it to activate a regulatory protein called transducin, which leads to the activation of cGMP phosphodiesterase, which breaks cGMP down into 5'-GMP. Reduction in cGMP allows the ion channels to close, preventing the influx of positive ions, hyperpolarizing the cell, and stopping the release of neurotransmitters (Kandel et al., 2000). Activation of a single molecule of rhodopsin, the photosensitive pigment in rods, can lead to a large reaction in the cell because the signal is amplified. One activated, rhodopsin can activate hundreds of transducin molecules, each of which in turn activate a phosphodiesterase molecule, which can break down over a thousand cGMP molecules per second (Kandel et al., 2000). Thus rods can have a large response to a small amount |
Poor = DoG Likes 2 Nap
|
|
|
What is the effect of High “resting” [cGMP]in photoreceptors?
|
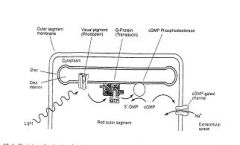
It causes open channels creating +_inward, depolarizing current
|
|
|
|
What is the effect of light on photoreceptors?
|
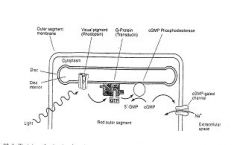
HYPERPOLARIZATION!
|
|
|
|
Describe light activatation of multi-stage, amplifying, 2nd messenger cascade within the outer segments of photoreceptors?
|
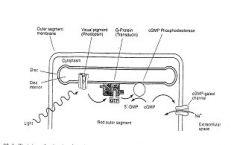
1. Photon captured by photopigment
2. Retinal conformation change activates photopigment 3. Photopigment activates G-protein (transducin) 4. Transducin activates phosphodiesterase 5. Phosphodiesterase hydrolyzes intracellular cGMP to 5'-GMP 6. Reduces [cGMP] and thus inactivates cation channel 7. reduces inward, depolarizing current |
|
|
|
What type of channels are located in photoreceptors?
|
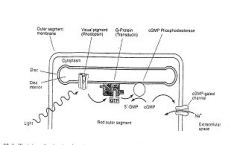
No voltage-dependent Na channels
i. No action potentials ii. Graded, receptor potentials only !!!! |
|
|
|
What are the 5 layers (alternation of cell bodies/fibers&synapses) involved in Retinal processing of signals?
|
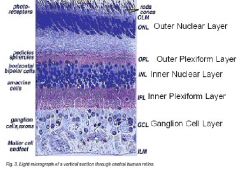
1. Outer nuclear layer
2. Outer plexiform layer 3. Inner nuclear layer 4. Inner plexiform layer 5. Ganglion cell layer |
rONPIG
|
|
|
What happens to light when it gets to the 5 layers Retinal processing of signals?
all layers before absorption by outer segments (except at fovea) |
Light passes thru all layers before absorption by outer segments (except at fovea)
|
|
|
|
What are the 5 cell types involved in retinal processing of signals?
|
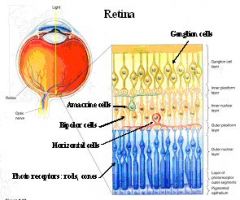
1. Photoreceptors
2. Bipolar cells 3. Ganglion cells 4. Horizontal cells 5. Amacrine cells |
Buy GAP Heels
|
|
|
What 3 retina cell types are involved in Information throughput?
|
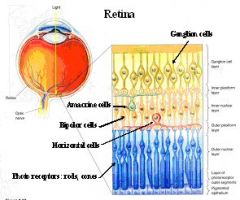
1. Photoreceptors
2. Bipolar cells 3. Ganglion cells |
Inexpensive : Pretty BaG
|
|
|
What 2 retina cell types are involved in Lateral information flow?
|
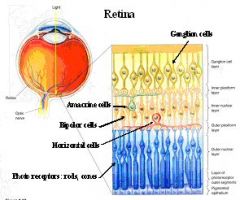
1. Horizontal cells
2. Amacrine cells |
Less = HAm is healthy
|
|
|
2 characteristics of photoreceptors?
|
(1) Photoreceptors
1. receptor potentials to light absorbtion 2. glutamate release decreases in response to light |
|
|
|
Describe bipolar cells of the retina?
|
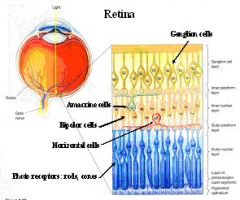
1. They have receptor potentials to photoreceptor & horizontal cell inputs
2. They have no voltage-dependent Na channels; no action potentials They have an antagonistic center-surround receptive field 5. They are Two types named by their response to light in Receptive Field center |
|
|
|
What are the 2 types of bipolar cells and what determines the two types of bipolar cells based on their response to light in Receptive Field Center?
|
1. ON - bipolar
2. OFF - bipolar Their response type is determined by different post-synaptic glutamate receptors |
|
|
|
Describe the ON - bipolar cell and the effect of light on it when light is in the center or off center?
|
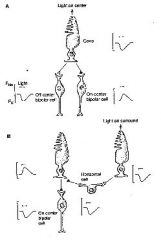
1)center depolarizes to light
2)receives “inhibitory” sign-reversing synapse 3)glutamate-gated 2nd messenger cascade to close cGMP-gated Na channels (similar to the light-activated cascade in outer segment) 4)glutamate-gated K channel opens +_outward current to hyperpolarize NOTES: When light hits a photoreceptor cell, the photoreceptor hyperpolarises, and its glutamate production decreases. An ON-cell will react to this change by depolarizing. The interactions between bipolar cells and the horizontal cells create an extra layer of complexity - ON bipolar cells will depolarise to a stimulus that is in the centre of their receptive field, and hyperpolarise to a stimulus that is in the periphery of the receptive field. |
|
|
|
Describe the OFF - bipolar cell and the effect of light on it when light is in the center or off center?
|
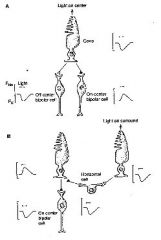
OFF-bipolar
1)center hyperpolarizes to light 2)receives “excitatory” sign-conserving synapse 3)glutamate-gated cation (Na) channel opens +_inward current to depolarize NOTES: When light hits a photoreceptor cell, An OFF-cell will depolarize when glutamate production increases(when light power decreases). The interactions between bipolar cells and the horizontal cells create an extra layer of complexity - OFF bipolar cells will hyperpolarize to a stimulus that is in the centre of their receptive field, and depolarize to a stimulus that is in the periphery of the receptive field. |
|
|
|
What is the role of the centre-surround relationship in bipolar cells?
|
This mutually inhibitory centre-surround relationship increases the contrast of the retinal image by enhancing the edges of the object that is viewed.
|
|
|
|
Describe the ganglion cells of the retina?
|
1. They are the output cells of the retina via axons through the optic nerve head and optic nerve
2. They have receptor potentials & action potentials to bipolar cell and amacrine cell inputs 3. They transmit Action Potentials long distance through optic nerve to thalamus, etc. 4. They have center-surround Receptive Fields. |
|
|
|
Relate ON-center and OFF-center types between ganglion cells and bipolar cells?
|
In ganglion cells, the ON-center and OFF-center types are conserved from bipolar cell inputs.
|
|
|
|
Describe the organization of ganglion cells' receptive fields?
|
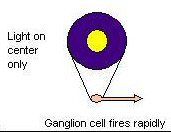
It is composed of inputs from many rods and cones, and it provides a way of detecting contrast, and is used for detecting objects' edges. Each receptive field is arranged into a central disk, the "centre", and a concentric ring, the "surround", each region responding oppositely to light. For example, light in the centre might increase the firing of a particular ganglion cell, whereas light in the surround would decrease the firing of that cell.
|
|
|
|
Describe an ON - center retinal ganglion cell?
|
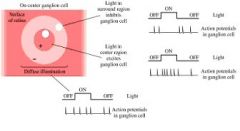
An on-center cell is stimulated when the center of its receptive field is exposed to light, and is inhibited when the surround is exposed to light. Stimulation of the center of an on-center cell's receptive field produces depolarization and an increase in the firing of the ganglion cell, stimulation of the surround produces a hyperpolarization and a decrease in the firing of the cell, and stimulation of both the center and surround produces only a mild response (due to mutual inhibition of center and surround). When photoreceptors in the center of an on-center ganglion cell's receptive field are stimulated, they stop releasing glutamate (because photoreceptors are depolarized in the absence of light and respond to light by hyperpolarizing). At their synapses with the on-center cell, glutamate acts as an inhibitory neurotransmitter, opening channels that hyperpolarize the cell. Stopping the release of glutamate inhibits an inhibitory effect, leading to an increase in the firing of the on-centre cell. Conversely, when photoreceptors in the surround of an on-center ganglion cell's receptive field are stimulated, although they respond by stopping the release of glutamate, at their synapses with the ganglion cell, glutamate acts as an excitatory neurotransmitter, opening channels that depolarize the cell. Stopping the release of glutamate inhibits an excitatory effect, leading to a decrease in the firing of the on-centre cell. A photoreceptor can make synapses with both on-center and off-center cells and thus has synapses in which glutamate is excitatory as well as those in which it is inhibitory.
|
|
|
|
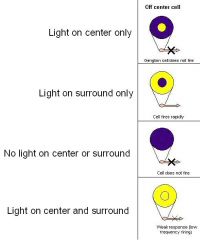
What could happen in these 4 scenarios of an ON - center retinal ganglion cell:
1. Light on center only 2. Light on surround only 3. No light on center or surround 4. Light on center and surround |

Diagram has answer
|
|
|
|
Describe an OFF -center retinal ganglion cell?
|
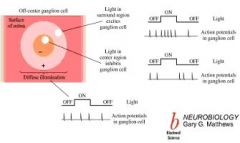
An off-center cell is inhibited when the center of its receptive field is exposed to light, and is stimulated when the surround is exposed to light. Stimulation of the center of an off-center cell's receptive field produces hyperpolarization and a decrease in the firing of the ganglion cell, stimulation of the surround produces a depolarization and an increase in the firing of the cell, and stimulation of both the center and surround produces only a mild response (due to mutual inhibition of center and surround). Therefore, an off-center cell is stimulated by activation of the surround and inhibited by stimulation of the center (see figure).
|
|
|
|
What could happen in these 4 scenarios of an OFF - center retinal ganglion cell:
1. Light on center only 2. Light on surround only 3. No light on center or surround 4. Light on center and surround |
See diagram
|
|
|
|
What is the general role of the center-surround receptive field organization in a ganglion cell?
|
It allows ganglion cells to transmit information not merely about whether photoreceptor cells are firing, but also about the differences in firing rates of cells in the center and surround. This allows them to transmit information about contrast. The size of the receptive field governs the spatial frequency of the information: small receptive fields are stimulated by high spatial frequencies, fine detail; large receptive fields are stimulated by low spatial frequencies, coarse detail. Retinal ganglion cell receptive fields convey information about discontinuities in the distribution of light falling on the retina; these often specify the edges of objects.
|
|
|
|
What are 2 general characteristics of lateral information flow in horizontal cells of the retina?
|
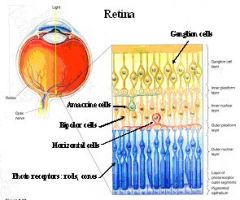
1. Receptive Field surround in bipolar cells is created by an “inhibitory” sign-reversing synapse from intervening horizontal cell.
2. No voltage-dependent Na channels; no action potentials; graded postsynaptic potentials only |
|
|
|
Give 3 reasons why Receptor Field surround in bipolar cells is created by an “inhibitory” sign-reversing synapse from intervening horizontal cells?
|
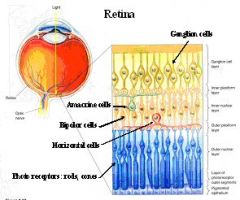
1. The “surround” photoreceptor to horizontal cell synapse is excitatory (glutamate-gated cation channel)
2. The horizontal cell to “center” photoreceptor synapse is inhibitory (glutamate-gated 2nd messenger cascade to close cGMP-gated Na). 3. This creates antagonistic surround responses in photoreceptors opposite the center response (regardless of ON- or OFF-type) NOTES: In submammalian species intracellular recordings from the cones have indicated that they receive a feed-back inhibitory message from horizontal cells (Baylor et al., 1971). In fish retinas there is morphological evidence that the horizontal cell lateral elements at the triad synapse produce spinules at which feed-back signalling occurs to the cone (Djamgoz and Kolb, 1993, for a review), In mammalian cones there is no unequivocal morphological evidence for this feed-back synapse but some kind of feed-back is expected at this site (see above). We know that photoreceptor neurotransmitter is released in the dark in the vertebrate retina. Thus the photoreceptor, whether it be rod or cone is in a depolarized state in the dark. On light stimulation the photoreceptor reacts with a hyperpolarization, transmitter release ceases but the postsynaptic bipolar cells respond with either hyperpolarization or depolarization of their membranes. The horizontal cells responds too, with a hyperpolarization, but a feedback synapse from the horizontal cell to the photoreceptor is also thought to occur. The feedback signal sums information from a network of horizontal cells connected over a wide spatial area of the outer plexiform layer. Thus, this large spatial area influences the photoreceptor and the bipolar cell to include a response coming from a surround region of retina. This local circuit provides the bipolar cell with a center-surround organization. |
|
|
|
Describe the amacrine cells in the retina and their characteristics?
|
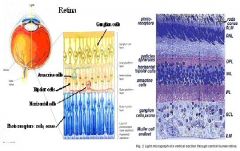
1. They are not as well understood
2. They have receptor potentials and action potentials to bipolar cell inputs 3. They have transient responses to sustained stimulation (i) ON, OFF and ON/OFF responses 4. They have large complex processes with pre- and post-synaptic functions 5. They have many specialized neurotransmitter types that “tile” the retina NOTES: Amacrine cells are interneurons in the retina which operate at the Inner Plexiform Layer (IPL), the second synaptic retinal layer where bipolar cells and ganglion cells synapse. The cell nuclei of amacrine cells are found in the Inner Nuclear Layer (INL). There are about 40 different types, most lacking axons. They are classified by the width of their field of connection, which layer(s) of the stratum in the IPL they are in, and by neurotransmitter type. Most are inhibitory using either GABA or glycine as neurotransmitters. Functionally, they are responsible for complex processing of the retinal image, specifically adjusting image brightness and, by integrating sequential activation of neurons, detecting motion. |
|

