![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
49 Cards in this Set
- Front
- Back
|
What are the Opioids derived from?
|
Opium poppy = Papaver Somniferum
-contains opiate compounds including Morphine & Codeine |
|
|
This is a tincture of opium used in the olden days, used for "nerves", cough, & diarrhea
|
Laudanum
|
|
|
What are the 3 different Opioid receptors?
|
Mu = Morphine
Delta = Enkephalin Kappa = Dynorphin |
|
|
What type of receptor are the Opioid receptors?
What actions do they possess? |
G-protein coupled
Close Ca++ channels on Presynaptic neurons, reducing evoked transmitter release Open K+ channels on Postsynaptic neuron, hyperpolarizing membranes |
|
|
What actions do Mu receptors produce?
|
1. Analgesic
2. Sedative 3. Euphoric effects 4. untoward side effects |
|
|
What actions do the Delta Opioid receptors possess?
|
Analgesia at spinal levels
|
|
|
What actions do the Kappa Opioid receptors possess?
|
1. may contribute to Analgesia
2. Primarily results in Dysphoria = anxiety, depression, unease |
|
|
Although the Sigma receptor is not an Opioid receptor, what effect may Opioids have on this receptor?
|
may contribute to Dysphoric effects
|
|
|
Explain the ways in which Opioid drugs interact with the body's endogenous opioid peptide system to limit pain
|
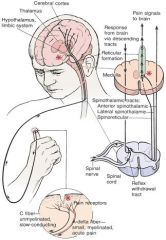
1. Pain-modulating descending pathways from CNS
-Periaqueductal Grey Matter (PAG) -Rostral Ventral Medulla (RVM) 2. Pre- and Postsynaptic Spinal actions -Inhibitory Postsynaptic Potential (IPSP) -inhibition of neurotransmitter release 3. Opioid receptors in peripheral tissues |
|
|
What are the CNS pharmacological effects of Opioids?
|
1. Analgesia = changes perception & experience of pain; does not decrease sensation
2. Euphoria/Dysphoria 3. Sedation 4. Respiratory depression 5. Cough suppression 6. Miosis (Parasympathetic) 7. Truncal Rigidity (impairs ventilation) 8. Nausea & Vomiting = Chemoreceptor Trigger Zone |
|
|
What are the Peripheral pharamacological effects of Opioids? (7)
|
1. Arterial & Venous dilation
2. Constipation 3. Biliary colic (cholinergic) 4. decreased Renal blood flow = decreased renal fxn 5. decreased Uterine tone 6. Endocrine alterations -increased ADH, Prolactin, Somatotropin release -decreased LH release 7. Histamine release -flushing -sweating -rashes & itching |
|
|
What are the clinical uses of Opioids? (5)
|
1. Acute or Chronic Pain
-Analgesic -no apparent maximal dose -less effective for neuropathy (use adjuvant analgesics such is Imipramine or GABApentin) 2. Acute pulmonary edema or MI = decrease the sensation of crisis 3. Cough = anti-tussive 4. Diarrhea = decrease GI motility 5. Anesthesia/preoperative meds = anesthetic sparing |
|
|
What are the toxicities of Opioids? (5)
|
1. Respiratory Depression = primary cause of death
2. Dysphoria 3. N/V 4. Constipation 5. Seizures = high doses - may be delta-mediated |
|
|
When dose Opioid Tolerance start?
After how long is tolerance clinically apparent? |
Starts with 1st dose
apparent in 2-3 wks |
|
|
Describe the tolerance timeline of the symptoms of opioid use
|
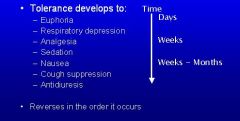
ERA-SNCA
|
|
|
What side effects are there no tolerance to with Opioid use? (3)
|
1. Miosis
2. Constipation 3. Seizures **cross tolerance occurs as well |
|
|
Describe the Abstinence Syndrome associated with Opioid Withdrawal
|
1. Dysphora
2. Rhinorrhea 3. Lacrimation 4. Yawning 5. Chills 6. Vomiting 7. Diarrhea 8. Anorexia 9. Insomnia 10. Anxiety 11. Hostility |
|
|
What is compulsive drug seeking in dependent opioid individuals due to?
|
due to avoiding the Withdrawal symptoms
|
|
|
What are the 2 drugs used to treat ACUTE Opioid Overdose?
|
1. Naloxone = IM or IV
- 1 to 2 hr duration 2. Nalmefene = IV -Half-life = 8-10 hrs **these can precipitate withdrawal symptoms |
|
|
What drug is used to prevent relapse in Opioid Addicts?
|
Naltrexone = Oral
-Half-life = 10 hrs |
|
|
What is the relative efficacy of Opioid drugs based on?
|
Analgesia
"Equianalgesic dose" = equal to 10 mg Morphine |
|
|
List the 5 High Efficacy Analgesic Opioids
What are they used for? |
1. Morphine
2. Methadone 3. Meperidine 4. Fentanyl 5. Alfentanil Severe pain = trauma, post-surgical, MI, etc |
|
|
List the properties of Morphine
|
1. High efficacy analgesic
2. Poor oral bioavailability 3. Duration is 4-5 hrs |
|
|
List the properties of Methadone
|
1. High Efficacy Analgesic
2. Longer acting = ~6 hrs; plasma half-life = ~24 hrs 3. Good Oral bioavailability 4. used as maintenance in addicts |
|
|
List the properties of Meperidine
|
1. High Efficacy Analgesic
2. Medium acting = 2-4 hrs 3. Antimuscuranic 4. metabolized to Normeperidine = psychoactive, seizures |
|
|
List the properties of Fentanyl
|
1. High Efficacy analgesic
2. short acting = 1-1.5 hrs 3. primarily acts at MU receptors 4. poor Oral bioavailability 5. transdermal dosage forms available |
|
|
List the properties of Alfentanil (5)
|
1. High efficacy analgesic
2. very short acting = 15-45 minutes 3. very potent 4. Parenteral only 5. useful for brief, painful procedures |
|
|
List the Low-Medium Efficacy Analgesics (5)
|
1. Codeine
2. Hydrocodone 3. Oxycodone 4. Propoxyphene 5. Tramadol |
|
|
List the properties fo Low-Medium Efficacy Analgesics
|
1. partial agonist or drugs that are not tolerated at higher doses
2. All typically administered orally 3. used for Moderate pain = broken bones, dental procedures, etc 4. often formulated with Aspirin, Acetominophen, Ibuprofen |
|
|
Low efficacy analgesic
|
Codeine
|
|
|
List the 2 Moderate Efficacy Analgesics
|
Hydrocodone
Oxycodone |
|
|
Very low efficacy Analgesic that is only administered orally
|
Propoxyphene
|
|
|
Low-Medium efficacious analgesic that has Propoxyphene-like metabolites; inhibits NE & Serotonin re-uptake
|
Tramadol
|
|
|
What are the advantages of the Mixed Agonist-Antagonist Analgesics?
|
believed to have less addictive potential & risk of respiratory depression
|
|
|
Mu partial agonist
a. Buprenorphine b. Butorphanol c. Nalbuphine d. Pentazocine |
Buprenorphine
|
|
|
Kappa agonist, Mu partial agonist or antagonist
a. Buprenorphine b. Butorphanol c. Nalbuphine d. Pentazocine |
Butorphanol & Pentazocine
|
|
|
Kappa agonist, Mu antagonist
a. Buprenorphine b. Butorphanol c. Nalbuphine d. Pentazocine |
Nalbuphine
|
|
|
What are the Anti-diarrheal Opioids?
|
Diphenoxylate
Loperamide (OTC) **have poor permeation of the BBB |
|
|
What are the Anti-tussive Opioids? (cough suppressants)
|
Codeine
Dextromethorphan (OTC) **poor permeation of the BBB |
|
|
What is the Opioid drug of abuse?
|
Heroin
|
|
|
1. What opioids are only administered Parenterally? (2)
2. What opioids that are given orally avoid 1st pass metabolism? (3) 3. What opioid is given transdermally? (1) 4. What opioid is given nasally? (1) |
1. Alfentanil & Nalbuphine
2. Methadone, Levorphanol, Codeine 3. Fentanyl 4. Butorphanol |
|
|
What is the prototypical duration of action of Opioids (unless otherwise noted)?
|
4 hours
|
|
|
How is Morphine metabolized?
|
Glucuronidated
*M-6G is more potent than Morphine |
|
|
What Opioid metabolite is psychoactive?
|
Normeperidine
|
|
|
What are the contraindications of Opioid usage? (5)
|
1. Head injuries = Vasodilation -> increases Intracranial pressure
2. Pregnancy = fetus addiction 3. Impaired pulmonary function 4. Liver or Kidney compromised patients 5. Endocrine disorders = can result in exaggerated & prolonged effects -Addison's disease -Hypothyroidism |
|
|
What are the drug interaction when Pure agonists are given with Mixed Agonist-Antagonists? (2)
|
1. decreased Analgesia
2. can precipitate withdrawal symptoms |
|
|
What drug interactions occur when opioids are combined with other sedative-hypnotics?
|
increased Sedation & Respiratory Depression
|
|
|
What drug interaction occur when Opioids are combined with Antipsychotics?
|
1. Increased sedation & Respiratory depression
2. increased risk of seizures |
|
|
What drug interactions occur when Opioids are combined with MAOI's?
|
1. Increased risk of Hyperpyrexic Coma (esp. Pargyline & Meperidine)
2. Hypertension |

