![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
36 Cards in this Set
- Front
- Back
|
Primary indication for pulmonary surfactant |
Membrane Disease (HMD)/ARDS -Preterm baby= 30-32 weeks normally |
|
|
Treatment strategies include |
Oxygen: enhances oxygenation directly, and by decreasing intrapulmonary shunting ***CPAP (Continuous Positive Airway Pressure) preterm babies (Stabilize FRC..answers usually CPAP!) Mechanical Ventilation Surfactant Replacement Therapy (Have to intubate them but don't have to go on mechan vent) IMPORTANT: Consider Extra-pulmonary causes: - Hypovolemia, Anemia - Acidosis, Hypoglycemia, Hypothermia - CNS hemorrhage, drugs, neuromuscular disease - Heart disease |
|
|
It has been shown that surfactant treatment at less than ______of life significantly decreases the _____________ |
2 hrs rates of death, air leak, and death or bronchopulmonary dysplasia in preterm infants. |
|
|
When should we intubate to administer surfactant? |
IN-SUR-E Trial/Method Intubation (Early) Surfactant (Early) Extubation (Early)With or without nCPAP |
|
|
INSURE method |
(INtubation-SURfactant-Extubation) in early and late premature neonates with respiratory distress: factors affecting the outcome and survival rate. |
|
|
RDS and Surfactant Replacement TherapyGoals |
○Prevent progression of disease process ○Intervene early to establish FRC in the delivery room and the NICU -CPAP -Appropriate Mechanical Ventilation Techniques/Management -Surfactant replacement |
|
|
Physical principles of surfactant administration |
Administered to replace missing pulmonary surfactant in respiratory distress syndrome (RDS) of newborn |
|
|
Define surfactant |
Surface-active agent that lowers surface tension (detergents) |
|
|
Define surface tension |
Force caused by attraction between like molecules that occurs at liquid–gas interfaces and holds liquid surface intact |
|
|
LaPlace’s Law Physical principle describing and quantifying: |
-The relation between internal pressure of drop or bubble -Amount of surface tension -Radius of drop or bubble -For bubble, which is liquid film with gas inside and out, LaPlace’s Law is: Pressure = (4 × surface tension)/radius |
|
|
In alveoli there is only one single air–liquid interface, LaPlace’s Law would be: |
Pressure = (2 × surface tension)/radius |
|
|
The higher the surface tension of the liquid, the greater is the _______, Which can what ______ |
compressing force inside the alveolus, which can cause collapse or cause difficulty in opening the alveolus |
|
|
Lowering the surface tension will have what effect? |
ease the alveolar opening allow for maintenance of recruitment |
|
|
Exogenous surfactants are clinically indicated for |
treatment or prevention of RDS in newborns |
|
|
Clinical Indications for Exogenous Surfactants |
-treatment or prevention of RDS in newborns -Prophylactic treatment -Rescue treatment: |
|
|
Prophylactic treatment: |
Prevention of RDS in very-low-birth-weight infants Infants with higher birth weights, but with evidence of immature lungs Infants who are at risk for developing RDS |
|
|
Rescue treatment: |
Retroactive or “rescue” treatment of infants who have developed RDS |
|
|
Composition of pulmonary surfactant |
Lipids 85 to 90% of surfactant by weight -Mostly phosphatidylcholine -Dipalmitoylphosphatidylcholine (DPPC)
(Other 10% is cholesterol) Proteins -Surfactant protein A (SP-A) (Reuptake) -Surfactant proteins B and C (SP-B, SP-C) (Spreading of surfactant) -Surfactant protein D (SP-D) |
|
|
Production and regulation of surfactant secretion:
Synthesized in? Major stimulus? Key feature? |
●Synthesized in type II alveolar cells and stored in vesicles termed lamellar bodies
●Major stimulus for secretion of lamellar bodies into alveolar space appears to be inflation of the lung (Exception C-sect- don't get all amniotic fluid squeezed out) ●10% of the intracellular pool is secreted every hour
●Key feature: recycling activity (Re-uptake) |
|
|
Types of exogenous surfactant preparations |
●Natural/modified natural surfactant Survanta (Bovine), Curosurf (Porcine), Infasurf
●Synthetic surfactant Lucinactant (Surfaxin) Clinical trials in Latin America were criticized for protocol based in potentially unethical principles.
●Synthetic natural surfactantNone at this time |
|
|
Signs NB gives you: unstable FRC |
Increase RR Grunting Nasal flaring Chest recoil |
|
|
Beractant (Survanta) Indications: |
A modified natural surfactant (bovine)
Indications for use: Prophylactic therapy of premature infants less than 1250 gram birth weight or with evidence of surfactant deficiency and risk of RDS
Agent should be given within 15 minutes of birth or ASAP
Rescue treatment of infants with evidence of RDS
Agent should be given within 8 hours of birth |
|
|
Beractant (Survanta) Dosage Administration |
Dosage 4 mg/kg of birth weight
Administration Do not shake Let stand at room temperature for 20 minutes Instilled into trachea through a 5-French catheter placed into the endotracheal tube (ETT)
Give in quarter doses from a syringe
During each quarter dose the infant is placed in a different position |
|
|
How to ensure homogenous distribution of SURVANTA? |
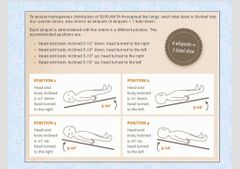
|
|
|
Calfactant (Infasurf) Indications: Treatment: |
Modified natural surfactant (bovine) Indications for use:Prevention (prophylaxis) of RDS in premature infants less than 29 weeks of gestational age and at high risk for RDS Preferably administered no more than 30 minutes after birth Treatment (rescue) of premature infants less than or equal to 72 hours of age who develop RDS and require endotracheal intubation |
|
|
Calfactant (Infasurf) Dosage Administration |
Dosage 3 mL/kg body weight at birth, delivered over two doses
Repeat doses, up to total of three doses; can be given 12 hours apart
Administration Side-port adaptor Catheter administration (5 F)
|
|
|
Poractant Alfa (Curosurf) Indications Unlabeled use
|
Natural surfactant (porcine) *most commonly used Cow based Indications for use: Treatment (rescue) of premature infants with RDS thus reducing mortality and pneumothoraces
Unlabeled uses: Severe meconium aspiration syndrome in term infants Respiratory failure caused by group B streptococcal infection in neonates |
|
|
Poractant Alfa (Curosurf) Dosage Administration |
Dosage 2.5 mL/kg birth weight; subsequent doses of 1.25 mL/kg birth weight can be given twice at 12-hour intervals if needed Maximum recommended total dose is 5 mL/kg Administration Warm to room temperature No need to reconstitute Administered in one dose or two aliquots through a 5-French catheter in ETT |
|
|
Mode of Action |
Replace and replenish deficient endogenous surfactant pool in neonatal RDS Can be recycled into type II cells and form a surfactant pool to regulate surface tension |
|
|
Clinical outcomes |
-Dramatic improvement in oxygenation
-Increase in functional residual capacity (FRC) or increased compliance Clearing of chest x-ray Blood gas (gas exchange) improvements Increased lung volumes (FRC & RV) Improved static compliance
|
|
|
Hazards and complications |
Airway occlusion, desaturation, bradycardia
High arterial oxygen (PaO2) values (Have to wean)
Overventilation and hypocapnia (Have to wean)
Apnea
Pulmonary hemorrhage- (treat: ice cold saline- vasoconstriction. Push epi. **go up on PEEP until blood stops coming out**) Typically: younger, smaller, PDA (patent ducts arternosis) |
|
|
AEROSURF |
(Not yet approved) Deliver surfactant without intubation! Delivered with aerosol |
|
|
Assessment |
Monitor pulse/cardiac rhythm (During and after administration) Signs of airway occlusion Color/activity level Chest rise Arterial oxygen saturation (Prevent hyperoxia Prevent hypoxia) |
|
|
Before treatment assess |
Assess the need for surfactant therapy. |
|
|
During treatment and short term assess |
●Monitor pulse and cardiac rhythm during and after administration.
●Monitor the infant for signs of airway occlusion (desaturation and bradycardia) during and after administration;
if obstruction is evident, remove the infant from the ventilator and manually ventilate;
in addition, saline lavage and aggressive suctioning to clear the airway may be needed. ●Monitor color and activity level of the infant. ●Monitor chest rise for level of ventilation, or use electronic monitor if available. ●Monitor arterial oxygen saturation and adjust Fio2 accordingly to prevent hyperoxia or hypoxia. ●Monitor transcutaneous Pco2 if possible, and be prepared to adjust level of ventilation as needed to prevent hypercarbia or hypocarbia. |
|
|
Long term assessment |
●Assess lung mechanics (exhaled volumes or peak inspiratory pressures) during mechanical ventilation to determine effectiveness of the exogenous agent in normalizing lung compliance. The instilled drug may cause changes within minutes in some cases. ●Assess the need for repeat dosing.Consider possible hazards if pulse, cardiac rhythm, or arterial/transcutaneous blood gas values deteriorate. |

